3. abnormal presentations
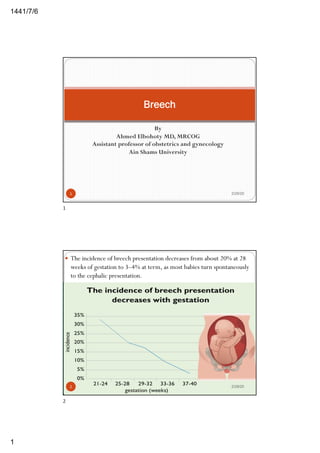
- 1. 6/7/1441 1 By Ahmed Elbohoty MD, MRCOG Assistant professor of obstetrics and gynecology Ain Shams University Breech 2/29/201 1 — The incidence of breech presentation decreases from about 20% at 28 weeks of gestation to 3–4% at term, as most babies turn spontaneously to the cephalic presentation. 2/29/202 2
- 2. 6/7/1441 2 2/29/203 3 Longitudinal lie. Frank breech presentation. I I Longitudinal lie. Complete breech presentation. 2/29/204 4
- 3. 6/7/1441 3 Longitudinal lie. Incomplete, or footling, breech presentation. 2/29/205 5 Causes of breech presentation — Prematurity — Uterine abnormality (septum,… — Multiparity — Multiple pregnancy — Pelvic mass — Placenta previae — Fetal malformation — But In most of cases no definitive cause 2/29/206 6
- 4. 6/7/1441 4 Risks — There is substantial Increased perinatal morbidity and mortality Due to; Prematurity Congenital abnormalities; hydrocephalus Cord prolapse Birth asphyxia Birth trauma intra-cranial haemorrhage 2/29/207 7 TERM BREECH WHAT TO DO??? 2/29/20 — Hannah et al., 2000 in Lancet.Term Breech trial: RCT 2083 women in 121 centers in 16 countries Better neonatal outcome with Elective CS with no difference in maternal outcome — Goffinet et al., 2006. PREMODA study inAJOG. Observational cohort prospective study with strict criteria before and during labour: no difference. A senior obstetrician was present at 92.3% of all vaginal deliveries. Pelviometry was employed in 82.5% of planned vaginal births — Doctors role: explain evidence and ensure understanding and supports the patients decision to make it as safe as possible 8 8
- 5. 6/7/1441 5 2/29/20 — The presence of a skilled birth attendant is essential for safe vaginal breech birth. — Units with limited access to experienced personnel should inform women that vaginal breech birth is likely to be associated with greater risk and offer antenatal referral to a unit where skill levels and experience are greater. 9 9 CS benefits and risks 2/29/20 — Women should be informed that planned caesarean section carries —a reduced perinatal mortality and early neonatal morbidity for babies with a breech presentation at term compared with planned vaginal birth. — Women should also be advised that planned caesarean section for breech presentation carries —a small increase in serious immediate complications for them compared with planned vaginal birth. 10 10
- 6. 6/7/1441 6 Long term effects — There is no evidence that the long term health of babies with a breech presentation delivered at term is influenced by how the baby is born. — Planned caesarean section for breech presentation does not carry any additional risk to long-term health outside pregnancy. — The long-term effects of planned caesarean section for term breech presentation on future pregnancy outcomes for them and their babies is uncertain. 2/29/2011 11 Management of Breech presentation at term — Unless contraindicated, ECV should be offered — Time — ECV should be offered at term from 37+0 weeks of gestation in multiparous — In nulliparous women, ECV may be offered from 36+0 weeks of gestation (have a low chance of spontaneous version) — Who? — ECV should only be performed by a trained practitioner or by a trainee working under direct supervision. — There is no general consensus on the eligibility for, or contraindications to, ECV. 2/29/2012 12
- 7. 6/7/1441 7 Women's attitude 2/29/20 — Although most women tolerate ECV, they should be informed that ECV can be a painful procedure. — The uptake of ECV is best increased by timely identification of the baby presenting by the breech and provision of evidence-based information. 13 13 2/29/2014 14
- 8. 6/7/1441 8 ECV 2/29/2015 15 Why not done in all breech cases 2/29/20 — The greatest impediment to the use of ECV is the nonidentification of breech presentation (20.0–32.5% of all breech presentations) and these have worse outcomes — The possibility of breech presentation should always be considered at clinical examination although abdominal palpation has a sensitivity of only 70%. — In the absence of routine third trimester ultrasound, particular care should be taken with high-risk groups, e.g. where a previous baby has been breech — Recurrence rate after one breech presentation is 9.9% (RR 3) 16 16
