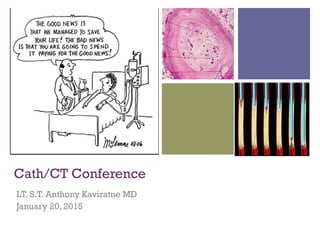
Chronic total occlusion
- 1. + Cath/CT Conference LT. S.T. Anthony Kaviratne MD January 20, 2015
- 2. + Case Presentation 56 year old male non-smoker with history of HLD and recent NSTEMI treated medically presented with chief complaint of ongoing chest pain with exertion. The patient initially presented 6 weeks ago to a OSH with 2 days of stuttering chest pain after completing Iron man triathlon. He noted severe chest discomfort at the end of his run but completed the race. Symptoms resolved with rest but would occur with exertion over the next 2 days. Patient was seen by OSH followed by cath which showed total occlusion of the right coronary artery but otherwise non obstructive mild disease. Per report attempt was made at opening the right coronary which was unsuccessful and medical therapy was pursued. Current symptoms similar initial which has not improved over the last 6 weeks.
- 3. + Past Medical History Coronary artery disease HLD ASA 81mg Plavix 75mg Lipitor 80mg Metoprolol XL 25mg Lisinopril 2.5mg PO qday Renexa 1000mg PO BID Nitro PRN Medications
- 4. + Social and Family History Tobacco: Denies Etoh: 6 beers/ week Recreation drug use: None Family History: - No known family members with CAD.
- 5. + Physical Exam: VS: sinus bradycardia but otherwise unremarkable. Male in NAD with normal work of breathing Neck: JVD 8 cm, Carotid upstroke was delayed. Cardiac: Normal S1 and S2. No murmurs/rubs/gallops Pul: CTAB Ext: No Edema Vascular: 2+biltateral and equal
- 6. + Labs Labs:WNL EKG: sinus with nonspecific T wave abnormalities throughout the precordium Echo: LVEF 55-60% with inferior and lateral wall hypokinesis. Mild MR. otherwise unremarkable. MPS: moderate to severe ischemia inferior and infralateral wall from mid to apex. SDS of 8 Previous cath LM: no disease LAD: mild luminal irregularities with left to right collaterals LCX: mild luminal irregularities RCA:Total occlusion with small bridging collaterals
- 7. +
- 8. + Approach to this patient? Should another attempt made at the CTO? Continue medical management? Further medical management or referral to CABG? How will this change the patient’s course?
- 9. + Management of Chronic Total Occlusion
- 10. + Objectives Define CTO and epidemiology PCI success rates and attempts and barriers to attempt Indications for PCI for CTO (when to consider CABG) Benefits of PCI to CTO Strategies for opening CTO with examples
- 11. + Chronic Total Occlusion (CTO) “True CTOs” are characterized by significant narrowing with lumen that results in complete interruption of antegrade blood flow (TIMI 0). “Functional CTO” which has minimal contrast penetration though the lesion without distal vessel opacification (TIMI 1) Registry data demonstrate that 15–30% of patients undergoing diagnostic coronary angiography will have at least one occluded coronary artery Retrospective review of >6500 patients reported CTO lesions in up to 52% of patient CABG has historically been the preferred revascularization option owing to its higher immediate procedural success rate in the CTO vessel Christofferson RD, Lehmann KG, Martin GV et al. Effect of chronic total coronary occlusions on treatment strategy. Am. J. Cardiol. 95(9),1088–1091 (2005).
- 12. + PCI success rates SYNTAX trial reported 50% success rates 70% of CTOs were successfully re-opened with PCI in the Canadian Multicenter registry Angiographic results of the PRAGUE-4 tria: 1-year patency after bypass grafting of collateralized CTO vessels only 23%. LAD CTOs were much better with 100% patency at 12 month Rathore S et al. Procedural and in-hospital outcomes after percutaneous coronary intervention for chronic total occlusions of coronary arteries 2002 to 2008: impact of novel guidewire techniques. JACC Cardiovasc. Interv. 2(6),489–497 (2009).
