Hepatitis b virus
•
10 gefällt mir•896 views
Hepatitis B is a viral infection. that attack liver and can cause both acute and chronic infection
Melden
Teilen
Melden
Teilen
Downloaden Sie, um offline zu lesen
Empfohlen
Empfohlen
Weitere ähnliche Inhalte
Was ist angesagt?
Was ist angesagt? (20)
Ähnlich wie Hepatitis b virus
The presentation is all about hepatitis (its causes, prevention, sign & symptoms) and its the importance of world hepatitis day. this day is celebrated to aware people abut hepatitis.World hepatitis day 28 july 2021

World hepatitis day 28 july 2021Associate Professor, B.Pharmacy College, Rampura, Godhra, Gujarat, India
Ähnlich wie Hepatitis b virus (20)
HEPATITIS_B_presentation disease control and management.ppt

HEPATITIS_B_presentation disease control and management.ppt
Bloodborne Pathogens & Disease Transmission by IMWCA

Bloodborne Pathogens & Disease Transmission by IMWCA
Epidemiologic characteristics of Hemocontact Infections. Viral hepatitis B. V...

Epidemiologic characteristics of Hemocontact Infections. Viral hepatitis B. V...
dysfunction of Liver system in body and the nursing intervention to the patient

dysfunction of Liver system in body and the nursing intervention to the patient
Kürzlich hochgeladen
(Deeksha) 💓 9920725232 💓High Profile Call Girls Navi Mumbai You Can Get The Service Of A Mumbai Call Girl At Any Time
WHATSAPP On Here:9920725232
Today call girl service available 24X7*▬█⓿▀█▀ 𝐈𝐍𝐃𝐄𝐏𝐄𝐍𝐃𝐄𝐍𝐓 CALL 𝐆𝐈𝐑𝐋 𝐕𝐈𝐏 𝐄𝐒𝐂𝐎𝐑𝐓 SERVICE ✅
⭐➡️HOT & SEXY MODELS // COLLEGE GIRLS
AVAILABLE FOR COMPLETE ENJOYMENT WITH HIGH PROFILE INDIAN MODEL AVAILABLE HOTEL & HOME
★ SAFE AND SECURE HIGH CLASS SERVICE AFFORDABLE RATE
★ 100% SATISFACTION,UNLIMITED ENJOYMENT.
★ >> 03-05-2024 (GRV)
★ All Meetings are confidential and no information is provided to any one at any cost.
★ EXCLUSIVE PROFILes Are Safe and Consensual with Most Limits Respected
★ Service Available In: - HOME & HOTEL 24x7 :: 3 * 5 *7 *Star Hotel Service .In Call & Out call SeRvIcEs :
★ A-Level (5 star escort)
★ Strip-tease
★ BBBJ (Bareback Blowjob)Receive advanced sexual techniques in different mode make their life more pleasurable.
★ Spending time in hotel rooms
★ BJ (Blowjob Without a Condom)
★ Completion (Oral to completion)
★ Covered (Covered blowjob Without condom
100% SAFE AND SECURE 24 HOURS SERVICE AVAILABLE HOME AND HOTEL SERVICES(Deeksha) 💓 9920725232 💓High Profile Call Girls Navi Mumbai You Can Get The S...

