SIES 2008
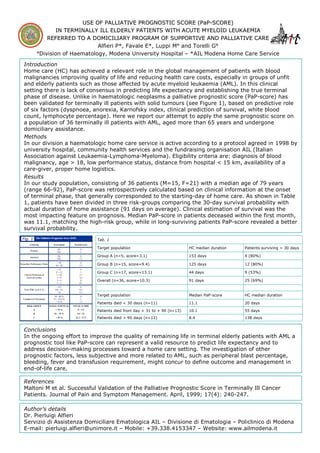
- 1. USE OF PALLIATIVE PROGNOSTIC SCORE (PaP-SCORE) (PaP- IN TERMINALLY ILL ELDERLY PATIENTS WITH ACUTE MYELOID LEUKAEMIA REFERRED TO A DOMICILIARY PROGRAM OF SUPPORTIVE AND PALLIATIVE CARE CARE Alfieri P*, Favale E*, Luppi M° and Torelli G° °Division of Haematology, Modena University Hospital – *AIL Modena Home Care Service Introduction Home care (HC) has achieved a relevant role in the global management of patients with blood malignancies improving quality of life and reducing health care costs, especially in groups of unfit and elderly patients such as those affected by acute myeloid leukaemia (AML). In this clinical setting there is lack of consensus in predicting life expectancy and establishing the true terminal phase of disease. Unlike in haematologic neoplasms a palliative prognostic score (PaP-score) has been validated for terminally ill patients with solid tumours (see Figure 1), based on predictive role of six factors (dyspnoea, anorexia, Karnofsky index, clinical prediction of survival, white blood count, lymphocyte percentage). Here we report our attempt to apply the same prognostic score on a population of 36 terminally ill patients with AML, aged more than 65 years and undergone domiciliary assistance. Methods In our division a haematologic home care service is active according to a protocol agreed in 1998 by university hospital, community health services and the fundraising organisation AIL (Italian Association against Leukaemia-Lymphoma-Myeloma). Eligibility criteria are: diagnosis of blood malignancy, age > 18, low performance status, distance from hospital < 15 km, availability of a care-giver, proper home logistics. Results In our study population, consisting of 36 patients (M=15, F=21) with a median age of 79 years (range 66-92), PaP-score was retrospectively calculated based on clinical information at the onset of terminal phase, that generally corresponded to the starting-day of home care. As shown in Table 1, patients have been divided in three risk-groups comparing the 30-day survival probability with actual duration of home assistance (91 days on average). Clinical estimation of survival was the most impacting feature on prognosis. Median PaP-score in patients deceased within the first month, was 11.1, matching the high-risk group, while in long-surviving patients PaP-score revealed a better survival probability. Fig. 1 Tab. 1 Target population HC median duration Patients surviving > 30 days Group A (n=5, score=3.1) 153 days 4 (80%) Group B (n=15, score=9.4) 125 days 12 (80%) Group C (n=17, score=13.1) 44 days 9 (53%) Overall (n=36, score=10.3) 91 days 25 (69%) Target population Median PaP-score HC median duration Patients died < 30 days (n=11) 11.1 20 days Patients died from day + 31 to + 90 (n=13) 10.1 55 days Patients died > 90 days (n=12) 8.4 138 days Conclusions In the ongoing effort to improve the quality of remaining life in terminal elderly patients with AML a prognostic tool like PaP-score can represent a valid resource to predict life expectancy and to address decision-making processes toward a home care setting. The investigation of other prognostic factors, less subjective and more related to AML, such as peripheral blast percentage, bleeding, fever and transfusion requirement, might concur to define outcome and management in end-of-life care. References Maltoni M et al. Successful Validation of the Palliative Prognostic Score in Terminally Ill Cancer Patients. Journal of Pain and Symptom Management. April, 1999; 17(4): 240-247. Author’s details Dr. Pierluigi Alfieri Servizio di Assistenza Domiciliare Ematologica AIL – Divisione di Ematologia – Policlinico di Modena E-mail: pierluigi.alfieri@unimore.it – Mobile: +39.338.4153347 – Website: www.ailmodena.it