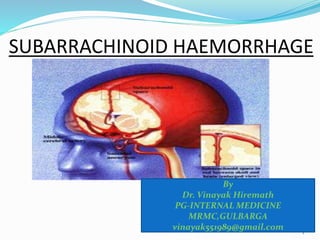
Subarachnoid hemorrhage
- 1. SUBARRACHINOID HAEMORRHAGE 1 By Dr. Vinayak Hiremath PG-INTERNAL MEDICINE MRMC,GULBARGA vinayak551989@gmail.com
- 2. SAH = extravasation of blood into the subarachnoid space
- 3. CLASSIFICATION OF STROKE 3 Stroke Primary Hemorrhagic (20% of Strokes) Primary Ischemic (80% of Strokes) Thrombotic 50% Embolic 30% Intracerebral Hemorrhage 15% Subarachnoid Hemorrhage 5%
- 4. INTRODUCTION Subarachnoid hemorrhage (SAH) is a pathologic condition that exists when blood enters the subarachnoid space The most common cause of SAH is trauma The most common cause of spontaneous SAH is an aneurysmal bleed (65-80%)
- 5. Anatomy of Subarachnoid space In the central nervous system, the subarachnoid cavity (subarachnoid space) is the interval between the arachnoid membrane and pia mater.
- 6. It is occupied by spongy tissue consisting of trabeculae (delicate connective tissue filaments that extend from the arachnoid mater and blend into the pia mater) and intercommunicating channels in which the cerebrospinal fluid is contained.
- 7. This cavity is small on the surface of the hemispheres of the brain. On the summit of each gyrus the pia mater and the arachnoid are in close contact, but in the sulci between the gyri, triangular spaces are left, in which the subarachnoid trabecular tissue is found.
- 8. At certain parts of the base of the brain, the arachnoid is separated from the pia mater by wide intervals, which communicate freely with each other and are named subarachnoid cisternae; in these the subarachnoid tissue is less abundant.
- 9. The subarachnoid space is the location of the interface between the vascular tissue and the cerebrospinal fluid and is active in the blood brain barrier.
- 12. When blood vessels of the brain are weak, abnormal, or under unusual pressure, a hemorrhagic stroke can occur. In hemorrhagic strokes, bleeding may occur within the brain, as an intracerebral hemorrhage. Or bleeding may occur between the inner and middle layer of tissue covering the brain (in the subarachnoid space), as a subarachnoid hemorrhage.
- 13. EPIDEMIOLOGY Incidence about 9-10/100,000/yr Higher in Japan (3 times) and Finland Mean age of onset 51 years (6th decade) Facts and figures Men predominate until age 40, then more women (55%); some studies – 3:2 ratio Seasonal (winter/spring), diurnal (late morning) and day (Sunday) 30 % rupture during sleep About 50 % of patients with an aneurysm have warning prior to SAH (6-20 days)
- 14. Case Fatality The Overall case fatality varied from 32-67% Population-based study in England with essentially complete case ascertainment 24 hour mortality: 21% 7 days: 37% 30 days: 44% Pobereskin JNNP 2001;70:340-3
- 15. OVERVIEW Highest mortality occurs immediately after the hemorrhage and then decreases rapidly Rebleeding is estimated to occur in 50% of ruptured aneurysms within 6 months of the first hemorrhage, and afterwards at 3% per year 50-60% of patients die after rebleeding and 25% are left disabled
- 16. Probably the best natural history data come from S Pakarinen: (Incidence, aetiology, and prognosis of primary subarachnoid hemorrhage: a study based on 589 cases diagnosed in a defined urban population during a defined period. Neurol Scand (Suppl) 1967; 29:1-128) Unselected series, involving the entire city of Helsinki, from 1954 to 1961; minimal surgical withdrawals; all sudden deaths were autopsied Mortality at 1 day was 32% Mortality at 1 week was 43% Mortality at 1 month was 56% Mortality at 6 months was 60%
- 17. ETIOLOGY CATEGORY CAUSES TRAUMA CLOSED, PENETRATING, ELECTRIC,ETC… VASCULAR ANEURYSMS, ATHEROSCLEROSIS, AVM, VASCULITIDES IDIOPATHIC BENIGN PERIMESENCEPHAIC SUBARACHNOID HEMORRHAGE BLOOD DYSCRASIAS LEUKEMIAS, HEMOPHILIAS, THROMBOCYTOPENIAS INFECTIONS DENGUE, LEPTOSPIROSIS, BACTERIAL MENINGITIS TOXINS AMPHETAMINES, COCAINE, NICOTINE, ANTICOAGULANTS NEOPLASMS GLIOMAS, MENINGIOMAS, HEMANGIOBLASTOMA, ETC
