dental abscess lec.pdf
- 2. • Abscess can affect any part of the body. In oral cavity, abscess affects roots of teeth, gum tissue or surrounding structures of the tooth. The experience of purulent build up is intensely painful & can abrade the supporting structures of the tooth leading to damage impossible to rectify.
- 3. What is Dental abscess? • Dental abscess, dentoalveolar abscess, tooth abscess or root abscess is a localized pus collection as a result of a bacterial infection associated with a tooth. • It’s an excruciating infection involving the root of a tooth (periapical abscess) or between the gum & a tooth.
- 4. Types of dental abscess are: 1. Periapical abscess: localized collection of pus at the tip of the root. 2. Gingival abscess: localized pus collection involves only gum tissue. 3. Periodontal abscess: localized pus collection involving bone adjacent to the tooth. 4. Pericoronal abscess: localized abscess involving the gum tissue surrounding the crown of a partially or fully erupted tooth [often associated with lower wisdom tooth]. 5. Combined periodontal/endodontic abscess.
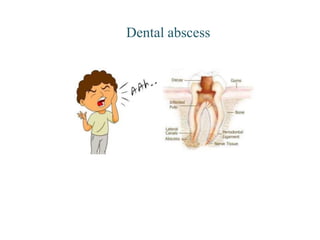
- 5. Periapical abscess: • As the image clearly represents, periapical abscess usually occurs as a result of untreated dental caries that further approaches the pulp & lead to inflammation of pulp due to bacterial invasion. • Periapical abscess is the most common of all the abscesses & usually seen associated with non-vital tooth. If left untreated can affect the surrounding structures of the tooth & eventually lead to extraction of the affected tooth.
- 6. Gingival abscess: • Gingival abscess occurs on the gum line of the tooth. The abscess is often due to external damage to the gum tissue either due to food lodgement or digging the area with a toothpick. • A localized purulent infection that involves themarginal gingiva or interdental papilla
- 8. O Etiology O Acute inflammatory response to foreign substances forced into the gingiva O Clinical Features O Localized swelling of marginal gingiva or papilla O A red, smooth, shiny surface O May be painful and appear pointed O Purulent exudate may be present O No previous periodontal disease
- 9. O Treatment O Elimination of foreign object O Drainage through sulcus with probe or light scaling O Follow-up after 24-48 hours
- 10. For the treatment of Gingival Abscess, the protocol should include the following: O Elimination of the foreign object, through careful debridement. O Drainage through the sulcus with a probe or lightscaling, O Rinsing with warm saline and follow-up after 24-48hours
- 11. Periodontal abscess: • Periodontal abscess is the advanced form of periodontal disease. The affected tooth already has pre-existing pocket & degree of bone loss. Despite of undergoing dental cleaning one can still get this abscess because the infected periodontal pocket contains trapped bacteria’s that tend to multiply & invade within the soft tissue.
- 12. What causes dental abscess? • Our mouth is a domain for over 6 billion bacteria’s, amongst which few are favorable & few are likely to harm one’s wellbeing. Lack o foral hygiene maintenance leads to plaque formation that further tend to decay the teeth & gums. • Dental abscess most commonly occur in cases of untreated cavities. Other possible causes include: 1. Trauma 2. Gingivitis (gum disease) 3. Cracked tooth 4. Food lodgement 5. Incorrect brushing technique 6. Poor oral hygiene
- 13. • Fail to treat the underlying cause can cause an abscess to occur. While none of these factors will directly lead to dental abscess formation. These are the risk factors that increase the likelihood of abscess formation if not treated at the initial stage.
- 14. Symptoms • In case you notice or experience any of these, the following indicates that you need to see your dentist as soon as possible: 1. Severe toothache, persistent in nature that can radiate to the jawbone, ear or neck area 2. Swollen lymph nodes 3. Fever 4. Pain on tapping the affected tooth 5. Unpleasant taste in the mouth 6. Sensitivity to hot or cold 7. Pain on chewing or biting 8. Pimple like bump on the gum or swelling.
- 15. Treatment • Tooth ache & swelling are the common signs of an infected tooth. Tooth abscess can be diagnosed by clinical & radiographic evaluation as well. • Abscess drainage should be initiated as early as possible via root canal treatment, incision & drainage or extraction. • Considerations regarding the treatment depend on: 1. Patient’s preference 2. Prognosis of the tooth 3. Patient’s economic status 4. Strategic value of the tooth
- 16. • In case of restorable tooth root canal treatment can be the mode of treatment. Whereas for non-restorable tooth need to be extracted. • In case of periodontal abscess: once abscess is drained, periodontal pocket need to be cleaned via scaling & root planing to prevent further infections.
- 17. • It’s highly important to see your dentist even if the signs & symptoms subside. The abscess needs to be drained via the treatment option chosen by your dentist. Good oral hygiene practice can reduce the risk of tooth abscess formation. • In case you have any of the above mentioned symptoms, you need to schedule an appointment at Dr. Sachdeva’s Dental Institute. Open cavity is the chief mode of entry of microorganisms into the pulp. If cavity or underlying cause not treated at the right time can lead to major complications.