Thyroid gland1
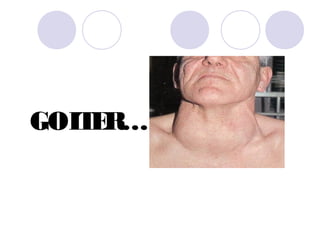
- 1. GOITER…
- 2. ANATOMY
- 3. Anatomy: • It consist of 2 lobes, each lobe is pear in shaped measure 2.4-4 cm length 1.5-2 cm in width 1-1.5 cm in thickness. • both lobes are connected by isthmus. •The weight in adult is approximately 10-20 gm. •The isthmus of the thyroid gland is located midway between apex of thyroid cartilage and suprasternal notch. •Located anteriorly in the lower neck, extending from the level of the fifth cervical vertebra down to the first thoracic •Second to fourth tracheal rings
- 5. * The thyroid gland is the largest endocrine organ in the body. * Highly vascularized; rich blood supply, venous drainage and lymphatics. * The blood flow to the thyroid gland is about 5ml/g/min. * Its function to secrete sufficient amount of thyroid hormone. Thyroid hormone promote normal growth and development and regulate energy and heat production. *The parafollicular cells of thyroid gland secrete calcitonin.
- 7. Physiology: * Primary function of the thyroid gland is the secretion of thyroid hormones - T4 (thyroxine) is primary released hormone - T3 (triiodothyronine) at least 10 times more active -T4 is converted to T3 peripherally * 100% of T4 is synthesized in the thyroid gland. * Only 25-30% of T3 is synthesized in thyroid gland and remaining 70-75% are coming from conversion (deiodination) of T4 into T3 in peripheral tissues.
- 8. •Thyroid hormone regulated by thyroid stimulating hormone (TSH) from the anterior pituitary gland. •The anterior portion of pituitary gland in turn is controlled by thyrotropin releasing hormone (TRH) from hypothalamus.
- 10. Effects of thyroid hormone: *Fetal brain and skeletal maturation. *Increase in basal metabolic rate. *Inotropic and chronotropic effects on heart. *Increases sensitivity to catecholamines. *Stimulates gut motility. *Increase bone turnover. *Increase in serum glucose, decrease in serum cholesterol.
- 11. The endocrine disorders in general can be manifested by either excess or deficiency in the secreting hormones.. Common problem related with thyroid 1)Thyrotoxicosis 2) Hypothyroidism 3)Thyroiditis 4) Goiter 5) Thyroid neoplasia
- 12. Leading cause of anterior neck masses. Children: - Most common neoplastic condition - Male predominance - Higher incidence of malignancy Adults - Female predominance - Mostly benign
- 13. History. Physical exam. Investigation of thyroid. Treatment.
- 14. Investigation of thyroid disease: • TSH level • Free T4 level • Free T3 level • Thyroid antibodies (anti-thyroglobuline antibodies, anti- peroxidase antibodies) • Thyroid ultrasound (U/S neck) • Radio active iodine uptake • Thyroid biopsy (FNA)
- 16. Fine needle aspiration cytology (FNAC): * For discrete thyroid swelling. * Best done under US guidance. * The only disease that cant be diagnosed by FNA is follicular carcinoma.
- 17. Isotope scanning: The uptake by the thyroid of a low dose of either: -Radiolabelled iodine ( I 123) - technetium (Tc 99) will demonstrate distribution of activity in the whole gland.
- 18. Goiter -Non specific term to indicate diffuse enlargement of thyroid gland. - Its only enlargement. - The most common presentation of a goiter case is painless mass in the neck.
- 19. Classification of Goitres Simple goiter: - No hormonal abnormalities and therefore no systemic effects. -Either diffuse or nodular. Simple Toxic goiter: -Increased in production of thyroid hormones. -Either diffuse (graves dis.) or nodular (single nodule or on the top of multinodular goiter. Neoplastic goiter: Either benign (adenoma) or malignant Inflammatory goiter: As many thyroiditis presentation: -Subacute granulomatous -Autoimmune (hashimot’s) -Reidel -Acute supporative
- 20. Clinical assessment of simple goiter: - Benign disease, colloid goiter, euthyroid , female (3rd -5th decade ) -Presented as mild enlargement of the gland, most of the time asymptomatic. -Complication might develop due to mass effect like tracheal compression or voice changes, but mostly asymptomatic. -Acute development—Hemorrhage or cyst >> acute pain ** investigation : 1.TFT 2.neck & chest x-ray 3. dx invest :US & FNAC 4.ISOTOPE SCAN
- 21. Prevention and treatment: 1) Iodine uptake: Iodination of salt Food 2) T4 administration. 3) Thyroidectomy
- 22. Toxic multinodular goiter: - Results from disorganized response of the gland to stimulation and contains areas of hyperplasia and hypoplasia side by side. These nodules are usually necrotic and hemorrhagic. - The commonest presentation is solitary nodule. - 20% risk of malignancy
- 23. Thyroid Uptake Scans (Technetium 99) –Scintigraphy (A)Normal (B) Graves disease: diffuse increased uptake in both thyroid lobes. (C) Toxic multinodulargoiter (TMNG): “hot”and “cold”areas of uneven uptake. (D) Toxic adenoma: increased uptake in a single nodule with suppression of the surrounding thyroid. (E) Thyroiditis: decreased or absent uptake.
- 24. Surgical treatment: * Unilateral total lobectomy * Frozen section examination * Surgery for multinodular goiter: Subtotal vs total thyroidectomy.