- 9. 6/7/1441 9 Absolute contraindications for ECV: — an absolute reason for caesarean section already exists (e.g. placenta praevia major). — Antepartum haemorrhage within the last 7 days — Abnormal cardiotocography — Major uterine anomaly — Ruptured membranes — Multiple pregnancy (except delivery of second twin). — rhesus isoimmunisation — Abnormal fetal doppler — where the mother declines or is unable to give informed consent.. 2/29/2017 17 Relative contraindications and needs additonal precautions if it will be done — Hypertension — oligohydramnios — major fetal anomalies — scarred uterus — ECV should be performed with additional caution where there is oligohydramnios or hypertension 2/29/2018 18
- 10. 6/7/1441 10 Previous one CS 2/29/20 — Women should be informed that ECV after one caesarean delivery appears to have no greater risk than with an unscarred uterus. 19 19 Benefits — ECV reduces the chance of breech presentation at delivery and therefore the associated risks, particularly of avoidable caesarean section. — With a trained operator, about 50% of ECV attempts will be successful (60% for MP and 40% for PG) but this rate can be individualised for them. 2/29/2020 20
- 11. 6/7/1441 11 Risks 2/29/20 — Women should be counselled that with appropriate precautions, ECV has a very low complication rate. — Nevertheless, a few case reports exist of complications such as placental abruption, uterine rupture and fetomaternal haemorrhage. — A 0.5% immediate emergency caesarean section rate and no excess perinatal morbidity and perinatal mortality. — The indication in over 90% being vaginal bleeding or an abnormal CTG following the procedure. — A small increase in neonatal unit admission OR1.48 after an unsuccessful attempt — Labour after ECV is associated with a slightly increased rate of caesarean section (OR 2) and instrumental delivery (OR 1.5) when compared with spontaneous cephalic presentation. — The risk of caesarean delivery may be greater with a shorter ECV to labour interval. — Women should be informed that few babies less than 3% revert to breech after successful ECV — Fetomaternal haemorrhage was detected in 2.4% of women, a third of which had more than 1 ml21 21 Prediction of success 2/29/20 — ECV success can be predicted to some extent, but the use of models to predict success should not be used routinely to determine whether ECV can be attempted. — Success rates depend on multiple variables. It is likely that case selection considerably affects success rates. — multiparity (OR 2.5) — nonengagement of the breech (OR 9.4) — use of tocolysis (OR 18) — a palpable fetal head (OR 6.3) — a maternal weight of less than 65 kg (OR 1.8) — posterior placental location (OR 1.9) — complete breech position (OR 2.3) — an amniotic fluid index greater than 10 (OR 1.8) 22 22
- 12. 6/7/1441 12 Failed ECV —Spontaneous turn to cephalic after an unsuccessful ECV attempt at 36+0 weeks of gestation or later occurs only in a few babies —Another trial using tocolysis —Planned CS —PlannedVD ?? 2/29/2023 23 How to increase the success rate? 2/29/20 — Use of tocolysis with betamimetics improves the success rates of ECV. — reserved for where the uterus is tense or for where a previous attempt without tocolysis has been unsuccessful. — A significant reduction in the incidence of caesarean (RR 0.33) has been demonstrated with the administration of betamimetic drugs where a previous attempt without tocolysis has been unsuccessful. — 250 micrograms of salbutamol in 25 ml of normal saline (10 micrograms/ml) by slow intravenous injection, or 250 micrograms of terbutaline subcutaneously. — There are insufficient data to support the use of nifedipine or atosiban compared with betamimetics and intravenous glyceryl trinitrate was inferior to subcutaneous terbutaline for tocolysis — Betamimetics should not be used in women with significant cardiac disease or hypertension, and will not be effective in those taking beta-blockers. Maternal palpitations, tachycardia, flushing, tremor and occasional nausea may be experienced. — Routine use of regional analgesia or neuraxial blockade is not recommended, but may be considered for a repeat attempt or for women unable to tolerate ECV without analgesia. — Regional anaesthesia requires less force and may reduce failure rates, particularly in conjunction with tocolysis (RR 0.61) 24 24
