Colorectal cancer.pptx by -MANOJIT(MS)
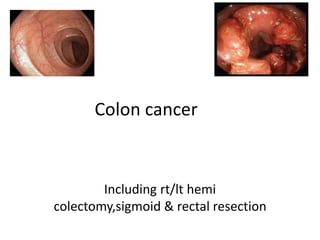
- 1. Colon cancer Including rt/lt hemi colectomy,sigmoid & rectal resection
- 2. Key facts • Colorectal cancer (CRCa) is the 2nd commonest tumour and commonest GI malignancy. • 1 in 18 of the population will suffer CRCa, • M:F::3:1. • Peak age of incidence 45-65 but is increasing in younger ages.
- 4. Pathological features • The predominant type is adenocarcinoma (mucinous, signet ring cell, and anaplastic subtypes). • Classified as well, moderately, or poorly differentiated
- 5. Predisposing factors include: • Polyposis syndromes (including FAP, HNPCC, juvenile polyposis); • Strong family history of colorectal carcinoma; • Previous history of polyps or crca; • Chronic ulcerative colitis or colonic crohn's disease; • Diet poor in fruit and vegetables.
- 6. Risk Factors Associated with Colon Cancer RISK FACTORS COMMENT Geographic variation Highest risk in Western countries and lowest risk in developing countries Age Risk increase sharply after the fifth decade Diet Increased with total and animal fat diets Physical inactivity Increased with obesity and sedentary life style Adenoma Risk dependent on type and size FAP penetrance in gene carriers 100% HNPCC penetrance in gene carriers 80% Hamartomatous syndromes Risk increased with Peutz-Jeghers syndrome and juvenile polyposis but not isolated juvenile polyps Previous history of colon cancer Increased risk for recurrent cancer Ulcerative colitis 10–20% after 20 years Radiation Associated with a mucinous histology and poor prognosis Ureterosigmoidostomy 100–500 times increased risk at or adjacent to the uretero-colonic anastomosis
- 7. Morphology • CRCa may occur as a polypoid, ulcerating, stenosing or infiltrative tumour mass. • The majority (75%) lie on the left side of the colon and rectum (rectum, 45%;descending/sigmoid; 30%; transverse; 5%; right-sided, 20%). • 3-5% have a synchronous carcinoma at time of diagnosis.
- 8. Clinical features Rectal location • PR bleeding: deep red on the surface of stools. • Change in bowel habit: difficulty with defecation, sensation of incomplete evacuation, and painful defecation (tenesmus).
- 9. Descending-sigmoid location • PR bleeding: typically dark red, mixed with stool, sometimes clotted. • Change in bowel habit: typically increased frequency, variable consistency, mucus PR, bloating, and flatulence.
- 10. Right-sided location • Iron deficiency anaemia may be the only elective presentation.
- 11. Emergency presentations • Up to 40% of colorectal carcinomas will present as emergencies. • Large bowel obstruction (colicky pain, bloating, bowels not open). • Perforation with peritonitis. • Acute PR bleeding.
- 12. Diagnosis and investigations Elective diagnosis • by PR examination or rigid sigmoidoscopy for rectal carcinoma. • Flexible sigmoidoscopy should identify up to 75% of tumours (left-sided). • Colonoscopy is generally a more reliable investigation.
- 14. • Barium enema is appropriate if colonoscopy is contraindicated or inappropriate. • Tumour marker (CEA) can be used to monitor disease if it is raised at diagnosis and falls to normal after resection.
- 15. CEA • A carcinoembryonic antigen (CEA) test is a blood test used to help diagnose and manage certain types of cancers, especially cancers of the large intestine and rectum. This test can also be used to help determine if a cancer treatment is working.
- 16. A normal level of CEA is less than or equal to 3 nanograms per milliliter (ng/mL). Increased levels of CEA may be found in the following cancers: • Colorectal or colon cancer • Medullary thyroid carcinoma • Breast cancer • Cancer of the gastrointestinal tract • Liver cancer • Lung cancer • Ovarian cancer • Pancreatic cancer • Prostate cancer
- 17. • The best use of CEA is as a tumor marker, especially for cancers of the gastrointestinal tract. When the CEA level is abnormally high before surgery or other treatment, it is expected to fall to normal following successful surgery to remove all of the cancer. A rising CEA level indicates progression or recurrence of the cancer. This must be confirmed , as the CEA test by itself is not specific enough to substantiate a recurrence of a cancer. In addition, levels >20 ng/ml before therapy may be associated with cancer which has already spread (metastatic disease).
