Oral antidiabetics
•Als PPTX, PDF herunterladen•
23 gefällt mir•8,687 views
Oral antidiabetics
Melden
Teilen
Melden
Teilen
Empfohlen
Empfohlen
Weitere ähnliche Inhalte
Was ist angesagt?
Was ist angesagt? (20)
Ähnlich wie Oral antidiabetics
Oral antidiabetics by Dr. Mushtaq Ahmed, Associate Professor, Pharmacology, P...

Oral antidiabetics by Dr. Mushtaq Ahmed, Associate Professor, Pharmacology, P...Dr Mushtaq Ahmad Hakim
Ähnlich wie Oral antidiabetics (20)
Veterinary Pharmacology of Hormone secreted by pancreas 

Veterinary Pharmacology of Hormone secreted by pancreas
oral hypoglycemic drugs.pptx this ppt is related to oral hypoglycemic drugs t...

oral hypoglycemic drugs.pptx this ppt is related to oral hypoglycemic drugs t...
Oral antidiabetics by Dr. Mushtaq Ahmed, Associate Professor, Pharmacology, P...

Oral antidiabetics by Dr. Mushtaq Ahmed, Associate Professor, Pharmacology, P...
Mehr von BikashAdhikari26
Mehr von BikashAdhikari26 (20)
Parts of Plant, plant tissues, microscopy and morphology

Parts of Plant, plant tissues, microscopy and morphology
Kürzlich hochgeladen
PEMESANAN OBAT ASLI : +6287776558899
Cara Menggugurkan Kandungan usia 1 , 2 , bulan - obat penggugur janin - cara aborsi kandungan - obat penggugur kandungan 1 | 2 | 3 | 4 | 5 | 6 | 7 | 8 bulan - bagaimana cara menggugurkan kandungan - tips Cara aborsi kandungan - trik Cara menggugurkan janin - Cara aman bagi ibu menyusui menggugurkan kandungan - klinik apotek jual obat penggugur kandungan - jamu PENGGUGUR KANDUNGAN - WAJIB TAU CARA ABORSI JANIN - GUGURKAN KANDUNGAN AMAN TANPA KURET - CARA Menggugurkan Kandungan tanpa efek samping - rekomendasi dokter obat herbal penggugur kandungan - ABORSI JANIN - aborsi kandungan - jamu herbal Penggugur kandungan - cara Menggugurkan Kandungan yang cacat - tata cara Menggugurkan Kandungan - obat penggugur kandungan di apotik kimia Farma - obat telat datang bulan - obat penggugur kandungan tuntas - obat penggugur kandungan alami - klinik aborsi janin gugurkan kandungan - ©Cytotec ™misoprostol BPOM - OBAT PENGGUGUR KANDUNGAN ®CYTOTEC - aborsi janin dengan pil ©Cytotec - ®Cytotec misoprostol® BPOM 100% - penjual obat penggugur kandungan asli - klinik jual obat aborsi janin - obat penggugur kandungan di klinik k-24 || obat penggugur ™Cytotec di apotek umum || ®CYTOTEC ASLI || obat ©Cytotec yang asli 200mcg || obat penggugur ASLI || pil Cytotec© tablet || cara gugurin kandungan || jual ®Cytotec 200mcg || dokter gugurkan kandungan || cara menggugurkan kandungan dengan cepat selesai dalam 24 jam secara alami buah buahan || usia kandungan 1_2 3_4 5_6 7_8 bulan masih bisa di gugurkan || obat penggugur kandungan ®cytotec dan gastrul || cara gugurkan pembuahan janin secara alami dan cepat || gugurkan kandungan || gugurin janin || cara Menggugurkan janin di luar nikah || contoh aborsi janin yang benar || contoh obat penggugur kandungan asli || contoh cara Menggugurkan Kandungan yang benar || telat haid || obat telat haid || Cara Alami gugurkan kehamilan || obat telat menstruasi || cara Menggugurkan janin anak haram || cara aborsi menggugurkan janin yang tidak berkembang || gugurkan kandungan dengan obat ©Cytotec || obat penggugur kandungan ™Cytotec 100% original || HARGA obat penggugur kandungan || obat telat haid 1 bulan || obat telat menstruasi 1-2 3-4 5-6 7-8 BULAN || obat telat datang bulan || cara Menggugurkan janin 1 bulan || cara Menggugurkan Kandungan yang masih 2 bulan || cara Menggugurkan Kandungan yang masih hitungan Minggu || cara Menggugurkan Kandungan yang masih usia 3 bulan || cara Menggugurkan usia kandungan 4 bulan || cara Menggugurkan janin usia 5 bulan || cara Menggugurkan kehamilan 6 Bulan
________&&&_________&&&_____________&&&_________&&&&____________
Cara Menggugurkan Kandungan Usia Janin 1 | 7 | 8 Bulan Dengan Cepat Dalam Hitungan Jam Secara Alami, Kami Siap Meneriman Pesanan Ke Seluruh Indonesia, Melputi: Ambon, Banda Aceh, Bandung, Banjarbaru, Batam, Bau-Bau, Bengkulu, Binjai, Blitar, Bontang, Cilegon, Cirebon, Depok, Gorontalo, Jakarta, Jayapura, Kendari, Kota Mobagu, Kupang, LhokseumaweCara Menggugurkan Kandungan Dengan Cepat Selesai Dalam 24 Jam Secara Alami Bu...

