Paeds hemato (thalassemia)
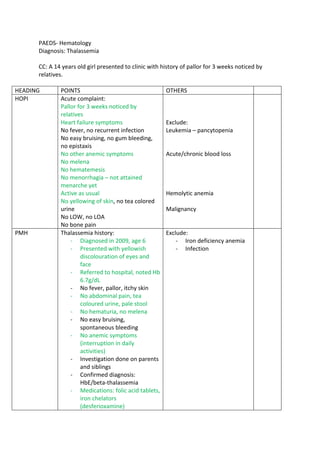
- 1. PAEDS- Hematology Diagnosis: Thalassemia CC: A 14 years old girl presented to clinic with history of pallor for 3 weeks noticed by relatives. HEADING POINTS OTHERS HOPI Acute complaint: Pallor for 3 weeks noticed by relatives Heart failure symptoms No fever, no recurrent infection No easy bruising, no gum bleeding, no epistaxis No other anemic symptoms No melena No hematemesis No menorrhagia – not attained menarche yet Active as usual No yellowing of skin, no tea colored urine No LOW, no LOA No bone pain Exclude: Leukemia – pancytopenia Acute/chronic blood loss Hemolytic anemia Malignancy PMH Thalassemia history: - Diagnosed in 2009, age 6 - Presented with yellowish discolouration of eyes and face - Referred to hospital, noted Hb 6.7g/dL - No fever, pallor, itchy skin - No abdominal pain, tea coloured urine, pale stool - No hematuria, no melena - No easy bruising, spontaneous bleeding - No anemic symptoms (interruption in daily activities) - Investigation done on parents and siblings - Confirmed diagnosis: HbE/beta-thalassemia - Medications: folic acid tablets, iron chelators (desferioxamine) Exclude: - Iron deficiency anemia - Infection
- 2. - Blood transfusion: 4-6 weeks interval, pre and post Hb levels (7 to 9 g/dL) - Complication of blood transfusion: itchiness (IV hydrocortisone pre transfusion), skin pigmentation, not attained menarche, no pubic & axillary hair - Complication of iron chelators: none - Monitoring: infectious screening negative, eye/hearing/ cardiac assessment normal, serum ferritin & thyroid level normal - Follow up: Paediatrics, thalassemia clinic, Ophthalmology, ENT, Medical (echo) No chronic disease No IBD Transfusion related complications: - Immediate: - Infection: HIV, Hep B, Hep C - Iron overload: cardiomyopathy, pericarditis, liver cirrhosis, hypersplenism, delayed growth & puberty, hypothyroidism, diabetes Iron chelators complication: - Desferioxamine (subcutaneous injection): local skin reaction, bone toxicity, ear toxicity, eye toxicity Monitoring: Monthly: Hb, RP, LFT 3 monthly: serum ferritin 6 monthly: infective screening (Hep B/C, HIV, VDRL) Annually: RBS, Echocardiogram, MRI Heart/liver, serum calcium/phosphate, Bone density scan, Hormone level (LH, FSH, Estrogen,Thyroid)
- 3. No worm infestation Drug hx - Folic acid tablet - Iron chelators (Desferral) - L-thyroxine - Vit C tablet - IV hydrocortisone (pre transfusion) Birth hx - Mother anemic, on Tab Iberet - Admitted to NICU for NNJ at day 1 of life, given phototherapy - Negative G6PD screening Diet hx - Avoid beef and Milo - Otherwise, not a picky eater. Consume vegetables and protein everyday Diet for thalassemia patient: - Avoid iron-rich food (red meat, cereals, chocolate, spinach) - Dairy product (rich in calcium) Developmental hx - Up to her age - Not physically active - Develop SOB and easily fatigue Family hx - Both parents: HbE/beta- thalassemia trait, asymptomatic - Brother: trait, asymptomatic - No history of malignancy - Similar symptoms - Carrier HEADING POINTS OTHERS General - Branula connected to IV PBRC - Pale, not icteric - Small built - No thalassemic facies Small for age: plot on growth chart Dark skin: pigmentation (iron overload) Scratch mark Thalassemic facies: frontal bossing, maxillary hyperplasia Bruises at arm: repeated blood transfusion
