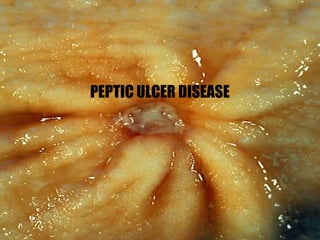
Peptic Ulcer Disease
- 2. INTRODUCTION Peptic Ulcer (PU) An abnormal area of mucosa due to damage by the pepsin and HCl of gastric juice, with consequent inflammation of underlying and surrounding tissues. Areas of mucosal ulceration from exposure to acid- pepsin secretions. Can be either benign or malignant. Occurs mostly in duodenum or stomach (low pH; aids pepsin’s action). Bleeding – when erosion progresses into the lamina propria and submucosa. [Lamina propria: below epithelium; constituent of the mucosa; in combination with epithelium, constitutes the mucosa].
- 3. Epidemiology: Is a common condition; Affects 10% of population worldwide. Duodenal Ulcers (DU) are more common than Gastric Ulcers (GU); occurs in duodenal cap. GU occurs in the lesser curvature of the stomach. Ulcers – usually self-healing, if balance between erosive and protective factors is restored. GERD – ulcers that occur in lower esophagus due to refluxing. ‘Non-ulcer Dyspepsia’ – clinical manifestations suggest PU, but endoscopic examination does not reveal any ulcer.
- 6. CLASSIFICATION 1] Acute Ulcers (Stress) 2] Chronic Ulcers – Gastric Ulcers (GU) Duodenal Ulcers (DU) ACUTE (STRESS) PU • Small, multiple mucosal ulcers in stomach; (in duodenum occasionally). • Etiology : Stress (main cause); Chronic use of NSAIDs; extensive burns; MI; Hemorrhage; Sepsis; Local irritants; Upper GI bleeding. • Hypoxic injury to mucosal cells and depletion of mucosal defence.
- 7. CHRONIC ULCERS: • Comprises Gastric Ulcers (GU) and Duodenal Ulcers (DU). Gastric Ulcers: • Less common; in lesser curvature of stomach. • Patients – low to normal gastric acid levels; but… hyperacidity (↑ed serum gastrin levels). • Impaired mucosal resistance mucosal digestion w/→ low or normal acid or pepsin levels. • Affects both sexes equally: > 40yrs. • Causes : H.pylori infection, pyloroduodenal reflux, mucosal trauma, local ischaemia, prolonged NSAIDs use.
- 8. Classification (contd’.) Duodenal Ulcers: • Most common type; occurs in duodenum. • 40 – 50 yrs.; more common in males. • Parietal cells’ and acid output is double that of normal persons.
- 10. ETIOLOGY Acid hypersecretion H.pylori infection Bronchial carcinoma Histamine, gastrin (excess) Cushing’s Syndrome Anxiety Liver Cirrhosis Stress Tea, Coffee (excess) Reduced Bicarbonate production Cigarettes Irregular and spicy diet.
- 12. AETIOLOGY • Multifactorial…. 1] Failure of Protective mechanisms: • Mucus, Bicarbonates, PGs, Mucosal renewal, Mucosal blood flow. 2] Injurious Factors: • Pepsin, Bile reflux, Gastric acid, H.pylori, Slow gastric emptying, PG deficiency. 3] Peptic Ulceration: • Drugs, Stress, Alcohol, Smoking. 4] Ineffective Healing: • Antacids, Antisecretory agents, Antimicrobials, Mucosal protectants, PGs analogues.
- 13. CLINICAL FEATURES Pain (discomfort to severe) – in epigastric region; When ulcers penetrate to other organs ( c/o backache, lower abdominal pain) ‘Burning or gnawing’ pain. Spontaneous night pain → Insomnia. ‘Chest pain’ (due to acid reflux). Weight change, dysphagia, vomiting, anaemia. DU: relative weight gain, burning, soreness, midmorning pain (relieved after taking food or milk) GU: Weight loss, Daytime pain, bloating, NV.
- 14. INVESTIGATIONS • General Examination : P/E and patient’s history. • Hematological Tests : ↓ed Hb levels (hematemesis, anaemia, melaena) ↑ed ESR (indicative of H.pylori infection). • Fibreoptic endoscopy (95% success rate in identifying ulcers). • Barium swallow test : X-ray of Ba -filled stomach and duodenum; 75% success rate.
