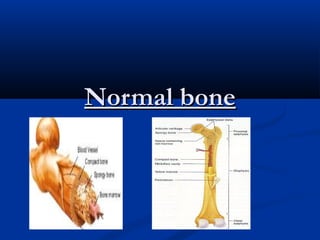
osteomylitis
- 2. Infectious Diseases ofInfectious Diseases of BoneBone 1.1. OsteomyelitisOsteomyelitis 2.2. Pott’s DiseasePott’s Disease
- 3. Definition:Definition: This is inflammation of bone and bone marrow,This is inflammation of bone and bone marrow, can occur in any age group which may be acute,can occur in any age group which may be acute, subacute or chronicsubacute or chronic OSTEOMYELITISOSTEOMYELITIS Classification:Classification: Non- bacterial osteomyelitis:Non- bacterial osteomyelitis: Viral osteomyelitisViral osteomyelitis SarcoidosisSarcoidosis Radiation osteomyelitisRadiation osteomyelitis
- 4. Bacterial osteomyelitis:Bacterial osteomyelitis: Acute suppurative osteomyelitisAcute suppurative osteomyelitis Acute haematogenous osteomyelitisAcute haematogenous osteomyelitis Acute non-haematogenous osteomyelitisAcute non-haematogenous osteomyelitis Chronic osteomyelitis:Chronic osteomyelitis: Chronic non-specific osteomyelitisChronic non-specific osteomyelitis Chronic specific osteomyelitis ( TB & Syphilis)Chronic specific osteomyelitis ( TB & Syphilis)
- 5. Etiology(CausesEtiology(Causes(( 11--HaematogenosHaematogenos….from blood stream <bacteremia>….from blood stream <bacteremia> 2-Direct invasion2-Direct invasion….from skin puncture in operation or open….from skin puncture in operation or open## 33--InjectionInjection….around a bone….around a bone 44--Pts withPts with….conditions or taking drugs that weaken immune system….conditions or taking drugs that weaken immune system The causal organism in both adults and children areThe causal organism in both adults and children are:.:. --S. aureus…. 70-90S. aureus…. 70-90%% --other etiological less often : GABS… Strept. pyogenes , S. pneumonia , H. influenza ,other etiological less often : GABS… Strept. pyogenes , S. pneumonia , H. influenza , E. coli , Pseudomonas , ProteusE. coli , Pseudomonas , Proteus --Salmonella typhi in Pt with sickle cell diseaseSalmonella typhi in Pt with sickle cell disease
- 6. Factors predisposing to bone infectionFactors predisposing to bone infection --Malnutrition and general debilityMalnutrition and general debility --Diabetes mellitusDiabetes mellitus --Corticosteroid administrationCorticosteroid administration --Immune deficiencyImmune deficiency --Immunosuppressive drugsImmunosuppressive drugs --Venous stasis in the limbVenous stasis in the limb --Peripheral vascular diseasePeripheral vascular disease --Loss of sensibilityLoss of sensibility --Iatrogenic invasive measuresIatrogenic invasive measures --TraumaTrauma
- 7. Definition:Definition: Acute osteomyelitis is an acuteAcute osteomyelitis is an acute inflammation of bone caused by an infectinginflammation of bone caused by an infecting organismorganism ACUTE HAEMATOGENIUSACUTE HAEMATOGENIUS OSTEOMYELITISOSTEOMYELITIS Haematogenous osteomyelitis is predominantly seen inHaematogenous osteomyelitis is predominantly seen in children and involves the highly vascular long boneschildren and involves the highly vascular long bones <Metaphysis> especially those of the lower limbs.<Metaphysis> especially those of the lower limbs. In adults, haematogenous spread is more common toIn adults, haematogenous spread is more common to the thoracolumbar spine than elsewhere…also feet ,the thoracolumbar spine than elsewhere…also feet , pelvis. that may be dt lowered resistant , local trauma ,pelvis. that may be dt lowered resistant , local trauma , damage muscle ,..etcdamage muscle ,..etc
- 8. 1-Inflammation: Initial inflammation with vascularInitial inflammation with vascular congestion and increased intra-osseous pressure.congestion and increased intra-osseous pressure. PathologyPathology (Stages of disease)(Stages of disease) Inflammation of boneInflammation of bone
- 9. 2-Suppuration: Pus within the bones forces its wayPus within the bones forces its way through the Haversian system and forms athrough the Haversian system and forms a subperiosteal abscesssubperiosteal abscess in 2-3 days.in 2-3 days. 3-Sequestrum:3-Sequestrum: Vascular obstruction and infectiveVascular obstruction and infective thrombus decrease or obstruct the periosteal andthrombus decrease or obstruct the periosteal and endosteal blood supply, causingendosteal blood supply, causing bone necrosisbone necrosis andand sequestrum formation in approximately 7 days.sequestrum formation in approximately 7 days. 4-Involucrum:4-Involucrum: This is new bone formation from theThis is new bone formation from the stripped surface of periosteum.stripped surface of periosteum.
