OSS -PLEURAL EFFUSION - BY OSMAN.pptx
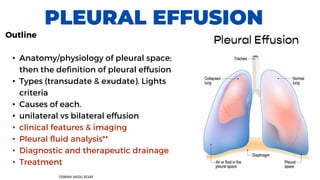
- 1. PLEURAL EFFUSION Outline • Anatomy/physiology of pleural space; then the definition of pleural effusion • Types (transudate & exudate). Lights criteria • Causes of each. • unilateral vs bilateral effusion • clinical features & imaging • Pleural fluid analysis** • Diagnostic and therapeutic drainage • Treatment OSMAN SAIDU SESAY
- 2. Symptoms • Patients with a small pleural effusion (< 300 mL) are often asymptomatic. • Characteristic symptoms - Dyspnea - Symptoms of hypoxia - Pleuritic chest pain (sharp retrosternal pain) - Dry, nonproductive cough - Symptoms of the underlying disease (e.g., fever in empyema, cachexia in cases of malignancy, symptoms of left-sided heart failure Clinical features of Pleural Effusion
- 3. Clinical features of Pleural Effusion Physical exam findings - SIGNS • Inspection and palpation • Asymmetric expansion (may be decreased) and unilateral lagging on the affected side • Reduced tactile fremitus due to fluid in the pleural space • Auscultation • Diminished or absent breath sounds over the area of effusion • There may be bronchial breathing above the effusion, where the lung is compressed • Pleural friction rub (squeaking sound of inflamed pleural layers rubbing together during inspiration and expiration) • Percussion: Stony dull percussion notes; i.e dullness over the area of effusion • With large effusions, there may be tracheal deviation away from the effusion
- 4. Imaging -Chest X-ray Indications • Standard initial imaging modality for detecting pleural effusion. • Lateral decubitus view (most sensitive): allows for detection of fluid collections as small as 5mL Unilateral Pleural Effusion Bilateral Pleural Effusion Supportive findings ⚬ Typically unilateral blunting of the costophrenic angle ⚬ Homogeneous density with a meniscus- shaped margin (meniscus sign) • Large effusion ⚬ Complete opacification of the lung ⚬ Mediastinal shift ⚬ Tracheal deviation away from the effusion (may be due to a space-occupying lesion)
- 6. Ultrasound Useful in identifying the presence of pleural fluid and in guiding diagnostic or therapeutic aspiration. Indications • Quick bedside assessment • Thoracentesis planning Supportive findings: hypoechoic or anechoic collection in the lower margins of the pleural cavity (costodiaphragmatic recess) • Very sensitive: can detect fluid amounts as low as 20 mL • Pleural fluid septations may be present. • Allows for detection of pleural thickening and pleural nodules Thoracic ultrasound is more sensitive than chest X-ray for diagnosing effusions and estimating effusion size
- 7. CHEST CT • Indications: gold standard for small effusions but use is limited because of radiation and contrast exposure • Procedure: chest CT without IV contrast is usually sufficient ⚬ With IV contrast: allows for the detection of underlying malignancy (e.g., metastases and/or primary tumor) ⚬ CT angiogram: helps to identify vascular pathology (e.g., dissection or AVM) • Supportive findings ⚬ Can detect > 3–5 mL of fluid ⚬ Fluid density measurement can help differentiate pleural effusion from empyema and hemothorax [10] ⚬ Disease-specific signs: See “Pleural empyema.”
- 8. Primary pleural fluid analysis Laboratory parameters Transudative effusion Exudative effusion Light criteria Pleural fluid protein/serum protein ratio ≤ 0.5 > 0.5 Pleural fluid LDH/serum LDH ratio ≤ 0.6 > 0.6 Pleural fluid LDH < ⅔ the upper limit of normal serum LDH Pleural fluid LDH > ⅔ the upper limit of normal serum LDHVery high LDH levels, e.g., > 1000 U/L, suggest empyema, malignancy, or rheumatoid effusion. Pleural fluid cholesterol < 45 mg/dL > 55 mg/dL Pleural fluid LDH < 200 U/L > 200 U/L Pleural fluid cholesterol: serum cholesterol ratio < 0.3 > 0.3
- 9. Adjunctive pleural fluid analysis Pleural fluid parameter Suggests transudative effusion Suggests exudative effusion • Physical appearance Clear fluid, Does not froth or form clots Cloudy or straw-colored fluid (may be hemorrhagic in rare cases) Froths when shaken and forms clots when left standing • Specific gravity ≤ 1.016 > 1.016 • pHNormal pH ∼ 7.6 7.4–7.55 < 7.3–7.45 • Glucose ≥ 60 mg/dL < 60 mg/dL • Total protein gradient(i.e., the difference between pleural fluid and serum total protein) > 3.1 g/dL lower than serum total protein < 3.1 g/dL lower than serum total protein • Albumin gradient > 1.2 g/dL lower than serum albumin < 1.2 g/dL lower than serum albumin
- 10. Thoracentesis • is a procedure that removes pleural fluid for diagnostic and/or therapeutic purposes. It is used to relieve symptoms (e.g., dyspnea) and/or obtain pleural fluid for analysis to help determine the underlying cause (e.g., infection, malignancy) • Diagnostic thoracentesis: the sampling(removal of a small amount) of pleural effusion for pleural fluid analysis and identification of the etiology. • Therapeutic thoracentesis: removal of pleural fluid to relieve symptoms (e.g., dyspnea) and treat respiratory failure
- 11. Indications - for Diagnostic thoracentesis • New unilateral effusion of uncertain etiology • Bilateral effusions with atypical findings (e.g., pleuritic chest pain, fever, disparate effusion sizes) • Indications for detailed pleural fluid analysis that impact management (e.g., cytology, culture, and sensitivity) Parapneumonic effusion > 5 cm Indications for Therapeutic Thoracentesis • Large symptomatic pleural effusions in select patients • Pleural effusions causing respiratory failure and/or obstructive shock • Complicated parapneumonic effusion Chest Tube Drainage A chest tube is a flexible plastic tube that is inserted through the chest wall and into the pleural space. It is used to remove air, fluid, pleural effusion, blood, chyle or pus from the intrathoracic space. It is also known as an intercostal catheter
- 12. The treatment of pleural effusion depends on its underlying cause and the severity of symptoms. Observation and monitoring: In some cases, particularly if the pleural effusion is small and asymptomatic, a watchful waiting approach may be adopted. Regular monitoring with imaging tests can help track the effusion's progression. Thoracentesis: it involves the removal of excess fluid from the pleural space using a needle and syringe. Pleural drainage: In cases where the effusion is recurrent, persistent, or malignant, or if a large volume of fluid needs to be drained, a chest tube may be inserted into the pleural space. TREATMENT Medications: Depending on the underlying cause, • Antibiotics are prescribed if the effusion is due to an infection, such as pneumonia. • NSAIDs or colchicine may be used to treat effusions caused by conditions like RA or SLE • Diuretics (like furosemide, etc) can be helpful in managing effusions related to heart failure or kidney disease. Pleurodesis: It involves the fusion of the two layers of the pleura using chemicals or irritants. This procedure aims to create adhesions between the pleural layers, preventing the accumulation of fluid. Indication -Malignant/non- malignant Pleural effusion. Surgical intervention: In certain cases, may involve procedures like VAT Surgery or open thoracotomy. Surgery may be required to remove thickened or infected pleura, repair underlying lung or chest wall abnormalities, or perform biopsies for diagnosis.