- 13. 6/7/1441 13 Safety measures 2/29/20 — ECV should be performed where ultrasound, cardiotocography and theatre facilities are available. — Ultrasound should be used during and after the ECV to confirm a normal fetal heart rate. — A transient (less than 3 minutes) fetal bradycardia after ECV is common,but should instigate continuous monitoring in a left lateral position, and if persistent and not improving after 6 minutes, should prompt preparation for category I caesarean section. — Urgent delivery should also be advised following the procedure if there is vaginal bleeding or unexplained abdominal pain, or if an abnormal CTG persists. — Cardiotocography should be performed after the procedure — ECV should be performed where facilities for monitoring and surgical delivery are available. — The standard preoperative preparations for caesarean section are not recommended for women undergoing ECV. — Following ECV, EFM is recommended. Women undergoing ECV who are D negative should undergo testing for fetomaternal haemorrhage and be offered anti-D. — fetomaternal haemorrhage was detected in 2.4% of women, a third of which had more than 1 ml. In one woman, the estimated fetomaternal haemorrhage was more than 30 ml. 25 25 Technique 2/29/20 — Woman lying on her back with left lateral tilt, legs half bent, bladder empty. — Perform when the uterus is relaxed. — First, push back the breech or shoulder, which is often down in the pelvis (vertical movement), then attempt rotation slowly, and always in the direction of foetal flexion: thus bringing either the head or the breech to the pelvic inlet by the shortest possible route. — Monitor the foetal heart rate after each attempt, and stop if the rate slows. — In most cases, foetal heart rate abnormalities improve within 30 minutes. 26 26
- 16. 6/7/1441 16 2/29/2031 31 Service provision 2/29/20 — There is no evidence to support any particular service model although larger institutions may consider a dedicated ECV clinic. 32 32
- 17. 6/7/1441 17 Other alternatives 2/29/20 — Women may wish to consider the use of moxibustion for breech presentation at 33–35 weeks of gestation, under the guidance of a trained practitioner. — Women should be advised that there is no evidence that postural management alone promotes spontaneous version to cephalic presentation. — Spontaneous version from breech to cephalic is unusual at term and occurs in only 8% of primigravid women after 36 weeks of gestation. — Where ECV at term has been unsuccessful, only 3 % of babies will spontaneously turn to cephalic presentation. 33 33 Breech presentation at term — Women should be informed that planned caesarean section carries — a reduced perinatal mortality and early neonatal morbidity for babies with a breech presentation at term compared with planned vaginal birth. — Women should be informed of the benefits and risks, both for the current and for future pregnancies, of planned caesarean section versus planned vaginal delivery for breech presentation at term. 2/29/2034 34
- 18. 6/7/1441 18 The technique of vaginal breech deliveries will remain integral component of obstetric practice as: — caesarean section may be inadvisable or not feasible in some patients — many women will opt for vaginal breech delivery — Intrapartum diagnosis of breech especially at advanced stage of labour — there are still unresolved issues regarding the best practice of delivering preterm breech and breech presentation in multiple pregnancies. 2/29/2035 35 —breech presentation at labour or at risk to be in labour 2/29/2036 36
- 19. 6/7/1441 19 How would you confirm the diagnosis? —An ultrasound scan (USS) is essential to confirm breech presentation. —All cases of women with preterm labour and women with preterm prelabour rupture of membranes (PPROM) should have an USS to check for fetal presentation 2/29/2037 37 Assessment of the risk factors for poor outcome 2/29/20 — Following the diagnosis of persistent breech presentation, women should be assessed for risk factors for a poorer outcome in planned vaginal breech birth. — If any risk factor is identified, women should be counselled that planned vaginal birth is likely to be associated with increased perinatal risk and that delivery by caesarean section is recommended. 38 38
- 20. 6/7/1441 20 Risk factors for poor outcome with VD 2/29/20 — Hyperextended neck on ultrasound. — High estimated fetal weight (more than 3.8 kg). — Low estimated weight (less than tenth centile). — Footling presentation. — Evidence of antenatal fetal compromise. The role of pelvimetry is unclear. 39 39 — Diagnosis of breech presentation for the first time during labour is not a contraindication for vaginal breech birth but individual cases should be assessed carefully before selection for vaginal breech birth. — Many factors can influence the choice of birth including: —the experience and the competency of the attending obstetrician —the wishes of the couple that usually determines the mode of delivery. —The presence of risk factors for poor outcome 2/29/2040 40
