Prostaglandins pharmacology
•Download as PPT, PDF•
33 likes•17,105 views
prostaglandins
Report
Share
Report
Share
Recommended
Recommended
More Related Content
What's hot
What's hot (20)
Viewers also liked
Viewers also liked (12)
Similar to Prostaglandins pharmacology
Similar to Prostaglandins pharmacology (20)
Chemistry of Prostaglandins,Leukotrienes and Thromboxanes.pptx

Chemistry of Prostaglandins,Leukotrienes and Thromboxanes.pptx
Chemistry of Prostaglandins,Leukotrienes and Thromboxanes.pptx

Chemistry of Prostaglandins,Leukotrienes and Thromboxanes.pptx
c. Prostaglandins, Thromboxanes and Leukotrienes.pdf

c. Prostaglandins, Thromboxanes and Leukotrienes.pdf
Chemistry of prostaglandins, leukotrienes and thromboxanes

Chemistry of prostaglandins, leukotrienes and thromboxanes
Prostaglandins-Introduction and Biological Importance

Prostaglandins-Introduction and Biological Importance
EICOSONOIDS METABOLISM FOR MBBS, LAB. MED.BDS.pptx

EICOSONOIDS METABOLISM FOR MBBS, LAB. MED.BDS.pptx
Chemistry of Prostaglandins, leukotrienes and thromboxanes(Advance medicinal ...

Chemistry of Prostaglandins, leukotrienes and thromboxanes(Advance medicinal ...
Prostaglandins,Angiotensin,Bradykinin-Dr.Jibachha Sah,M.V.Sc,Lecturer

Prostaglandins,Angiotensin,Bradykinin-Dr.Jibachha Sah,M.V.Sc,Lecturer
Recently uploaded
+971581248768 Mtp-Kit (500MG) Prices » Dubai [(+971581248768**)] Abortion Pills For Sale In Dubai, UAE, Mifepristone and Misoprostol Tablets Available In Dubai, UAE CONTACT DR.Maya Whatsapp +971581248768 We Have Abortion Pills / Cytotec Tablets /Mifegest Kit Available in Dubai, Sharjah, Abudhabi, Ajman, Alain, Fujairah, Ras Al Khaimah, Umm Al Quwain, UAE, Buy cytotec in Dubai +971581248768''''Abortion Pills near me DUBAI | ABU DHABI|UAE. Price of Misoprostol, Cytotec” +971581248768' Dr.DEEM ''BUY ABORTION PILLS MIFEGEST KIT, MISOPROTONE, CYTOTEC PILLS IN DUBAI, ABU DHABI,UAE'' Contact me now via What's App…… abortion Pills Cytotec also available Oman Qatar Doha Saudi Arabia Bahrain Above all, Cytotec Abortion Pills are Available In Dubai / UAE, you will be very happy to do abortion in Dubai we are providing cytotec 200mg abortion pill in Dubai, UAE. Medication abortion offers an alternative to Surgical Abortion for women in the early weeks of pregnancy. We only offer abortion pills from 1 week-6 Months. We then advise you to use surgery if its beyond 6 months. Our Abu Dhabi, Ajman, Al Ain, Dubai, Fujairah, Ras Al Khaimah (RAK), Sharjah, Umm Al Quwain (UAQ) United Arab Emirates Abortion Clinic provides the safest and most advanced techniques for providing non-surgical, medical and surgical abortion methods for early through late second trimester, including the Abortion By Pill Procedure (RU 486, Mifeprex, Mifepristone, early options French Abortion Pill), Tamoxifen, Methotrexate and Cytotec (Misoprostol). The Abu Dhabi, United Arab Emirates Abortion Clinic performs Same Day Abortion Procedure using medications that are taken on the first day of the office visit and will cause the abortion to occur generally within 4 to 6 hours (as early as 30 minutes) for patients who are 3 to 12 weeks pregnant. When Mifepristone and Misoprostol are used, 50% of patients complete in 4 to 6 hours; 75% to 80% in 12 hours; and 90% in 24 hours. We use a regimen that allows for completion without the need for surgery 99% of the time. All advanced second trimester and late term pregnancies at our Tampa clinic (17 to 24 weeks or greater) can be completed within 24 hours or less 99% of the time without the need surgery. The procedure is completed with minimal to no complications. Our Women's Health Center located in Abu Dhabi, United Arab Emirates, uses the latest medications for medical abortions (RU-486, Mifeprex, Mifegyne, Mifepristone, early options French abortion pill), Methotrexate and Cytotec (Misoprostol). The safety standards of our Abu Dhabi, United Arab Emirates Abortion Doctors remain unparalleled. They consistently maintain the lowest complication rates throughout the nation. Our Physicians and staff are always available to answer questions and care for women in one of the most difficult times in their lives. The decision to have an abortion at the Abortion Clinic in Abu Dhabi, (United Arab Emirates)+971581248768+971581248768>> SAFE AND ORIGINAL ABORTION PILLS FOR SALE IN DUBAI AND ABUDHA...

