Urinary_System-1.ppt
- 2. 27-2 General Structure and Functions of the Urinary System General Concept: Waste products accumulate in blood Are toxic Must be removed to maintain homeostasis Urinary System organs remove waste products from the blood then from the body Major homeostatic system
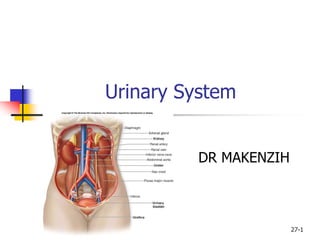
- 3. 27-3 General Structure and Functions of the Urinary System Organs of the Urinary System: Kidneys Ureters Urinary Bladder Urethra Primary organs: kidneys filter waste products from the bloodstream convert the filtrate into urine. The Urinary Tract: Includes: ureters urinary bladder urethra Because they transport the urine out of the body.
- 4. 4
- 5. 5
- 6. 6
- 7. 27-7 Functions of the Urinary System Removing waste products from the bloodstream. Storage of urine. the urinary bladder is an expandable, muscular sac that can store as much as 1 liter of urine Excretion of urine. Blood volume regulation. the kidneys control the volume of interstitial fluid and blood under the direction of certain hormones Regulation of erythrocyte production. as the kidneys filter the blood, they are also indirectly measuring the oxygen level in the blood Erythropoietin (EPO): hormone produced by kidney Released if blood oxygen levels fall Stimulates RBC production in red bone marrow
- 8. 27-8 Kidneys: Gross and Sectional Anatomy Retroperitoneal Anterior surface covered with peritoneum Posterior surface against posterior abdominal wall Superior pole: T-12 Inferior pole: L-3 Right kidney ~ 2cm lower than left Adrenal gland on superior pole
- 9. 9
- 10. 27-10 Kidneys: Gross and Sectional Anatomy Hilum: concave medial border Renal sinus: internal space Houses blood vessels, lymphatic vessels, nerves Houses renal pelvis, renal calyces Also fat
- 11. 27-11 Kidneys: Gross and Sectional Anatomy Surrounding tissues, from deep to superficial: Fibrous capsule (renal capsule) Dense irregular CT Covers outer surface Perinephric fat (adipose capsule) Also called perirenal fat Completely surrounds kidney Cushioning and insulation Renal fascia Dense irregular CT Anchors kidney to posterior wall and peritoneum Paranephric fat Between renal fascia and peritoneum
- 12. 12
- 13. 27-13 Kidneys: Gross and Sectional Anatomy Sectioned on a coronal plane: Renal Cortex Renal arches Renal columns Renal Medulla Divided into renal pyramids 8 to 15 per kidney Base against cortex Apex called renal papilla
- 14. 27-14 Kidneys: Gross and Sectional Anatomy Minor calyx: Funnel shaped Receives renal papilla 8 to 15 per kidney, one per pyramid Major calyx Fusion of minor calyces 2 to 3 per kidney Major calyces merge to form renal pelvis Renal Lobe Pyramid plus some cortical tissue 8 to 15 per kidney
- 15. 15
- 16. 16
- 17. 27-17 Blood Supply to the Kidney About 20 to 25% of cardiac output to kidneys Path: Renal artery to segmental arteries to interlobar arteries to arcuate arteries to interlobular arteries to: Afferent arteriole to glomerulus to efferent arteriole to peritubular capilaries and vasa recta
- 18. 18
- 19. 27-19 Blood Supply to the Kidney Blood plasma is filtered across the glomerulus into the glomerular space. Once the blood plasma is filtered blood leaves the glomerulus enters an efferent arteriole. efferent arteriole is still carrying oxygenated blood a gas and nutrient exchange with the kidney tissues has not yet occurred.
- 20. 27-20 Blood Supply to the Kidney The efferent arterioles branch into one of two types of capillary networks: peritubular capillaries vasa recta these capillary networks are responsible for the actual exchange of gases and nutrients Peritubular capillaries: primarily in cortex Vasa recta: surround the thin tubes that project into the medulla.
- 21. 27-21 Blood Supply to the Kidney Path for veins: Interlobar veins to arcuate veins to interlobar veins to the renal vein
- 22. 22
- 23. 27-23 Nephrons The functional filtration unit in the kidney. Consists of the following: Renal corpuscle Glomerulus Glomerular capsule (Bowman’s capsule) Proximal convoluted tubule (PCT) Nephron loop (loop of Henle) Ascending loop of Henle Descending loop of Henle Distal convoluted tubule (DCT) collectively called the renal tubule In both kidneys: approximately 2.5 million nephrons. Are microscopic: measure about 5 centimeters in length.
- 24. 27-24 Nephrons Cortical Nephrons Near peripheral edge of cortex Short nephron loops Have peritubular capillaries Juxtamedullary nephrons Near corticomedullary border Long nephron loops Have vasa recta
- 25. 25
- 26. 27-26 Urine Formation Three processes Filtration Renal corpuscle: forms filtrate From blood to tubule Reabsorption Mostly PCT Water and salt: rest of nephron From tubule to blood Secretion From blood to tubule
- 27. 27-27 Renal Corpuscle Vascular pole Afferent and efferent arterioles Tubular pole Connects to PCT Two structures: Glomerulus and glomerular capsule Glomerulus Capillary bed High pressure fenestrations
- 28. 27-28 Renal Corpuscle Glomerular Capsule Parietal layer Simple squamous epithelium Visceral layer Podocytes Pedicels Filtration slits Capsular space (Bowman’s capsule): location of filtrate Filtration membrane Fenestrations Filtration slits
- 29. 29
- 30. 30
- 31. 27-31 Proximal Convoluted Tubule Begins at tubular pole of the renal corpuscle. Cells: simple cuboidal epithelium actively reabsorb from the filtrate: almost all nutrients (glucose and amino acids) electrolytes plasma proteins Osmosis: reabsorption of 60% to 65% of the water in filtrate. Have microvilli Solutes and water: moved into blood plasma via the peritubular capillaries.