- 21. 6/7/1441 21 Decision 2/29/20 — Any decision to perform a caesarean section needs to be balanced against the potential adverse consequences that may result from this. — Clinicians should counsel women in an unbiased way that ensures a proper understanding of the absolute as well as relative risks of their different options. — individualised assessment of the long-term risks of caesarean section based on their individual risk profile and reproductive intentions, and counselled accordingly. 41 41 Benefits of CS 2/29/20 — Planned caesarean section leads to a small reduction in perinatal mortality compared with planned vaginal breech delivery. — Planning delivery for a breech baby, the risk of perinatal mortality is approximately 0.5/1000 with caesarean section after 39+0 weeks of gestation; and approximately 2.0/1000 with planned vaginal breech birth.This compares to approximately 1.0/1000 with planned cephalic birth. — Perinatal death is reduced due to three factors: — the avoidance of stillbirth after 39 weeks of gestation — the avoidance of intrapartum risks and the risks of vaginal breech birth — and that only the last is unique to a breech baby. 42 42
- 22. 6/7/1441 22 Risks of CS 2/29/20 — Planned caesarean section for breech presentation at term carries a small increase in immediate complications for the mother compared with planned vaginal birth — Caesarean section increases the risk of complications in future pregnancy, including the risks of opting for vaginal birth after caesarean section, the increased risk of complications at repeat caesarean section and the risk of an abnormally invasive placenta.The risk of abnormally invasive placentation increases from 0.31% with one prior caesarean section to 2.33% with four30 and the incidence is rising. — caesarean section has been associated with a small increase in the risk of stillbirth (OR 1.47) for subsequent babies although this may not be causal. 43 43 Vaginal 2/29/20 — Vaginal breech birth increases the risk of low Apgar scores and serious short-term complications, but has not been shown to increase the risk of long-term morbidity. — Selection of appropriate pregnancies and skilled intrapartum care may allow planned vaginal breech birth to be nearly as safe as planned vaginal cephalic birth. — Maternal complications are least with successful vaginal birth; planned caesarean section carries a higher risk, but the risk is highest with emergency caesarean section which is needed in approximately 40% of women planning a vaginal breech birth. 44 44
- 23. 6/7/1441 23 Intrapartum ECV 2/29/20 — It may be considered if informed consent is possible, providing the membranes are intact and no contraindications exist 45 45 Intrapartum care 2/29/2046 46
- 24. 6/7/1441 24 2/29/20 In breech: The presenting fetal diameter is bitrochanteric diameter (the distance between the outer points of the hips) and it is the same as the biparietal diameter 47 47 — Labour should be allowed to continue as long as there is evidence of progressive cervical dilatation and descent of the presenting part without any evidence of maternal or fetal compromise. — Women should have a choice of analgesia in labour, including epidural analgesia. 2/29/2048 48
- 25. 6/7/1441 25 Induction and augmentation — Women should be informed that induction of labour is not usually recommended. — Augmentation of slow progress with oxytocin should only be considered if the contraction frequency is low in the presence of epidural analgesia. 2/29/2049 49 However these Criteria should be fulfilled to allow the trial of vaginal delivery 2/29/2050 50
- 26. 6/7/1441 26 2/29/20 — Where a woman presents with an unplanned vaginal breech labour, management should depend on the stage of labour, whether factors associated with increased complications are found, availability of appropriate clinical expertise and informed consent. — Women near or in active second stage of labour should not be routinely offered caesarean section. — Where time and circumstances permit, the position of the fetal neck and legs, and the fetal weight should be estimated using ultrasound, and the woman counselled as with planned vaginal breech birth 51 51 Risks versus benefits 2/29/20 CS in advanced labour for breech presentation may be complex due to increased risks of: • GA with non fasted mother • Technical difficulties delivering the breech low in the pelvis 52 52
