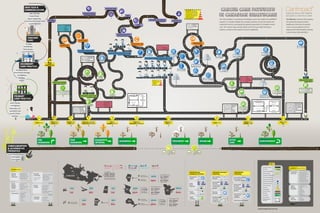
CanIMPACT Clinical Map - Jones
- 1. PREVENTIVE SCREENING INITIAL FP CONCERN/ EXAM/PRESENTATION CONTINUITY WITH FP CANCER DIAGNOSIS BY FP TRANSITIONPREVENTION TRANSFER TO PRIMARY CARE LONG-TERM CARE CONFIRMED SPECIALIST DIAGNOSIS GENETICS CENTRE EMERGENCY ACUTE CARE EMR LABS INTERNAL NETWORKSINTERNET TELEHEALTH PATHOLOGY LAB CANCER REGISTRY INTERNAL MEDICINE EMERGENCY Practice EMR Diagnostic Cycle Medical Test Results Referral LABLAB RxRx Referral RxRx Diagnosis DxRx Remission/ Good outcomeBiopsy Investigations Remission/ Good outcome Problematic outcome Progression/ Recurrence Partial Remission Discharge Cycle End of Life/Hospice/ Home based Care Skilled Nursing Home/ HOSPITAL EMR INCIDENT OR SYMPTOM Rural patients rely heavily on Primary Care for access to all applicable care needs. PATIENT PORTAL NP/Nurse RN/RPN/LPN Family Physician Oncology NurseGPO Oncology Specialist Surgical Oncologist Oncology Nurse Nutritionist GPO Surgical Oncologist Palliative Therapist Patient Navigator Palliative Therapist Radiation Oncologist Occupational Therapist Medication Advisor Oncology Specialist Family Physician Medical Oncologist TREATMENT AFTER CARE REHAB PRIMARY CARE PRACTICE PERI DIAGNOSIS DIAGNOSTIC INTERVAL DIAGNOSIS SURVIVORSHIP PRIMARY CARE TEAM PALLIATIVE CARE CANCER CARE SPECIALIST TEAM MULTIDISCIPLINARY CANCER CARE TEAM Community Clinic Ambulatory Care Genetics Centre Investigations Pharmacy Family Practice SECONDARY CARE PRACTICE Radiology Surgery General Practice Oncology Oncology Practice Investigations TERTIARY CARE INFO TECH & COMMUNICATION Cancer Surgery Cancer Pain Clinic Radiotherapy Oncology Labs & Imaging Mgt Clinical Decision Support Tools Hospital Websites Patient Portal EMR/EHR/PHR COMPLEMENTARY & ALTERNATIVE THERAPIES Homeopathy Naturopathy Ancient Healing Systems Testing for Hereditary & Familial Cancers 50% Breast Cancer cases are screen detected and 50% through Primary Care Breast Cancer patients adhere to Hormonal Treatment for 5-10 years. About 20% Colorectal Cancer patients present symptoms first in Emergency. Lab Tests/Radiology/ Mammogram or other diagnostic tests 43% visit ER due to adverse chemo reactions. Care Planning 5% Breast Cancer patients get Neoadjuvant therapy. Continuity of Care Plan Surgery Radiation Hormone Treatment Clinical Trials Surveillance Chemo Psychosocial Supportive Care Complementary Psychosocial Support Support Groups/ Religious Organizations Psychosocial Supportive Care Surveillance Patient Population - Colorectal/Breast Initial Investigation Burden on Patient Reinforcing Behaviour Symptoms True Diagnosis Inconclusive + - + +- - Treatment Effectiveness End of Life Care Reinforcing Limiting Reinforcing Reinforcing Survivorship Chronic Population Primary Care Family Physicians More Primary care Increased Patient Load More Primary care + + + + + + + + - Increasing the effectiveness of Cancer treatment, grows the population of survivors, who live longer with manageable (but expensive) chronic illnesses. Uncertainty in diagnostic interval can erode FP relationship with potential for adverse effect on survivorship. Care Assistance & Managing Comorbidities The Clinical Map is a synthesis of findings across the modes of CanIMPACT research. It visually models the complex systems of care for breast and colorectal cancers, portraying the general processes of Canadian cancer care. The system map reveals salient clinical issues while aiming to express a sense of the system’s actual complexity. The Mission: Enhance the capacity of community based primary healthcare clinicians to provide care to cancer patients and to improve the links between primary care and specialty providers. 