- 18. Risk Factors Hypertension Cigarette smoking Oral contraceptives Alcohol consumption (debatable) Diurnal variations in blood pressure Pregnancy and parturition Slight increased risk during lumbar puncture and/or cerebral angiography in patient with cerebral aneurysm Slight increased risk with advancing age Following cocaine abuse
- 19. Higher chance if: Female 3rd trimester of pregnancy Middle-aged Abuse of stimulant drugs –Connective tissue disorder –Family history
- 20. PATHOPHYSIOLOGY Modifiable Risk Factors >HPN >Smoking >excessive intake of foods high in fats and cholesterol Non-modifiable Risk Factors> Advanced Age >Gender >Heredity Triggering Factors >Sudden extreme emotion Arterio venous malformation Cerebral aneurysm rupture Bleeding into the brain tissue and subarachnoid space
- 21. Blood Clots in the Subarachnoid Space Brain Compression Blood supply interruption Tissue Necrosis Neuronal Death Increase Intracranial Pressure T total Paralysis Regional Paralysis Epileptic Seizure : increase intraocular pressure= blindness Death Coma
- 22. PATHOPHYSIOLOGY CEREBRAL BLOOD FLOW AND METABOLISM RAISED ICT IMPAIRED VASODILATORY AUTOREGULATION VASOSPASM WITH GLOBAL ISCHEMIA BLOOD (‘TOXIC’) BLOCKAGE OF THE ARACHNOID GRANULATIONS SYMPATHETIC SURGE MI PULMONARY EDEMA
- 23. CEREBRAL BLOOD FLOW/VOLUME/METABOLISM CBF is globally decreased after SAH Mean CBF decreases with time after SAH; it reaches a nadir in 10 to 14 days, after which it slowly increases toward normal, In patients with poor grades, CBF and cerebral metabolism may remain depressed for weeks ; Cerebral blood volume is markedly increased in patients with severe neurological deficits
- 24. INTRACRANIAL PRESSURE RESPONSES Mean ICP was 10 mm Hg in patients with clinical grades 1 and 2, 18 mm Hg in patients with clinical grades 2 and 3, and 29 mm Hg in those with clinical grades 3 to 5. Vasospasm, which was more common in patients with a poor clinical grade and larger SAH, was associated with a significant rise in ICP from a mean of 16 mm Hg in those without vasospasm to 29 mm Hg in those with vasospasm
- 25. An aneurysm is an abnormal widening or ballooning of a portion of an artery due to weakness in the wall of the blood vessel
- 26. Internal carotid artery Posterior communicating artery aneurysm
- 27. 27
- 29. Mechanism of formation of aneurysms One theory is – that they result from a developmental defect in the media & elastica Other theory says that aneurysmal process is initiated by the focal destruction of internal elastic membrane caused by hemodynamic forces acting at bifurcations & branching of arteries As a result of local weakness in vessel wall intima bulges out covered only by adventetia The sac gradually enlarges and subsequently rupture 29
- 30. 30 For patients of SAH who arrive alive at hospital, the mortality rate over the next month is about 45%. Of those who survive, more than 50% are left with major neurologic deficits as a result of Initial hemorrhage, Cerebral vasospasm with infarction, or Hydrocephalus.
- 31. If the patient survives but the aneurysm is not obliterated, the rate of rebleeding is about 20% in the first 2 weeks, 30% in the first month, and about 3% per year afterwards The annual risk of rupture for aneurysms <10 mm in size is 0.1%, and for aneurysms >10 mm in size is 0.5– 1%; the surgical morbidity rate far exceeds these percentages 31
- 32. 32 GIANT ANEURYSMS, those >2.5 cm in diameter account for 5% of cases. The three most common locations are -The terminal internal carotid artery, -Middle cerebral artery (MCA) bifurcation, and -Top of the basilar artery. Their risk of rupture is ~6% in the first year after identification and may remain high indefinitely. They often cause symptoms by compressing the adjacent brain or cranial nerves.