Cara Menggugurkan Kandungan Dengan Cepat Selesai Dalam 24 Jam Secara Alami Bu...Cara Menggugurkan Kandungan 087776558899
❤️ Chandigarh Call Girls☎️98151-579OO☎️ Call Girl service in Chandigarh ☎️ Chandigarh Call Girls Service ☎️ Call Girls In Chandigarh BEST CALL GIRL ESCORTS SERVICE IN CHANDIGARH CALL WATTSAPP 98151-579OO THE MOST BEAUTIFUL INDEPENDENT ESCORT CALL GIRL SERVICE In Chandigarh WE ARE PROVIDING GENUINE CALL GIRL SERVICE
I AM A a NATURAL BRUNETTES, SLIM BODY, NATURAL LONG HAIR AND ALL TYPE OF HAIR IS A NATURAL BRUNETTE IN THE MOST BEAUTIFUL MODELS INDEPENDENT ESCORT GIRL I AM A NATURAL BRUNETTE WITH ROOM AND HOTEL AND A NATURAL BRUNETTE WITH A BODY MADE FOR SIN AND ALL TYPE OF ME ALL THE TIME
I SEND YOU A HAIR, VERY SOCIABLE AND FUNNY, READY TO ENTERTAIN TO ENTERTAIN U AND MAKE FORGET ABOUT TO AGET ENTERTAINMENT YOU AND MAKE FORGET ABOUT ALL THE PROBLEMS. LET'S HAVE A WONDERFUL TIME TOGETHER AND FORGET ABOUT EVERYTHING ALL TYPE SERVICE ENJOYMENT SAFE AND SECURE IN CALL OUT CALL HOME AND HOTEL ANYTIME AVAILABLE
AND ALL TYPE SERVICE ENJOYMENTPANCHKULA INDEPENDENT BEST CALL GIRL ESCORTS SERVICE IN PANCHKULA INDEPENDENT CALL GIRL Chandigarh Call Girls In Chandigarh BEST Call Girls in CHANDIGARH Escort Service provide Cute Nice sweet and Sexy Models in beautiful CHANDIGARH city cash in hand to hand call girl in CHANDIGARH and CHANDIGARH escorts. HOT & SEXY MODELS // COLLEGE GIRLS IN CHANDIGARH AVAILABLE FOR COMPLETE ENJOYMENT WITH HIGH PROFILE INDIAN MODEL AVAILABLE HOTEL & HOME ★ SAFE AND SECURE HIGH CLASS SERVICE AFFORDABLE RATE ★ 100% SATISFACTION,UNLIMITED ENJOYMENT. ★ All Meetings are confidential and no information is provided to any one at any cost.
★ EXCLUSIVE Profiles Are Safe and Consensual with Most Limits Respected
★ Service Available In: - HOME & 24x7 :: 3 * 5 *7 *Star Hotel Service .In Call & Out call
Services :
★ A-Level (5 star escort)
★ Strip-tease
★ BBBJ (Bareback Blowjob)Receive advanced sexual techniques in different mode make their life more pleasurable.
★ Spending time in hotel rooms
★ BJ (Blowjob Without a Condom)
★ Completion (Oral to completion)
★ Covered (Covered blowjob Without a Condom)-❤️ Chandigarh Call Girls Service☎️98151-579OO☎️ Call Girl service in Chandigarh ☎️ Chandigarh Call Girls Service ☎️ Call Girls In Chandigarh❤️ Chandigarh Call Girls☎️98151-579OO☎️ Call Girl service in Chandigarh ☎️ Ch...