+971581248768>> SAFE AND ORIGINAL ABORTION PILLS FOR SALE IN DUBAI AND ABUDHA...?#DUbAI#??##{{(☎️+971_581248768%)**%*]'#abortion pills for sale in dubai@
Recently uploaded (20)
FAIRSpectra - Enabling the FAIRification of Spectroscopy and Spectrometry

FAIRSpectra - Enabling the FAIRification of Spectroscopy and Spectrometry
pumpkin fruit fly, water melon fruit fly, cucumber fruit fly

pumpkin fruit fly, water melon fruit fly, cucumber fruit fly
PATNA CALL GIRLS 8617370543 LOW PRICE ESCORT SERVICE

PATNA CALL GIRLS 8617370543 LOW PRICE ESCORT SERVICE
Locating and isolating a gene, FISH, GISH, Chromosome walking and jumping, te...

Locating and isolating a gene, FISH, GISH, Chromosome walking and jumping, te...
Thyroid Physiology_Dr.E. Muralinath_ Associate Professor

Thyroid Physiology_Dr.E. Muralinath_ Associate Professor
+971581248768>> SAFE AND ORIGINAL ABORTION PILLS FOR SALE IN DUBAI AND ABUDHA...

+971581248768>> SAFE AND ORIGINAL ABORTION PILLS FOR SALE IN DUBAI AND ABUDHA...
Human & Veterinary Respiratory Physilogy_DR.E.Muralinath_Associate Professor....

Human & Veterinary Respiratory Physilogy_DR.E.Muralinath_Associate Professor....
Selaginella: features, morphology ,anatomy and reproduction.

Selaginella: features, morphology ,anatomy and reproduction.
Pulmonary drug delivery system M.pharm -2nd sem P'ceutics

Pulmonary drug delivery system M.pharm -2nd sem P'ceutics
The Mariana Trench remarkable geological features on Earth.pptx

The Mariana Trench remarkable geological features on Earth.pptx
Biogenic Sulfur Gases as Biosignatures on Temperate Sub-Neptune Waterworlds