- 33. Saccular aneurysms occur at the bifurcations of the large to medium-sized intracranial arteries. Rupture is into the subarachnoid space, in the basal cisterns and often into the parenchyma of the adjacent brain. Approximately 85% of aneurysms occur in the anterior circulation, mostly on the circle of Willis. About 20% of patients have multiple aneurysms, - - many at mirror sites bilaterally. 33
- 34. 34
- 35. Aneurysms are seldom seen in childern on autopsy and so SAH in childern is rare Beyond childhood they gradually increase in size & the frequency of rupture increases between 35-65 yrs of age There is increased incidence of polycystic kidneys, fibromuscular dysplasia of extracranial arteries, moyamoya, AV malformations & coarctation of aorta Numerous studies have documented familial occurrence of saccular aneurysms, lending support to the idea that genetic factors may play a role in their development 35
- 36. As an aneurysm develops, it typically forms a neck with a dome. At the site of rupture (most often the dome) the wall thins, and the tear that allows bleeding is often 0.5 mm long. Aneurysm size and site are important in predicting risk of rupture. Those >7 mm in diameter and Those at the top of the basilar artery and At the origin of the posterior communicating artery are at greater risk of rupture. 36
- 37. 37
- 39. The main symptom is a severe headache that starts suddenly (often called thunderclap headache). It is often worse near the back of the head. Many persons often describe it as the "worst headache ever" and unlike any other type of headache pain. The headache may start after a popping or snapping feeling in the head. Other symptoms: and alertness Eye discomfort in bright Mood and personality changes, including and irritability (especially Nausea and vomiting
- 40. often with neck stiffness, and vomiting is common 40
- 41. Pain at other sites Occipital and posterior cervical pain may signal a posterior inferior cerebellar artery (PICA) or anterior inferior cerebellar artery aneurysm. Pain in or behind the eye and in the low temple can occur with an expanding MCA aneurysm 41
- 42. Loss of consciousness At the moment of aneurysmal rupture with major SAH, the ICP suddenly rises. This may account for the sudden transient loss of consciousness that occurs in nearly half of patients which may be preceded by headache. In 10% of cases, aneurysmal bleeding is severe enough to cause loss of consciousness for several days. 42
- 43. meningismus neck stiffness photophobia back pain
- 44. Numbness in part of the body Stiff neck
- 46. focal neurologic deficits: oculomotor palsy hemiparesis ocular hemorrhage
- 47. What causes symptoms & signs? Blood leaking from the aneurysm Local pressure effects of the aneurysm Associated ICH Emboli
- 48. CLINICAL MANIFESTATIONS- cont. FOCAL NEUROLOGICAL DEFICITS Although sudden headache in the absence of focal neurologic symptoms is the hallmark of aneurysmal rupture, FOCAL NEUROLOGIC DEFICITS MAY OCCUR. Anterior communicating artery or MCA bifurcation aneurysms may rupture into the adjacent brain or subdural space and form a hematoma large enough to produce mass effect. The common deficits that result include hemiparesis, aphasia, and abulia (progressive drowsiness or slow mentation) 48
- 49. Anatomic – clinical corellation of focal neurological Deficits Third nerve palsy (ptosis, diplopia,dilatation of pupil & divergent squint) indicates an aneurysm at the junction of post. Comunicating &post. Cerebral arteries A sixth nerve palsy may indicate an aneurysm in the cavernous sinus .but uni or bilateral palsy could be because of raised ICP Unilateral blindness indicates aneurysm lying anteromedially in the circle of willis usually at the origin of opthalmic artery 49
- 50. Anatomic – clinical corellation of focal neurological Deficits- cont Transient paresis of one or both lower limbs indicates ant comunicating A. aneurysm that has interfered with circulation in ant. Cerebral arteries. Hemiperesis or aphasia suggests aneurysm at the first bifurcation of middle cerebral artery 50
- 51. 51 The side of aneurysmal rupture may be indicated by monocular pain unilateral preponderace of headache or unilateral preretinal(subhyaloid) hemorrhage (Terson Syndrome)
- 52. D/D Other conditions which may present as severe headache need to be differentiated, like:- Cerebral venous thrombosis, Diffuse vasospasm (call-flemming syndrome), Pituatry apoplexy, Hypertensive encephalopathy, Intracranial or extracranial arterial dissection CSF examination assumes great importance in differentiating these conditions from SAH 52
- 53. D/D- SAH to be differentiated from THUNDERCLAP HEADACHE is a variant of migraine that simulates a SAH. Headache of explosive onset may also be caused by ingestion of sympathomimetic drugs or ingestion of tyramine containg foods in a pt. who is taking MAO inhibitors Sudden severe headache may also be a symptom of phaeochromocytoma 53
- 54. D/D Before concluding that a patient with sudden, severe headache has thunderclap migraine or any other type of severe headache, a definitive workup for aneurysm is always required in the form of CT scan, Lumbar puncture, and if the diagnosis still remains doubtful, then cerebral angiography 54
- 55. DELAYED NEUROLOGIC DEFICITS There are four major causes of delayed neurologic deficits: 1. RERUPTURE/REBLEED, 2.HYDROCEPHALUS 3.VASOSPASM 4.HYPONATREMIA. 55
