Thyroid Hormone Synthesis, Secretion, and Regulation (39
- 4. • An important component in the synthesis of thyroid hormones is iodine. Thyroid hormones are synthesized from the amino acid tyrosine. • The synthesis requires the iodination of tyrosine molecules and the combination of two iodinated tyrosine residues. • T3 is frequently considered the physiologically active hormone, and consequently the one on which most athletes and bodybuilders focus their energies on. • T4 is a prohormone and a reservior for the most active thyroid hormone (T3). • T4 is converted as required in the tissues by Iodothyronine deiodinase.
- 5. • Thyroglobulin (Tg) is a dimeric protein produced by the follicular cells of the thyroid and used within the thyroid gland. • (Tg) is a precursor of thyroid hormones which are produced when thyroglobulin's tyrosine residues are combined with iodine and a protein is subsequently cleaved.. • Each thyroglobulin molecule contains approximately 100-120 tyrosine residues, but only (20) of these are iodinated by thyroperoxidase in the folliculear colloid. • Therfore,each Tg molecule form only approximately 10 thyroid hormone molecules.
- 11. • The nature of the enzyme thyroperoxidase • Oxidation of iodide to active iodine, iodination of tyrosine residues and coupling of iodotyrosines are catalyzed by a heme- containing particulate bound peroxidase called thyroperoxidase which requiresH2O2 for its activity. • Iodine trapping: The thyroid gland concentrates iodine by actively and selectively transporting it from the circulation. The transport mechanism is called as iodide trapping or iodide- pump. • The iodide trapping is done :_ • 1-Against electrical gradient. • 2-Against concentration gradient. • Iodide transporter pump is located in the basal plasma membrane in association with Na+-K+ dependent ATP ase and requires a simultaneous activity of the soduim pump. • Energy is provided by hydrolysis of ATP followed by a K+ influx and Na+ efflux.
- 12. • Iodide Metabolism * Concentration of iodide (I ¯ ) :- • The thyroid along with other epithelial tissue mammary gland, salivary and stomach is able to concentrate I ¯ against electrochemical gradient. * Oxidation of I ¯ :- • The thyroid is only tissue that can oxidize (I ¯) to higher valence state (I+) .This step involves a heme-containing peroxidas and occurs at the luminal surface of the follicular cell. * Iodination of Tyrosine:- • Oxidized iodide reacts with tyrosyl residues in thyroglobulin .The 3 position of the aromatic ring is iodinated first and then the 5 position to form MIT and DIT, this occurs within seconds in luminal thyroglobulin. * Coupling of iodotyrosyls :- • The coupling of two DIT molecules to form T4 or of MIT and DIT to form T3 occurs within the thyroglobulin molecule.
- 13. Plasma transport Most of the thyroid hormone circulating in the blood is bound to transport proteins. Only a very small fraction of the circulating hormone is free (unbound) and biologically active
- 14. • T3 and T4 in plasma are carried by tow specific plasma proteins: • 1-Thyroxine binding globulin (TBG) . • 2-Thyroine binding prealbumin (TBPA). • When binding capacity of the above two carreir proteins is saturated,then they can be bound to serum albumin also.
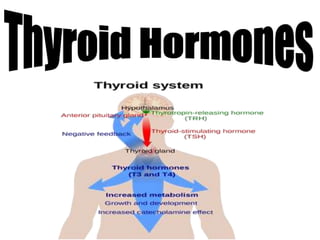
- 16. • Control of TSH Secretion • TSH stimulates the synthesis and release of thyroid hormones from the thyroid gland. The secretion of TSH from the anterior pituitary gland is controlled by:- * 1-Circulating concentrations of thyroid hormones. • Thyroid hormones reduce TSH secretion by negative feedback. * 2-Thyrotrophic-releasing hormone (TRH). • TSH secretion is stimulated by TRH, produced in the hypothalamus .
- 20. • Thyroid Function Tests • 1- The concentration of TBG and its degree of saturation with T3 and T4. • 2- Concentration of free T3 and T4. • 3-The status of hypothalamus and anterior pituitary with their respective outputs of TRH and TSH . • 4- The response of the pituitary to TRH and response of the thyroid to TSH .
- 25. Hypothyroidism
- 26. • Hypothyroidism is the result from any condition that results in thyroid hormone deficiency. * Iodine deficiency: Iodide is absolutely necessary for production of thyroid hormones; without adequate iodine intake, thyroid hormones cannot be synthesized. * Primary thyroid disease: Inflammatory diseases of the thyroid that destroy parts of the gland are clearly an important cause of hypothyroidism. * Congenital hypothyroidism: May be due to absence of the thyroid gland (athyreosis) or may occur secondarly to defects of thyroid hormone synthesis. • Secondary hypothyroidism: Results from pituitary or hypothalamic disease that produce a deficiency of TSH .
- 27. • Laboratory Evaluation of Hypothyroidism • Hypothyroidism may be suspected by symptoms and signs, but the diagnosis needs to be confirmed biochemically. * Free T4 levels are low, T3 levels may within normal limits. TSH is raised in primary hypothyroidism which is the most common cause of hypothyroidism. If TSH is not elevated, it is important to look for pituitary or hypothalamic disease. * In older individuals, biochemical screening for hypothyroidism with a single TSH is recommended. * Thyroid autoantibodies suggest Hashimoto's thyroiditis * LDL may be elevated
- 28. Hyperthyroidism