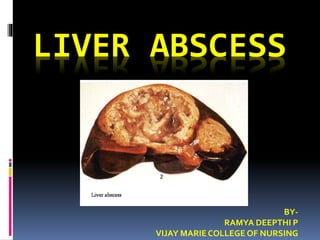
Liver abscess
- 1. LIVER ABSCESS BY- RAMYA DEEPTHI P VIJAY MARIE COLLEGE OF NURSING
- 2. INTRODUCTION Liver abscess are more common in developing countries. Majority of them are due to parasitic infestations- amoebic, echinococcosis. It is rarely seen in developed countries.
- 3. Etiology I. Bacterial infections a. Pyogenci liver abscess b. Pyophlebitis abscess c. Cholangitic abscess II. Parasitic infestations A. Protozoal disease a. Amoebiasis b. Malaria c. Kala azar B. Helmenthic disease a. Ascariasis b. Liver flukes c. Echinococcosis (Hydatid disease) C. Leptospirosis D. Syphilis
- 4. PYOGENIC LIVER ABSCESS Most liver abscess re of bacterial in origin. Infecting organisms are- 1. Garm negative bacteria- E. Coli, Pseudomonas Klebsiella, enetrobacter Route of entry to liver are- a. Portal vein b. Arterial supply c. Ascending infection from biliary tract d. Direct invasion of liver from nearby source e. Penetrating injury f. Cryptogenic (unknown)
- 5. Morphology Gross: Depends on the cause of pyogenic liver abscess Abscess may be single or multiple Vary in size from few millimeters to massive lesion If single, abscess is usually walled off by a thick fibrous capsule.
- 6. Microscopic changes Multiple neutorphilic abscess with areas of necrosis are seen n the liver parenchyma. Adjacent area shows pus, inflammation, congestion and proliferating fibroblasts Causative organism can be occasionally identified with special strains or when material is cultured.
- 7. Clinical features Pain in liver origin- right upper quadrant Fever Tenderness Hepatomegaly Rarely jaundice Investigations reveal raised total leukocyte count with neutrophilia Elevated serum liver enzyme levels Positive blood cultures.
- 8. II. AMOEBIC LIVER ABSCESS AMOEBIC LIVER ABSCESS IS MORE COMMON IN DEVELOPING COUNTRIES. However it is not as common as pyogenic abscess. Pathogenesis is caused by Entamoeba Histolytica. It spreads form intestinal lesions Parasite occurs in 2 forms-Trophozoite and cystic form. Cysts are more infective stages of the parasite and are found in contaminated water and food.
- 9. GROSS APPEARANCE: Amoebic liver abscess are solitary, often found in the right hepatic lobe. Multiple abscess are found only in advanced cases. Size of abscess vary Centre part of abscess contains necrotizing area filled with reddish brown, thick pus which resembles anchovy or chocolate sauce.
- 10. MICROSCOPIC CHANGES: Necrotic area consists of degenerated hepatocytes, inflammatory cell infiltarte, red blood cells, strands of connective tissue and necrotic debris. Trophozoites of amoebae are usually found in the necrotic area especially at the margins These cells resemble foamy macrophages and at times becomes difficult to distinguish them from macrophages.
- 11. Complications of amoebic abscess Large abscess may rupture, penetrate the diaphragm and enter into lung Rupture into pleural cavity , peritoneal cavity or pericardia sac.
- 12. III. HYDATID DISEASE Hydatid disease is caused by the larval stage of small tapeworm Echinococcus Granulosis. It is common in sheep and occur in humans with close contact with them. Dog is the definite host. Sheep, cattle and humans are intermediate hosts.
- 13. Pathogenesis Man acquires this infection by eating contaminated vegetables or water and those handling dogs. The embryo is liberated form the ovum in the small intestine of man. It gains access to blood stream and are carried to the liver by portal veins. These are trapped in liver where they grown into cysts. This cyst grows very slowly, may rupture giving multiple cysts and spreads to distant parts of the body.
- 14. Clinical features Uncomplicated hydatid disease remains for longer time silently and may produce only dull ache in the liver region.
- 15. Morphology Hydatid cyst grows slowly and may reach a size of 10cm in few years. a. Outer pericyst or adventitia: Has fibroblastic proliferation, esinophils and giant cells. It later forms as thick fibrous capsule b. Intermediate ecto cyst: Which is composed of acellular laminated hyaline material c. Inner endo cyst: it is the innermot germinal layer consisting of daughter cysts and hooklets which projects into lumen.
- 16. complications Rupture of cyst into peritoneal cavity, bile ducts and lungs causes anaphylactic reaction Fine needle aspiration is an absolute contraindication INVESTIGATIONS Peripheral blood smear X-ray examination serology
- 17. Thank you…