- 4. Vital signs: afebrile, not tachypneic, not tachycardic Hands, face, neck, mouth: - No clubbing, palmar erythema, leukonychia, koilonychia, palmar pallor - Conjunctival pallor, no scleral jaundice - No lymphadenopathy - Others: Tanner stage 2 breast - No angular stomatitis, no glossitis, pale mucous membrane Stigmata of chronic liver disease: iron overload Stigmata of anemia Delayed growth & puberty: iron overload Abdominal Inspection: - Distended, injection marks at lumbar area Palpation: - Hepatosplenomegaly - Liver: firm edge, smooth, 14cm - Spleen: smooth, firm, traube’s space dull, 7cm Hepatosplenomegaly Lipodystrophy/scar periumbilical: iron chelators Cardiovascular Normal Arrythmia Pericarditis Heart failure – displaced apex beat Respiratory, Neuro Normal Diagnosis: HbE/Beta thalassemia intermedia Justify: present later at age more than 2 years old, less anemia Differentials: - IDA - Leukemia - G6PD deficiency INVESTIGATION EXPECTED FINDINGS OTHERS Diagnosis: 1. FBC Anemia: Hb 6.7 g/dL MCV: microcytic MCH: hypochromic Hct: low Platelet: normal TWC: normal Exclude: Infection Leukemia
- 5. 2. Full blood picture 3. Iron studies 4. Hb Electrophoresis 5. High performance liquid chromatography (HPLC) Hypochromic, microcytic anemia Anisopoikilocytosis Target cells, tear drop cells Low iron High TIBC Mentzer index Low ferritin HbA decreased/absent HbF increased Quantification of HbA2 and HbF Mentzer index (MCV/RBC): <13 for IDA, >13 for thalassemia Serum ferritin: iron overload Monitoring: 1. FBC 2. Iron studies 3. LFT 4. Infective screening Hb: pre and post Platelet count WBC Serum ferritin Serum bilirubin Liver enzymes Hep B/C HIV VDRL Pre transfusion Hb: 9-10g/dL Post transfusion Hb: 13.5-15.5 g/dL Iron overload Iron overload For monitoring Before 1st blood transfusion Iron overload
- 6. 5. Random blood sugar 6. TFT, serum calcium/phosphate/PTH 7. Hormone level (FSH, LH, estrogen) 8. MRI heart, liver, bone density scan Diabetes Iron overload Iron overload Iron overload MANAGEMENT POINTS OTHERS OTHERS Blood transfusion therapy Start when: - Hb <7g/dL on 2 occasions, 2 weeks apart, absence of infection - Impaired growth - Severe bone changes - Hepatosplenomegaly Pre transfusion ix: - Phenotyping (ABO, Rh) - Viral screening - LFT Hypertransfusion regime (thalassemia major) Frequency: once a month Pre transfusion Hb: 9-10g/dL Post transfusion Hb: 13.5-15.5 g/dL Monitoring: - Acute transfusion reaction - LFT Iron overload Iron chelation therapy Start when: - >10 blood transfusion - Serum ferritin > 1000mcg/L 1) DFO (Desferioxamine, Desferal) - Subcutaneous injection - SE: ear, eye, bone toxicitiy, local skin reaction/lipodystrophy 2) DFP (Deferiprone) - Oral TDS
- 7. - SE: agranulocytosis 3) DFX (Deferasirox, Ejade) - Oral OD - SE: renal impairment Diet - Avoid iron rich food (red meat, cereals, chocolate, spinach) - Dairy products - Oral folate supplementation - Vitamin C supplementation Surgical: Splenectomy Bone marrow transplant (hematopoietic stem cell transplantation) Indication: - Evidence of hypersplenism - Massive splenomegaly Pre op immunization - Pneumococcal vaccine - Hib vaccine - Meningococcal vaccine Post op chemoprophylaxis Oral Penicillin Donor: siblings Done before 5 y/o Contraindication: - Hepatomegaly - Iron chelation therapy - Iron overload Hypersplenism: Splenomegaly with persistent leucopenia/thrombocytopenia Risk of splenic rupture/infarct Genetic counselling Relatives at risk Hereditary nature Prevention of transmission Monitoring - Monthly: Hb, RP, LFT - 3 monthly: serum ferritin - 6 monthly: infective screening (Hep B/C, HIV, VDRL) - Annually: RBS, Echocardiogram, MRI Heart/liver, serum calcium/phosphate, Bone density scan, Hormone level (LH, FSH, Estrogen,Thyroid