- 25. Solitary thyroid nodule: Are common, being a feature of many different thyroid diseases The essential clinical problem, particularly when the lesion is Solitary, is to distinguish between Benign and Malignant disease (nodule).
- 26. Assessment of the thyroid nodule - A nodule in hyperthyroid patient is highly unlikely to be malignant. - Dominant nodule in MNG : Malignancy rate may approach that of solitary nodule 20% Size ,pain ,age ,previous neck radiation Voice changes Pressure symptoms Consistency of the nodule(hard ,fixed) Lymphadenopathy 26
- 27. Investigations: Hormones: T4 , T3 , TSH Neck & Chest X-ray Diagnostic investigations: Needle biopsy and FNAC Ultrasonography Isotope scanning 27
- 28. Treatment Hormone administration Very little evidence to affect benign nodule Indications for surgery Clinical features and suspicious or definite FNAC result. If continue enlarge despite TSH suppression Mechanical symptoms Cosmetic 28
- 29. Thyroid Cancer Rare: Less than 1% of all malignancies Wide spectrum of biological behavior If treated appropriately there is high survival rate Types : Papillary Follicular Anaplastic Medullary Lymphoma Rare secondary 29
- 30. Papillary Carcinoma The Commonest Iodine rich areas Affects children and young adults more, F>M. Previous neck irradiation It has lymphatic spread more than blood (the cervical lymph glands may be palpable long before the primary lesion in the thyroid become palpable) It could be intra, extra thyroid or multicentric. Clinical presentation: nodule with or without cervical lymphoadenopathy, voice changes, airway obstruction if enlarged. Dx: clinical assessment and FNAC 30
- 31. Follicular Carcinoma Higher incidence in iodine deficient areas Low association with radiation. Female to male ratio 3:1 Affects older age group Stimulated by TSH The cells in this tumor retain their normal follicular configuration, encapsulated and solitary. Spreads by blood stream to the brain, bone, lung.. It is not diagnosed by FNA Dx: frozen section Tt: total thyroidectomy. 31
- 32. Anaplastic carcinoma This is the worst type being poorly differentiated and highly invasive. Peak incidence 60-80 years Females more than males Rapid local tissue infiltration Rapid blood metastasis -Long standing goiter-rapid changes in voice and breathing FNAC is diagnostic Surgery, radiotherapy, chemotherapy 32
- 33. Treatment of differentiated thyroid carcinoma: *Total Thyroidectomy is the treatment of choice. *Treatment objectives: Eradicate the primary tumor Reduce the incidence of metastasis Facilitate treatment of metastasis Minimal morbidity 33
- 34. Post operative treatment Thyroxin T4 Replacement Suppress TSH Thyroglobuline • Sensitive indicator for residual or recurrent tumor Radioactive Iodine • Detect metastatic disease • Ablation 34
- 35. Thyroidectomy Indication: - Suspected or proven malignancy. - Thyrotoxicosis. - Tracheal/ esophageal compression - Cosmetic. - Cold nodule for Graves’ Disease - When I131 is contraindicated (pregnancy) - Large Goiters less likely to respond to ATD or I131.
- 36. Pre-operative preparation: 1) the patient should be euthyroid to decrease the risk of arrythmia. (Give PTU +/- beta-blocker before surgery. PTU is better pre-surgical prophylaxis because it additionally blocks peripheral conversion of T4 to T3). 2) Vocal cords should be checked 3) Patient should be warned for post op complication 4) stable (cold) iodine treatment to decrease gland vascularity (usually administer 10 to 14 days before surgery) 5) beta-blocker therapy Generally, antithyroid drug therapy should be administered until thyroid functions normalize (4-8 wk).
- 37. Operations: •Solitary benign nodule requires lobectomy •Cancer requires total thyroidectomy •Thyrotoxicosis or large multinodular goiter requires subtotal or total thyroidectomy
- 38. 1- hemorrhage 2- laryngeal edema 3- nerve damage *recurrent laryngeal nerve *superior laryngeal nerve 4- thyroid storm 5- hypocalcaemia 6- wound infection 7-recurrent thyrotoxicosis or hypothyroidism Complications of Thyroidectomy:
- 39. 1. hemorrhage Rapid expanding of neck swelling (hematoma) Caused airway compromised Incident 0.3 - 1% Features: sudden difficulty in breathing
- 40. Nerve damage Recurrent laryngeal nerve injury Mechanism: partial/ complete transection / burn/ compromised blood supply Features: true vocal cord paresis/ paralysis Hoarseness of voice / difficulty in breathing Prevention: identification intra operatively
- 41. Thyroid storm Acute life threatening, hypermotabolic state Caused by excessive release of thyroid hormones Features: fever, tachycardia, hypertension, neurological, GI disturbance
- 42. hypoparathyroidism Function of PTH - increases serum calcium ( bone resorption, increasing renal absorption of calcium, and stimulating the synthesis of the biologically active form of vitamin D (1,25-dihydroxy vitamin D) - increases renal excretion of phosphorous. - Lead to hypocalcemia
- 43. Hypocalcemia ( transient or permanent) Direct trauma to the parathyroid glands, devascularization of the glands, or removal of the glands during surgery.
- 44. Follow up Review symptoms and thyroid function test every 4 to 6 week until thyroid levels are stabilized on a low dose of antithyroid medication. thyroid function at least every 3 months for the first year. After 12-18 months, stop antithyroid medication or decrease it in patients with Graves hyperthyroidism to determine if the patient has gone into remission.
- 45. THANK YOU