7. tpn for critically ill patients
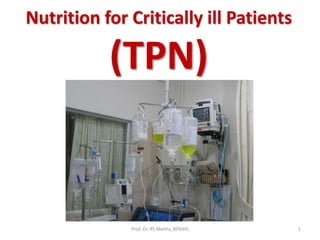
- 1. Nutrition for Critically ill Patients (TPN) 1Prof. Dr. RS Mehta, BPKIHS
- 2. Nutrition • Nutrition allows the body to be provided with all basic nutrients substrates and energy required for maintaining or restoring all vital body functions from carbohydrate and fat and for building up body mass from amino acid. 2Prof. Dr. RS Mehta, BPKIHS
- 3. Clinical Manifestations: Malnutrition • Weight loss • Reduced basal metabolism • Depletion skeletal muscle and adipose (fat) stores • Decrease tissue turgor • Bradycardia • Hypothermia 3Prof. Dr. RS Mehta, BPKIHS
- 4. 4Prof. Dr. RS Mehta, BPKIHS
- 5. 5Prof. Dr. RS Mehta, BPKIHS
- 6. Total Parentral Nutrition 6Prof. Dr. RS Mehta, BPKIHS
- 7. Total Parenteral Nutrition Indication • When normal oral feeding is not possible. e.g.: Chron’s disease, gastric & esophageal carcinoma, paralytic ileus, generalized peronitis, GI. obstruction, intractable vomiting. • When food is incompletely absorbed. e.g.: Major burns, multiple injuries, radiation therapy, ulcerative colitis, chemotherapy treatment, short bowel syndrome. • When food intake is undesirable, in case it is prudent to rest the bowel. e.g.: Post GIT surgery, chronic inflammatory diseases, intractable diarrhea. 7Prof. Dr. RS Mehta, BPKIHS
- 8. Total Parenteral Nutrition Indication • In patients who are able to ingest food, but refuse to do so. e.g.: Geriatric post-operative patients, adolescents with anorexia nervosa, some psychiatric patients with prolonged depression. • In patients who, as a consequence of their illness are going to be, or have been NPO for 5 – 7 days. 8Prof. Dr. RS Mehta, BPKIHS
- 9. Indications for TPN Short-term use • Bowel injury, surgery, major trauma or burns • Bowel disease (e.g. obstructions, fistulas) • Severe malnutrition • Nutritional preparation prior to surgery. • Malabsorption - bowel cancer • Severe pancreatitis • Malnourished patients who have high risk of aspiration Long-term use (HOME PN) • Prolonged Intestinal Failure • Crohn’s Disease • Bowel resection 9Prof. Dr. RS Mehta, BPKIHS
- 10. Parenteral Nutrition Central Nutrition • Subclavian line • Long period • Hyperosmolar solution • Full requirement • Minimum volume • Expensive • More side effect Peripheral nutrition • Peripheral line • Short period < 14days • Low osmolality < 900 mOsm/L • Min. requirement • Large volume • Thrombophlebitis 10Prof. Dr. RS Mehta, BPKIHS
- 11. Routes of TPN Central TPN (usual osmolarity = 2000 mosmol/L) Advantages: Can provide full nutritional support (No limits in concentration of dextrose and amino acids) No risk of thrombophlebitis, No pain. Disadvantages: Requires surgery More risk of sepsis than peripheral TPN High risk of mechanical complications 11Prof. Dr. RS Mehta, BPKIHS
- 12. Routes of TPN Peripheral TPN maximum osmolarity; neonates = 1100/L, Pediatrics = 1000/L, Adults = 900/L Advantages: Does not require surgery Less risk of sepsis than central TPN No risk of mechanical complications Disadvantages: High risk of thrombophlebitis Painful Does not provide full nutrition support. Needs more fluids to provide more nutrition. (maximum dextrose = 7.5% and AA = 2.5%). 12Prof. Dr. RS Mehta, BPKIHS
- 13. Note PPN can infuse through central line but central TPN can NOT infuse through the peripheral line 13Prof. Dr. RS Mehta, BPKIHS
- 14. Prof. Dr. RS Mehta, BPKIHS Calculating the Osmolarity of a Parenteral Nutrition Solution Multiply the grams of dextrose per liter by 5. Example: 100 g of dextrose x 5 = 500 mOsm/L Multiply the grams of protein per liter by 10. Example: 30 g of protein x 10 = 300 mOsm/L Multiply the (mEq per L sodium + potassium + calcium + magnesium) X 2 Example: 80 X 2 = 160 Total osmolarity = 500 + 300 + 160 = 960 mOsm/L 14
- 15. Parenteral Nutrition • Peripheral Parenteral Nutrition (15 lit D5W/day for a 70 kg !!!) • Central Parenteral Nutrition (TPN) – Needs CV-line to administer hyperosmolar solutions 15Prof. Dr. RS Mehta, BPKIHS
- 16. Estimation of energy expenditure Harris-Benedict equations: • BEE (men) (kcal/day): 66.47+13.75W+5H-6.76A • BEE (women) (kcal/day): 655.1+9.56W+1.85H-4.68A • TEE (kcal/day): BEE × Stress factor × Activity factor • Stress factors: Surgery, Infection: 1.2 Trauma: 1.5 Sepsis: 1.6 Burns: 1.6-2 • Activity factors: sedentary: 1.2 , normal activity: 1.3, active: 1.4 , very active: 1.5 16Prof. Dr. RS Mehta, BPKIHS
- 17. Stress level • Normal/mild stress level: 20-25 kcal/kg/day • Moderate stress level: 25-30 kcal/kg/day • Severe stress level: 30-40 kcal/kg/day Pregnant women in second or third trimester: Add an additional 300 kcal/day 17Prof. Dr. RS Mehta, BPKIHS