- 56. 2.HYDROCEPHALUS Acute hydrocephalus can cause stupor and coma and can be mitigated by placement of an external ventricular drain. More often, subacute hydrocephalus may develop over a few days or weeks and causes progressive drowsiness or slowed mentation (abulia) with incontinence.. It may clear spontaneously or require temporary ventricular drainage. 56
- 57. Hydrocephalus-cont. Chronic hydrocephalus may develop weeks to months after SAH and present as normal pressure hydrocephalus (NPH) manifested by gait difficulty, incontinence, or impaired mentation. Subtle signs may be a lack of initiative in conversation or a failure to recover independence 57
- 58. 3.VASOSPASM Causes symptomatic ischemia and infarction in ~30% of patients and is the major cause of delayed morbidity and death. Signs of ischemia appear 4–14 days after the hemorrhage, most often at 7 days. The severity and distribution of vasospasm determine whether infarction will occur. Vasospasm is believed to result from direct effects of clotted blood and its breakdown products on the arteries within the subarachnoid space. 58
- 59. VASOSPASM- cont. Spasm of major arteries produces focal symptoms referable to the appropriate vascular territory. All of these focal symptoms may present abruptly, fluctuate, or develop over a few days. In most cases, focal spasm is preceded by a decline in mental status. Patient may develop fluctuating hemiperisis or aphasia Severe cerebral edema in patients with infarction from vasospasm may increase the ICP enough to reduce cerebral perfusion pressure. 59
- 60. 4.HYPONATREMIA Hyponatremia. Hyponatremia may be profound and can develop quickly in the first 2 weeks following SAH. There is both natriuresis and volume depletion with SAH, so that patients become both hyponatremic and hypovolemic. Both atrial natriuretic peptide (ANP)and brain natriuretic peptide (BNP) have a role in producing this "cerebral salt-wasting syndrome.“ There may some role of antidiuretic hormone also, causing water retention Typically it clears over the course of 1–2 weeks and, in the setting of SAH, should not be treated with free-water restriction as this may increase the risk of stroke. 60
- 61. SYSTEMIC CHANGES ASSOCIATED WITH SAH ECG changes suggestive of subendicardial or myocardial ischemia Elevation of troponis/CPK (MB) levels In some patients cardiac dysfunction may be severe enough to cause fall in EF % and heart failure There is evidence that structural myocardial lesions produced by circulating catecholamines and excessive discharge of sympathetic neurons may occur after SAH, causing these ECG changes and a reversible cardiomyopathy sufficient to cause shock or congestive heart failure. Hyponatremia D. Insipidus Albuminuria, Glycosuria leukocytosis 61
- 63. NON CONTRAST CT SCAN. CT Scan is Initial investigative procedure The extent and location of subarachnoid blood on noncontrast CT scan help locate the underlying aneurysm, identify the cause of any neurologic deficit, and predict delayed vasospasm. A high incidence of symptomatic vasospasm in the MCA and ACA has been found when early CT scans show subarachnoid clots >5 x 3 mm in the basal cisterns or layers of blood >1 mm thick in the cerebral fissures. CT scans less reliably predict vasospasm in the vertebral, basilar, or posterior cerebral arteries. 63
- 64. More than 95% of cases have enough blood to be visualized on a high-quality NONCONTRAST CT SCAN obtained within 72 h. 64
- 65. CT scan reveals subarachnoid hemorrhage in the right sylvian fissure; no evidence of hydrocephalus is apparent.
- 66. (A)Noncontrast CT demonstrates subarachnoid hemorrhage (arrows). (B)3-D reconstruction image from a CT angiogram demonstrates an aneurysm (arrow) from the anterior communicating artery as the cause of the bleed.
- 67. IMAGING STUDIES-cont. Exact site of offending aneurysm can be inferred from the location of main clot in CT scan Collection of blood in the anterior inter-hemispheric fissure indicates rupture of an ant. Communicating artery Blood in sylvian fissure – middle cerebral artery Blood in ant. Perimesencephalic cistern- post. Communicating artery or distal basilar artery aneurysm MRI can also detect blood in the proton density sequence 67
- 68. Lab investigations-cont If the scan fails to establish the diagnosis of SAH and no mass lesion or obstructive hydrocephalus is found, Then a lumbar puncture should be performed to establish the presence of subarachnoid blood. Usually CSF becomes grossly bloody within 30 minutes of bleed with RBC counts upto 1 million/c mm or more Lysis of the red blood cells and subsequent conversion of hemoglobin to bilirubin stains the spinal fluid yellow within 6–12 h. This xanthochromic spinal fluid peaks in intensity at 48 h and lasts for 1–4 weeks, depending on the amount of subarachnoid blood 68
- 69. Angiography Once the diagnosis of hemorrhage from a ruptured saccular aneurysm is suspected, four-vessel conventional x-ray angiography (both carotids and both vertebrals) is generally performed to localize and define the anatomic details of the offending aneurysm and to determine if other unruptured aneurysms exist). CT angiography is an alternative method for locating the aneurysm and may be sufficient to plan definitive therapy. 69
