Case Presentation: Pancreatic Clinical Chemistry Abnormalities
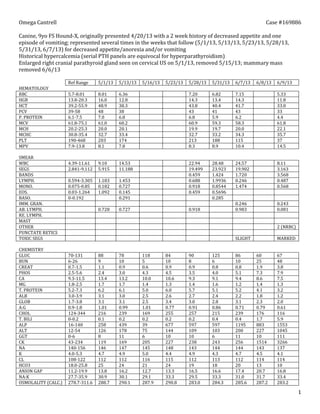
- 1. 1 Canine, 9yo FS Hound-X, presented 4/20/13 with a 2 week history of decreased appetite and one episode of vomiting; represented several times in the weeks that follow (5/1/13, 5/13/13, 5/23/13, 5/28/13, 5/31/13, 6/7/13) for decreased appetite and/or vomiting Historical hypercalcemia (serial PTH panels are equivocal for hyperparathyroidism) Enlarged right cranial parathyroid gland seen on cervical US on 5/1/13, removed 5/15/13 Mild ventral edema noted throughout hospitalization. 5/1/13 5/13/13 5/16/13 5/23/13 5/28/13 5/31/13 6/7/13 6/8/13 6/9/13 HEMATOLOGY RBC 8.01 6.36 7.20 6.82 7.15 5.33 HGB 16.0 12.8 14.3 13.4 14.3 11.8 HCT 48.9 38.3 43.8 40.4 41.7 33.0 PCV 48 38 43 41 43 33 P. PROTEIN 7.0 6.8 6.8 5.9 6.2 4.4 MCV 61.0 60.2 60.9 59.3 58.3 61.8 MCH 20.0 20.1 19.9 19.7 20.0 22.1 MCHC 32.7 33.4 32.7 33.2 34.3 35.7 PLT 203 174 213 188 115 37 MPV 8.1 7.8 8.3 8.9 10.4 14.5 SMEAR WBC 9.10 14.53 22.94 28.48 24.57 8.11 SEGS 5.915 11.188 19.499 23.923 19.902 3.163 BANDS 0.459 1.424 1.720 3.568 LYMPH. 1.183 1.453 0.688 1.9936 0.246 0.487 MONO. 0.182 0.727 0.918 0.8544 1.474 0.568 EOS. 1.092 0.145 0.459 0.5696 BASO. 0.291 0.285 IMM. GRAN. 0.246 0.243 AB. LYMPH. 0.728 0.727 0.918 0.983 0.081 RE. LYMPH. MAST OTHER 2 (NRBC) PUNCTATE RETICS TOXIC SEGS SLIGHT MARKED CHEMISTRY GLUC 88 78 118 84 90 125 86 60 67 BUN 9 10 5 10 8 6 10 25 48 CREAT 1.1 0.9 0.6 0.9 0.9 0.8 0.8 1.9 3.8 PHOS 2.4 3.0 4.3 4.5 3.5 4.0 5.1 7.3 7.9 CA 13.4 13.2 10.0 10.6 9.3 9.1 9.4 8.6 7.5 MG 1.7 1.7 1.4 1.3 1.4 1.6 1.2 1.4 1.3 T. PROTEIN 6.2 6.1 5.0 6.0 5.7 5.1 5.2 4.1 3.2 ALB 3.1 3.0 2.5 2.6 2.7 2.4 2.2 1.8 1.2 GLOB 3.1 3.1 2.5 3.4 3.0 2.8 3.1 2.3 2.0 A:G 1.01 0.99 1.01 0.77 0.91 0.86 0.71 0.79 0.61 CHOL 216 239 169 255 257 215 239 176 116 T. BILI 0.1 0.2 0.2 0.2 0.2 0.4 0.4 1.7 5.9 ALP 258 439 39 677 597 597 1195 883 1553 ALT 126 178 75 144 109 103 200 227 1045 GGT 8 11 6 10 10 6 11 10 111 CK 119 169 205 227 238 243 256 1514 3266 NA 146 147 145 148 143 144 144 143 137 K 4.7 4.9 5.0 4.4 4.9 4.3 4.7 4.5 4.1 CL 112 112 116 115 112 113 112 114 114 HCO3 25 24 21 24 19 18 20 13 10
- 2. 2 ANION GAP 13.8 16.2 12.7 13.3 16.5 16.6 17.4 20.7 16.8 NA:K 30.9 30.1 29.1 33.3 29.5 33.3 31.0 31.7 33.4 OSMOLALITY (CALC.) 288.7 290.1 287.9 290.8 283.0 284.3 285.6 287.2 283.2 AMY 1011 1229 1008 1358 1373 1151 1235 1723 1042 LIP 4440 6120 4800 7240 7860 8040 9780 14500 18380 OTHER TESTS PLI >1000 850 PT 19.9 APTT >120 DIMER >5000 PLATELET 37 FIBRINOGEN 200 K9INR 3.00 Hypercalcemia is present initially, and resolves following parathyroidectomy, trending towards and eventually resulting in hypocalcemia at the end of the patient’s hospitalization. Mild hypomagnesemia is present on all chemistry panels performed. Hypercalcemia is likely due to hyperparathyroidism, and resolves accordingly following parathyroidectomy. Hypomagnesia is likely due to hypercalcemia initially, as elevated calcium inhibits renal reabsorption of Mg. Persistent hypomagnesemia prior to and following parathyroidectomy may be due to a third space syndrome (likely the result of persistent hypoalbuminemia). Hypomagnesemia may be the cause of hypocalcemia, as Mg is needed for the synthesis and release of PTH, and thus hypomagnesemia may eventually result in a secondary hypocalcemia. There is increased ALP activity, total bilirubin, and GGT, indicating cholestasis. An elevating trend of these values indicates that cholestasis is worsening throughout the course of the patient’s hospitalizations. A trending increase in ALT activity suggests hepatocellular injury. As with cholestasis, it appears that hepatocellular injury is worsening throughout the patient’s hopsitalizations (particularly the last three days), due to a marked increase in these values in the last days of hospitalization. Amylase is normal or mildly elevated during hospitalization, while lipase has a worsening trend of severe elevation (4440-18380; RR 