- 10. 5-Resolution or progression to complications5-Resolution or progression to complications:: With antibiotics and surgical treatment early in the course of disease, osteomyelitis resolves without any complications.
- 11. Clinical featuresClinical features Children:.Children:. presents withpresents with --Severe painSevere pain,, Malaise andMalaise and aa FeverFever --Local redness, swelling, warmth and oedema areLocal redness, swelling, warmth and oedema are later signslater signs --Lymphadenopathy is common but non-specificLymphadenopathy is common but non-specific AdultsAdults:.:. --Mild fever and BackacheMild fever and Backache --Others….chills, irritability, swelling and rednessOthers….chills, irritability, swelling and redness over the affected boneover the affected bone
- 12. Clinical featuresClinical features --In Pts with DM, PVD, Peripheral neuropathyIn Pts with DM, PVD, Peripheral neuropathy there may be no pain or fever the onlythere may be no pain or fever the only symptoms may be the area of skin break-downsymptoms may be the area of skin break-down
- 13. DIAGNOSISDIAGNOSIS 11--Complete Medical HistoryComplete Medical History…. Ask about…. Ask about --Recent infections elsewhereRecent infections elsewhere --Past medical Hx, family medical HxPast medical Hx, family medical Hx --Medication usageMedication usage 22--Physical ExaminationPhysical Examination …. Look for…. Look for -Area of tenderness, redness, swelling-Area of tenderness, redness, swelling --Decrease or painful range of motionDecrease or painful range of motion --Open soresOpen sores
- 14. INVESTIGATIONSINVESTIGATIONS 11--LaboratoryLaboratory:.:. Blood Tests:Blood Tests: - CRP..- CRP.. elevated within 12–24 hrselevated within 12–24 hrs --ESR ..ESR .. elevated within 24–48 hourselevated within 24–48 hours - WBCs ..- WBCs .. elevated *leucocytosiselevated *leucocytosis** --Hb ..Hb .. may be diminished *Anemiamay be diminished *Anemia** Blood cultures...Blood cultures... are +ve in less than half of casesare +ve in less than half of cases Needle aspiration:Needle aspiration: to identify the type of infection and assist with theto identify the type of infection and assist with the initial choice of antibiotic, and tests for sensitivityinitial choice of antibiotic, and tests for sensitivity Biopsy:Biopsy: to cultural and Abx sensitivityto cultural and Abx sensitivity
- 15. 22--RadiologyRadiology PLAIN X-RAYPLAIN X-RAY:: --In 1In 1stst wk x-ray shows no abnormality of the bone; By the 2wk x-ray shows no abnormality of the bone; By the 2ndnd wkwk there may be a faint extra-cortical outline due to periosteal newthere may be a faint extra-cortical outline due to periosteal new bone formationbone formation --Later there is patchy rarefaction of the metaphysisLater there is patchy rarefaction of the metaphysis
- 16. MP of acute osteomyelitisMP of acute osteomyelitis Inflammation of boneInflammation of bone
- 18. 1.1. PathologicalPathological fracturefracture 2.2. Spread of infection: eg. Arthritis (jointSpread of infection: eg. Arthritis (joint inflammation), myositis (muscle inflammation)inflammation), myositis (muscle inflammation) or neuritis (nerve inflammation)or neuritis (nerve inflammation) 3.3. Blood spread: causing toxaemia & septicaemiaBlood spread: causing toxaemia & septicaemia 4.4. Chronic suppurative osteomyelitis: includingChronic suppurative osteomyelitis: including sequestrum formation and skin sinus formationsequestrum formation and skin sinus formation 5.5. Damage to the growth plate causing subsequentDamage to the growth plate causing subsequent growth deformitygrowth deformity Complications of osteomyelitisComplications of osteomyelitis::
- 19. Pott's diseasePott's disease Pott's diseasePott's disease is a presentation of extrais a presentation of extra pulmonary tuberculosis that affects the spine, apulmonary tuberculosis that affects the spine, a kind of tuberculous arthritis of the intervertebralkind of tuberculous arthritis of the intervertebral joints.joints. The lower thoracic and upper lumbar vertebraeThe lower thoracic and upper lumbar vertebrae are the areas of the spine most often affected.are the areas of the spine most often affected.
