Cancer of Prostate- Easy PPT for Nursing Students
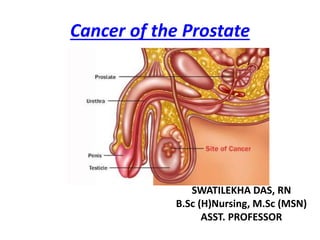
- 1. Cancer of the Prostate SWATILEKHA DAS, RN B.Sc (H)Nursing, M.Sc (MSN) ASST. PROFESSOR
- 2. Cancer of Prostate • Cancer of the prostate is the most common cancer in men (other than non-melanoma skin cancer) and is the second most common cause of cancer deaths in American men. • African American men are twice as likely than men of any other racial or ethnic group to die of prostate cancer.
- 4. Risk factors • Risk factors include increasing age, a family history, and possibly a high-fat diet. Endogenous hormones, such as androgens and estrogens, also may be associated with the development of prostate cancer.
- 5. Clinical Manifestations • Usually asymptomatic in early stage • Nodule felt within the substance of the gland or extensive hardening in the posterior lobe Advanced Stage • Lesion is stony hard and fixed. • Obstructive symptoms occur late in the disease: difficulty and frequency of urination, urinary retention, decreased size and force of urinary stream.
- 6. Cont. • Blood in urine or semen; painful ejaculation. • Cancer can spread to lymph nodes and bone. • Symptoms of metastases include backache, hip pain, per rectal discomfort, anemia, weight loss, weakness, nausea, oliguria, and spontaneous pathologic fractures; hematuria may result from urethral or bladder invasion. • Sexual dysfunction.
- 7. Assessment and Diagnostic Methods • Digital rectal examination (DRE; preferably by the same examiner). • The diagnosis is confirmed by a histologic examination of tissue removed surgically by transurethral resection of the prostate (TURP), open prostatectomy, ultrasound-guided transrectal needle biopsy, or fine- needle aspira-tion. • Prostate-specific antigen (PSA) level; transrectal ultra- sound; bone scans, skeletal x-rays, and MRI; pelvic CT scans; or monoclonal antibody-based imaging may also be used.
- 8. Medical Management • Treatment is based on the patient’s life expectancy, symptoms, risk of recurrence after definitive treatment, size of the tumor, Gleason score, PSA level, likelihood of complications, and patient preference. Management can range from nonsurgical methods that involve “watchful waiting” to surgery (eg, prostatectomy).
- 9. Radical Prostatectomy • Removal of the prostate, seminal vesicles, tips of the vas deferens, and often the surrounding fat, nerves, and blood vessels through suprapubic approach (greater blood loss), perineal approach (easily contaminated, incontinence, impotence, and rectal injury common), or retropubic approach (infection can readily start). • This procedure is used with patients whose tumor is con-fined to the prostate. • Sexual impotency and various degrees of urinary incontinence commonly follow radical prostatectomy.
- 10. Radiation Therapy • Teletherapy (external beam radiation therapy [EBRT]): treatment option for patients with low risk prostate cancer • Brachytherapy (internal implants): commonly used mono- therapy treatment option for early, clinically organ-confined prostate cancer
- 11. Hormone Therapy • Androgen deprivation therapy (ADT): accomplished either by surgical castration (bilateral orchiectomy, removal of the testes) or by medical castration with the administration of medications, such as luteinizing hormone–releasing hormone (LHRH) agonists.
- 12. Other Therapies • Chemotherapy • Cryosurgery for those who cannot physically tolerate surgery or for recurrence • Repeated TURPs to keep urethra patent; suprapubic or transurethral catheter drainage when repeated TUR is impractical • Opioid or nonopioid medications to control pain with metastasis to bone • Blood transfusions to maintain adequate hemoglobin levels
