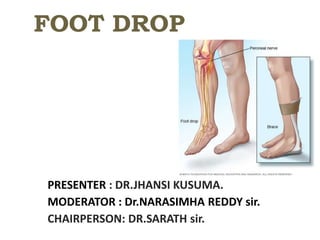
Foot Drop: Causes, Symptoms and Treatment
- 1. FOOT DROP PRESENTER : DR.JHANSI KUSUMA. MODERATOR : Dr.NARASIMHA REDDY sir. CHAIRPERSON: DR.SARATH sir.
- 2. Definition : Inability to actively dorsiflex and evert the foot due to damage to common peroneal nerve. Foot drop is the condition where the propulsion is partially impaired due to change in the gait. The foot is plantar flexed and inverted due to paralysis of dorsiflexers and evertors of the foot , causing a high steeping gait.
- 3. ANATOMY OF LEG: Three compartments : Posterior/ flexor compartment: ( TN) Superficial: Gastrocnemius, Soleus, Plantaris. Middle: Flexor Hallucis Longus, Flexor digitorum longus. Deep: Tibialis posterior Anterior/Extensor compartment: (DPN) Tibialis anterior Extensor hallucis longus Extensor digitorum longus Peroneus tertius Lateral / peroneal compartment: (SPN) Peroneus longus Peroneus brevis
- 4. DORSIFLEXOR MUSCLE -Tibialis anterior -Extensor hallucis longus -Extensor digitorum longus - Peroneus tertius
- 5. TIBIALIS ANTERIOR Origin : upper two thirds of lateral surface of tibia and adjacent interosseous membrane. Insertion: medial surface of medial cuneiform and the base of 1st metatarsal bone. Nerve supply : receive twigs from deep peroneal nerve and recurrent genicular nerve. Action: dorsiflexion of foot at ankle joint and invertor of the foot at midtarsal and Subtalarjoint.
- 6. EXTENSOR HALLUCIS LONGUS Origin: medial part of anteromedial surface of the middle two forth of fibula and adjacent interosseous membrane. Insertion: base of terminal phalanx of great toe. Nerve supply: Deep peroneal nerve. Action: Dorsiflexion of foot at ankle and dorsiflexion of great toe.
- 7. EXTENSOR DIGITORUM LONGUS Origin: upper three fourth of anteromedial surface of fibula, adjacent interosseous membrane and anterior intermuscular septum Insertion: EDL is divided into four tendon on the dorsum of foot. Nerve supply: deep peroneal nerve Action: produce dorsiflexion of ankle joint and dorsiflexion of lateral four toes.
- 11. The common fibular nerve (common peroneal nerve; external popliteal nerve; lateral popliteal nerve is the smaller terminal branch of the sciatic nerve. The common fibular nerve has root values of L4, L5, S1, and S2. It arises from the superior angle of the popliteal fossa and extends to the lateral angle of the popliteal fossa, along the medial border of the biceps femoris. It then winds around the neck of the fibula to pierce the fibularis longus and divides into terminal branches of superficial fibular nerve and deep fibular nerve. Before its division, the common fibular nerve gives off several branches in the popliteal fossa.
- 12. Common peroneal nerve Superficial peroneal nerve: Nerve of lateral compartment of leg Motor branches : peroneous longus peroneous brevis Sensory supply : lateral aspect of lateral 1/3 rd of leg &dorsum of foot , 2nd , 3rd,4th,interdigital clefts Deep peroneal nerve: Nerve of anterior compartment of leg Motor branches : -Tibialis anterior -Extensor hallucis longus -Extensor digitorum longus Peroneous tertius Sensory supply : 1st interdigital clefts
- 14. Before dividing into terminal branches : CPN branches - Cutaneous branches: Lateral sural cutaneous nerve: (lateral cutaneous nerve of calf) - supplies the skin of the upper two- thirds of the lateral side of leg. sural communicating nerve - it runs on the posterolateral aspect of the calf and joins the sural nerve. Articular branches: Superior lateral genicular nerve Inferior lateral genicular nerve Recurrent genicular nerve Motor branches: There is only one motor branch that arises directly from common fibular nerve, the nerve to the short head of the biceps femoris muscle.
- 15. • Fasiculi of the peroneal nerve - larger and have less connective tissue • Fewer autonomic fibers, so in any injury, motor and sensory fibers bear the brunt of the trauma. • More superficial course, especially at the fibular neck • Adheres closely to the periosteum of the proximal fibula VULNERABILITY OF PERONEAL NERVE
- 17. I. Traumatic: • Tendon injuries to dorsiflexors of foot • Neurogenic 4 Causes of Foot Drop •A) Above the level of common peroneal nerve At the thigh : Fracture of shaft of femur. Penetrating injuries. At the hip: Posterior dislocation of hip. Fracture around the hip. Acetabular fractures. At gluteal region : Deep IM injection. At the spine : IVDP Spina bifida Tumors. CNS : Cerebral tumors and space occupying lesion.