- 18. Fluid: mL/day • 30-40 mL/kg 19Prof. Dr. RS Mehta, BPKIHS
- 19. Protein (amino acids) • Maintenance: 0.8-1 g/kg/day • Normal/mild stress level: 1-1.2 g/kg/day • Moderate stress level: 1.2-1.5 g/kg/day • Severe stress level: 1.5-2 g/kg/day • Burn patients (severe): Increase protein until significant wound healing achieved • Solid organ transplant: Perioperative: 1.5-2 g/kg/day 20Prof. Dr. RS Mehta, BPKIHS
- 20. Protein need in Renal failure • Acute (severely malnourished or hypercatabolic): 1.5-1.8 g/kg/day • Chronic, with dialysis: 1.2-1.3 g/kg/day • Chronic, without dialysis: 0.6-0.8 g/kg/day • Continuous hemofiltration: ≥ 1 g/kg/day 21Prof. Dr. RS Mehta, BPKIHS
- 21. Protein need in Hepatic failure • Acute management when other treatments have failed: – With encephalopathy: 0.6-1 g/kg/day – Without encephalopathy: 1-1.5 g/kg/day • Chronic encephalopathy – Use branch chain amino acid enriched diets only if unresponsive to pharmacotherapy • Pregnant women in second or third trimester – Add an additional 10-14 g/day 22Prof. Dr. RS Mehta, BPKIHS
- 22. Fat • Initial: 20% to 40 % of total calories (maximum: 60% of total calories or 2.5 g/kg/day) – Note: Monitor triglycerides while receiving intralipids. • Safe for use in pregnancy • I.V. lipids are safe in adults with pancreatitis if triglyceride levels <400 mg/dL 23Prof. Dr. RS Mehta, BPKIHS
- 23. Components of TPN Formulations Macro: Calorie: Dextrose 20%, 50% Intralipid 10%, 20% Protein: Aminofusion 5%, 10% Micro: Electrolytes (Na, K, Mg, Ca, PO4) Trace elements (Zn, Cu, Cr, Mn, Se) 24Prof. Dr. RS Mehta, BPKIHS
- 24. Dextrose • 20%, 50% ( from CV-line) • 3.4 kcal/g • 60-70% of calorie requirements should be provided with dextrose 25Prof. Dr. RS Mehta, BPKIHS
- 25. Dextrose: Contraindications • Hypersensitivity to corn or corn products • Hypertonic solutions in patients with intracranial or intra-spinal hemorrhage 26Prof. Dr. RS Mehta, BPKIHS
- 26. Abrupt withdrawal • Infuse 10% dextrose at same rate and monitor blood glucose for hypoglycemia 27Prof. Dr. RS Mehta, BPKIHS
- 27. Monitoring 28Prof. Dr. RS Mehta, BPKIHS
- 28. Prof. Dr. RS Mehta, BPKIHS Monitoring • Avoid overfeeding • Avoid respiratory problem • Promote nitrogen retention • Triglyceride clearance • Fluid and electrolyte • Weight • Liver function 29
- 29. Complications of TPN 30Prof. Dr. RS Mehta, BPKIHS
- 30. Prof. Dr. RS Mehta, BPKIHS Complication • Mechanical: occlusion, catheter removal, improper rate, thromboses, pneumothorax. • Infection: catheter related • Metabolic: re-feeding syndrome, hyperglycemia, fluid & electrolyte disturbance • Organic system: hepatobiliary complication, respiratory, cardiovascular, renal 31
- 31. 32Prof. Dr. RS Mehta, BPKIHS
- 32. Prof. Dr. RS Mehta, BPKIHS Transitional Feeding • Maintain full PN support until pt is tolerating 1/3 of needs via enteral route • Decrease TPN by 50% and continue to taper as the enteral feeding is advanced to total • TPN can reduce appetite if >25% of calorie needs are met via PN • TPN can be tapered when pt is consuming greater than 500 calories/d and d-c’d when meeting 60% of goal • TPN can be rapidly decreased if pt is receiving enteral feeding in amount great enough to maintain blood glucose levels 33
- 33. TPN • Doctors decide patient needs it • Dietitian sees patient • Decides best regime • Orders bag from pharmacy • Made up aseptically to requirements • Start low and build up • Monitor bloods 34Prof. Dr. RS Mehta, BPKIHS
- 34. Access for PN • Usually central line in ICU – keep a clean port if PN may be needed. 5 lumen • Short term PN – can have PIC (need a different formula) or PICC • Long-term TPN – tunnelled subclavian catheter (Hickman) or subcutaneous port is usually inserted – OBSERVE STRICT ASEPSIS if handling these lines. 35Prof. Dr. RS Mehta, BPKIHS
- 35. 36Prof. Dr. RS Mehta, BPKIHS
- 36. Overfeeding • Lactic acidosis • Hyperglycaemia • Increased infections • Liver impairment (Alk phos, ALT, GGT, acalculous cholecystitis) • Persistent pyrexia 37Prof. Dr. RS Mehta, BPKIHS
- 37. Complex nutrition: Monitoring • Urea, Electrolytes, phosphate, calcium, magnesium • Glucose • LFTs • Fluid balance • Haematology • Weight • Trace elements if long-term 38Prof. Dr. RS Mehta, BPKIHS
- 38. Conclusion • Do not forget about feeding • Keep an eye on whether nutritional targets are being met • Speak to the surgeons and dietician • Do not be reluctant to start PN in a supplemental capacity • Avoid hyperglycaemia • Nutrition is often neglected 39Prof. Dr. RS Mehta, BPKIHS
- 39. Thank you Prof. Dr. RS Mehta, BPKIHS 40
- 40. 41Prof. Dr. RS Mehta, BPKIHS