- 21. Tuberculosis of the spine in an Egyptian mummy
- 22. Clinical presentation:Clinical presentation: 1.1. Back painBack pain 2.2. FeverFever 3.3. Night sweatingNight sweating 4.4. AnorexiaAnorexia 5.5. Weight lossWeight loss 6.6. Spinal mass, sometimes associated withSpinal mass, sometimes associated with numbness, paraesthesia or muscle weakness ofnumbness, paraesthesia or muscle weakness of the legsthe legs
- 23. DiagnosisDiagnosis Blood tests – elevated erythrocyte sedimentationBlood tests – elevated erythrocyte sedimentation rate (ESR)rate (ESR) Tuberculin skin testTuberculin skin test Radiographs of the spineRadiographs of the spine Bone scanBone scan CT of the spineCT of the spine Bone biopsyBone biopsy MRIMRI
- 24. Pott’s Disease; X-ray Pott’s Disease; MRI
- 25. ComplicationsComplications Vertebral collapse resulting in kyphosisVertebral collapse resulting in kyphosis Spinal cord compressionSpinal cord compression Sinus formationSinus formation Paraplegia (called Pott's paraplegia)Paraplegia (called Pott's paraplegia)
- 26. Tuberculous in long bonesTuberculous in long bones Commonly around the knee, affects metaphysis andCommonly around the knee, affects metaphysis and epiphysis, rarely diaphysisepiphysis, rarely diaphysis Well-defined lytic areaWell-defined lytic area
- 27. Tuberculous arthritisTuberculous arthritis The hip and knee are theThe hip and knee are the most commonly affectedmost commonly affected peripheral joints.peripheral joints. Characterized by joint spaceCharacterized by joint space narrowing and erosions whichnarrowing and erosions which may lead to extensive destructionmay lead to extensive destruction of the articular cortex.of the articular cortex.
- 28. HEREDITARYHEREDITARY BONE DISORDERSBONE DISORDERS 1.1. AchondroplasiaAchondroplasia 2.2. Osteogenesis imperfectaOsteogenesis imperfecta 3.3. osteopetrosisosteopetrosis
- 29. AchondroplasiaAchondroplasia Clinically: Long bones are short and thick short extremities dwarfism Cranial and vertebral bone spared relatively large head and trunk Normal intelligence, life span and reproductive ability
- 31. Osteogenesis imperfectaOsteogenesis imperfecta 1-Generalized osteopenia: brittle bones, resulting in recurrent fractures and skeletal deformity 2-Most patients have an abnormally thin sclera with blue hue Abnormally thin sclera with blue hueAbnormally thin sclera with blue hue
- 32. 3. Laxity of joint ligments leads to hypermobilty 4. Involvement of the bones of the inner and middle ear produces deafness 5. Some patients have dentinogenesis imperfecta: small, fragile and discolored teeth due to deficiency of dentin 6. The skin may be abnormally thin and the skin is susceptible to easy bruising
- 33. Osteogenesis imperfectaOsteogenesis imperfecta Brittle bones Laxity of joint ligamentsLaxity of joint ligaments
- 35. OsteopetrosisOsteopetrosis Marble bone Hereditary defect leading to thick sclerotic bones Pathology: -Increased bone density and thickening of bone cortex -The thickened bones are brittle and fracture easily
- 36. X-ray findings: Symmetrically generalized osteosclerosis Long bones may have broadened metaphyses, resulting in an "Erlenmeyer flask" deformity
- 37. Osteopetrosis X-ray findings Osteosclerosis Erlenmeyer flask shaped deformity Symmetrically generalized Osteosclerosis Long bones may have broadened metaphyses, resulting in an "Erlenmeyer flask" deformity
- 38. Metabolic Diseases ofMetabolic Diseases of BoneBone
- 39. OsteoporosisOsteoporosis Refers toRefers to increased porosityincreased porosity of skeleton.of skeleton. Osteoporotic bones:Osteoporotic bones: Thin and fragile and are susceptible to fracture.Thin and fragile and are susceptible to fracture. Occurs due toOccurs due to:: Loss of organic bone matrix and minerals.Loss of organic bone matrix and minerals. Resulting inResulting in :: DecreasedDecreased bone massbone mass andand densitydensity.. DecreasedDecreased thicknessthickness of cortical and trabecularof cortical and trabecular bone.bone.