- 27. 6/7/1441 27 Vaginal breech delivery 2/29/2053 53 Breech delivery 2/29/2054 54
- 28. 6/7/1441 28 Setting 2/29/20 — Birth in a hospital with facilities for immediate caesarean section should be recommended with planned vaginal breech birth, but birth in an operating theatre is not routinely recommended. 55 55 2/29/20 Senior experienced obstetrician Help is essential so communicate (ISBAR) 56 56
- 29. 6/7/1441 29 Team and care — Senior midwifery, obstetric, anaesthetic and paediatric staff should be alerted to the possibility of a vaginal breech delivery.An experienced obstetrician should be available to supervise labour and delivery. — One-to-one midwifery care should also be available. — If the membranes rupture spontaneously, vaginal examination is required immediately to exclude umbilical cord prolapse. — If the membranes do not rupture spontaneously, then amniotomy should only be performed for standard obstetric indications. — Continuous electronic fetal monitoring is the mainstay for monitoring the fetus during labour. — The presence of meconium is an unreliable sign of fetal distress in breech presentation. — Fetal blood sampling from the fetal buttock is technically possible but generally not advised. 2/29/2057 57 Position 2/29/20 — Either a semirecumbent or an all-fours position may be adopted for delivery and should depend on maternal preference and the experience of the attendant. — If the latter position is used, women should be advised that recourse to the semirecumbent position may become necessary. 58 58
- 30. 6/7/1441 30 epidural analgesia 2/29/20 — Women should be informed that the effect of epidural analgesia on the success of vaginal breech birth is unclear, but that it is likely to increase the risk of intervention. 59 59 Fetal monitoring 2/29/20 —Women should be informed that while evidence is lacking, continuous electronic fetal monitoring may lead to improved neonatal outcomes. 60 60
- 32. 6/7/1441 32 management 2/29/20 — The first stage of labour should be managed according to the same principles as with a cephalic presentation. — To reduce the risk of cord compression, amniotomy is reserved for definite clinical indications. — Where the progress is slow, caesarean section should be considered. In the presence of epidural analgesia and a contraction frequency of fewer than four in ten, however, oxytocin may be considered. — A passive second stage to allow the descent of the breech to the perineum prior to active pushing is recommended — If the breech is not visible within 2 hours of the passive second stage, caesarean section should normally be recommended. 63 63 Basic principles during the 2nd stage: — Adequate descent of the breech in the passive second stage is a prerequisite for encouragement of the active second stage. — avoid handling the breech (hands off) — Many breeches will deliver without assistance — Tactile stimulation of the fetus may result in reflex extension of the arms or head, and should be minimised.. — avoid handling the umbilical cord — Art is to know when you interfer — keep the sacrum anterior — delay active pushing until the breech has descended to the pelvic floor — delay placing the mother in the lithotomy position until the fetal anus is visible over the posterior fourchette — avoid traction at all times. — Care must be taken in all manoeuvres to avoid fetal trauma: the fetus should be grasped around the pelvic girdle (not soft tissues) and the neck should never be hyperextended. — Selective rather than routine episiotomy is recommended 2/29/2064 64
- 33. 6/7/1441 33 Signs that delivery should be assisted include 2/29/20 — lack of tone or colour, or delay, commonly due to extended arms or an extended neck. — there is evidence of poor fetal condition — if there is a delay of more than 5 minutes from delivery of the buttocks to the head, or of more than 3 minutes from the umbilicus to the head. 65 65 2/29/2066 66
- 34. 6/7/1441 34 2/29/20 — Assistance, without traction, is required if there is delay or evidence of poor fetal condition. — All obstetricians and midwives should be familiar with the techniques that can be used to assist vaginal breech birth. — The choice of manoeuvres used, if required to assist with delivery of the breech, should depend on the individual experience/preference of the attending doctor or midwife.67 67 2/29/2068 68
