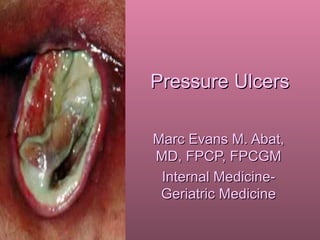
Pressure ulcers
- 1. Pressure Ulcers Marc Evans M. Abat, MD, FPCP, FPCGM Internal Medicine- Geriatric Medicine
- 2. Definition • Any lesion caused by unrelieved pressure leading damage of underlying tissue – Synonymous to decubitus ulcer and bedsores but the above term denotes the primary pathophysiologic factor
- 3. Staging • Stage I – Nonblanchable erythema of intact skin; may also be other discoloration, warmth, edema and induration – 10-fold increase in risk of developing higher-staged ulcers
- 4. • Stage II – Partial-thickness skin loss involving the epidermis or also the dermis • Stage III – Extend to the subcutaneous tissues and deep fascia – Typically show undermining • Stage IV – Involve muscle and bone
- 5. Stage I Stage II Stage III Stage IV
- 11. • Eschar formation – Full-thickness injury – Has to be removed prior to staging • Pressure-related blister formation – Cannot be staged clinically
- 12. Epidemiology • Acute care setting – Stage II and higher prevalence 3-11%, incidence 1-3% – After 1 week of confinement, incidence 28%, prevalence 8-30% – >50% occur in patients >70 years old
- 13. • In nursing homes – Prevalence of 20-33% and incidence of 11- 14% • Sepsis – Most serious complication of pressure ulcers – In-house mortality of 60% when the ulcer is the source of bacteremia
- 14. • Infected pressure ulcers – Most common infection in skilled nursing facilities (6% of residents) • Osteomyelitis – In 26% of non-healing pressure ulcers
- 15. • Associated with prolonged and expensive hospitalizations • Associated with pain – 59-85% of those who can communicated describe pain – 45% report ulcer pain as “horrible”
- 16. • Increased mortality – 60% at 1 year after discharged for those who develop a pressure ulcer
- 17. Pathophysiology • 4 factors implicated: pressure, shearing forces, friction and moisture • Muscle and subcutaneous tissuemore sensitive to pressure injury
- 19. • Pressure on bony prominences – 100-150 mmHg on regular mattress while lying down – 300 mmHg on ischial tuberosities while sitting – Enough to decrease transcutaneous oxygen tension to 0 • Other factors may lower the time or pressure needed to cause full-thickness injuries
- 20. • Shearing forces-tangential forces on the skin when the patient slides while sitting or lying down in an elevated position – Lowers the pressure needed to cause ulcers • Friction leads to intraepidermal blistersunroofed, leading to superficial erosions • Moisturemay lead to maceration
- 23. • Effect of pressure – Ischemia and accumulation of cellular toxins – Damage begins in deeper tissues – Persistent pressurevascular leakage and interstitial edemaeventual hemorrhage (stage I) • Superimposed bacterial infection (both deep and superficial)
- 25. Presentation • Any disease that leads to immobility predisposes to pressure ulcers • Risk factors other than immobility – Incontinence (particularly fecal) – Nutritional factors (decreased lymphocyte count, hypoalbuminemia, inadequate intake, decreased body weight, depleted triceps skin fold)
- 26. • Other factors – Dry skin – Increased body temperature – Decreased blood pressure – Age – Age-related skin changes
- 27. Assessment • Includes assessment of risk factors, including nutritional assessment • Location, size, stage and wound characteristics of ulcer at onset – Includes assessment of tracts, undermining, tunneling, exudate, necrotic tissue, granulation and epithelialization
- 29. • Follow-up assessment using above parameters at least weekly – PUSH score – Decrease in ulcer size over 2 weeks usually predicts healing • Sinograms to assess tract extent • Cultures using needle aspiration or biopsy speciments; may include bone biopsys – Culture of swabs not helpful as bacterial colonization in eventual – Important if ulcer does not heal after 4 weeks or if with obvious infection
- 32. • Osteomyelitis diagnosis may be difficult due to similarity of pressure-induced bone changes – Presence of abnormal plain radiograph, WBC count of 15,000 and ESR >120 mm has probability of osteomyelitis of 70%
- 33. • Most common bacterial isolates – Gram (-) aerobic rods (45% of isolates) – Gram (+) aerobic cocci (39%) – Bacteroides species, most common anaerobic isolate
- 34. Management Pharmacologic • Vitamin and mineral supplementation for those with deficiencies • Systemic antibiotics indicated for patients with – Sepsis – Cellulitis – Osteomyelitis – Prevention of bacterial endocarditis in those with VHD and requiring debridement
- 35. • Broad spectrum antibiotics for those with suspected bacteremia, pending culture results – Ampi-sulbactam – Carbapenems – Pip-tazo – Clindamycin/metronidazole + quinolones
- 36. • Vancomycin for methicillin-resistent Staphylococcus aureus • Deeper ulcers may have some benefit for topical antibiotics – Silver sulfadiazine x 2 weeks – Avoid iodophors, sodium hypochlorite or acetic acid (toxic to fibroblast)
- 37. Nonpharmacologic • Adequate dietary, especially protein intake – Target 30-35 kcal/kg BW/day with 1.25- 1.50 g CHON/kg BW – May use alternative feeding methods if oral intake is inadequate – Vitamin and mineral supplementation
- 38. • Use of pressure-relieving devices – Regular air/foam mattresses – Egg-crate foam mattresses – Static mattresses (should not bottom out and provide at least 2.5 cm of support) • Usually appropriate for those who can still assume different positions – Dynamic mattresses • Air-fluidized mattresses • Low-air loss mattresses