- 42. Types of OsteoporosisTypes of Osteoporosis LocalizedLocalized : e.g. disuse of a limb: e.g. disuse of a limb GeneralizedGeneralized: involves entire skeleton.: involves entire skeleton. 1.1. Primary:Primary: Old age (Senile)Old age (Senile) Estrogen deficiency (postmenopausal)Estrogen deficiency (postmenopausal) 1.1. Secondary:Secondary: (due to underlying disease)(due to underlying disease) CushingCushing’’s disease (Hypercortisolism)s disease (Hypercortisolism) Drugs (Heparin and Steroids)Drugs (Heparin and Steroids)
- 43. Postmenopausal OsteoporosisPostmenopausal Osteoporosis Due to estrogen deficiencyDue to estrogen deficiency Estrogen deficiencyEstrogen deficiency increased resorption ofincreased resorption of bone by osteoclasts and decreased formationbone by osteoclasts and decreased formation of bone by osteoblasts.of bone by osteoblasts.
- 44. Peak bone massPeak bone mass Osteoporosis Menopause •↓ estrogen •↑ osteoclast activity Aging •↓ activity of osteoblasts •↓ physical activity Physical activityPhysical activity NutritionNutrition Genetic factorsGenetic factors
- 45. Clinical findingsClinical findings:: Bone painBone pain Weight bearing bones predisposed toWeight bearing bones predisposed to Compression of vertebral bodies (most common)Compression of vertebral bodies (most common) Colles’ fracture of distal radius.Colles’ fracture of distal radius. Fracture femoral neck.Fracture femoral neck. Loss of height and kyphosisLoss of height and kyphosis
- 46. 46
- 47. Diagnosis:Diagnosis: Dual energy X ray absorptiometry (DEXA)Dual energy X ray absorptiometry (DEXA) to evaluate bone density.to evaluate bone density.
- 49. Osteonecrosis (Avascular necrosisOsteonecrosis (Avascular necrosis(( Ischemic infarction of bone & bone marrow.Ischemic infarction of bone & bone marrow. Causes of ischemia:Causes of ischemia: Vascular interruption (fracture)Vascular interruption (fracture) Corticosteroids (most common)Corticosteroids (most common) Sickle cell diseaseSickle cell disease Common sites includeCommon sites include Femoral headFemoral head Scaphoid bone.Scaphoid bone.