- 70. Angiography-cont. in 5-10% pts with aneurysmal bleed , there may not be any evidence of aneurysmal rupture on angiography. It may be because in some cases obliteration of lesion occurs In some lesions were somewhat more benign Pts without evidence of an offending aneurysm or an arteriovenous malformationhave a better prognosis 70
- 71. Angiography-cont. Perimesencephalic hemorrhage also caries a better prognosis In this cisterns surrounding midbrain & upper pons gets filled up with blood Mild headache, no vasospasm Usually no aneurysm is found at the expected site i.e. at the top of basillary artery 71
- 72. Lab Inv. – cont. Close monitoring (daily or twice daily) of electrolytes is important because hyponatremia can occur precipitously during the first 2 weeks following SAH An asymptomatic troponin elevation is common. 72
- 73. ECG Changes The electrocardiogram (ECG) frequently shows ST- segment and T-wave changes similar to those associated with cardiac ischemia. Prolonged QRS complex, increased QT interval, and prominent "peaked" or deeply inverted symmetric T waves are usually secondary to the intracranial hemorrhage ( cerebral T waves). Serious ventricular dysrhythmias are unusual 73
- 74. 74
- 75. ECHO Echocardiography reveals a pattern of regional wall motion abnormalities that follow the distribution of sympathetic nerves rather than the major coronary arteries The sympathetic nerves themselves appear to be injured by direct toxicity from the excessive catecholamine release. 75
- 76. TREATMENT The medical management of SAH focuses on Protecting the airway, Managing blood pressure Preventing rebleeding prior to treatment, Managing vasospasm, Treating hydrocephalus, Treating hyponatremia, and Preventing pulmonary embolus. 76
- 77. Because rebleeding is common, all patients who are not candidates for early aneurysm repair are put on bed rest in a quiet room and are given stool softeners to prevent straining. If Headache or neck pain is severe, mild sedation and analgesia are prescribed. Extreme sedation is avoided because it can obscure changes in neurologic status. Adequate hydration is necessary to avoid a decrease in blood volume predisposing to brain ischemia. So adequate amount of fluid is administered so as to maintain above normal circulating blood volume & central venous pressure 77
- 78. Managing raised ICP Intracranial hypertension following aneurysmal rupture occurs secondary to subarachnoid blood, parenchymal hematoma, acute hydrocephalus, or loss of vascular autoregulation. Perilesional edema if infarct occurs 78
- 79. Managing raised ICP- cont. Patients who are stuporous should undergo emergent ventriculostomy to measure ICP and to treat high ICP in order to prevent cerebral ischemia. Medical therapies designed to combat raised ICP e.g., mild hyperventilation, mannitol, and sedation can also be used as needed. (Mannitol dose-25-100gm q4h) High ICP refractory to treatment is a poor prognostic sign 79
- 80. MANAGING BP Prior to definitive treatment of the ruptured aneurysm, care is required to maintain adequate cerebral perfusion pressure while avoiding excessive elevation/fall of arterial pressure. If the patient is alert, it is reasonable to lower the blood pressure to <150 systolic using nicardipine, labetolol, or esmolol. If the patient has a depressed level of consciousness, then ICP(Intracranial pressure) should be measured and the cerebral perfusion pressure targeted to 60–70 mmHg. 80
- 81. Managing Seizure Activity Seizures are uncommon at the onset of aneurysmal rupture. The quivering, jerking, and extensor posturing that often accompany loss of consciousness with SAH are probably related to the sharp rise in ICP or, perhaps, acute generalized vasospasm rather than seizure. Use of anti-seizure drugs is controvercial. However, phenytoin is often given as prophylactic therapy since a seizure may promote rebleeding. 81
- 82. MANAGING VASOSPASM Vasospasm remains the leading cause of morbidity and mortality following aneurysmal SAH. Treatment with the calcium channel antagonist nimodipine (60 mg PO every 4 h) improves outcome, perhaps by preventing ischemic injury Nimodipine can cause significant hypotension in some patients, which may worsen cerebral ischemia in patients with vasospasm 82
- 83. Managing Hydrocephalus Acute hydrocephalus can cause stupor or coma. It may clear spontaneously or require temporary external ventricular drainage. When chronic hydrocephalus develops, permanent ventricular shunting is the treatment of choice. 83
- 84. Role of Steroids Glucocorticoids may help reduce the head and neck ache caused by the irritative effect of the subarachnoid blood. There is no good evidence that they reduce cerebral edema, are neuroprotective, or reduce vascular injury, and Their routine use therefore is not recommended 84
- 85. Adjunctive Therapies and Measures Keep the patient's core body temperature at 37.2°C Consider antiemetics for nausea or vomiting. Elevate the head of the bed 30° to facilitate intracranial venous drainage. Emergent ventricular drainage by the neurosurgeon may be necessary. Maintain the patient's serum glucose level at 80-120 mg/dL; use sliding or continuous infusion of insulin if necessary. Fluids and hydration Do not over hydrate patients because of the risks of hydrocephalus. Patients with subarachnoid hemorrhage (SAH) may also have hyponatremia from cerebral salt wasting.