❤️ Chandigarh Call Girls☎️98151-579OO☎️ Call Girl service in Chandigarh ☎️ Ch...Rashmi Entertainment
Kürzlich hochgeladen (20)
Call Girls Mussoorie Just Call 8854095900 Top Class Call Girl Service Available

Call Girls Mussoorie Just Call 8854095900 Top Class Call Girl Service Available
Call Girls in Lucknow Just Call 👉👉 8875999948 Top Class Call Girl Service Ava...

Call Girls in Lucknow Just Call 👉👉 8875999948 Top Class Call Girl Service Ava...
Call Girls in Lucknow Just Call 👉👉8630512678 Top Class Call Girl Service Avai...

Call Girls in Lucknow Just Call 👉👉8630512678 Top Class Call Girl Service Avai...
Call Girls Rishikesh Just Call 9667172968 Top Class Call Girl Service Available

Call Girls Rishikesh Just Call 9667172968 Top Class Call Girl Service Available
Circulatory Shock, types and stages, compensatory mechanisms

Circulatory Shock, types and stages, compensatory mechanisms
Race Course Road } Book Call Girls in Bangalore | Whatsapp No 6378878445 VIP ...

Race Course Road } Book Call Girls in Bangalore | Whatsapp No 6378878445 VIP ...
(RIYA)🎄Airhostess Call Girl Jaipur Call Now 8445551418 Premium Collection Of ...

(RIYA)🎄Airhostess Call Girl Jaipur Call Now 8445551418 Premium Collection Of ...
Call girls Service Phullen / 9332606886 Genuine Call girls with real Photos a...

Call girls Service Phullen / 9332606886 Genuine Call girls with real Photos a...
Difference Between Skeletal Smooth and Cardiac Muscles

Difference Between Skeletal Smooth and Cardiac Muscles
Lucknow Call Girls Just Call 👉👉8630512678 Top Class Call Girl Service Available

Lucknow Call Girls Just Call 👉👉8630512678 Top Class Call Girl Service Available
Cardiac Output, Venous Return, and Their Regulation

Cardiac Output, Venous Return, and Their Regulation
Call Girl in Chennai | Whatsapp No 📞 7427069034 📞 VIP Escorts Service Availab...

Call Girl in Chennai | Whatsapp No 📞 7427069034 📞 VIP Escorts Service Availab...
Cara Menggugurkan Kandungan Dengan Cepat Selesai Dalam 24 Jam Secara Alami Bu...

Cara Menggugurkan Kandungan Dengan Cepat Selesai Dalam 24 Jam Secara Alami Bu...
👉 Chennai Sexy Aunty’s WhatsApp Number 👉📞 7427069034 👉📞 Just📲 Call Ruhi Colle...

👉 Chennai Sexy Aunty’s WhatsApp Number 👉📞 7427069034 👉📞 Just📲 Call Ruhi Colle...
Call 8250092165 Patna Call Girls ₹4.5k Cash Payment With Room Delivery

Call 8250092165 Patna Call Girls ₹4.5k Cash Payment With Room Delivery
Lucknow Call Girls Service { 9984666624 } ❤️VVIP ROCKY Call Girl in Lucknow U...

Lucknow Call Girls Service { 9984666624 } ❤️VVIP ROCKY Call Girl in Lucknow U...
Call Girls Wayanad Just Call 8250077686 Top Class Call Girl Service Available

Call Girls Wayanad Just Call 8250077686 Top Class Call Girl Service Available
❤️ Chandigarh Call Girls☎️98151-579OO☎️ Call Girl service in Chandigarh ☎️ Ch...