35% Patients require Psychosocial Support 10-12% On-going psychosocial care UNDER CONSTRUCTION Telehealth could be a solution to preventing unnecessary travel for medical consultations with Physicians PRE DIAGNOSIS Psychosocial Support CANCER CARE PATHWAYS IN CANADIAN HEALTHCARE CANCER CARE PATHWAYS IN CANADIAN HEALTHCARE ® RESEARCH SYNTHESIS MAP CANCER CARE PATHWAYS IN CANADIAN HEALTHCARE Nurse/Patient Navigator TREATMENT CONTINUITY STRATEGIES Interoperable Electronic Communication & Information Systems EMR LABS HOSPITAL EMR Multidisciplinary Care Teams (Integrated Practice Units) Psychosocial Support PREVENTION AND DIAGNOSIS STRATEGIES Health System Integration EMR LABS HOSPITAL EMR Patient Activation Health Promotion SURVIVORSHIP STRATEGIES Multicomponent initiatives Interoperable Electronic Communication & Information Systems EMR LABS HOSPITAL EMR Nurse/Patient Navigator & Education Physician Education Survivorship & Primary Care support to “unattached patients” New Colorectal Cancer cases by provinces (2015) 25.1 K New Breast Cancer cases by provinces (2015) 25.2 K Lifetime probablity of Colorectal Cancer M: 1 in 14 F: 1 in 16 Colorectal Cancer Breast Cancer 9200 9800 Lifetime probablity of Breast Cancer High continuity more likely to be screen-detected High comorbidity less likely to be screen-detected F: 1 in 9 25% (MB) 28% (AB) 25% (MB) 28% (AB) Rural ON & MB more likely to be screen-detected than urban. to 25% (MB) 28% (AB) 7-13%7-13%7-13% Screen Detected 28 days28 days screen-detected symptom-detected 28 days 34 days34 days34 days Median Diagnostic Interval ONONON ON immigrants less likely to be screen-detected Ontario Breast Screening Program Diagnostic Assessment Program Colorectal Cancer Breast Cancer 970 860 MBMBMB Colorectal Cancer Breast Cancer 920 780 NSNSNS Nova Scotia Breast Screening Program LEAN on cME 19 days19 days screen-detected symptom-detected 19 days 21 days21 days21 days Median Diagnostic Interval ABABAB Comprehensive Breast Care Program Clinical Breast Health Program eReferral Colorectal Cancer Breast Cancer 3150 3400 7-13%7-13%7-13% 30 days30 days screen-detected symptom-detected 30 days 30 days30 days30 days Median Diagnostic Interval BC immigrants less likely to be screen-detected BCBCBC Colorectal Cancer Breast Cancer 6600 6100 CANADACANADACANADA Colorectal Cancer Breast Cancer 2160 2300 QCQCQC Colorectal Cancer Breast Cancer 120 110 PEIPEIPEI Colorectal Cancer Breast Cancer 560 360 NLNLNL Colorectal Cancer Breast Cancer 770 710 SKSKSK Cancer Related Agencies & NGOs Canadian Partnership Against Cancer Canadian Cancer Society Canadian Breast Cancer Foundation Clinical Colleges Colleges of Physicians, Surgeons, Nursing Canadian College of Family Physicians Licensing Bodies, Professional Standards & Certifiers Communities Faith Communities & Congregations Community groups Voluntary Sector Foundations Support Groups Individuals & Families Persons as Patients Family Members Friends & Social Circle National Policy & Governance Canadian Task Force on Preventive Health Care Federal Ministry of Health Canadian Institutes of Health Research (CIHR) Provincial & Territorial Ministries of Health Provincial Cancer Agencies Provincial Health Regions or Districts Regional Cancer Programs Ontario Institute for Cancer Research STAKEHOLDERS CanIMPACT Research Team Contributors to the map Eva Grunfeld, Univ of Toronto Geoff Porter, Dalhousie Jonathan Sussman, McMaster Julie Easley, Dalhousie June Carroll, Univ of Toronto Patti Groome, Queen’s Bo Miedema, Dalhousie Sharon Matthias, Edmonton Mary Ann O’Brien, U of Toronto Marg Fitch, Univ of Toronto Patient Advisory Committee Marg Fitch, Co Chair Sharon Matthias, Co Chair Dawn Powell Julie Easley Nancy Schneider Margaret Tompson Catarina Versaevel Bonnie Vick Richard Wassersug OCADU sLab Team Peter Jones Prateeksha Singh Smriti Shakdher Legend Type of Care Clinical Role in Journey Clinical Process/Workflow Primary Care Stages Colorectal Cancer Patient Flow Breast Cancer Patient Flow Typical Cancer Patient Flow Info Tech & Communication Secondary Care Practice Primary Care Practice Tertiary Care Recommendation Cancer Clinical Flow Cancer Stages Other Flows Facts & Statistics Qualitative Research Information Copyright (c) 2016 Strategic Innovation Lab, OCAD University