- 15. MANAGEMENT Objectives : a] To relieve pain and discomfort. b] To accelerate healing. c] To prevent recurrence and complications. GENERAL MEASURES Regular small meals (avoid late snacks – stimulate nocturnal gastric secretion). Avoid spicy food. Avoid strong coffee, tea, smoking, alcohol. Avoid NSAIDs (aspirin). Avoid anxiety and stress (indulge in a tranquil lifestyle; hobbies). Avoid excess of Bed rest.
- 16. PHARMACOLOGICAL TREATMENT Objectives : • Relieve symptoms (neutralize acid or reduce acid secretion). • Promote healing (enhance mucosal resistance, reduce acid secretion, eliminate bacterial gastric infection). 1] ANTACIDS • Sole Tx in young patients (< 40 yrs.) and • Those with chronic, stable, mild symptoms. • Egs.: Al. Hydroxide, Mg. Sulphate 2] ANTISECRETORY AGENTS I. Proton Pump Inhibitors (PPIs) II. H2-receptor antagonists or blockers (H2RA or H2RB)
- 17. PROTON PUMP INHIBITORS (PPIs) • More rapid healing of DUs; • OD at bedtime for 6 – 8 weeks. • Omeprazole (20 mg); Esomeprazole (20 mg); Lansoprazole (30 mg); Pantoprazole; Rabeprazole. • Powerfully inhibit H+ /K+ -ATPase pathway (final step in gastric acid secretion). • Omeprazole: - Prodrug; concentrates in parietal cells; - Binds irreversibly to H+ /K+ -ATPase→ Achlorhydria. - Though acid-metabolized, it inhibits future acid secretion ( B↑ A). - t1/2 = 1 hr; Duration of action is 24 hrs. (irreversible enzyme inhibition). - OD dose is sufficient. • Side effects : NVD, Constipation, headache, Rashes, Pruritis, Abdominal pain, Bronchospasm, Muscle & joint pain, Dry mouth, Blurred vision, Depression
- 18. H2RAs or H2RBs • Block histamine-mediated acid secretion from parietal cells. • Ranitidine (300 mg), Cimetidine (800 mg), Famotidine (40 mg) and Nizatidine. • OD at bedtime for 6 – 8 weeks. • In ZES, Stress ulcers. • Ranitidine Bismutrex • Ranitidine + protective Bismuth; for 4 – 8 weeks • Side effects : GI side effects, Confusion, Depression, Hallucinations, Bradycardia, AV block (rare). • Absorption may be reduced by co-administration with high doses (2gms) of Sucralfate. • Cimetidine : • potentiates actions of Warfarin, Theophylline, Phenytoin and beta blockers.
- 19. 3] MUCOSAL PROTECTANTS • Form a protective coat by binding w/ ulcer crater. • Egs. : Bismuth Chelate (Tripotassium dicitratobismuthate); Sucralfate (Al.Hydroxide + sucrose+ sulfate); forms a paste on ulcer surface; 2 gms bd Bismuthate Chelate : • Active vs H.pylori, es mucosal resistance levels↑ , es↓ pepsin secretion. • Tablets – more palatable. • Liquid form – has ammonia to maintain colloidal state; So, dilute before use. • Consume w/ glass of water. • Don’t consume w/ food, milk and antacids (minimum of 30 mins. ac and pc ). • Can cause greyish-black stools.
- 20. Sucralfate : • Same action of bismuth. • Also, stimulates additional PG synthesis and mucus secretion. • Twice daily is sufficient. 4] ANTIBIOTICS • Mainly to eradicate H.pylori. • Tetracyclines, Metronidazole, Amoxycillin (commonly used). • Can be co-administered w/ PPIs and Ulcer protectives. • Tetracyclines can cause photosensitivity; Metronidazole can cause diarrhoea;
- 21. 5] ANTIMUSCARINICS / ANTISPASMODICS • Block acid secretion. • Atropine, Propantheline, Hyoscine, Pirenzepine. • Adjunct to antacids. • Restricted use – Low therapeutic index, Antimuscarinic side effects. • Useful at night (lower side effects, to reduce motility → retains antacids in stomach). • Pirenzepine – Binds selectively to gastric M2 receptors; reduce acid and pepsin secretion.
- 22. 6] PROSTAGLANDINS • PGE analogues are used ( Acid-inhibiting and cytoprotective properties). • Misoprostol, Arbaprostil and Enprostil. • Arbaprostil and Enprostil – inhibit gastric secretion and release. • PGS – less effective than H2RAs. • Side effects : Diarrhoea, Abdominal pain.
- 24. SURGERY • Gastrectomy, Vagatomy. • Rarely performed; • For complicated, resistant and relapsing ulcers; • Can cause weight loss, anaemia, malabsorption syndrome, carcinoma.
