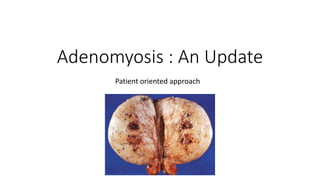
Adenomyosis
- 1. Adenomyosis : An Update Patient oriented approach
- 2. What is the problem? • Diagnosis is difficult • Management is more difficult • So we need Patient orient way approach
- 3. Diagnosis : not easy • up to 80% of adenomyotic uteri contain associated pathology, such as myomas that could have similar clinical presentations • about one-third ofwomen suffering from endometriosis have concomitant adenomyosis, with overlapping and usually heavier symptoms
- 4. Symptoms • asymptomatic in about 35% of the cases • whereas 50% of women with symptoms have menorrhagia, 30% have dysmenorrhea, and 20% have metrorrhagia
- 5. What we know • The definitive diagnosis of adenomyosis is based on histologic examination after hysterectomy.
- 6. MCQ • Do u think adenomyosis a disease of :- a) Nulliparous b) Multiparous c) Low parity d) All above
- 7. Is it related to parous women?!!! • It was deemed that adenomyosis was a typical condition of parous women. However, adenomyosis has become more relevant in the setting of infertility
- 8. So why parous women?? • The incidence of adenomyosis is increased after uterine surgery, cesarean section, postpartum endometritis, pregnancy, uterine trauma, and surgery
- 9. So what about nulliparous women? • because more and more women are delaying childbearing due to social reasons and better imaging techniques have identified adenomyosis in women labeled as having ‘‘unexplained infertility’
- 10. How to reach diagnosis?? • Clinical picture : not reliable • Ultrasonography : may be • MRI : Yes
- 11. Clinical picture • Examination : inconclusive : ?? Enlarged tender uterus • Especially during menses
- 12. TVUS: challenge • 75% sensitive • 84% specific • 2D vs 3D !!!!
- 13. 2D : suggestive signs • Asymmetrically enlarged uterus • Round cystic areas within the myometrium • Inhomogeneous, irregular myometrial echotexture in an indistinctly defined myometrial area • Myometrial hypoechoic linear striations • Illdefined endometrial stripe
- 14. Should we do 3D? • If only 1 of the typical TVS features associated with symptoms like menometrorrhagia, dysmenorrhea, or infertility pls consider MRI for accuracte diagnosis.
- 15. So What is the role of 3D? • For evaluation of the JZ • JZ thickness JZmax R 6 to 8 mm was significantly more associated with histologically proven adenomyosis than other 2D features • Exclude other pathologies
- 16. MRI : the gold standard • The diagnostic accuracy of MRI in the diagnosis of adenomyosis has long been established • (1) thickening of the JZ to at least 8 to 12 mm • (2) ratio JZ maximum-to-total myometrium over 40% • (3) difference between the maximum and the minimum thickness of the JZ = 5 mm • Not during menstruation
- 18. Hysteroscopy: Is there a role? • Seldom use in diagnosis of adenomyosis • To evaluate uterine cavity
- 19. Adenomyosis & infertility : negative impact • Uterine dysperistalsis • Excess concentration of free radicals at endometrial level • Altered ndometrial vasculature • Associated pathology : myoma or endometriosis
- 20. IVF Outcome • Less favourable outcome regarding pregnancy rate , live birth rate • More miscarriage rate • Should be clearly explained to the patients
- 21. In IVF • Suppression of adenomyosis by long-term down-regulation with GnRH agonists has to be considered to improve the outcome.
- 22. Best approach : long protocol • ovarian hyperstimulation with high gonadotropin doses and embryo freezing . • The transfer could be postponed after 2 to 4 months of GnRH agonist therapy with hormone replacement therapy used in frozen–thawed cycles
- 23. If not seeking infertility : LUG • The efficacy of levonorgestrel–intrauterine systems in the treatment of adenomyosis-related pain and heavy menstrual bleeding could be explained by different mechanisms: • (1) a direct progestogenic effect on ectopic adenomyosis foci • (2) decidualization and atrophy of the eutopic endometrium • (3) modulation of endometrial factors altered in adenomyosis
- 24. LUG • Effective • Follow up by symptoms, CA125, TVS
- 25. GnRH a depot • An alternative • Not more than 6 month
- 26. HIFU • Controversial • No evidence till now
- 27. Why it may of value? • Seeking to improve fertility outcomes in patients with Localised Adenomyosis
- 28. Uterine sparing surgery • Usually by hysteroscopy • Resection of specific points • Placenta accreta is a common complication • Uterine rupture has been reported
- 29. MCQ • Do u think adenomyosis a disease of :- a) Nulliparous b) Multiparous c) Low parity d) All above