- 39. 6/7/1441 39 2/29/2077 77 When to intervene — Prolonged 2nd stage — Pathological CTG — Back is posterior — Stopped progression at umbilicus level: — If perineum is rigid: Episiotomy — If arms are extended or Nuchal arm: : Lovset manouvre, deliver posterior arm — Arms delivered but head doesn’t follow with the next contactions:Asses where is the head — if it is outside the pelvis: flex, rotate with suprapubic pressure — if inside the pelvis assist its delivery 2/29/2078 78
- 43. 6/7/1441 43 2/29/2085 85 The Burns-Marshall method — The baby should be allowed to hang until the nape of the neck is visible so that its weight exerts gentle downwards and backwards traction to promote flexion of the fetal head. — The fetal trunk is then swept in a wide arc over the maternal abdomen by grasping both the feet and maintaining gentle traction; the aftercoming head is slowly born in this process. 2/29/2086 86
- 44. 6/7/1441 44 2/29/2087 87 The Mauriceau-Smellie-Viet manoeuvre — The Mauriceau-Smellie-Viet (MSV) manoeuvre encourages flexion of the fetal head. One hand should be placed above the fetus with one finger on the fetal occiput and one finger on each of the fetal shoulders. — The other hand should be placed below the fetus and two fingers should be placed adjacent to the fetal nose on the maxillae. Fingers should not be placed in the fetal mouth as this may be associated with jaw traction and subsequent dislocation. — Both hands are used to promote flexion of the head.The fetal body is raised upward in an arc completing delivery. — An assistant may apply suprapubic pressure to further promote flexion. 2/29/2088 88
- 46. 6/7/1441 46 2/29/2091 91 In up to 20% of vaginal breech deliveries, obstetric Killand forceps may be required to deliver the fetal head 2/29/2092 92
- 48. 6/7/1441 48 95 2/29/20 95 Management of fetal head entrapment: — Call for help – inform anaesthetist, paediatric staff, senior midwife and maternity operating theatre staff — Perform McRobert's manoeuvre as per shoulder dystocia — Apply suprapubic pressure as per shoulder dystocia — MSV manoeuvre should be reattempted in conjunction with suprapubic pressure — Rotate baby to sacro–transverse position — Administer tocolysis; consider 100 micrograms intravenous glyceryl trinitrate (GTN) — Attempt forceps delivery — Surgical management. 2/29/2096 96
- 49. 6/7/1441 49 Emergency surgical management of fetal head entrapment includes: — cervical incisions — symphysiotomy — Caesarean section — If the baby is still alive, an alternative to cervical incision and symphysiotmy is delivery by caesarean section. — The baby will need to be supported and pushed up from below. — Bracht manouver 2/29/2097 97 Duhrssen's incisions — If the head fails to deliver despite additional manoeuvres, then consideration should be made for performing cervical incisions.These are known as Duhrssen's incisions. — Ring forceps should be applied to the cervix in pairs, parallel to each other at 2, 6 and 10 o'clock.An incision should be made between each pair of forceps. — The main difficulties when performing cervical incisions for head entrapment at breech delivery are achieving adequate analgesia and exposure. — There is a significant risk of haemorrhage; the cervical incision may extend upwards within the broad ligament causing broad ligament haematoma. 2/29/2098 98
- 50. 6/7/1441 50 Preterm breech 2/29/20 — Consider caesarean section for women presenting in suspected, diagnosed or established preterm labour between 26+0 and 36+6 weeks of pregnancy with breech presentation. NICE 2015 — The mode of delivery should be individualised based on the stage of labour, type of breech presentation, fetal wellbeing and availability of an operator skilled in vaginal breech delivery. — Women should be informed that caesarean section for breech presentation in spontaneous preterm labour at the threshold of viability (22–25+6 weeks of gestation) is not routinely recommended. — Women should be informed that planned caesarean section is recommended for preterm breech presentation where delivery is planned due to maternal and/or fetal compromise. 99 99 Intrapartum 2/29/20 — Labour with a preterm breech should be managed as with a term breech. Where there is head entrapment, incisions in the cervix (vaginal birth) or vertical uterine incision extension (caesarean section) may be used, with or without tocolysis. — Specific problem encountered during preterm breech delivery is delivery of the trunk through an incompletely dilated cervix; this occurs in up to 14% of vaginal deliveries. — In this situation, lateral cervical incisions have been used to release the after-coming head. — Incisions at 2, 6 and 10 o’clock. Similar rates of head entrapment have been described for vaginal and abdominal delivery. — For head entrapment at caesarean delivery, it may be necessary to extend the uterine incision to a J shape or invertedT100 100