- 86. INTERVENTIONAL MANAGEMENT Early aneurysm repair prevents rerupture/rebleeding and allows the safe application of techniques to improve blood flow (e.g., induced hypertension and hypervolemia) An aneurysm can be "clipped" by a neurosurgeon or "coiled" by an endovascular surgeon. 86
- 87. 87 Hunt - Hess scale is helpful in assessing the patient before deciding for intervntional management
- 88. HUNT-HESS SCALE GRADE1: Mild headache, normal mental status, no cranial nerve or motor findings –(GCS* score 15, no motor deficits) GRADE 2: Severe headache, normal mental status, may have cranial nerve deficit –(GCS score 13–14, no motor deficits) GRADE 3: Somnolent, confused, may have cranial nerve or mild motor DEFICIT- (GCS SCORE 13–14, WITH MOTOR DEFICITS) GRADE 4 : Stupor, moderate to severe motor deficit, may have intermittent reflex posturing- (GCS score 7–12, with or without motor deficits) GRADE 5: Coma, reflex posturing or flaccid (GCS score 3–6, with or without motor deficits) 88
- 89. Management based on HH scaleGrades 1 & 2 Current approach is to go for intervention within 24 hrs This will prevent rebleed and will allow measures to be taken to improve cerebral circulation Grade 3 patients- if their condition allows , they too would be benefitted by the procedure Grade4- the outcome is generally poor but some times by putting a ventricular drain and improving the grade, pt89
- 90. 90 SURGICAL REPAIR •Involves placing a metal clip across the aneurysm neck, thereby immediately eliminating the risk of rebleeding. •This approach requires craniotomy and brain retraction, which is associated with neurologic morbidity.
- 91. 91 Endovascular techniques involve placing platinum coils, or other embolic material, within the aneurysm via a catheter that is passed from the femoral
- 92. . Endovascular techniques-CONT The aneurysm is packed tightly to enhance thrombosis and over time is walled-off from the circulation The benefit of endovascular therapy is durable. However, some aneurysms have a morphology that is not amenable to endovascular treatment. Thus, surgery remains an important treatment option But for aneurysms which are not approachable by surgery, endovascular technique would become the only choice 92
- 93. INTERNATIONAL SUBARACHNOID ANEURYSM TRIAL (ISAT) The only prospective randomized trial of surgery versus endovascular treatment for ruptured aneurysm, the International Subarachnoid Aneurysm Trial (ISAT), was terminated early when 24% of patients treated with endovascular therapy were dead or dependent at 1 year compared to 31% treated with surgery, a significant 23% relative reduction. After 5 years, risk of death was lower in the coiling group, Although the proportion of survivors who were independent was the same in both groups Risk of rebleeding was low, but more common in the coiling group 93
- 94. GRADE CT APPEARANCE 1 NONE 2 < 1mm thickness 3 > 1mm thickness 4 Diffuse with parenchymal/ventricular extension FISHERS GRADE CT APPEARANCE 0 NONE 1 MINIMAL 2 MINIMAL WITH IVH 3 THICK 4 THICK WITH IVH CLAASSENS MODIFICATION
- 95. GRADE GCS NEURODEFICIT 1 15 ABSENT 2 13-14 ABSENT 3 13-14 PRESENT 4 7-12 ABSENT/PRESENT 5 <7 ABSENT/PRESENT WORLD FEDERATION OF NEUROSURGEONS (WFNS)
- 96. GRADE CLINICAL PRESENTATION 1 CONSCIOUS 2 DROWSY 3 DROWSY WITH DEFICIT 4 MAJOR NEURODEFICIT 5 MORIBUND BOTTERELL ET AL
- 97. Discharge Plan Activity patient will need to have someone with for the next several days to watch for worsening of symptoms (see below) and to allow to rest. Start with light activity around the house for the first 3 days at home. Gradually increase activity starting with short walks 1-2 times per day. Avoid contact sports, skating, bike riding, or other such activities for 6 weeks. Encourage pt to do passive range of motion Nutrition : Instruct the relative to feed pt on time with proper food low in Na Low in cholesterol low in fat and give citrus fruits ,moderate in fluid intake and increase fiber diet to improve health..
- 98. Medications Take medications as prescribed and gradually decrease pain medications as pain improves. Instruct pt and their relative to follow medication regimen Educate and instruct the patient and her family to monitor BP and PR before giving medication Follow up with primary care physician for all medical issues.