❤️ Chandigarh Call Girls☎️98151-579OO☎️ Call Girl service in Chandigarh ☎️ Ch...
Russian Call Girls In Pune 👉 Just CALL ME: 9352988975 ✅❤️💯low cost unlimited ...

Russian Call Girls In Pune 👉 Just CALL ME: 9352988975 ✅❤️💯low cost unlimited ...
Oral antidiabetics
- 2. Meglitinide Analogs Sulphonylureas Thiazolindinediones Metformin (Biguanides) Alpha Glucosidase Inhibitors
- 3. Classification of oral anti-diabetic drugs A. Enhance Insulin Secretion 1. Sulfonylureas (K+ ATP channels blockers) • First Generation: Tolbutamide • Second Generation: Glibenclamide, Glipizide, Gliclazide, Glimepiride 2. Meglitinide analouges: Repaglinide, Nateglinide 3. Glucagon-like peptide (GLP-1) receptor agonists (injectable): Exenadite, Liraglutide 4. Dipeptidyl peptidase-4 (DPP-4) inhibitors: Sitagliptin, Vildagliptin, Saxagliptin, Alogliptin, Linagliptin B. Overcome Insulin Resistance 1. Biguanides (AMPK activators): Metformin 2. Thiazolidinediones (PPARγ activator): Pioglitazone C. Miscellaneous 1. α-Glucosidase inhibitors: Acarbose, Miglitol, Voglibose 2. Amylin analogue: Pramlintide 3. Dopamine D2 receptor agonist: Bromocriptine 4. Sodium Glucose Co-Transport 2 (SGLT 2) inhibitor: Dapagliflozine
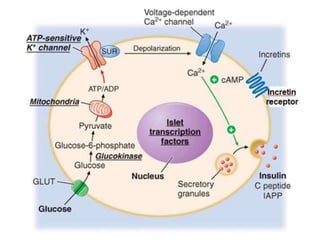
- 5. Sulfonylureas (K+ ATP channels blockers) Insulin secretagogue Requires at least 30% functional β cells • Glibenclamide, Glicazide, Glipizide, Glimepiride • MOA: ↑ insulin secretion by acting on sulfonylurea receptor at ATP sensitive K+ channel • Acts by blocking the K+ ATP channel that reduces influx of rectifying K+ ion current & causes partial depolarization of pancreatic beta-cells increased influx of Ca++ ions as well as release of Ca++ from intracellular stores & promotes exocytotic release of insulin. • Chronic use: sensitize the target tissue to the action of insulin • Slow hepatic degradation of insulin • Reduces glucagon secretion
- 7. Pharmacokinetics: • Well absorbed orally • High plasma protein bound (90%) • Single daily dose is sufficient Adverse Effects: • Hypoglycaemia • Non specific Side effects: weight gain, nausea, vomiting, flatulence, diarrhoea, constipation, headache, paresthesia; mild and infrequent • Hypersensitivity: Rashes, photosensitivity, purpura, transient leukopenia, rarely agranulocytosis • SU + alcohol: flushing, disulfiram-like reaction Should not be used in pregnancy and lactating mothers !
- 8. MEGLITINIDE/PHENYLALANINE ANALOGUES Mechanism of Action: • K+ ATP channel blockers; quick and short lasting action • Normalises meal time glucose levels Repaglinide and Nateglinide: • Quickly absorbed and rapidly metabolised • Administered before each major meal, omit if meal missed. • Lower incidence of hypoglycaemia Indication: • Type 2 DM with pronounced postprandial hyperglycaemia • Along with Metformin/long acting insulin S/E: Mild headache, dyspepsia, arthralgia weight gain Avoid in liver disease!
- 10. GLUCAGON-LIKE PEPTIDE-1 (GLP) RECEPTOR AGONISTS MOA: GLP-1 is an important incretin released from the gut in response to ingested glucose. It induces insulin release from pancreatic β cells, inhibits glucagon release from α cells, slows gastric emptying and suppresses appetite. Exenatide: • Synthetic dipeptidyl peptidase-4 (DPP-4) enzyme resistant analogue. • Activates GLP receptors • Cannot be given orally • Used as an add-on drug to metformin/SU/Pioglitazone • Lowers postprandial as well as fasting blood glucose, HbA1c and body weight S/E: nausea/vomiting, tolerance develops later Liraglutide: • Highly bound to plasma proteins: longer duration of action
