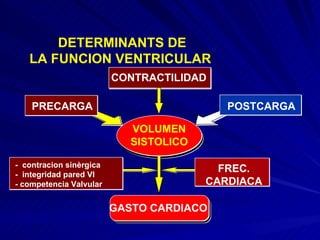
Determinantes de la función ventricular izquierda
- 1. DETERMINANTS DE LA FUNCION VENTRICULAR VOLUMEN SISTOLICO PRECARGA CONTRACTILIDAD GASTO CARDIACO FREC. CARDIACA POSTCARGA - contracion sinèrgica - integridad pared VI - competencia Valvular
- 2. Contracciòn: excitación- ingreso de calcio / puentes cruzados Actina –Miosina Relajaciòn: salida de calcio CORAZON COMO BOMBA: GENERAR PRESION Y DESPLAZAR VOLUMEN
- 3. La elevaciòn de la presiòn diastòlica final del VI Aumento De Presiòn en la AI- Aumento de presiòn Venosa pulmonar y Aumento de Presiòn Venocapilar Pulmonar (PVCP).
- 6. Hipertensión / IHD / LVD IAM Remodelamiento Arritmia VI IC Prevención (o retraso) de la Disfuncion ventricular izquierda
- 7. EVOLUCION DE ESTADIOS CLINICOS NORMAL Asymptomatic LV Dysfunction Compensated CHF Decompensated CHF No symptoms Normal exercise Normal LV fxn No symptoms Normal exercise Abnormal LV fxn No symptoms Exercise Abnormal LV fxn Symptoms Exercise Abnormal LV fxn Refractory CHF Symptoms not controlled with treatment INSUFICIENCIA CARDIACA
- 8. Correccion de factores agravantes MEDICATIONES Endocarditis Obesidad Hipertension Estrès Dieta : excesos Embarazo Arritmias (FA) Infectiones Hipertiroidismo Tromboembolismo
- 9. EDEMA AGUDO CARDIOGENICO PRESION DIASTOLICA FINAL DEL VI PRESION AURICULAR IZQ . CONGESTION EDEMA Intersticial EDEMA Alveolar PV PCP HIPERTENSION VENOCAPILAR PULMONAR (PCP > 25 mmHg)
- 11. DISNEA EDEMA INJURGITACION YUGULAR INSUFICIENCIA CARDIACA
Hinweis der Redaktion
- Pathophysiology of Congestive Heart Failure. Determinants of ventricular function. Ventricular function, and cardiac function in general, depends upon the interaction of four factors that regulate the volume of blood expelled by the heart (the cardiac output): contractility, preload, afterload, and heart rate. The first three determine the volume of blood expelled with each beat (the stroke or ejection volume), while the heart rate affects the cardiac output by varying the number of contractions per unit time. These four factors, which are intrinsic regulators of heart function, are all influenced by the nervous system. In the failing heart, especially in ischemic heart disease, it is also important to consider some purely mechanical factors, such as the synergy of ventricular contraction, the integrity of the septum, and the competence of the atrioventricular valves.
- Important Concepts. Clinical stages in the evolution of heart failure Heart failure is a continuous spectrum of changes, from the subtle loss of normal function to the presence of symptoms refractory to medial therapy. The patient with cardiomyopathy may maintain overall normal ventricular function; the progression of dysfunction may be sudden or gradual. Asymptomatic ventricular dysfunction is characterized by the absence of symptoms or decline in functional capacity, even in the absence of treatment. It may be associated with different changes in cardiac physiology, including ventricular dilatation, regional wall motion abnormalities, and decreases in the LV ejection fraction and of other parameters of ventricular function. The absence of symptoms may be explained by the heart’s functional reserve capacity and by the activation of compensatory mechanisms opposing the deterioration of cardiac function. In compensated heart failure the symptoms are controlled by medical therapy. In decompensated heart failure, symptoms persist despite usual therapy and are refractory to adjustments in drugs and dosages.
- Treatment of Heart Failure. Correction of aggravating factors Often a lack of response to conventional therapy for heart failure is due to the presence of uncorrected aggravating or precipitating factors. It is important to always consider the possibility of such factors, particularly in cases of refractory failure. AF: atrial fibrillation.