- 51. 6/7/1441 51 Twins 2/29/20 — Women should be informed that the evidence is limited, but that planned caesarean section for a twin pregnancy where the presenting twin is breech is recommended. — Routine emergency caesarean section for a breech first twin in spontaneous labour, however, is not recommended. — The mode of delivery should be individualised based on cervical dilatation, station of the presenting part, type of breech presentation, fetal wellbeing and availability of an operator skilled in vaginal breech delivery. 101 101 2nd twin 2/29/20 — Routine caesarean section for breech presentation of the second twin is not recommended in either term or preterm deliveries. 102 102
- 52. 6/7/1441 52 SBA 2/29/20103 103 — When performing vaginal breech delivery you... — Always have the patient in the lithotomy position Attempt to deliver flexed legs by pulling the heels Attempt to keep the sacrum posterior May use suprapubic pressure to deliver the fetal head Pull the umbilical cord to ensure it remains loose 2/29/20104 104
- 53. 6/7/1441 53 — For assisted vaginal delivery... — The Burn Marshall method involves delivering the baby by extension The Mauriceau-Smellie-Veit method involves delivering the baby by flexion by placing one finger in the baby's mouth and two fingers alongside the nose The pelvic grasp in Lovsett’s manoeuvre is a routine part of delivery for delivering the babies arms Upwards traction should only commence when the fetal chin has reached the perineum Wrigleys forceps should always be used to deliver the fetal head 2/29/20105 105 SBA — Fetal head entrapment during vaginal breech delivery... a. Consider rotating the body to sacro-transverse position b. Is more likely in term infants compared to pre-term infants c. Often requires cephalocentesis d. Should be managed with Duhrssens incisions at 3, 6 and 9 o’clock e. Wrigleys forceps should be used to achieve delivery 2/29/20106 106
- 54. 6/7/1441 54 — The correct answer is consider rotating the body to sacro- transverse position, then flexing the head via supra pubic pressure, apply traction and rotate to scaro anterior and deliver with forceps. 2/29/20107 107 Breech extraction is allowed only in 2nd twin delivery 2/29/20108 108
- 56. 6/7/1441 56 2/29/20111 111 Malpresentation Ø Breech Ø Face Ø Brow Ø Shoulder Ø Cord Ø Compound 2/29/20112 112
- 58. 6/7/1441 58 Transverse lie. Right acromiodorsoposterior position (RADP). The shoulder of the fetus is to the mother's right, and the back is posterior. 2/29/20115 115 Consequences — Presnting part, ill-fitting — Uterine Contractions, poor — Membranes, rupture early- cord prolapse — Labour, difficult, long, obstructed — Birth trauma — Operative intervention 2/29/20116 116
- 59. 6/7/1441 59 Mother, Fetus and neonate — Increased perinatal mortality and morbidity ü Fetal malformation üIntrauterine fetal death üCord proplase üBirth trauma, üBirth asphysixa üInfection, fetus, neonate and mother üUterine rupture üThromboembolism in the mother 2/29/20117 117 For Optimal Result — Early diagnosis, — Planned delivery — Experienced staff — Well equipped hospital — Cross match 2 unit — Adequate hydration — Monitor in Labour — Pain relief 2/29/20118 118
- 60. 6/7/1441 60 Face Presentaion — 1:300 — Full extension of the head — Presenting part: Face — Denominator: Omentum/Chin — Diameter; Subomento bregmatic 9.5cm — Presentation, Mento anterior–Vaginal delivery Mento posterior- Ceasaeran section 2/29/20119 119 2/29/20120 120
- 61. 6/7/1441 61 Causes — Anenecephaly — Prematurity — Multifetal pregnancy — Polyhydramnious — Neck tumours — Sternomastoid spasm — Multiparty 2/29/20121 121 Diagnosis — Abdominal — Vaginal 2/29/20122 122
- 62. 6/7/1441 62 Brow Presentation — 1:800, 1:2000 deliveries — The area between the orbital ridge and the anterior fontenalle — Most unfavourable of all presentation — Transient presentation; Full flexion—Occiput Full extension---Face 2/29/20123 123 Dignosis and management — Delivery?? 2/29/20124 124
- 63. 6/7/1441 63 Shoulder presentation qCauses — Multiparty — Prematurity — Multiple pregnancy — Polyhydrmanious congenital uterine anomly — Contacted pelvis — Pelvic tumour, placenta previae 2/29/20125 125 Compound presentation — Limb, limbs, umbilical cord alongside the presenting part; cephalic or breech 2/29/20126 126
