Acute Lower Limb Ischaemia.pptx
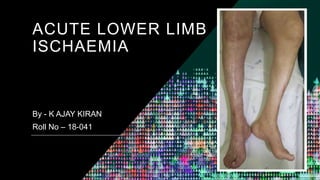
- 1. ACUTE LOWER LIMB ISCHAEMIA By - K AJAY KIRAN Roll No – 18-041
- 2. Definition • Sudden occlusion of an artery. • Sudden decrease in limb perfusion that causes a potential threat to a limb viability • Mainly Caused by an Embolus • It may also happens when Thrombosis occurs on an atherosclerotic plaque. • Although the outcome is usually less dramatic because collaterals are likely to have developed in Chronic arterial stenosis.
- 3. Aetiology of Acute Lower Limb Ischaemia I EMBOLISM • Atrial fibrillation • Mural thrombosis • Vegetations • Proximal aneurysms • Atherosclerotic plaque
- 4. II Thrombosis • Atherosclerosis • Popliteal aneurysm • Bypass graft occlusion • Endovascular stent or stent graft occlusion • latrogenic (localised arterial dissection post endovascular intervention, e.g. arterial closure device failure) • Thrombotic conditions
- 5. III Rare causes • Dissection • Trauma (including iatrogenic) • Illicit drug use • External compression • Popliteal entrapment • Cystic adventitial disease • Iliac endofibrosis
- 6. Embolic occlusion • An embolus is an object that has become lodged in a vessel causing obstruction having been carried in the bloodstream from another site. • It is often a thrombus that has become detached from the heart or a proximal vessel.
- 7. •Sources of emboli include Left atrium in Atrial fibrillation Left ventricular mural thrombus following MI Vegetations on heart valves in infective endocarditis Thrombi on atherosclerotic plaque • Emboli may lodge in any vessel and produce Ischaemia cause Ischaemic symptoms or gangrene and resulting in Critical Limb Ischaemia
- 8. Clinical outcome after Acute Lower Limb Ischaemia
- 9. Clinical Features • Embolic arterial occlusion is an emergency that requires immediate treatment • Ischaemia between 6-12 hours is partly reversible but beyond 12 hours is usually irreversible and results in limb loss • The limb is cold and the toes cannot be moved, which contrasts the venous occulsion when muscle function is not affected.
- 10. • The sudden dramatic symptoms in the form of 6Ps • Pain • Pallor • Paralysis • Loss of Pulsation • Paraesthesia • Poikilothermia
- 11. • The diagnosis can be made clinically in a patient who has no history of intermittent claudication and has a source of emboli. • Suddenly develops severe pain – unbearable, burning and bursting type. • Limb becomes pale – cold and mottled • Movement becomes progressively more difficult and sensation is lost and followed by total paralysis.
- 12. • Pulses are absent distally but the femoral pulse may be palpable , characteristically peripheral pulses below the level of embolism are not palpable. • Numbness of the limb – Paraesthesia – If untreated, necrosis of the muscles followed by gangrene of the limb can occur within a few hours i.e., 6-24 hours
- 13. Thrombosis • Thrombosis is the of formation of solid mass in circulation from the constituents of flowing blood, the mass itself is called a thrombus. • Thrombi can lodge in a blood vessel and block the flow of blood. • Depriving the tissues of normal blood flow nad oxygen, • Resulting in damage and destruction or even death of the tissue.
- 14. Arterial Trauma • Also causes acute limb Ischaemia. • The causes are - Pressure on a major artery by an angulated bone. - Intimal rupture of a major artery due to fracture or dislocation. - Injury to a major artery by a bone fragment. - Supracondylar fracture of femur. - Dislocated knee.
- 15. INVESTIGATIONS • Acute limb Ischaemia is a surgical emergency and the diagnosis is usually clear from History and Examination.
- 16. •Blood examination - Hb, RBC count, WBC count, ESR, CRP, Platelet count, FBS , HbA1c Lipid Profile – Total cholesterol HDL, LDL and Triglycerides. Serum – Lactate, Urea, creatinine, and electolytes. • ECG and Echocardiogram • Chest X ray
- 17. Duplex Ultrasound • Non invasive technique uses – Doppler with B mode ultrasound to provide an image of vessels. • Locate anatomical lesion and degree of stenosis. • Arterial waveforms assessed to detect the degree of stenosis or occlusion. • Normal elastic arteries – Triphasic waveforms • Lesion of moderate stenosis (50% reduction ) – Biphasic waveforms • More than 70% stenosis – Monophasic waveforms. Imaging Modalities
- 18. • It allows both the visualisation of vessels and detailed assessment of waveforms and blood flow. • Change in the peak systolic velocity (PSV) – indicate the degree of stenosis. • PSV is measured in the normal artery proximal to stenosis and then within the stenosis.
- 19. • Combination of PSV, waveform assessment and visualisation of the artery provides useful information on the severity of stenosis. • Accurate, cost effective and safe • Aortoiliac segment can be difficult to visualize particularly in obese patients – CT angiogram useful.