- 13. +
- 14. + Barriers to CTO attempt PCI technical complexity: Difficulty crossing CTO with wires, Operator skill Unique complications Vessel perforation Contrast nephropathy Radiation injury: Av floro time 46 min+/- 25 (3.2Gy +/- 2.1) Possible loss of collaterals Economic disincentive: labor and resources Physician skepticism Higher short term MACE rate (in hospital elective 0.9-6.5% vs. 1.2% non CTO) Higher mortality (in house 0.5% with failed CTO 1-2.6%). 30 day high as 1.1%
- 15. + Indications for PCI for CTO PCI is warranted when all three of the following conditions are met: The occluded vessel is responsible for the patient's symptoms or in selected patients with silent ischemia in whom there is a large amount of myocardium at risk. The myocardial territory of the occluded artery is viable The likelihood of success is >60 percent with estimated rate of death <1% and MI < 5%. 2011 ACCF/AHA/SCAI Guideline for Percutaneous Coronary Intervention Class IIa: PCI of a chronic total occlusion in patients with appropriate clinical indications and suitable anatomy is reasonable when performed by operators with appropriate expertise. (Level of Evidence: B) Stone et al. “Percutaneous Recanalization of Chronically Occluded Coronary Arteries: A Consensus Document”. Circulation. 2005;112:2364-2372
- 16. + CABG over PCI for CTO Left main disease Complex three-vessel disease, particularly in patients with insulin-requiring diabetes, severe left ventricular dysfunction, or chronic kidney disease. An occluded proximal left anterior descending coronary artery that supplies a viable anterior wall that is not favorable for PCI. Multiple CTOs with a low anticipated rate of success Multivessel disease
- 17. + What are the benefits?
- 18. + Long term survival with CTO Hannan EL, Racz M, Holmes DR, et al. Impact of completeness of percutaneous coronary intervention revascularization on long-term outcomes in the stent era. Circulation 2006;113:2406–12
- 19. + Long Term outcome of Recanalization of CTO: Survival Jones et al JACC:CV intervention April 2012 Muhammad et al, Cath and CV intervention 3/2013
- 20. + Impact on angina TOAST-GISE (Total Occlusion An- gioplasty Study–Società Italiana di Cardiologia Invasiva) trial, CTO-PCI success was associated with 86% angina-free survival, whereas CTO-PCI failure was associated with 70% angina-free survival (p =0.008) The COURAGE nuclear substudy reported reduction in ischemic myocardium measured by MPS showed PCI plus OMT (-2.7%) vs. OMT (-0.5%) PRISON II trial, the proportion of patients with CCS angina class ≥3 was reduced from 62% at baseline to 25% at 6 month Other trials, 85–90% of patients with CTO lesions are reported as symptomatic of 'typical angina
- 21. + Improved Tolerability of Acute Coronary Syndrome Events In a STEMI CTO of a nonculprit vessel is a independent predictor of early mortality and cardiogenic shock. Van der Schaaf et al showed CTO is increased twofold compared with STEMI patients with single-vessel disease (1- year mortality 63 vs 31%) The presence of CTO in a non-IRA has a comparable effect on the outcome of non-STEMI (NSTEMI) patients Bataille Y, Dery JP, Larose E et al. Deadly association of cardiogenic shock and chronic total occlusion in acute ST-elevation myocardial infarction. Am. Heart J. 164(4),509–515 (201 van der Schaaf RJ, Timmer JR, Ottervanger JP et al. Long-term impact of multivessel disease on cause-specific mortality after ST elevation myocardial infarction treated with reperfusion therapy. Heart 92(12),1760–1763 (2006
- 22. +
- 23. + Other possible benefits Reduction in ICD therapy In patient’s with LVEF >35% CTOs have a greater risk of sudden cardiac death or appropriate ICD therapy compared with non- CTO patients (VACTO trial 21% CTO vs. 7% non CTO) Benefit on LV function and geometry Using CMR demonstrated wall thickening improved in successful PCI
- 24. + Factors influencing procedural outcomes More experienced operators leads to be more success rates (FAST-CTO study report 67% first 75 cases rising to 87% in second 75 cases) Geometry of the lesion (shorter length, tapered cap, microchannels, duration of CTO, calcium, tortuosity) Bridging collateral, cap continuation with minor branches Using specific guidewires for CTO (from expert-CTO trial) greater stiffness at the tip tapered tip to engage in microchannels (nl 0.014, CTO 0.009) hydrophilic or very lubricious coating to traverse Low profile balloon for pre-dilatation
- 25. + PCI strategies Antegrade approach Parallel wire technique Retrograde technique IVUS guided “knuckle wire” technique Controlled Antegrade Retrograde Tracking (CART)
- 32. + Control antegrade retrograde tracking (CART)
- 33. + Questions?
