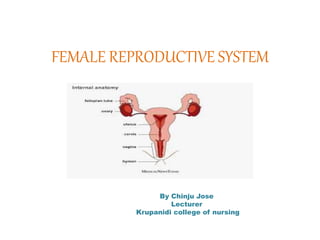
FEMALE REPRODUCTIVE SYSTEM.pptx
- 1. FEMALE REPRODUCTIVE SYSTEM By Chinju Jose Lecturer Krupanidi college of nursing
- 2. FUNCTIONS OF FEMALE REPRODUCTIVE SYSTEM Functions include Producing gametes called eggs, Secreting sex hormones (such as estrogen), Providing a site for fertilization, Gestating a fetus if fertilization occurs, Giving birth to a baby, Breastfeeding baby after birth
- 3. Female Reproductive system External organs Mons pubis Labia majora Labia minora Vestibule Bartholin gland clitoris Internal organs Vagina Cervix Uterus Fallopian tube ovaries
- 4. EXTERNAL GENITALIA The function of the external female reproductive structures are • To enable sperm to enter the body and • to protect the internal genital organs from infectious organisms.
- 5. The vulva FUNCTIONS ARE Acts as sensory tissue during sexual intercourse Assists in micturition by directing the flow of urine Protects the internal female reproductive tract from infection
- 6. STRUCTURE OF VULVA The vulva is a collective term for several anatomical structures. Mons pubis – a subcutaneous fat pad located anterior to the pubic symphysis. It formed by the fusion of the labia majora. Labiamajora– two hair-bearing external skin folds. They extend from the monspubis posteriorly to the posterior commissure (a depression overlying the perineal body)
- 7. Labia minora – two hairless folds of skin, which lie within the labia majora. • They fuse anteriorly to form the hood of the clitoris and extend posteriorly either side of the vaginal opening. • They merge posteriorly, creating a fold of skin known as the fourchette.
- 8. Vestibule – the area enclosed by the labia minora. It contains the openings of the vagina (external vaginal orifice, vaginal introitus) and urethra. Bartholin’s glands – secrete lubricating mucus from small ducts during sexual arousal. They are located either side of the vaginal orifice.
- 9. Clitoris – located under the clitoral hood.
- 10. blood SUPPLY AND LYMPHATICS • The arterial supply to the vulva is from the paired internal and external pudendal arteries • Venous drainage is achieved via the pudendal veins. • Lymph drains to the nearby superficial inguinal lymph nodes.
- 11. Internal organs • Vagina = “birth canal” • • A tube like, muscular but elastic organ • • About 4 to 5 inches long in an adult woman. • • PH- 4 acidic • • It is the passageway for sperm to the egg and for menstrual • bleeding • • Organ of copulation and forms the birth canal of parturition
- 12. VAGINA
- 13. • Posterior wall of vagina is 10 c m long • Anterior wall is only 7.5 cm length • The upper end of the vagina is known as the vault Pink in appearance • It connects the external genital organs to the uterus.the organ of sexual intercourse in women.
- 14. • There are Four fornics of the vagina • One anterior – front of cervix • One posterior – behind • Two lateral – either side of cervix
- 15. Relations of vagina • Anterior to the vagina – lie the bladder and the urethra which are closely connected to the anterior vaginal wall • Posterior to the vagina – lie the pouch of douglas, the rectum and the perineal body; each occupying one third of the posterior vaginal wall
- 16. • Laterally – on the upper two third are the pelvic fascia and the ureters, which pass beside the cervix • Superior to the vagina – lies the utreus • Inferior to the vagina – lies the external genitalia
- 18. UTERUS
- 19. UTERUS • The uterus is a hollow muscular pear-shaped organ, that is located anteroposteriorly in the pelvic cavity. • It lies in the pelvic cavity between the urinary bladder and the rectum • It is about 7.5 cm long, 5 cm wide and its walls are about 2.5 cm thick. • It weighs between 30 and 40 grams
- 20. PARTS OF THE UTERUS For the descriptive purpose uterus can be divided into three distinct parts. • Fundus • Body • Cervix
- 21. • Fundus- This is the dome-shaped part of the uterus above the openings of the uterine tubes. • Body- This is the main part. It is narrowest inferiorly at the internal os where it is continuous with the cervix. • Cervix (‘neck’ of the uterus) - This protrudes through the anterior wall of the vagina, opening into it at the external os.
- 22. LAYERS OF THE UTERUS • Perimetrium • Myometrium • Endometrium
- 23. PERIMETRIUM. • This is peritoneum, which is distributed differently on the various surfaces of the uterus. • • Anteriorly it lies over the fundus and the body where it is folded on to the upper surface of the urinary bladder. This fold of peritoneum forms the vesicouterine pouch. • Posteriorly the peritoneum covers the fundus, the body and the cervix, then it folds back on to the rectum to form the rectouterine (pouch of Douglas).