- 20. Digital Subtraction Angiography • Standard investigation for Acute Limb Ischaemia. • Image is digitalised by computer and background ( bone, soft tissues ) removed to provide clear images. • It should be chosen in such a way that both inflow and outflow can be evaluated. • Intra-arterial vasodilators can be used to reduce vasospasm in the vessels distal to the site of occlusion, and thus enhance visualisation of the distal arterial bed. • Patients with severe renal insufficiency, carbon dioxide angiography may be considered
- 21. CT & MR Angiography – • Useful where duplex ultrasound is not possible (intrathoracic arteries) or produces poor image (Aortoiliac segment). • MR has the added advantage of avoiding the need for ionizing radiation and iodinated contrast . • MRA now the first line investigation for PVD.
- 22. Staging of Acute Lower Limb Ischaemia
- 23. TREATMENT
- 24. Goals of Treatment • Restoration of blood flow • Preservation of limb and life • Prevention of recurrent thrombosis
- 25. Approach to Acute Lower Limb Ischaemia
- 27. • -> Immediate administration of 5000 U of HEPARIN IV can reduce the extension and maintain patency of surrounding vessels until the embolus can be treated. • -> Opioid analgesic for the relief of pain is essential because it is severe and constant. • Embolectomy and Thrombolysis are the available treatments.
- 28. EMBOLECTOMY • Local or GA may be used • The artery, bulging with clot , is exposed and held in silastic vessel loops. • Through a transverse incision the clot begins to extrude and is removed, together with the embolus, with help of a FOGARTY Balloon catheter.
- 29. • The Catheter with its balloon tip, is introduced both proximally and distally until is deemed to have passed the limit of the clot. • Balloon is inflated and catheter withdrawn slowly together with obstructing material. • Procedure repeated until bleeding occurs
- 30. • Angiogram is performed in the operating theatre at end of procedure to ensure that flow to the distal legs has been restored. • Postoperavtively , HEPARIN therapy is continued until long term anticoagulantion with warfarin is established to reduce the chance of further embolism
- 31. A A Fogarty catheter is inserted through an arteriotomy in the common femoral artery and fed distally down the superf icial femoral artery and through the embolus. B The balloon is inflated and the catheter withdrawn, removing the embolus; the deep femoral and iliac arteries are similarly treated.
- 33. THROMBOLYSIS • At the arteriography of Ischaemic limb a narrow catheter is passed into the occluded vessel and left embedded within the clot • Tissue Plasminogen Activator is infused through the catheter and regular arteriogram are carried out to check the extent of lysis . In succesful cases it is achieved within 24 hours • Method should abandoned if there is no progression of dissolution of clot with time.
- 34. Slow infusion • Streptokinase 5000 units/hour • Tissue plasminogen activator (t-PA) 0.5 mg/hour • Urokinase 4000 IU/min for 2 hours, then 2000 IU/min for 2 hours, then 1000 IU/min Pulsed spray • t-PA 0.3 mg per pulse every 30 seconds • Urokinase 5000 IU per pulse every 30 seconds High-dose bolus • t-PA 5-mg bolus every 10min three times, then 3.5mg/hour for up to 4 hours, then (if required) as for slow infusion Suggested drug regimens for thrombolysis
- 35. A-Before thrombolysis B-During successful lysis ANGIOGRAM OF AN OCCLUDED POPLITEAL ARTERY
- 36. Contraindications to THROMBOLYSIS • Active internal bleeding • Pregnancy • Stroke within 2 months • Transient ischaemic attack within 2 months • Known intracerebral tumour, aneurysm or arteriovenous malformation • Severe bleeding tendency
- 37. • Craniotomy within 2 months • Vascular surgery within 2 weeks • Abdominal surgery within 2 weeks • Puncture of a non-compressible vessel or biopsy within 10 days • Previous gastrointestinal haemorrhage • Trauma within 10 days
- 38. Compartment Syndrome • Limbs that have been subject to sudden ischaemia followed by revascularisation, oedema is likely. • Muscles swell within confined fascial compartments and this can itself be a cause of tissue ischaemia, • Both local muscle necrosis and nerve damage due to pressure, and systemic effects such as renal failure secondary to the liberation of muscle breakdown products.
- 39. • Liberal concomitant usage of fasciotomy following revascularisation of a prolonged ischaemic limb is advis able. • Classical clinical picture is of severe pain out of proportion with clinical findings worsens with time, despite appropriate analgesia.
- 40. • Patient often complains of numbness/paraesthesia. • On examination limb reveals a tense compartment with passive flexion and extension of muscles causing pain. • Treatment is urgent compartment fasciotomy to release the compression.
- 41. ANGIOPLASTY • Percutaneous transluminal angioplasty is indicated in short stenotic lesions in large vessels – in iliac and femoropopliteal lesions • The ballon catheter is introduced percutaneously over a guidewire across the lesion.
- 42. • Under fluoroscopic control, the balloon is dilated until satisfactory widening of the lumen is achieved • This procedure is relatively safe and simple. • Immediate IV infusion of HEPARIN – 10000 IU is necessary to reduce the extension of the thromboembolism
- 44. Source • Bailey and Love’s – Short Practice of Surgery • European Society for Vascular Surgery (ESVS) 2020 Clinical Practice Guidelines on the Management of Acute Limb Ischaemia • Manipal Manual of Surgery • S Das – Clinical Surgery
- 45. Thank You