- 42. • Debridement – Sharp debridement – Mechanical approaches (wet-to-dry dressing, irrigation, hydrotherapy) • Irrigation pressure 4-15 psi using a 30-cc syringe with a 18G needle – Enzymatic approaches (collagenases) – Autolytic approaches (contraindicated in infected ulcers)
- 43. • Occlusive dressings for clean wound – Not proven to me more effective for stage III or IV ulcers but reduces the nursing time needed • Moist gauze dressing using normal saline for the ulcer base • The aim of dressing the ulcer is to maintain a moist environment for would healing and autolytic debridement
- 46. • Skin sealants – Prevents friction and protects from adhesives – Contains alcohol and should not be used under most hydrocolloids
- 47. • Impregnated gauze – Gauze impregnated with saline or other substances – Make sure that impregnating substance is not harmful to wound healing – Limited absorbent capacity
- 48. • Composite dressings – Combination of different dressing groups – Properties depend on the components
- 49. • Transparent film dressing – Polyurethane and polyethylene membrane coated with a layer of acrylic, hypoallergenic adhesive – Promotes epithelialization, moist wound healing – Bacterial barrier, autolysis – May reinjure wound on removal – Can lead to wound edge maceration – Not for wounds with moderate to heavy exudation
- 50. • Hydrocolloid – Gelatin or carboxymethycellulose in a polyisobutylene adhesive base – Moist would healing with absorption of light to moderate wound fluid – Increased wear time – Reduces pain, promotes autolysis – Not for those withg heavy exudate – Odor on removal – Limited absorption
- 51. • Hydrogels – May or may not have supporting fabric net – High water content with varying gel forming material – Moist wound healing with low to moderate drainage – Promotes autolysis – Reduces pain and rehydrates dry wounds; cooling effect – Does not cause reinjury on removal – Can dry out or may macerate surrounding tissues – Candidiasis may occur with inappropriate use
- 52. • Wound fillers – Made of copolymer starch or dextranomer beads which absorb wound fluid to form a gel – Moderate to large absorption and fills up dead space – Moisture retentive and promotes autolysis – Requires another dressing to hold it in – May have an odor – Requires wound irrigation to remove
- 53. • Enzyme debriding agent – Can debride necrotic tissue – Hard eschar chould be removed first – Discontinued when granulation appears – Require secondary dressing – May be inhibited by irrigation solutions
- 54. • Alginates – Calcium or sodium salts of alginic acid – Moisture retentive and promotes autolysis – Moderate to large moisture absorption – Reduces pain and can fill dead space – Should not be used in low-exudate wounds and may dry out
- 55. • Lubricating agents – Promotes moist wound healing – Limited autolysis – Reduces pain – Requires secondary dressing – Non-absorptive – May be used to impregnate gauze
- 56. • Foams – Hydrophilic and non- adherent modified polyurethane foam – In wafers, pillows; with film covers – Surfactant impregnated or with a charcoal layer – Moderate to large absorption – Moist wound healing – Can be used with topical medications and infected wounds – Requires taping
- 57. • Collagen – Bovine collagen attached to nylon mesh, or powder or paste – Also comes in 90% collagen and 10% alginate – Absorbs small to moderate exudate – Non-adherent – For contaminated, infecteed wounds – Can be used with topical agents – Requires secondary dressing – Sensitivity to bovine material
- 58. • Surgical correction (attempted only in clean wounds) – Primary closure – Skin grafting – Myocutaneous flaps • 30% complication rate • Complications included necrosis, dehiscence, flap infection, hematoma • 70% healing rate by time of discharge – Removal of underlying bony prominences
- 59. • Other modalities – Hyperbaric oxygen therapy • Effects not statistically significant – Growth factors • For ulcers that do not heal with a comprehensive approach – Larvae therapy – Vacuum-assisted closure • Reduces bacterial load and improves perfusion and granulation – Electrical stimulation • Improves healing in small trials; dose and type of wound to be applied with not yet determined
- 60. Prevention • Systematic risks assessment – Braden scale • A score of 18 or less in any patient indicates risk for pressure ulceration – Norton scale
- 63. • Appropriate skin care – Systematic skin inspection – Skin cleaning with mild cleansing agent at time of soiling and at regular intervals – Minimize skin dryinguse moisturizers – Minimize excessive moisture – Minimize friction and shear forces – Ensure adequate dietary intake
- 64. • Frequent repositioning every 2 hours for supine patients – The back should be at a 30° angle with the support surface; avoid a 90° angle – Minimize head elevation to compelling indications like postfeeding or if in respiratory distress • If patient needs to be seated, should not be for more than 1 hour; positions are shifted every 15- 30 minutes – May use pillows behind the knees, back or neck to provide more support – Avoid doughnut rings (increases venous congestion)
- 65. • Off-loading devices of extremities in the supine or seated position • Sheepskin and foam egg crate mattress (or other foam overlays) – Inexpensive but do not have the capability of reducing pressure enough to reduce injury • Use of pressure-relieving mattresses – 60% reduction in incidence of pressure ulcers
- 66. • Treatment of infections distant from clean pressure ulcers – Bacteremia from distant infections may seed in the clean ulcer due to least resistance