- 32. 27-32 Nephron Loop (loop of Henle) originates at end of proximal convoluted tubule projects toward and/or into the medulla. Each loop has two limbs. descending limb: from cortex toward and/or into the medulla ascending limb: returns back to the renal cortex
- 33. 33
- 34. 34
- 35. 27-35 Distal Convoluted Tubule begins at the end of the thick ascending limb of the nephron loop adjacent to the afferent arteriole (important physiologically) Juxtaglomerular apparatus. primary function: Secretion From blood plasma to filtrate. secretes ions potassium (K+) acid (H+) Reabsorption of water also occurs: influenced by two hormones Aldosterone antidiuretic hormone (ADH).
- 36. 27-36 Collecting Collecting Ducts Function in a well hydrated person: transport the tubular fluid into the papillary duct and then into the minor calyx. Function in a dehydrated person: water conservation more-concentrated urine is produced. ADH can act on the collecting duct epithelium Cells become permeable to water Water moves from filtrate into blood plasma Involves vasa recta.
- 37. 27-37 Innervation of the Kidney innervated by a mass of autonomic nervous system fibers called the renal plexus. The renal plexus accompanies each renal artery enters the kidney through the hilum.
- 38. 27-38 Urinary Tract : Ureters long, fibromuscular tubes conduct urine from the kidneys to the urinary bladder. average 25 centimeters in length retroperitoneal. ureters originate at the renal pelvis extend inferiorly to enter the posterolateral wall of the base of the urinary bladder. wall is composed of three concentric tunics. mucosa muscularis adventitia.
- 39. 27-39 Urinary Tract – Urinary Bladder The urinary bladder: expandable, muscular container serves as a reservoir for urine positioned immediately superior and posterior to the pubic symphysis. in females the urinary bladder is in contact with the uterus posterosuperiorly and with the vagina posteroinferiorly. in males it is in contact with the rectum posterosuperiorly and is immediately superior to the prostate gland. is a retroperitoneal organ. when empty exhibits an upside-down pyramidal shape. Filling with urine distends it superiorly until it assumes an oval shape.
- 40. 27-40 Urinary Tract – Urinary Bladder Trigone posteroinferior triangular area of the urinary bladder wall formed by imaginary lines connect the two posterior ureteral openings and the anterior urethral opening. The trigone remains immovable as the urinary bladder fills and evacuates. It functions as a funnel directs urine into the urethra as the bladder wall contracts four tunics mucosa submucosa Muscularis: called the detrusor muscle adventitia. Internal urethral sphincter (smooth muscle)
- 41. 41
- 42. 42
- 43. 43
- 44. 27-44 Micturition (Urination) The expulsion of urine from the bladder. Initiated by a complex sequence of events called the micturition reflex. The bladder is supplied by both parasympathetic and sympathetic nerve fibers of the autonomic nervous system.
- 45. 27-45 Urethra Fibromuscular tube exits the urinary bladder through the urethral opening at anteroinferior surface conducts urine to the exterior of the body. Tunica mucosa: is a protective mucous membrane houses clusters of mucin-producing cells called urethral glands. Tunica muscularis: primarily smooth muscle fibers help propel urine to the outside of the body. Two urethral sphincters: Internal urethral sphincter restrict the release of urine until the pressure within the urinary bladder is high enough External urethral sphincter and voluntary activities needed to release the urine are activated.
- 46. 27-46 Urethra The internal urethral sphincter involuntary (smooth muscle) superior sphincter surrounding the neck of the bladder, where the urethra originates. a circular thickening of the detrusor muscle controlled by the autonomic nervous system The external urethral sphincter inferior to the internal urethral sphincter formed by skeletal muscle fibers of the urogenital diaphragm. a voluntary sphincter controlled by the somatic nervous system this is the muscle children learn to control when they become “toilet-trained”
- 47. 27-47 Female Urethra Has a single function: to transport urine from the urinary bladder to the vestibule, an external space immediately internal to the labia minora 3 to 5 centimeters long, and opens to the outside of the body at the external urethral orifice located in the female perineum.
- 48. 48
- 49. 27-49 Male Urethra Urinary and reproductive functions: passageway for both urine and semen Approximately 18 to 20 centimeters long. Partitioned into three segments: prostatic urethra is approximately 3 to 4 centimeters long and is the most dilatable portion of the urethra extends through the prostate gland, immediately inferior to the male bladder, where multiple small prostatic ducts enter it membranous urethra is the shortest and least dilatable portion extends from the inferior surface of the prostate gland through the urogenital diaphragm spongy urethra is the longest part (15 centimeters) encased within a cylinder of erectile tissue in the penis called the corpus spongiosum extends to the external urethral orifice
- 50. 50
- 51. 27-51 Aging and the Urinary System Changes in the size and functioning of the kidneys begin at 30. Gradual reduction in kidney size. Reduced blood flow to the kidneys. Decrease in the number of functional nephrons. Reabsorption and secretion are reduced. Diminished ability to filter and cleanse the blood. Less aldosterone or antidiuretic hormone. Ability to control blood volume and blood pressure is reduced. Bladder decreases in size. More frequent urination. Control of the urethral sphincters—and micturition—may be lost.
- 52. 52