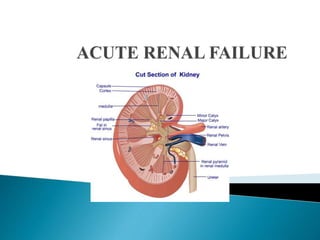
Acute renal failure
- 3. DEFINITIONS Acute renal failure is a sudden reduction in kidney function that results in nitrogenous wastes accumulating in the blood.
- 4. Anuria – no urine output or less than 100mls/24 hours Oliguria - <500mls urine output/24 hours or <20mls/hour Polyuria - >2.5L/24 hours
- 5. ARF Pirouz Daeihagh, M.D.Internal medicine/Nephrology Wake Forest University School of Medicine. Downloaded 4.6.09
- 7. Pre-renal = 55% Renal parenchymal (intrinsic)= 40% Post-renal = 5-15%
- 11. Any condition that significantly reduces renal perfusion pressure and causes a decreased glomerular filtration rate and azotemia* may cause prerenal kidney failure. Clinical conditions that may result in prerenal kidney failure include but are not limited to: extracellular fluid losses secondary to burns, prolonged vasoconstriction (hypertension), and reduced cardiac output as seen in patients with shock syndrome or congestive heart failure. If prerenal failure is identified early and treated correctly, the kidney dysfunction may be reversible. If the underlying cause continues to affect renal perfusion, it may lead to ischemic damage to the nephron and acute tubular necrosis (ATN). *Azotemia is a medical condition characterized by abnormally high levels of nitrogen- containing compounds (such as urea, creatinine, various body waste compounds, and other nitrogen-rich compounds) in the blood.
- 12. Problems affecting the flow of blood before it reaches the kidneys 1) Dehydration vomiting, diarrhea, water pills, or blood loss. 2) Disruption of blood flow to the kidneys . *Major surgery with blood loss, severe injury or burns, or infection in the bloodstream.
- 13. * Blockage or narrowing of a blood vessel carrying blood to the kidneys. * Heart failure or heart attacks causing low blood flow. * Liver failure causing changes in hormones that affect blood flow and pressure to the kidney
- 14. Actual damage to the nephrons and renal parenchyma characterize intrarenal failure. Clinical conditions that result in intrarenal damage can be categorized under kidney disease or acute tubular necrosis. ATN is a common type of acute renal failure in the critically ill patient. The use of nephrotoxic drugs (streptomycin, penicillin, and amphotericin) in older patients or in individuals with underlying renal insufficiency place patients at a higher risk of developing ATN. The risk for ATN is also higher in patients with prolonged prerenal factors. ATN is a potentially reversible type of renal failure but it may take weeks or months before adequate renal function returns.
- 15. Nephrotoxicants may act at different sites in the kidney, resulting in altered renal function. The site of injury by selected nephrotoxicants are shown.
- 16. Post-renal failure is caused by clinical conditions that cause obstruction to urine flow. Any problem that stops the excretion of urine may cause this type of ARF. Common conditions associated with post-renal failure are tumors, benign prostatic hypertrophy, kidney stones and bladder neck obstruction. If post-renal failure is untreated it may result in actual nephron damage and intrarenal failure.
- 18. Hyperkalemia Volume overload Vascular access
- 19. Weakness Lethargy Muscle cramps Paresthesias Hypoactive DTRs Dysrhythmias
- 20. K > 5.5 -6 Tall, peaked T’s Wide QRS Prolong PR Diminished P Prolonged QT QRS-T merge – sine wave
- 22. Problems affecting the movement of urine out of the kidneys. a) Kidney stone: usually only on one side. b) Cancer of the urinary tract organs or structures near the urinary tract that may obstruct the outflow of urine. c) Medications.
- 23. d) Bladder stone. e) Benign prostate hyper plasia (the most common cause in men). f) Blood clot. g)Bladder cancer.
- 25. Renal Problems with the kidney itself that prevent proper filtration of blood or production of urine(25-40%). Blood vessel diseases Blood clot in a vessel in the kidneys Injury to kidney tissue and cells
- 26. Medical treatment ◦ Fluid and dietary restrictions ◦ Maintain Electrolytes ◦ May need dialysis to jump start renal function ◦ May need to stimulate production of urine with IV fluids, Dopomine, diuretics, etc. ◦ Hemodialysis ◦ Peritoneal dialysis ◦ Continous renal replacement therapy (CRRT) ◦ Nursing interventions.
- 27. Introduction- Chronic kidney disease (CKD), also known as chronic renal disease (CRD), is a progressive loss in renal function over a period of months or years. Chronic kidney disease is diagnosed as a result of screening of people known to be at risk of kidney problems, such as those with high blood pressure or diabetes and those with a blood relative with chronic kidney disease. It is differentiated from acute kidney disease in that the reduction in kidney function must be present for over 3 months. Chronic kidney disease is identified by a blood test for creatinine. Higher levels of creatinine indicate a lower glomerular filtration rate and as a result a decreased capability of the kidneys to excrete waste products.