- 25. MYOMETRIUM. • This is the thickest layer of tissue in the uterine wall. • It is a mass of smooth muscle fibres interlaced with areolar tissue, blood vessels and nerves. ENDOMETRIUM Made up of the Columnar epithelial cells Consist mucous secreting tubular glands
- 26. BLOOD SUPPLY, LYMPH DRAINAGE AND NERVE SUPPLY • Arterial supply. This is by the uterine arteries, branches of the internal iliac arteries. • Venous drainage internal illiac vein • Lymph drainage. Deep and superficial lymph vessels drain lymph from the uterus and the uterine tubes to the aortic lymph nodes and groups of nodes associated with the iliac blood vessels
- 27. SUPPORTING STRUCTURES TO THE UTERUS • The uterus is supported in the pelvic cavity by surrounding organs, muscles of the pelvic floor and ligaments that suspend it from the walls of the pelvis • • Broad ligaments- These are formed by a double fold of peritoneum, one on each side of the uterus. • • Round ligaments-These are bands of fibrous tissue between the two layers of broad ligament.
- 28. • Uterosacral ligaments- These originate from the posterior walls of the cervix and vagina and extend backwards, one on each side of the rectum, to the sacrum. • Transverse cervical (cardinal) ligaments- These extend one from each side of the cervix and vagina to the side walls of the pelvis.
- 29. SUPPORTING STRUCTURES TO THE UTERUS
- 30. THE CERVIX • The cervix is the lower portion of the uterus, an organ of the female reproductive tract. It connects the vagina with the main body of the uterus,acting as a gateway between them. • Anatomically and histologically, the cervix is distinct from the uterus, and hence we consider it as a separate anatomical structure.
- 32. • The cervix is composed of two regions; the ectocervix and the endocervical canal. • The ectocervix is the portion of the cervix that projects into the vagina. It is lined by stratified squamous non-keratinized epithelium. • The opening in the ectocervix, the external os, marks the transition from the ectocervix to the endocervical canal
- 33. • The endocervical canal (or endocervix) is the more proximal, and ‘inner’ part of the cervix. It is lined by a mucus-secreting simple columnar epithelium. The endocervical canal ends, and the uterine cavity begins, at a narrowing called the internal os.
- 34. THE CERVIX
- 35. Functions of cervix • It facilitates the passage of sperm into the uterine cavity. This is achieved via dilation of the external and internal os. • Maintains sterility of the upper female reproductive tract. The cervix, and all structures superior to it, are sterile. This ultimately protects the uterine cavity and the upper genital tract by preventing bacterial invasion. This environment is maintained by the frequent shedding of the endometrium, thick cervical mucus and a narrow external os.
- 36. UTERINE TUBES The uterine (Fallopian) tubes are about 10 cm long and extend from the sides of the uterus between the body and the fundus.
- 37. UTERINE TUBES • They lie in the upper free border of the broad ligament and their trumpet-shaped lateral ends, penetrate the posterior wall, opening into the peritoneal cavity close to the ovaries. • The end of each tube has fingerlike, projections called fimbriae. • The longest of these is the ovarian fimbria, which is in close association with the ovary.
- 38. The fallopian tube has four segments including • interstitial • Isthmus • ampulla • infundibulum.
- 39. FUNCTIONS • The uterine tubes propel the ovum from the ovary to the uterus by peristalsis and ciliary movement. • The secretions of the uterine tube nourish both ovum and spermatozoa. • Fertilisation of the ovum usually takes place in the uterine tube, and the zygote is propelled into the uterus for implantation.
- 40. OVARY • The ovaries are the female gonads, which produce the ova. SITUATION • The Ovary is situated in the ovarian fossa on the lateral pelvic wall, but the position of the ovary is variable.
- 41. • They are 2.5–3.5 cm long, 2 cm wide and 1 cm thick. • Each is attached to the upper part of the uterus by the ovarian ligament and to the back of the broad ligament. • STRUCTURE • The ovaries have two layers of tissue. • • Medulla-This lies in the centre and consists of fibrous tissue, blood vessels and nerves.
- 42. Cortex. • This surrounds the medulla. It has a framework of connective tissue, or stroma, covered by germinal epithelium. • It contains ovarian follicles in various stages of maturity, each of which contains an ovum.
- 43. FUNCTIONS • The ovary is the organ in which the female gametes are stored and develop prior to ovulation. • Their maturation is controlled by the hypothalamus and the anterior pituitary gland,
- 44. FUNCTIONS OF OVARIES AND TESTES