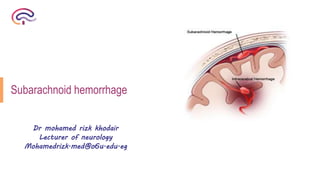
SAH
- 1. Subarachnoid hemorrhage Dr mohamed rizk khodair Lecturer of neurology Mohamedrizk.med@o6u.edu.eg
- 2. Definition Extravasation of blood into the subarachnoid space
- 3. Etiology of SAH: Ruptured saccular aneurysm (75%): - M=F, 5th or 6th decade, with elevated BP. - Usually, congenital berry aneurysms in circle of Willis. -Sites: 40% Anterior Communicating artery 30% posterior communicating 20% MCA 10% posterior circulation - 2-3% mycotic aneurysm (especially infective endocarditis). Arteriovenous Malformation (AVM) (10%): - M >F, 2nd to 4th decades, or other vascular malformations Other less common causes: Hemostatic failure Cerebral vasculitis Brain tumors Trauma Drug abuse
- 4. Risk Factors: a) Hypertension. b) Smoking, alcohol. c) Family history. d) Polycystic kidneys, Ehlers-Danlos Type IV, pseudoxanthoma elasticum, fibromuscular dysplasia.
- 5. Clinical Features: Thunderclap Headache: Acute, paroxysmal, and sudden in onset, "worst headache in my life". Develop in seconds; achieve maximal intensity in minutes, and last hours to days (6 - 72). ■ 10 - 43% of patients have a warning leak (sentinel headaches an mild to moderate in intensity, usually occur within 2 weeks of overt SAH, and are not accompanied by other neurological symptoms). Loss of consciousness: in about 50% of cases Partial or generalized seizures
- 6. Focal symptoms & signs if: Associated ICH Local pressure of aneurysm (Ex, Post com art aneurysm compress 3rd nerve). Cerebral ischemia Meningismus: Nuchal stiffness, especially in flexion, may be absent in deep coma. Kernig's sign (flex thigh to 90" with knee bent, then straighten knee, positive sign if this causes pain in the hamstrings) Brudzinski's sign (flex patient's neck, involuntary hip flexion is a positive sign). Raising leg sign (Lasègue’s sign). Ocular Hemorrhage: Between retina & vitreous. Subhyaloid Hemorrhage: blood seen near the optic disc obscuring the retinal vessels Irritability or photophobia Sudden death
- 7. Physical Findings: Nuchal stiffness. Papilledema Diminished consciousness Third nerve palsy. Bilateral weakness in legs. Sixth nerve palsy Aphasia, hemiparesis Nystagmus or ataxia. Visual neglect Retinal & subhyaloid hemorrhage.
- 8. Diagnostic approach A. Non contrast CT scan: 1. The clinical diagnosis of SAH is best confirmed with brain CT. Sensitivity: 95 -98% sensitivity of CT scanning within 12 hours. 2. CT confirms the presence of SAH and hydrocephalus, intraparenchymal hematoma, intraventricular hemorrhage, or subdural hemorrhage.
- 9. B. Lumbar Puncture: Indication : Classic history of SAH and negative noncontract CT. Should never be done prior to CT scanning. Finding : Three tube test: should see a in traumatic tap versus steady level of RBCs in true SAH Opening pressure (>20 cm H20) seen in 60% of cases. Xanthochromia: □ Represents lysis of RBCs with degradation of heme products into bilirubin □ Present as early as 4-6 hours after SAH and persist for 2-3 weeks. □ Detected by centrifugation or spectrophotometry which is more sensitive. Contraindication : 1) Infection at the site. 2) Coagulopathy, drug induced or otherwise. 3) Raised ICP particularly with posterior fossa pathology. Risk : rebleeding , herintation
- 10. C. Magnetic Resonance Imaging (MRI) brain: 1. The most sensitive sequences were FLAIR and T2* (gradient echo). 2. The sensitivity of T2* was 94% under 4 days from the ictus and 100% between 4 &14 days. D. Angiography: Indication 1) Positive CT or lumbar puncture. 2) Screening in selected circumstances: a. Positive family History. b. Inherited condition associated with incidence of intracranial aneurysms.