- 34. + Summery CTO are common angiographic finding and a common reason for referral to CABG PCI to CTO are complex requiring a lot of resources with unique risk/complications associated with it. PCI to CTO technically challenging and financial disincentives prevent more attempts. PCI to CTO should be considered in patients who are symptomatic despite OMT, CABG but now with failed grafts, and in patients with large area of myocardium in jeopardy (specially if they are unwilling to undergo CABG).
- 35. + Patient outcome PCI of the CTO attempted with antegrade approach and was successful. Procedure took 4 hours with 65 min of fluoro time. His symptoms resolved and returned to exercising 1 month later without any symptoms. 6 month follow up: Patient started training for “fun” 12 month outcome: Patient had atypical symptoms was re cathed with patent RCA stent with no other significant lesions. 18 months: Patient completed his 2 half marathon and 1 full. Planning on attempting Iron man again.
Hinweis der Redaktion
- Canadian CTO registery reported about 18% prevelance In addition, many CTO patients have multivessel disease and will more frequently require target vessel revascularization (TVR) after PCI The SYNTAX trial assessed the optimal method of revascularization for patients with multivessel CAD,[15] of whom around one-quarter in each treatment arm had at least one CTO. CTOs contribute significantly to the SYNTAX score owing to their complexity and lower success rate compared with non-CTO PCI. Hence the presence of a CTO currently represents one of the most common reasons for CABG referral Less than 50% of SYNTAX CTO lesions were successfully treated by PCI. In comparison, 70% of CTOs were successfully re-opened with PCI in the Canadian Multicenter registry,[7] and success rates of &gt;85% are now reported in high volume centers
- Widimsky P, Straka Z, Stros P et al. One-year coronary bypass graft patency: a randomized comparison between off-pump and on-pump surgery. Angiographic results of the PRAGUE-4 trial. Circulation 110(22),3418–3423 (2004).
- Canadian CTO registry data demonstrate that out of 1697 patients, only 10% had attempted CTO PCI. In total, 20% had PCI performed in non-CTO arteries, 44% were treated with medical therapy and 26% underwent CABG
- Jones et al investigated the impact of procedural success on mortality following CTO in a cohort of 6,996 patients undergoing PCI for stable angina at a single center between 2003 and 2010. Of these patients, 836 (11.9%) underwent PCI for CTO and 582 (69.6%) of the PCIs were successful. Among the successful procedures, stents were implanted in 97% of patients, of which a majority were drug-eluting stents. Just over half of the CTO patients had single-vessel disease while 46.1% had lesions in multiple vessels. Nearly 80% of patients underwent single-vessel PCI and the remainder underwent CTO PCI as part of a multivessel procedure. Patients who were treated successfully were more likely to be treated for an occlusion of the left anterior descending coronary artery.
- Between 2006 and 2011, 2,020 consecutive patients were included. A total of 141 patients (7%) presented with cardiogenic shock on admission. The prevalence of 1 CTO and &gt;1 CTO in a non-infarct-related artery was 23% and 5%, respectively, among patients with shock compared with 6% and 0.5% in patients without shock (P &lt; .0001). Independent predictors of cardiogenic shock included left main-related MI (odds ratio [OR] 6.55, 95% CI 1.39-26.82, P = .019), CTO (OR 4.20, 95% CI 2.64-6.57, P &lt; .001), creatinine clearance &lt;60 mL/min (OR 3.41, 95% CI 2.32-4.99, P &lt; .0001), and left anterior descending-related MI (OR 2.20, 95% CI 1.51-3.23, P &lt; .0001). Thirty-day mortality was 100% in shock patients with &gt;1 CTO, 65.6% with 1 CTO, and 40.2% in patients without CTO (P &lt; .0001). After adjustment for left ventricular ejection fraction and renal function, CTO remained an independent predictor for 30-day mortality (hazard ratio [HR] 1.83; 95% CI 1.10-3.01, P = .02).