- 18. Emergency presentations • Commonly diagnosed by abdominal CT scan. • Single contrast enema may be used when the diagnosis of large bowel obstruction is possible and CT scanning is unavailable. • Acute PR bleeding is sometimes investigated by urgent colonoscopy.
- 19. Staging investigations • Assessment of the presence of metastases (liver, lung or para-aortic): commonest investigation is thoracoabdominal CT scanning. CXR and liver ultrasound is an alternative. • Assessment of local extent. For colonic carcinoma CT scanning is adequate. For rectal cancer pelvic MRI and transrectal ultrasound are commonly used. • Assessment of synchronous tumours. If not diagnosed by colonoscopy or barium enema, one of these is usually performed to identify synchronous tumours.
- 20. Pathological staging Duke's (approx. % 5y survival) • A, confined to bowel wall only. • B, through bowel wall. • C, any with +ve lymph nodes. • D, any with metastases.
- 21. Treatment Potentially curative treatment • Suitable for technically resectable tumours with no evidence of metastases (or metastases potentially curable by liver or lung resection). • Surgical resection (with lymphadenectomy) is the only curative treatment.
- 22. • Typical operations: – right/transverse: right/extended right hemicolectomy; – left: left hemicolectomy; – sigmoid/upper rectum: high anterior resection; – anorectal: abdomino-perineal resection (APER). – lower rectum: low anterior resection/APER;
- 23. STANDARD RESECTIONS OF THE COLON
- 27. Rectal resection
- 29. • Preoperative (neoadjuvant) chemoradiotherapy may be used in rectal cancer to increase the chance of curative resection. • Adjuvant chemotherapy (5-FU based) is offered for tumours with positive lymph nodes or evidence of vascular invasion. • Hepatic or lung resection may be offered to a few patients with suitable metastases and a clear resection of the primary tumour
- 30. Palliative treatment For unresectable metastases or unresectable tumours. • Chemotherapy may effectively extend life expectancy with a good quality of life. • Obstructing tumours may be endoluminally stented with self-expanding metal stents or transanally ablated if rectal. • Surgery reserved for untreatable obstruction, bleeding, or severe symptoms.
- 31. LIVER METS. • NEARLY 50% PTS PRESENTS WITH ISOLATED LIVER METS AMENABLE TO SURGICAL RESECTION IN THE FORM OF HEPATECTOMY. 1) WEDGE RESECTION. 2) ANATOMIC UNISEGMENTAL OR POLYSEGMENTAL RESECTION. 3) LOBAR RESECTION.
- 32. NON RESECTIONAL SURGERY • Hepatic Art. Infusion. • Cryo-ablation. • Radio Frequency Ablation (RFA).
- 33. PULONARY METS. • ~2% of pts of lung mets are amenable to metastectomy.
- 34. ISOLATED METS to other sites • Oophorectomy for ovarian mets. • Bone mets are treated with internal fixation & irradiation. • Brain mets are treated with Sx if possible, or steroid & irradiation.
- 35. CHEMO THERAPEUTIC AGENTS • 5 FU is the mainstay. • IRINOTECAN & OXALIPLATIN has established beneficial effect.
- 36. BIOLOGIC RESPONSE MODIFIERS • BEVACIZUMAB is a monoclonal antibody directed against vascular endothelial growth factor. • CETUXIMAB – AN ANTIBODY DIRECTED AGAINST ENDOTHELIAL GROWTH FACTOR.
- 37. PALLIATIVE MEDICAL THERAPY • Narcotic Agents. • Antidepressants. • Local Nv Block. • Epidural Analgesic Pumps.
- 38. • 5-FU: steatosis • Irinotecan: steatohepatitis • Oxaliplatin: sinusoidal/vascular injury • Bevacizumab – Potential wound healing complications – Need to wait 6-8 wks before surgical resection • Cetuximab: no acute or chronic effects to date Incidence of postoperative complications increases with prolonged use
- 39. • Acneiform Eruption Associated With EGFR Inhibitors