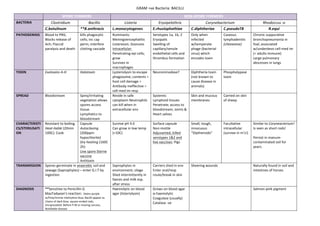
Gram positive bacilli
- 1. GRAM +ve Bacteria: BACILLI SPORE FORMERS NON-‐SPORE FORMERS BACTERIA Clostridium Bacillis Listeria Erysipelothrix Corynebacterium Rhodoccus :o C.botulinum **B.anthracis L.monocytogenes E.rhusiophathiae C.diphtheriae C.pseudoTB R.equi PATHOGENISIS Blood to PNS; Blocks release of Ach; Flaccid paralysis and death kills phagocytic cells; inc cap perm; interfere clotting cascade Ruminants: Meningoencephalitis Listereosis: Zoonosis Intracellular: Penetrating epi cells; grow Survives in macrophages Serotypes 1a, 1b, 2 Erysipalis Swelling of capillary/venule endothelial cells and thrombus formation Only when infected w/temperate phage (bacterial virus) which encodes toxin Caseous lymphadenitis (cheeeeese) Chronic suppurative bronchopneumonia in foal; associated w/underdevo cell-‐med im (= adults immune) Large pulmonary abscesses in lungs TOXIN Exotoxins A-‐H Holotoxin Lysteriolysin to escape phagosome; contents = host cell damage = Antibody ineffective = cell-‐med im resp Neurominodase? Diphtheria toxin (not known to cause disease in animals) Phospholypase toxin SPREAD Bloodstream Spiny/irritating vegetation allows spores access tissue. Lymphatics to bloodstream Reside in safe cytoplasm Neutrophils can kill when in extracellular env Systemic Lymphoid tissues Penetrate; access to bloodstream; Joints & Heart valves Skin and mucous membranes Carried on skin of sheep CHARACTERISTI CS/STERILISATI ON Resistant to boiling. Heat-‐liable (20min 100C): Cook Capsule Autoclaving (200ppm hypochlorite) Dry heating (160C 2h) Live spore Sterne vaccine Antitoxin Survive pH 4.0 Can grow in low temp (<10C) Surface capsule Non-‐motile Adjuvanted, killed serotypes 1&2 and live vaccines: Pigs Small, tough, innocuous “Diptheroids” Facultative intracellular (survive in m’s!) Similar to Coryneacterium! Is seen as short rods! Persist in manure-‐ contaminated soil for years. TRANSMISSION Spores germinate in anaerobic soil and sewage (Saprophytes) – enter G.I.T by ingestion. Saprophytes in environment; silage Shed intermittently in faeces and milk esp. after stress Carriers shed in env Enter oral/resp route/break in skin Sheering wounds Naturally found in soil and intestines of horses DIAGNOSIS **Sensitive to Penicillin G MacFadyean’s reaction: Stains purple w/Polychrome methylene blue; Bacilli appear as chains of dark blue, square ended rods; encapsulated. Before P.M or moving carcass; Notifiable disease Haemolytic on blood agar (listeriolysin) Grows on blood agar α-‐haemolytic Coagulase (usually) Catalase -‐ve Salmon-‐pink pigment
- 2. GRAM +ve Bacteria: BACILLI Arcanobacterium Acintomyces Nocardia Mycobacterium A.pyrogens A.viscosus A.bovis N.asteroides M.bovis *Badgers & Cattle Other Abscesses (liver) Summer mastitis Ovine foot disease Pyolysin: cytotoxic for phagocytic cells Actinomycosi s in dogs Localised granulomato us abscess of skin/thoracic lesion Lumpy jaw in cattle Granulomatous lesions of soft tissues and bone Granulomatous lesions; able to survive and grow in macrophages Chronic -‐> fatal Pneumonia & wasting Disease beings in lesion elsewhere in body; slow multiplication; phagocytosis; inhib phagosome-‐lys fusion Sensitisation via lymphocyte recognition; infectious granuloma (tubercle) M.xenopi: Cold-‐blooded M.avian: Common in pigs at slaughter Poultry (wild birds and free range) Deer: common. M.bovis inc [Horses: Naturally resistant; rare] [Dogs: M.tuberculosis from humans] [Sheep/Goats: V.rare] Several extracellular pore-‐forming toxins If infection not destroyed by CMI of granuloma; release bacilli; tubercles in other tissues and organs Upper resp tract and genital tracts of domestic animals Ruminal wall May progress into abdomen (pyothorax) Lesions more difficult to treat than acintom. As resistant to number of antimicrobials Cattle >6months: Respiratory route via Alimentary tract (post-‐natal, calf infection) and congenital route. Adult: After resp infection as tuberculosis bronchiolitis; bronchiolar spread; TB pneumonia; Caseous liquefaction & bronchiectasis; open case Similar to Coryneacteriu: Chinese characteristics in W, N, M arrangement Curved/swollen ends Filamentous; branching Prefers anaerobic but not strict anaerobe Forms branching rods much shorter than actinomycetes [Isolation PM: inject material into guinipig (v.susceptible): act as a biological filter; succumb to disease if M.bovis present – now discontinued] Relatively resistant to drying (viable for yrs), antibiotics and chemical agents: common to pre-‐ treat specimens w/NaOH/Oxalic acid to destroy normal bacteria leaving mycobacteria unharmed Round-‐ended rods Strict anaerobes Slow growing Some saprophytic will grow in colonies in few days but pathogenic take 2-‐8 weeks Opportunistic pathogen Soft grey granules: when squashed, organism released Oral bacteria; inoculated into tissues by trauma Soil bacterium Shedding into env – lesion excretion; ‘open case’: udder/uterus/resp tract; coughing Immunity does develop but inadequate Grows slowly on blood agar: small white colonies surrounded by zone of β-‐haemolysis after 48 hours. Non-‐acid fast Catalase +ve Partially acid-‐fast; cell walls contain mycolic acids (like mycobacteria) Mycolic acid repels aq stain Although G+ve in cell wall structure, are difficult to stain; Acid fast Zeihl-‐Neelsen stain used instead. TESTS: Single, comparative intradermal test of PPD – TCA precipitated tuberculin. M.bovis and M.avian – both injected intradermally – exam after 72h [Cattle susceptible to M.avian (localised lesions); PPD w/M.avian would cause sensitisation alone] CMI response! = Swelling + Oedema = +ve (Type IV reaction) No Vac as interfere w/test. IF-‐γ stimulation test: Collect blood; culture lymphocytes; stimulate w/PPD ELISA (useless as v.little/no antibody!): Measure release of IF-‐γ PCR/Immunofluorescence – look for bacteria
- 3. GRAM +ve Bacteria: BACILLI