- 28. Causes of chronic kidney disease (CKD) include the following: Diabetic kidney disease. Hypertension. Vascular disease (Angina & MI). Glomerular disease (primary or secondary). Cystic kidney diseases. Tubulointerstitial disease ( nephritis affecting the interstitium of the kidneys) Urinary tract obstruction or dysfunction Recurrent kidney stone disease Congenital (birth) defects of the kidney or bladder Unrecovered acute kidney injury
- 29. Tiredness Weakness Not sleeping well Less desire to eat than usual Nausea Itching Shortness of breath Altered taste Altered mental state
- 30. Although chronic kidney disease cannot be cured, it is possible to slow the damage to the kidney in most patients. Doctor may recommend any of the following: Controlling protein in the urine by restricting the amount of protein in the diet or medication. Taking ACE inhibitors or angiotensin II receptor antagonists to slow the progression to chronic renal failure. Reducing the use of and the dosages of drugs that may be toxic to the kidneys. Managing the complications of chronic renal disease such as fluid overload, high blood phosphate or potassium levels, low blood level of calcium, and anemia.
- 34. There are 3 types of dialysis Hemodialysis, Dialysis of soluble substances and water from the blood by diffusion through a semipermeable membrane; separation of cellular elements and colloids from soluble substances is achieved by pore size in the membrane and rates of diffusion.
- 37. Lowering high blood pressure. Controlling blood sugar and lipid levels. Staying hydrated. Controlling salt in the diet. Quitting smoking. Undergoing dialysis, a medical process that cleans the blood. Having a kidney transplant. Counseling for you and your family about dialysis and/or transplant options.
- 38. To help reduce your chance of chronic kidney failure, take the following steps: Get a physical exam every year that includes a urine test to monitor your kidney's health. Do not smoke. Stop smoking if you are a smoker. Maintain a healthy weight. Drink water and other fluids to stay hydrated. People who have diabetes, previously known kidney disease, high blood pressure, or are over the age of 60 should be screened regularly for kidney disease. People with a family history of kidney disease should also be screened regularly.
- 39. Glomerulo nephritis e.g, Streptococcal bacterial infections may damage the glomeruli. Acute interstitial nephritis 1) Medications such as antibiotics, anti-inflammatory medicines (for example, aspirin, brufen), and water pills . 2) infections and immune-related diseases such as lupus , leukemia, lymphoma, and sarcoidosis.
- 42. Causes include shock (decreased blood supply to the kidneys), drugs (especially antibiotics) and chemotherapy agents, toxins and poisons, and dyes used in certain kinds of x-rays. Accidents, injuries complications from surgeries (eg.Heart-bypass surgery) Polycystic kidney. produce less erythropoietin
- 43. RISK FACTORS Advanced age Blockages in the blood vessels in your arms or legs Diabetes High blood pressure Heart failure Kidney diseases Liver disease
- 44. Symptoms Vomiting and/or diarrhea, which may lead to dehydration. Nausea. Weight loss. Nocturnal urination. pale urine. Less frequent urination, or in smaller amounts than usual, with dark coloured urine
- 45. Haematuria. Pressure, or difficulty urinating. Itching. Bone damage. Non-union in broken bones. Muscle cramps (caused by low levels of calcium which can cause hypocalcaemia).: Abnormal heart rhythms. Muscle paralysis.
- 46. Swelling of the legs, ankles, feet, face and/or hands. Shortness of breath due to extra fluid on the lungs Pain in the back or side Feeling tired and/or weak. Memory problems. Difficulty concentrating. Dizziness. Low blood pressure.
- 47. Other symptoms include Anorexia Pruritus Seizures (if blood urea nitrogen level is very high) Shortness of breath (if volume overload is present). Decrease osmolality(A measurement of urine concentration that depends on the number of particles dissolved in it). Increase urinary sodium. Pericarditis. Pericardial effusion. Pleural effusion. Decrease calcium and bicarbonate. Defect in platelet functionings
- 48. PHASES OF ARF Initiating phase Oliguric phase Diuretic phase Recovery phase
- 49. Diagnosis History collection. Physical examination. 1 Asterixis and myoclonus 2 Peripheral edema (if volume overload is present) 3 Pulmonary rales (if volume overload is present) 4 Elevated right atrial pressure (if volume overload is present)
- 50. Identification of precipitating cause. Serum creatinine and BUN level .(n 7-18mg/dl) Serum electrolytes. Urine analysis. Renal bladder ultra sound. Renal scan. CT scans and MRI scan (to identify lesion and masses) The urine will be examined under a microscope. biopsy
- 51. Medical and Pharmacological Treatment correcting fluid and electrolyte balance. Correct dehydration. Correct dehydration. Keeps other body systems working properly Furosemide, Torsemide, ethacrynic acid calcium gluconate Sodium bicarbonate dialysis
- 52. NUTRITIONAL THERAPY Provide protein diet. Calori requirements are met with high carbo-hydrate meals (carbo-hydrates have a protein-sparing effect. Foods and fluid containing potassium or phosphorous (banana, coffee) are restricted. Patient may require parenteral nutrition.
- 53. Prevention A careful history(nephrotoxic antibiotic agent aminoglycosides, gentamicin, tobramicine, etc.) blood tests and urinalysis Drink enough fluids Difficulties urinating or blood in the urine should prompt a visit Treat hypotension promptly. Prevent and treat infections promptly. Pay special attention to wound, burns and other precursors of sepsis.
- 54. COMPLICATIONS ARF can affect the entire body Infection Hyperkalaemia, Hyperphosphataemia, hyponatraemia water overload Pericarditis Pulmonary oedema.
- 55. Reduced level of consciousness. Immune deficiency. NURSING MANAGEMENT Excess fluid volume related to decreased Glomerular filtration rate and sodium retention Risk for infection related to alterations in the immune system and host defenses Imbalanced nutrition: less than body requirements
- 56. Risk for injury related to GI bleeding Sleep pattern disturbances related to disease condition Providing skin care Providing support Patient Teaching and Home Healthcare Guidelines conclusion
- 57. THANK YOU