- 99. Genetics of Intracranial Aneurysms Ref. Neurosurgery clinics of North America, July 1998, pp 485-493 Observations to suggest genetic involvement: Association of various heritable disorders with ICA The familial aggregation of ICA in the absence of known systemic disorder Heritable Disorders associated with ICA: Heritable CT disorder account for at least 5% of the cases of ICA True frequency may be higher due to variability in phenotypic expression and negative family history due to new mutation The most important ones are: Ehlers-Danlos type IV Marfan’s syndrome NF1 ADPKD
- 100. Ehlers-Danlos Syndrome Type IV Defeciency of collagen type 3 Mutation in the gene encoding for pro 1(III) chain of type III collagen Joint hypermobility, hyperelastic/fragile skin, abnormal scaring Type IV is least common and the most lethal Prevalence 1/50,000-500,000 Vascular catastrophes account for the great majority of deaths Clues to the diagnosis Facial appearance: thin nasal bridge, thin lips, lobeless ears, prematurely aged appearance Bruising tendency, MVP, spontaneous pneumothorax, abnormal scarring, varicose veins ICA: Prevalence?, 14 in 202 patient Saccular or fusiform, located in the cavernous sinus Thin walled, difficult to repair
- 101. Marfan’s syndrome Mutation in gene encoding fibrillin-1 (glycoprotein, major component of microfbrils in ECM and elastic tissues) Prevalence 1/10,000-20,000 Abnormalities of the skeleton, cardiovascular system, eyes, spinal meninges Variability in the phenotypic expression ICA: Saccular or fusiform, dissecting aneurysms Propensity to the proximal internal carotid artery Fragility of the connective tissue is not a major problem Ectasia and tortuosity of the vessels
- 102. Neurofibromatosis type 1 Mutation in NF1 gene encoding neurofibromin which may have regulatory role in the development of connective tissue Prevalence 1/3000-5000 Café-au-lait spot, lish nodule, neurofibroma Vascular complication; stenosis rupture, aneurysm, fistula ICA: Saccular or fusiform Vascular fragility, distorted anatomy Association with intracranial arterial occlusive disease
- 103. ADPKD Mutation in two genes PKD1 and PKD2 PKD1 linked disease is more severe Polycystin encoded by PKD1 is an integral membrane protein, play a role in the integrity of ECM of CT Most common monogenetic disorder Prevalence 1/400-1000 Cysts in kidney, liver, spleen, pancreas, ovaries Cardiovascular abnormalities: MVP, aortic and cervicocephalic dissection, coronary and AAA ICA: Saccular, fusiform, dissecting Vascular fragility Ruputre occurs in earlier age, increased risk of developing new ICA ICA in 25% of patient with ADPKD at autopsy, 10% on MRA Family screening with MRA yields ICA in 20-25% Cause of death in one-fifth ADPKD account for 2-7% of all ICA
- 104. Familial ICA First described by Chamber et al. In 1954 With the exception of ADPKD, Ehlers-Danlos IV, Pompe disease, Idiopathic nonarteriosclerotic cerebral calcification there is no association with heritable CT disease 7-20% of first or second-degree relatives of patient with SAH have ICA First-degree relatives of patient with SAH have twice to fivefold increase risk of having ICA First-degree relatives have threefold increased risk compared to second-degree relatives Inheritance pattern is unknown, most likely multifactorial, or AD
- 105. ICA: Rupture at younger age (5 year earlier), 71% has ruptured by age of 50 Vs 42% in nonfamilial ICA Anterior communicating artery aneurysms are underrepresented, MCA is overrepresented Rupture at smaller size Increase female preponderance Larger multiplicity Siblings are more likely to harbor aneurysms at the same side at mirror sites Severity of hemorrhage is similar to nonfamilial ones
- 106. Screening for familial ICA Why? Poor prognosis once ruptured Low surgical risk for the nonruptured (5% morbidity, 2% mortality) Caveat: aneurysms may develop over short period of time Indication for surgery for asymptomatic ICA is still unclear (critical size) Who? Families with two or more affected members Restricted to first-degree relatives (yield 9-29%) Monozygotic twin When? Screening between the ages of 35-65 Youngest patient with familial ICA is 6 years old De novo aneurysms occur at a rate of 2% per year Repeat screening at 6-month to 5-year intervals
- 107. Screening for familial ICA …/cont’d How? MRA is the most widely used Critical size for detection 3-5 mm Helical CT angiography Coventional angiography ICA gene Current approaches Screen the human genome for ICA gene by testing a large number of distinct highly pleomorphic genetic markers Analyze variations in the sharing of marker alleles among affected sibling pairs Candidate gene sequence analysis e.g., PKD1 or COL3A1
- 108. Heritable Disorders Associated with Intracranial Aneurysms Disorder Inheritance Pattern Locus Gene Gene Product Achondroplasia AD 4p16.3 FGFR3 Fibroblast growth factor receptor 3 Alkaptonuria AR 3q2 AKU ? ADPKD AD 16p13.3 PKD1 Polycystin Cohen syndrome AR 8q22 CHS1 ? Ehlers-Danlos Syndrome type I AD 9q COL5A1 Ollagen type V Ehlers-Danlos Syndrome type IV AD 2q31 COL3A1 Collagen type III Fabry disease AR XL-R Xq22.1 -galactosidase A Kahn syndrome AR ? ? ? Marfan’s syndrome AD 15q21.1 FBN1 Fibrillin-1 NF1 AD 17q11.2 NF1 Neurofibromin Noonan syndrome AD 12q22 NS1 ?