- 18. B ) At or below the level of common peroneal nerve Direct injuries: incised and penetrating injuries Fracture & dislocations around knee Fracture of lateral condyle of tibia Fracture/ dislocation of head/neck of fibula , compound fracture of upper 1/3rd of tibia Iatrogenic : •High tibial skeletal traction • Tight plaster around knee • High tibial osteotomy •Total knee replacement Others: Lateral meniscal cyst Exostosis Tumor of head of fibula Lateral meniscal tumour.
- 19. III. METABOLIC: • Diabetes mellitus • Beri beri • Alcoholic neuritis IV. EXOGENOUS TOXIN: • Lead • Arsenic • Mercury 6 II. INFECTIVE: • leprosy • Poliomyelitis • Guillain-Barré Syndrome • Syphilis
- 21. SYMPTOMS 1. Weakness in dorsiflexion and eversion of foot. 2. High stepping gait 3. Sensory loss : Loss of sensation in the areas supplied by peroneal nerve. In the stance phase of foot drop patient, the outer part of fore foot comes in contact with ground first instead of heal. This results in accumulation of stress in the lateral part of fore foot and Causes ulceration.
- 22. High stepping gait due to paralysis of anterior muscles. Foot slap followed by heel strike Toe drag during swing phase Increased hip and knee flexion 18 GAIT OF FOOT DROP
- 23. 1.SIGNS OF SENSORY DENERVATION: Cutaneous sensation is impaired over the lateral aspect of the lower leg and ankle and dorsum of the foot. 2.Sign of motor denervation : • paralysis/weakness: Reduced dorsiflexion and eversion of the foot and toe extension. The patients will compensate by having a steppage gait. • Loss of tone • Areflexia • Insensibility to compression • Atrophy/wasting of muscles involved. • Inversion and plantar flexion are normal. SIGNS:
- 24. Sign of Autonomic denervation : Loss of sweating Vasomotor paralysis: Early- warm/ pink Late - cold /cyanotic Loss of cutaneous ridges and folds. Atrophy of subcutaneous tissues. Trophic ulceration Loss of hair.
- 25. TYPES OF FOOT DROP • Type I – High Above the level of fibular head deep peroneal nerve • TYPE II- LOW Below the level of fibular head superficial peroneal nerve
- 26. • High lesion : total /complete foot drop. • Unable to dorsiflex and invert foot. • Able to do eversion. • Wasting of ant group of muscles. • Loss of sensation over the 1st webspace. 16 • Type I – High Above the level of fibular head - deep peroneal nerve Clinical features of type 1 foot drop
- 27. • Low lesion : incomplete foot drop. • Unable to do eversion. • Able to do dorsiflexion and inversion of the foot. • Wasting of outer half of leg. • Sensation lost over outer leg and foot. 17 Clinical features of type 2 foot drop • TYPE II- LOW Below the level of fibular head - superficial peroneal nerve
- 28. DIAGNOSIS: Plain X-ray : Post-Traumatic - tibial/fibula injury and ankle injury….. MYELOGRAM CT SCAN Magnetic Resonance Imaging (MRI): compressive mass lesion to the peroneal nerve, Spine tumors, IVDP, spina bifida ELECTRODIAGNOSIS : Electromyography (EMG) and nerve conduction study (NCV/NCS ) SD curve (strength duration curves) Tinel sign Autonomic tests Special Investigations
- 29. TINELS SIGN : ASSESSMENT OF RECOVERY: Gentle percussion, from distal to proximal, by a finger or percussion hammer along the course of a injured nerve. A transient tingling sensation should be felt by the patient on the distribution of the injured nerve rather than at the area percussed, and the sensation should persist for several seconds after stimulation. A positive Tinel's sign is presumptive evidence that regenerating axonal sprouts that have not obtained complete myelinization are progressing along the endoneronal tube.
- 30. Special investigation: Leprosy : Bacteriological examination, foot pad culture, histamine test, biopsy, immunological test. Diabetes mellitus - Blood sugar level. Syphilis - Serological test.