- 12. DIPEPTIDYL PEPTIDASE-4 (DPP-4) INHIBITORS DPP-4 enzyme causes rapid degradation of endogenous GLP- 1, thus orally active inhibitors of this enzyme have been developed as indirectly acting insulin secretagogues. Sitagliptin: • MOA: Acts as competitive and selective DPP-4 inhibitor & potentiates the action of GLP-1 and GIP. • Boosts postprandial release, decreases glucagon secretion and lowers meal time as well as fasting blood glucose in Type 2DM • Body weight neutral, low risk of hypoglycaemia • Well absorbed orally, little metabolised, largely excreted unchanged in urine • Dose reduction needed in renal dysfunction • S/E: nausea, loose stools, headaches, rashes, allergic reactions, edema
- 14. BIGUANIDES (METFORMIN) Biguanides do not cause insulin release, but presence of insulin is essential for their action. MOA: Metformin causes activation of AMPK, leading to: • Suppression of hepatic gluconeogenesis • Enhances insulin-mediated glucose uptake and disposal in skeletal muscle and fat • Interferes with mitochondrial respiratory chain and promotes peripheral glucose utilization • Retards glucose absorption of glucose, hexose, amino acids, Vit B12 Adverse Effects: Hypoglycaemia in overdose, Lactic acidosis, Vitamin B12 deficiency Contraindicated in hypotensive states, heart failure, severe respiratory, hepatic and renal disease, alcoholics Advantages: nonhypoglycaemic, weight loss, prevents long term complications, prolongs beta cell life Limiting feature: gastrointestinal intolerance
- 16. THIAZOLIDINEDIONES (PPARγ ACTIVATOR): MOA: Pioglitazone is selective agonist for the nuclear peroxisome proliferator-activated receptor γ (PPARγ) expressed mainly in fat cells, and in muscle cells. It enhances transcription of insulin responsive genes & tends to reverse insulin resistance by enhancing GLUT4 receptor expression and translocation. • Suppresses hepatic gluconeogenesis • Additionally, lowers serum triglyceride, raises HDL • Well tolerated S/E: plasma volume expansion, edema, weight gain, headache, myalgia, mild anaemia, increased risk of fracture esp. in elderly women Contraindicated in liver disease and in CHF
- 18. Miscellaneous α GLUCOSIDASE INHIBITORS Acarbose: MOA: Inhibits α-glucosidases (enzyme responsible for digestion of carbohydrates in the brush border of small intestine mucosa) slow down and decrease digestion and absorption of polysaccharides and sucrose. Dose 50–100 mg TDS is taken at the beginning of each major meal. Additionally it promotes GLP-1 release. S/E: Flatulence, abdominal discomfort, loose stool; Poor patient acceptability Miglitol: It has a smaller molecule than acarbose, and it is a stronger inhibitor of sucrase. Potency for other α-glucosidases is equivalent to acarbose. Dose: 25–100 mg TDS at beginning of each meal. Voglibose: It has properties, use and side effects similar to that of acarbose. Dose: 0.2–0.3 mg TDS just before meals.
- 20. AMYLIN ANALOGUE Amylin is produced by pancreatic β cells and acts in the brain to reduce glucagon secretion from α cells, delay gastric emptying, retard glucose absorption and promote satiety. Pramlintide: • Synthetic amylin analogue injected s.c. before meal attenuates postprandial glycaemia and exerts centrally mediated anorectic action. • Reduction in body weight is additional benefit. Bromocriptine: it is dopamine D2 agonist that acts on hypothalamic dopaminergic control of the circadian rhythm of hormone (GH, prolactin, ACTH) release and reset it to reduce insulin resistance. Dapagliflozin: It inhibits sodium-glucose co-transport-2 (SGLT-2), which is major transporter for glucose reabsorbtion in the proximal tubules. Thus it induces glucosuria and lowers blood glucose in type 2 DM, as well as causes weight loss.
- 24. HbA1c?
- 26. THANK YOU FOR YOUR KIND ATTENTION ! FOR FURTHER REFERENCE PLEASE SEE K. D. TRIPATHI!