12-147 IU/L). This may be due to a pancreatic lesion or primary renal failure. Given that BUN and creatinine remain within normal limits (until the last two days of hospitalization), renal failure is an unlikely cause. Additionally, elevated PLI is diagnostic for pancreatitis. However, urinalyses were not performed during hospitalization, thus USG is not available and primary renal failure cannot be entirely ruled out. Hypoalbuminemia is persistent beginning 5/16/13, with a worsening trend noted over the duration of hospitalization. This may be due to loss as a result of protein-losing enteropathy and/or nephropathy (PLE/PLN), and/or liver disease/failure. Concurrent increased ALT activity indicates some degree of hepatocellular injury, lending support to liver disease/failure being the cause of hypoalbuminemia. From 5/28/13-6/7/13, there is a moderate leukocytosis with a moderate neutrophilia and degenerate left shift, as well as an monocytosis. A moderate lymphopenia is noted on 6/7/13. These changes are consistent with an inflammatory response with a stress component. On 6/9/13, leukocytes are within normal limits, and neutrophils are in the low normal range. However, a degenerative left shift is still present, as bands outnumber neutrophils, and there are a marked amount of toxic neutrophils present. Additionally, a mild normocytic, normochromic anemia and severe thrombocytopenia are present. Together, these parameters indicate that a severe, overwhelming inflammatory response is present, and gives the patient a guarded to poor prognosis. A coagulation panel on 6/9/13 reveal a markedly elevation of PT, APTT, and D-dimers. This indicates that there are decreased coagulation factors, and there are likely abnormalities in all arms of the coagulation cascade (intrinsic, extrinsic, and/or common pathways). Markedly elevated D-dimers indicates that disseminated intravascular
- 3. 3 coagulation (DIC) is present. Alone, this gives the patient a poor prognosis, and when combined with other hematological and chemical abnormalities, gives the patient a grave prognosis. Hypoglycemia, elevated BUN, creatine, and phosphorus, mild decrease in bicarbonate (indicating metabolic acidosis), as well marked changes in all enzymes of the chemistry panel, combined with hematological parameters and the coagulation panel indicate that the patient has severe disease in the pancreas, and is likely experiencing a septic event. The most likely explanation is that, in addition to chronic pancreatitis, the patient is suffering from a pancreatic adenocarcinoma (based on ultrasonographic appearance of the pancreas, as well as lymph nodes that were biopsied and found to be devoid of lymphoid tissue but with many neoplastic cells), with widespread metastatic multiorgan metastasis. This is may have served as the trigger for DIC and vascular injury. Other tests that could have been performed during hospitalization include: Urinalysis and UPC to rule out primary renal failure as a cause for elevated BUN and creatinine, as well as elevated amylase and lipase Blood gas to fully evaluate the patient’s acid/base status, with an arterial blood gas being preferred for evaluation of lung pathology and potential PTE Serial coagulation panels to assess coagulation status as a primary disease process during the course of hospitalization(s), especially due to persistent elevations in ALT and ALP, as well as hypoalbuminemia (all potential indicators of liver disease/failure) Based on the patient’s rapid decline and grave prognosis, the owners elected humane euthanasia on 6/9/13. Diagnosis at necropsy was a pancreatic adenocarcinoma with widespread multiorgan metastasis (including the liver, lungs, spleen, and multiple lympho nodes), secondary pancreatic necrosis and fat necrosis with saponification, and hemorrhage into the distal gastrointestinal tract. Petechiae were present in multiple organs, supporting the clinical diagnosis of DIC. No renal lesions were noted.