- 31. MANAGEMENT OF FOOT DROP
- 32. TREATMENT : • Conservative treatment : shows high incidence of recovery • Splintage – splint knee in 20° of flexion and ankle in 90° for night time • In day time, walking is allowed by using ‘foot- drop appliance’ • Varieties of foot drop appliances: i) dynamic-spring shoe ii) static- back stop shoe 26
- 33. • Ankle foot orthotics (AFO) -support the foot with light-weight leg braces and shoe inserts • Exercises -strengthen the muscle, help to maintain range of motion (ROM) and improve gait • Electrical Functional Stimulations -electrically stimulate the peroneal nerve 27
- 34. SURGICAL MANAGEMENT TENDON TRANSFER SURGERIES: BARR’S TECHNIQUE OBER’S TECHNIQUE KAUFER’S PROCEDURE SRINIVASAN TECHNIQUE TENDO ACHILLIS LENGTHENING PROCEDURES BONE SURGERIES: 1. LAMBRINUDI ARTHRODESIS 2. TRIPLE ARTHODESIS 3.CAMPBELLS post bone block 4.ANKLE ARTHODESIS
- 35. 1. BARR’S TECHNIQUE (anterior transfer of tibialis posterior) cast: long leg - calcaneovalgus- foot 3weeks after 3 weeks --B/K cast- foot-N ;ankle- DF – 6weeks >6WEEKS - remove cast- Rehabilitation 6 months- Double bar foot drop brace
- 36. 2. OBER’S TECHNIQUE • ( tendon passed through ant comparment of leg) • Classic- 3rd metatarsal • HATTS modified obers- medial cuneiform • Post op = barrs
- 37. 3. KAUFER’S PROCEDURE ( split transfer of tibialis post tendon)
- 38. 4. SRINIVASAN TECHNIQUE ( two tailed transfer of tibialis post)
- 39. • Post op: • B/K- foot in 70 deg dorsiflexion • >3weeks- non-weight bearing reeducative exercises Advantage of Srinivasan technique : can correct both foot drop & toe drop
- 40. 5. TENDO ACHILLIS LENGTHENING A. WHITES TECHNIQUE: (open) Posteromedial incision- expose tendo calcaneus Long cast- knee extension ;ankle-dorsiflexion 1ST post op- weightbearing Knee extension – 3weeks Short leg- 3 weeks AFO- ankle in neutral dorsiflexion
- 42. B. HAUSER TECHNIQUE: • Posteromedial incision- expose tendocalcaneus • Plantaris tendon- incised-beneficial • Cast- mid thigh to toe knee-full flexion; ankle-neutral dorsiflexion – 6 weeks >6WEEKS- AFO
- 43. C. PERCUTANEOUS LENGTHENING OF TENDOCALCANEUS • Position: prone knee-E; ankle- DF 3 partial tenotomies 1.medially 2.proximally & medially at musculotendinous junction 3.laterally in between 2 incisions if the Heel in -varus-2 incisions medially if the heel valgus in - 2 incisions laterally After suregery Mx = White technique i.e.. ( long leg casting )
- 45. D. Semi open sliding tenotomy of tendocalcaneus • Position-prone • 2 longitudinal incision of 2cm along the tendocalcaneus • Plantaris tendon- tenotomy • Post op-=Hauser technique
- 47. BONE SURGERIES: 1. LAMBRINUDI ARTHRODESIS 2. TRIPLE ARTHODESIS 3.CAMPBELLS post bone block 4.ANKLE ARTHODESIS
- 48. 1. LAMBRINUDI ARTHRODESIS Indication: Isolated fixed equinus deformity older than 10 years of age C/I : flail foot hip& knee instability requiring brace Lateral x-ray - if ant subluxation of talus present then 2 stage plantar arthodesis Complications : 1. ankle instability 2.residual varus/valgus due to muscle imbalance 3.Pseudoarthrosis of talonavicular joint
- 50. • Long leg Cast & Sutures Removed – 10-14 days • Short leg cast- x –ray satisfactory • Weight bearing allowed after 6weeks • Short leg walking cast applied till - fusion complete(3months)
- 51. 2.TRIPLE ARTHODESIS • Most effective stabilizing procedure in the foot. • Subtalar-calcaneocuboid-talonavicular joints are fused Indicated when most of the weakness and deformity are at the subtalar & mid tarsal joints. • obtain stable& static realignment of foot . • To remove deforming forces. • To arrest progression of deformity . • To Eliminate pain. • To eliminate use of short leg brace/ provide sufficient correction for fitting long leg brace. To obtain near normal correction of foot After Rx: walk with crutches / walker
- 54. 3. CAMPBELL post bone block • Permits lengthening of tendocalcaneus & ankylosing both ankle and subtalar joints • Incision: medial and parallel to TA • FHL retracted to capsule of ankle joint is exposed • Post part of talus and articular surfaces of ankle and subtalar joints- excised. • Turn large flaps of bone distally from the posterior aspect of the tibia and proximally from the superior aspect of the calcaneus, overlapping them successively. • Ilium- large bony bridge across the ankle and subtalar joints • post op: ankle- plaster cast- A/K- foot at right angle >4 weeks- boot cast ( snugly fitting) full weight bearing delayed > 8-12 weeks cast immobilisation- until fusion walking on irregular surfaces will be difficult.
- 55. Turn large flaps of bone distally from the posterior aspect of the tibia and proximally from the superior aspect of the calcaneus, overlapping them successively
- 56. 4. ANKLE ARTHODESIS • Recommended by Barr & Record for Severe paralytic equinus deformity in adults when muscle suitable for transfer are not available. • Subcutaneous plantar fasciotomy & lengthening of Tendo calcaneus followed by ankle arthodesis .
- 57. THANK YOU…