- 11. Complications Neurological complications Neurological complications 1) Rebleeding: Risk factors of rebleeding Uncontrolled blood pressure Fibrinolysis of clot around the ruptured aneurysm
- 12. 2) Vasospasm: Def Clinical or symptomatic vasospasm: Delayed ischemic neurological deficit (DIND) Radiographic vasospasm: On cerebral angio arterial narrowing with slowing of filling Timing Occurs 4 to 14 days after hemorrhage. Spontaneously resolve over the next 7days. Risk factors 1) Poor initial clinical state 2) Large SAH or IVH 3) Increased age 4) Angiographic dye 5) Hypertension 6) Hypotension Mech Unknown but may be: Direct effect of blood on the adventitia of the artery Release of VC sub (serotonine, PGs) from vessel wall or blood clot C/P Causes infarction in 30% of patients (Spasm of major arteries stroke syndromes). Diagnosis 1) Angiography: arterial narrowing with slowing of filling. 2) Transcranial Doppler: narrowing of arterial lumen & blood flow velocity.
- 13. 3) Seizure: 4) Hydrocephalus: a. Immediate: Within 3 days, due to intraventricular blood. Ttt by ventriculostomy b. Delayed (subacute): Develops over a few days or weeks progressive drowsiness or slowed mentation (abulia) with incontinence, Due to pia-arachnoid adhesions or permanent impairment of the arachnoid granulations. 5) Others: - Brain edema. - Intracerebral hematoma. - Cognitive & personality changes.
- 14. Systemic complications a. Neurogenic pulmonary edema. b. Cardiac ECG changes: • Prolonged QT, ST segment or T wave changes. • Arrhythmias especially ventricular tachycardias. c. Hypertension: due to pain, ↑catecholamines. d. GIT hemorrhage. e. Hyponatremia: due to Syndrome of Inappropriate ADH Secretion (SIADH) , Cerebral salt-wasting syndrome
- 15. Differential diagnosis: Differential diagnosis of sudden unexpected headache Sudden severe headache with neck rigidity Sudden severe headache without neck rigidity 1) SAH: Abrupt & reach maximum within seconds Diffuse & poorly localized spread to back of head, neck & back (as blood track down the spinal arachnoid space) 1) Migraine: Preceeded by aura Unilateral, throbbing Associated with photophobia 2) Meningitis/ encephalitis: Less abrupt over 1-2days Associated with high fever, tachycardia, seizures 2) Post-traumatic headache: due to Soft tissue damage after injury Dilatation of intracranial vessels pulsating headache worsen with head movement, sneezing or exertion 3) Stroke: Cerebellar stroke: sudden severe headache + nausea, vomiting + vertigo, ataxia Intraventricular hemorrhage: may mimic SAH 3)Thunderclap headache 4) Acute obstructive hydrocephalus
- 16. Treatment 1. Hospitalization: ICU monitoring Bed rest in dark quiet room 2. General Management: as stroke
- 17. 3. Medical management: 1`-Analgesics Codeine 30-60mg/2-3hr Morphine 2-3mg IV/2-3hr Acetylsalicylic acid is CI 2-Sedation As phenobarbital 30-60mg IV/6hr prophylaxis against seizures & bl pressure Over sedation is CI 3-Anti-emetics Avoid Phenothiazine which lower seizures threshold. 4-H2 blokers risk of stress uler 5-Constipation 6-Nimodipine 60mg/4hr
- 18. 4. Surgical management Ruptured saccular aneurysm Neurosurgial clipping Endovasular coiling Aim Exclude the aneurysm from circulation Promote thrombosis of the aneurysm Tecq Open craniotomy with placement of 1 or more clips on aneurysmal neck Placement of 1 or more platinum coils via intrarterial catheter Advant The definitive ttt High efficacy Diagnostic & therapeutic Craniotomy not needed Disadv Requires craniotomy Clip may damage neural or vascular structures High short-term mortality (31%) & morbidity Risk of vessel perforation 24% mortality.
- 19. C. Specific Management: 1) Vasospasm: a) Nimodipine (60 mg orally q 4 h) improves outcome (SE; hypotension). b) "Triple-H" therapy (hypertension, hemodilution, and hypervolemia). c) Plasma volume expansion / dopamine --> raise arterial pressure -> increase cerebral perfusion; requires monitoring of BP and CVP. d) MgS04; inhibit vasospasm. e) Endovascular: - Percutaneous transluminal angioplasty (balloon dilatation) 2) Rebleeding: prophylactic; a. Avoid ↑ BP, cough, straining. b. Mild sedation. c. Short term antifibrinolytic. d. Early surgical treatment. 3) hydrocephalus: a. Acute hydrocephalus; may clear spontaneously or require ventricular drainage b. Chronic hydrocephalus; ventricular shunting. 4) Increased ICP: a. Emergent ventriculostomy b. Medical therapies: mild hyperventilation, mannitol, and sedation.
- 20. Monitoring patient by: 1) Clinical examination. 2) Continuous ECG. 3) Follow up; BP, electrolytes, fluid balance. 4) TC