(Deeksha) 💓 9920725232 💓High Profile Call Girls Navi Mumbai You Can Get The S...Ahmedabad Call Girls
Independent Call Girls Hyderabad 💋 9352988975 💋 Genuine WhatsApp Number for Real Meet
WHATSAPP On Here: 9352988975
Today call girl service available 24X7*▬█⓿▀█▀ 𝐈𝐍𝐃𝐄𝐏𝐄𝐍𝐃𝐄𝐍𝐓 CALL 𝐆𝐈𝐑𝐋 𝐕𝐈𝐏 𝐄𝐒𝐂𝐎𝐑𝐓 SERVICE ✅
⭐➡️HOT & SEXY MODELS // COLLEGE GIRLS
AVAILABLE FOR COMPLETE ENJOYMENT WITH HIGH PROFILE INDIAN MODEL AVAILABLE HOTEL & HOME
★ SAFE AND SECURE HIGH CLASS SERVICE AFFORDABLE RATE
★ 100% SATISFACTION,UNLIMITED ENJOYMENT.
★ All Meetings are confidential and no information is provided to any one at any cost.
★ EXCLUSIVE PROFILes Are Safe and Consensual with Most Limits Respected
★ Service Available In: - HOME & HOTEL 24x7 :: 3 * 5 *7 *Star Hotel Service .In Call & Out call SeRvIcEs :
★ A-Level (5 star escort)
★ Strip-tease
★ BBBJ (Bareback Blowjob)Receive advanced sexual techniques in different mode make their life more pleasurable #G05.
★ Spending time in hotel rooms
★ BJ (Blowjob Without a Condom)
★ Completion (Oral to completion)
★ Covered (Covered blowjob Without condom
100% SAFE AND SECURE 24 HOURS SERVICE AVAILABLE HOME AND HOTEL SERVICESIndependent Call Girls Hyderabad 💋 9352988975 💋 Genuine WhatsApp Number for R...

Independent Call Girls Hyderabad 💋 9352988975 💋 Genuine WhatsApp Number for R...Ahmedabad Call Girls
Kürzlich hochgeladen (20)
(Deeksha) 💓 9920725232 💓High Profile Call Girls Navi Mumbai You Can Get The S...

(Deeksha) 💓 9920725232 💓High Profile Call Girls Navi Mumbai You Can Get The S...
Independent Call Girls Hyderabad 💋 9352988975 💋 Genuine WhatsApp Number for R...

Independent Call Girls Hyderabad 💋 9352988975 💋 Genuine WhatsApp Number for R...
Jaipur Call Girls 9257276172 Call Girl in Jaipur Rajasthan

Jaipur Call Girls 9257276172 Call Girl in Jaipur Rajasthan
Nanded Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet

Nanded Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet
Jalna Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet

Jalna Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet
kozhikode Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet

kozhikode Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet
Thoothukudi Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet

Thoothukudi Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet
surat Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet

surat Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet
Patna Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet

Patna Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet
Kochi call girls Mallu escort girls available 7877702510

Kochi call girls Mallu escort girls available 7877702510
Malda Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet

Malda Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet
dhanbad Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet

dhanbad Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet
Mangalore Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet

Mangalore Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet
Sambalpur Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet

Sambalpur Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet
Call Girl in Bangalore 9632137771 {LowPrice} ❤️ (Navya) Bangalore Call Girls ...

Call Girl in Bangalore 9632137771 {LowPrice} ❤️ (Navya) Bangalore Call Girls ...
ooty Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet

ooty Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet
Erode Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet

Erode Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet
Top 20 Famous Indian Female Pornstars Name List 2024

Top 20 Famous Indian Female Pornstars Name List 2024
neemuch Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet

neemuch Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet
Bareilly Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet

Bareilly Call Girls 👙 6297143586 👙 Genuine WhatsApp Number for Real Meet
Hepatitis b virus
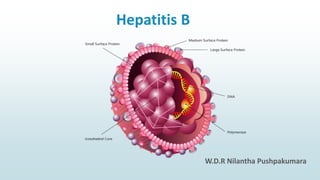
- 1. Hepatitis B W.D.R Nilantha Pushpakumara
- 2. Objectives • To determine what is hepatitis B ? • Transmission of hepatitis B virus • To determine symptoms after infection of hepatitis B • Preventive measures that can be taken to avoid transmission
- 3. Content ➢ What is hepatitis B ➢ Epidemiology of hepatitis B ➢ Causes for hepatitis B ➢ Transmission of hepatitis B virus ➢ Common ways of hepatitis B transmission ➢ Symptoms ➢ Diagnosis ➢ Treatment ➢ Prevention
- 4. What is Hepatitis B • Hepatitis B is a viral infection • that attack liver and can cause both acute and chronic diseases • It is the most serious type of viral hepatitis • Majority of patients with chronic HBV (CHB) infection will have chronic liver disease • Some with CHB infection develop a primary liver cancer, hepatocellular carcinoma (HCC) later in life
- 5. Hepatitis B in the World • Hepatitis B virus (HBV) infection is a global public health problem • 2 billion people have been infected • It is estimated that there are 248 million HBV carriers in the world (positive for hepatitis B surface antigen [HBsAg]) • 1 million people die each year from hepatitis B and its complications • Approximately 2 people die each minute from hepatitis B
- 6. In Sri Lanka • prevalence of HBV infection in Sri Lanka is estimated to be less than 2%
- 7. What causes hepatitis B ? • It is caused by hepatitis B Virus • It is a DNA virus
- 8. Transmission of hepatitis B (HBV) • The virus is highly contagious • Transmitted through contact with the blood or other body fluids of an infected person • Hepatitis B virus can survive outside of the body for at least 7 days • It is an important occupational hazard for health care workers
- 9. Concentration of Hepatitis B Virus in Various Body Fluids High Moderate Low/Not detectable Blood Semen Urine Serum Vaginal fluid Faeces Wound exudate Saliva Sweat Tears Breastmilk
- 10. Most common ways of hepatitis B transmission include : • Sexual contact • Sharing of injecting equipment (used for injecting drugs) • Needlestick injuries in a health care setting • Reuse of unsterilized or inadequately sterilized needles • Sharing personal items such as razors, toothbrushes, or hair and nail clippers • Perinatal Transmission Congenital or Vertical transmission is quite common from carrier mothers The risk to babies is high if the mother is HBeAg positive (60- 90%) and low if Negative (5-15%)
- 11. Needle stick injury sharing injecting drugs
- 12. unsterilized tattooing equipment contamination vaccine equipment unsterilized body piercing equipment
- 13. • Hepatitis B does NOT spread by contaminated food or water, and cannot spread through casual or social contact such as kissing, sneezing or coughing, hugging, or eating food prepared by a person with hepatitis B High Risk Groups • Injecting drug users • Sex workers • Men who have sex with men • Medical and paramedical personnel • People from endemic regions • Hemophiliacs and other patients requiring blood and blood product treatment
- 14. What are the symptoms • Feeling very tired • Mild fever • Headache • Loss of appetite • Nausea • Abdominal pain • Tan-colored bowel movements (stools) • Dark urine • Yellowish eyes and skin (jaundice). Jaundice usually appears only after other symptoms have started to go away
- 15. • Hepatitis B can also cause a chronic infection • This can later develop to cirrhosis or hepatocellular carcinoma
- 16. Diagnosis • Laboratory confirmation is essential • Number of blood tests are available to diagnose and monitor infected people • These tests can distinguish between chronic and acute infection • Laboratory detection mainly focuses on detection of Hepatitis B surface antigen • All donated blood is screened for Hepatitis B
- 17. Treatment • No specific treatment for acute Hepatitis B • Maintaining comfort and adequate nutrition balance is essential • Chronic infection is treated with oral antiviral agents • These medicines can slow the progression of cirrhosis, reduce liver cancers and improve the life span
- 18. Prevention To avoid transmission of hepatitis B: • consider being vaccinated • practice safer sex (use a condom) • wash hands after touching blood or body fluids • wear disposable gloves if giving someone first aid, or cleaning up blood or body fluids • avoid sharing toothbrushes, razors, needles, syringes, personal hygiene items and grooming aids or any object that may come into contact with blood or body fluids
- 19. • Use new and sterile injecting equipment for each injection • Cover all cuts and open sores with a band aid or bandage • Wipe up any blood spills and then clean the area with household bleach • Throw away personal items such as tissues, menstrual pads, tampons and bandages in a sealed plastic bag.