- 25. PUD CPGs [Clinical Practice Guidelines]
- 26. Therapeutic regimes used for eradication of H.pylori Colloidal bismuth subcitrate 1 tab (120mg) qid or 2 (240mg) tablets bd Amoxycillin 500mg tds or Tetracycline 500mg tds Metronidazole 400mg tds [for 2 weeks] Omeprazole 40mg daily or 20mg bd Amoxycillin 500mg tds or Clarithromycin 500mg tds [for 2 weeks]
- 27. For H.pylori-induced ulcers (contd’.) Omeprazole 20mg daily or bd and two of the following: - Metronidazole 400mg bd - Amoxycillin 500mg bd - Clarithromycin 250mg or 500mg bd [for 1 week] H2 receptor antagonist (Ranitidine 300mg daily or Famotidine 40mg daily) - Amoxycillin 500mg tds - Metronidazole 400mg tds [for 2 weeks]
- 28. Non-H.pylori Related Peptic Ulcer Disease A. NSAIDs and PUD First step – withdrawal or reduction of NSAID dose to the lowest minimum. For NSAID-induced DU and smaller GU, full dose of H2RA for a minimum of 8 weeks. For larger GUs, • PPIs (eg. Omeprazole at 20 - 40 mg/day) for 8 weeks or • H2RA (full dose) for upto 12 weeks is as effective. • PG analogue (Misoprostol 800 ug/day in divided doses) is also effective in healing NSAID induced GU and possibly DU. If the clinical situation requires the continued administration of NSAIDs in the presence of healed ulcer, concurrent administration of anti-secretory drugs or PG analogue is recommended.
- 29. B. Refractory Ulcer Non-healing ulcer / resistant ulcer / ‘slow- to-heal’ ulcer Are PUs that do not heal following at least 3 months of treatment with H2RA or PPIs at standard doses recommended for ulcer healing. Management • Where specific Dx has been made, appropriate therapies should be given. • Multiple biopsies of ulcers (at least 6) at each and every endoscopy until healing is complete and documented. • All patients should be advised to stop smoking. • Stop or reduce the use of NSAIDs and steroid when this is feasible. Consider alternative in place of NSAIDs.
- 30. Treatment Options: PPIs • The best option for treatment. • A higher dose is usually necessary and it may be necessary to continue treatment for at least 3 months. • Surgical option should be considered if ulcer remains unhealed after 6 months of therapy. • In case of relapse following termination of treatment, maintenance therapy with PPIs at dosages comparable to that used for ulcer healing may be necessary to prevent relapses.
- 31. C. Long-Term Maintenance Therapy H2RA • There is conclusive evidence that H2RAs substantially reduce the frequency of symptomatic relapse, and reduce the recurrence of DU haemorrhage. PPIs • Effective and safe alternative to the H2RAs. Other substances (sucralfate, PG analogues or antacids) are not used to the same extent as the H2RAs for long term therapy. Intermittent treatment – an alternative option; may be more cost effective to long term maintenance therapy. There is yet no evidence to prove that intermittent therapy is a safe and effective alternative to continuous maintenance therapy. Until more conclusive data is available, continuous therapy is preferred. In patients with no contraindications, surgery is an alternative to long term maintenance therapy.
- 32. D. Stress Ulcers Prophylaxis is directed towards the • reduction of the volume of gastric acid secretion thereby reducing its acidity (ie increase in pH) or • offering mucosal protection (cytoprotective effect). Sucralfate; Antisecretory agents (H2RAs and PPIs) Bolus a. Cimetidine 200 mg i.v. b. Ranitidine 50 mg i.v. Continuous infusion a. Cimetidine 50-100 mg hourly after a bolus of 200 mg b. Ranitidine 6.25 - 12 mg hourly after a bolus of 50 mg
- 33. Quadruple Therapy • Bismuth, 2 antibiotics, 1 PPI or H2RB for 14 days. • Usual dosages: • Bismuth subsalicylate (two 262-mg tablets 3-4x/day or 30 mL liquid 3-4x/day) • Metronidazole one 250-mg tablet 4x/day • Tetracycline one 500-mg capsule 4x/day • PPI (same dosage as in triple therapy) or • H2RAs – Nizatidine (one 150-mg capsule 2x/day) or – Famotidine (one 20-mg tablet 2x/day) – Cimetidine (one 400-mg tablet 2x/day) – Ranitidine (one 150-mg tablet 2x/day) (www.healthcommunities.com)
- 34. THANK YOU!!!