- 109. Heritable Disorders Associated with Intracranial Aneurysms …/cont’d Disorder Inheritance Pattern Locus Gene Gene Product Osler-Rendu- Weber disease AD 9q34.1 HHT1 Endoglin Osteogenesis imperfecta type 1 AD 17q22.1 COL1A1 Collagen type 1 Pompe disease AR 17q23 GAA -Glucosidase Pseudoxanthoma elasticum AD & AR ? ? ? Rambaud syndrome AR ? ? ? Tuberous sclerosis AD 9q34/16p13.3 TSC1/TSC2 ?/Tuberin Wermer syndrome AD 11q13 MEN1 ? 3M syndrome AR ? ? ? 1-Antitrypsin deficiency AcoD 14q32.1 P1 1-Antitrypsin
- 110. How well a patient with subarachnoid hemorrhage does depends on a number of different factors, including: Location and amount of bleeding Complications Older age and more severe symptoms can lead to a poorer outcome. People can recover completely after treatment. But some people die even with treatment. Prognosis:
- 112. TO SUM-UP SAH is a neurolgical emergency It is less common but an important cause of stroke(5%) saccular/berry aneurysmal rupture is the commonest cause of SAH Most common presenttion is an excruciating headache which needs to be differentiated from other causes of severe headache including thunderclap migrane CT scan is very helpful in making a dianosis and differentiating it from other headaches of severe intensity If CT is negative but there s strong suspecion of SAH then one should go for CSF examination If othe CT scan & CSF are inconclusive then cerebral angiography is the last resort Complications include rerupture, hydrocephalus, vasospasm and hyponatremia 112
- 113. 113 Management icludes – bed rest, maintaing a clear airway, managing BP, giving adequate amount of fluids, monitoring hyponatremia preventing vasospasm and instituting measures to lower ICP one third of patients are prone to develop rebleed which can be effectively taken care of by interventional modalities i.e. surgical (clipping)/ endovascular technique (coiling) Randomzed trial (ISAT) has shown coiling to superior to clipping
- 114. References MS Greenberg. Handbook of Neurosurgery. Seventh Edition. New York: Thieme Medical Publishers; 2010. AH Kaye. Essential Neurosurgery. Third Edition. Oxford: Blackwell Publishing Ltd; 2005. MG Yasargil. Microneurosurgery. New York: Thieme Medical Publishers Inc; 1994. Zivin J. Hemorrhagic cerebrovascular disease. In: Goldman L, Schafer AI, eds. Goldman's Cecil Medicine. 24th ed. Philadelphia, PA: Elsevier Saunders; 2011:chap 415. http://www.strokecenter.org/professionals/brain- anatomy/blood-vessels-of-the-brain/
- 115. References: Naggara ON, White PM, Guilbert F, et al. Endovascular treatment of intracranial unruptured aneurysms: systematic review and meta-analysis of the literature on safety and efficacy. Radiology. 2010;256:887-897. Reinhardt MR. Subarachnoid hemorrhoid. J Emerg Nurs. 2010;36:327-329. Tateshima S, Duckwiler G. Vascular diseases of the nervous system: intracranial aneurysms and subarachnoid hemorrhage. In: Daroff RB, Fenichel GM, Jankovic J, Mazziotta JC. Bradley’s Neurology in Clinical Practice. 6th ed. Philadelphia, PA: Elsevier Saunders; 2012:chap 51C.
- 116. . Avoiding Pitfalls in the Diagnosis of Subarachnoid Hemorrhage. JA Edlow and LR Caplan. N Engl J Med 342:29-36, 2000 . Unruptured Intracranial Aneurysms - Risk of Rupture and Risks of Surgical Intervention. ISUIA Investigators. N Engl J Med; 339: 1725- 33, 1998 . Intracranial Aneurysms and Subarachnoid Hemorrhage: An Overview. B Weir and RL Macdonald. Chapter 214 (pp 2191-2213) in Neurosurgery, 2nd edition, volume II, 1996, editors RH Wilkins and SS Rengachary, published by McGraw-Hill . Relation of Cerebral Vasospasm to Subarachnoid Hemorrhage Visualized by Computerized Tomographic Scanning. CM Fisher JP Kistler and JM Davis. Neurosurgery, 6:1-9, 1980 . Factors Influencing the Outcome of Aneurysm Rupture in Poor Grade Patients: A Prospective Series. L Disney, B Weir, M Grace et al Neurosurgery 23: 1-9 1988
- 117. Thank you!