Biogenic Sulfur Gases as Biosignatures on Temperate Sub-Neptune Waterworlds
Prostaglandins pharmacology
- 2. Prostaglandins and related compounds are collectively known as eicosanoids. Most are produced from arachidonic acid, a 20-carbon polyunsaturated fatty acid (5,8,11,14-eicosatetraenoic acid). The eicosanoids are considered "local hormones." They have specific effects on target cells close to their site of formation. They are rapidly degraded, so they are not transported to distal sites within the body. But in addition to participating in intercellular signaling, there is evidence for involvement of eicosanoids in intracellular signal cascades. INTRODUCTION
- 3. DISCOVERY OF PROSTAGLANDINS • It was discovered by Ulf Von Euler (1930) • He extracted from human semen. • It is secreted from prostate gland. • Structure of prostaglandins - proposed by Bergstrom (1950).
- 4. Examples of eicosanoids: prostaglandins prostacyclins thromboxanes leukotrienes epoxyeicosatrienoic acids. They have roles in: inflammation fever regulation of blood pressure blood clotting immune system modulation control of reproductive processes & tissue growth regulation of sleep/wake cycle.
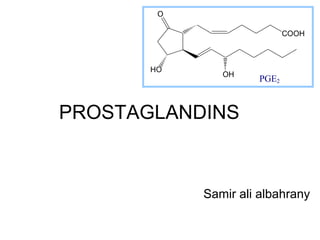
- 5. Arachidonic acid COOH PGE2 (prostaglandin E2) is an example of a prostaglandin, produced from arachidonic acid. COOH O HO OH PGE2
- 6. Prostaglandin receptors: Prostaglandins & related compounds are transported out of the cells that synthesize them. Most affect other cells by interacting with plasma membrane G-protein coupled receptors. ♦ Depending on the cell type, the activated G- protein may stimulate or inhibit formation of cAMP, or may activate a phosphatidylinositol signal pathway leading to intracellular Ca++ release.
- 7. Prostaglandin receptors are specified by the same letter code. E.g., receptors for E-class prostaglandins are EP. Thromboxane receptors are designated TP. Multiple receptors for a prostaglandin are specified by subscripts (E.g., EP1, EP2, EP3, etc.). Different receptors for a particular prostaglandin may activate different signal cascades. Effects of a particular prostaglandin may vary in different tissues, depending on which receptors are expressed. E.g., in different cells PGE2 may activate either stimulatory or inhibitory or G-proteins, leading to either increase or decrease in cAMP formation.
- 8. Prostaglandin H2 Synthase catalyzes the committed step in the “cyclic pathway” that leads to production of prostaglandins, prostacyclins, & thromboxanes. Different cell types convert PGH2 to different compounds. leukotrienes phospholipids arachidonate diacylglycerol prostaglandin H2 prostacyclins thromboxanes other prostaglandins Lipoxyganase PGH2 Synthase Prostacyclin Synthase Thromboxane Synthase Linear pathway Cyclic pathway Two major pathways of eicosanoid metabolism. Cyclic pathway:
- 9. PGH2 Synthase is a heme-containing dioxygenase, bound to ER membranes. (A dioxygenase incorporates O2 into a substrate). PGH2 Synthase exhibits 2 activities: cyclooxygenase & peroxidase. COOH COOH O O OH COOH O O OOH 2 O2 2 e− arachidonic acid PGG2 PGH2 Cyclooxygenase Peroxidase
- 10. Ibuprofen and related compounds block the hydrophobic channel by which arachidonate enters the cyclooxygenase active site. Non-steroidal anti-inflammatory drugs (NSAIDs), such as aspirin and derivatives of ibuprofen, inhibit cyclooxygenase activity of PGH2 Synthase. They inhibit formation of prostaglandins involved in fever, pain, & inflammation. They inhibit blood clotting by blocking thromboxane formation in blood platelets. CH COOHH3C CH2 CH CH3H3C Ibuprofen
- 11. Aspirin acetylates a serine hydroxyl group near the active site, preventing arachidonate binding. The inhibition by aspirin is irreversible. However, in most body cells re-synthesis of PGH2 Synthase would restore cyclooxygenase activity. Aspirin + + PGH2 Synthase (active) COOH O C CH3 O Enz-Ser CH2 OH COOH OH Salicylic acid Enz-Ser CH2 Acetylated PGH2 Synthase (inactive) O C CH3 O
- 12. Thromboxane A2 stimulates blood platelet aggregation, essential to the role of platelets in blood clotting. Many people take a daily aspirin for its anti- clotting effect, attributed to inhibition of thromboxane formation in blood platelets. This effect of aspirin is long-lived because platelets lack a nucleus and do not make new enzyme.