- 53. Definition: Localized disorder of bone Due to: Excessive bone resorption followed by disorganized bone replacement Resulting in: Thickened but weak bone that is susceptible to deformity and fracture
- 54. Stages of paget disease 1. Osteolytic: osteoclastic activity predominates 2. Mixed ostelytic-osteoblastic 3. Osteosclerotic: osteoblastic activity predominates " burnout stage"
- 55. 55
- 56. Etiology: 1. Possible slow virus infection 2. Possible genetic predisposition
- 57. Clinical features: 1. Asymptomatic in most cases 2. Bone pain and deformities 3. Fractures 4. Warmth of overlying skin due to hypervascularity
- 58. Forms of involvement: 1. Monosteotic (15%): involving one bone 2. Polyosteotic (85%) : involving multiple bones Common sites include the skull, pelvis, femur and vertebrae
- 59. PATHOLOGYPATHOLOGY MicroscopicallyMicroscopically :: Haphazard arrangement of cement lines, creating aHaphazard arrangement of cement lines, creating a mosaic patternmosaic pattern Skull involvement:Skull involvement: 1.1. Increase head sizeIncrease head size 2.2. Foramina narrowing causes impingement of cranialForamina narrowing causes impingement of cranial nerves, often leading to deafnessnerves, often leading to deafness 3.3. Involvement of facial bones may produce a lion-likeInvolvement of facial bones may produce a lion-like faciesfacies
- 60. X-rays: Bone enlargement with lytic and sclerotic areas Lab investigation: Highly elevated serum alkaline phosphatase Complication: Osteosarcoma Others sarcomas
- 62. Osteolytic changes of the skullOsteolytic changes of the skull
- 63. Mosaic pattern of lamellar boneMosaic pattern of lamellar bone
- 64. BONE TUMORSBONE TUMORS BENIGN TUMORS OF BONEBENIGN TUMORS OF BONE
- 65. Classification of benign tumors of boneClassification of benign tumors of bone:: 1.1. OsteomaOsteoma 2.2. Osteoid osteomaOsteoid osteoma 3.3. OsteoblastomaOsteoblastoma 4.4. OsteochondromaOsteochondroma 5.5. OsteochondromatosisOsteochondromatosis 6.6. EnchondromaEnchondroma
- 66. OsteomaOsteoma Definition:Definition: Benign neoplasm that frequently involves the skullBenign neoplasm that frequently involves the skull and facial bonesand facial bones
- 67. Osteoid osteomaOsteoid osteoma Definition:Definition: Benign,Benign, painful growthpainful growth of the diaphysis of a long bone,of the diaphysis of a long bone, often the tibia or femuroften the tibia or femur Clinically:Clinically: 1.1. Males> femalesMales> females 2.2. Age: 5-25 yearsAge: 5-25 years 3.3. Pain that is worse at night and relieved by aspirinPain that is worse at night and relieved by aspirin X-rayX-ray:: Central radiolucency surrounded by sclerotic rimCentral radiolucency surrounded by sclerotic rim
- 69. OsteoblastomaOsteoblastoma Similar to an osteoid osteoma but is largerSimilar to an osteoid osteoma but is larger (>2cm) and often(>2cm) and often involves vertebraeinvolves vertebrae
- 70. OsteochondromaOsteochondroma (Exostosis(Exostosis(( Definition:Definition: Benign boney capped with cartilage that originates fromBenign boney capped with cartilage that originates from epiphyseal growth plateepiphyseal growth plate Clinical presentation:Clinical presentation: 1.1. Adolescent malesAdolescent males 2.2. Firm solitary growths at the end of the long bonesFirm solitary growths at the end of the long bones 3.3. They may be asymptomatic or it causes pain, deformity or itThey may be asymptomatic or it causes pain, deformity or it can undergo malignant transformation (rare)can undergo malignant transformation (rare)
- 72. OsteochondromatosisOsteochondromatosis Multiple hereditary exostosis in which there isMultiple hereditary exostosis in which there is multiple symmetric osteochondromasmultiple symmetric osteochondromas
- 73. EnchondromaEnchondroma Definition:Definition: Benign cartilaginous growth within the medullaryBenign cartilaginous growth within the medullary cavity of bone, usually involving the hands and feetcavity of bone, usually involving the hands and feet Typically solitary and asymptomatic and require noTypically solitary and asymptomatic and require no treatmenttreatment
Hinweis der Redaktion
- Osteoporotic vertebral body (right) shortened by compression fractures, compared with a normal vertebral body.
- Vertebrae, osteoporosis - Gross, cut surfaces
- Pathophysiology of postmenopausal and senile osteoporosis
- Femoral head with a subchondral, wedge-shaped pale yellow area of osteonecrosis
- Osteonecrosis of the head of the femur. A coronal section shows a circumscribed area of subchondral infarction with partial detachment of the overlying articular cartilage and subarticular bone.
- Diagrammatic representation of Paget disease of bone, demonstrating the three phases in the evolution of the disease.
