Lecture 10 valvular heart disease - Pathology
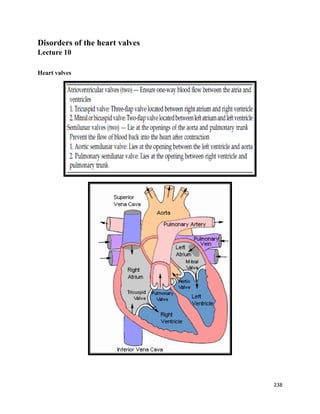
- 1. Disorders of the heart valves Lecture 10 Heart valves 238
- 2. Disorders of the heart valves Damage and dysfunction of the heart valves most commonly occurs as a result of : Infective endocarditis or Rheumatic fever Ischemia Direct trauma Congenital defects or abnormalities of the heart valves Overview Two major types of changes are seen in heart valves: Stenosis and Regurgitation (also called insufficiency or incompetence) Aortic Stenosis Mitral Stenosis Aortic Regurgitation • Acute and Chronic Mitral Regurgitation • Acute and Chronic Valvular Stenosis The valve opening narrows The valve leaflets may become fused or thickened that the valve cannot open freely obstructs the normal flow of blood EFFECTS: the chamber behind the stenotic valve is subject to o greater stress must generate more pressure or work o hard to force blood through the narrowed opening initially, the heart compensates for the additional workload by gradual hypertrophy and dilation of the myocardium heart failure 239
- 3. Valvular Insufficiency or Regurgitation Scarring and retraction of valve leaflets or weakening of supporting structures incomplete closure of the valve result to leakage or backflow of blood from the previous chamber EFFECTS: o causes the Heart to pump the same blood twice (as the blood comes back into the chamber) o the Heart dilates to accommodate more blood (the usual blood it needs to pump + regurgitated blood) o ventricular dilation and hypertrophy eventually leads to heart failure Heart sounds 240
- 4. Heart Murmur: is an extra or unusual sound heard during a heartbeat. Mnemonic: Systolic Murmurs ( ASaMR) Diastolic Murmurs (ARMS) Aortic Stenosis Aortic Stenosis Overview: Normal Aortic Valve Area: 3-4 cm2 Symptoms: Occur when valve area is 1/4th of normal area. Types: o Supravalvular o Subvalvular o Valvular 241
- 5. The normal aortic valve consists of three thin and pliable valve leaflets Bicuspid aortic valve (BAV) is a congenital condition of the aortic valve where two of the aortic valvular leaflets fuse during development resulting in a valve that is bicuspid (2 leaflets) instead of the normal tricuspid configuration. Persons born with an abnormal bicuspid valve are particularly susceptible to calcification later in life. Normally the only cardiac valve that is bicuspid is the mitral valve (bicuspid valve). Aortic Stenosis 242
- 6. Aortic Stenosis causes & Consequences may be due to rheumatic heart disease, atherosclerosis, congenital valvular disease or malformations narrowing of the aortic valve flow of blood from the left ventricle to the aorta blood volume and pressure in the left ventricle Left ventricle hypertrophy develops as a compensatory mechanism to continue pumping blood through the narrowed opening Patients under 70: >50% have a congenital cause Patients over 70: 50% due to degenerative 243
- 7. Pathophysiology of Aortic Stenosis Clinical Manifestations fatigue & exertional dyspnea – 1st symptoms – due to CO and pulmonary congestion chest pain (angina) – most common symptom o occurs during exercise – due to inability of the heart to increase coronary blood flow to cardiac muscle exertional syncope, vertigo, periods of confusion -- CO weakness, orthopnea, PND, pulmonary edema (severe cases) signs of right-sided heart failure –- end-stage symptoms - if untreated, survival rate: 1.5-3 years Auscultation: harsh, rough, mid-systolic ejection murmur 244
- 8. Management of AS General- IE prophylaxis in dental procedures with a prosthetic AV or history of endocarditis. Medical: o limited role since AS is a mechanical problem. o restrict activity o digitalis o Na+ restriction, diuretics o Nitroglycerin – for chest pain Surgical: o Aortic Balloon Valvotomy- shows little benefit. o Surgical Replacement: Definitive treatment (even in elderly and CHF) 245
- 9. Mitral Stenosis Mitral stenosis Definition Mitral stenosis is characterized by thickening, fibrosis and hardening of the mitral annulus, such as mitral orifice narrows and blood cannot pass by to the left ventricle. obstruct blood flow from left atrium to the left ventricle that prevents LV proper filling during diastole The consequence of this is the accumulation of blood in the left atrium and then to the lungs (heart failure and pulmonary edema). Normal MV Area: 4-6 cm2 , symptoms begin at areas less than 2 cm2 Mitral Stenosis Overview Most common valvular disorder in Rheumatic Heart Disease (RHD) Considered late complications of rheumatic fever. Rheumatic fever is a late sequela to Group A β-hemolytic streptococcal infection of the throat. However, most often strep infection is asymptomatic and thereby properly left untreated (treatment consist in eradication of infection with penicillin). 246
- 10. 14 days after the onset of infection a series of immune complexes are formed with high affinity for connective tissue (like heart valves – M protein). Mitral stenosis occurs after a free interval of 10-20 years from initial rheumatic attack, but is often asymptomatic in the early stages. The incidence of rheumatic mitral stenosis decreased in recent years due to the identification and proper treatment of beta-hemolytic streptococci infection. However, the condition is quite common in cold and wet climates. Mitral Stenosis 247
- 11. Mitral Stenosis Pathophysiology MS Symptoms & Signs Progressive Dyspnea (70%): LA dilation pulmonary congestion (reduced emptying) : worse with exercise, fever, tachycardia, and pregnancy Increased Transmitral Pressures: Leads to left atrial enlargement Arrhythmia (irregular heart beats) called atrial fibrillation. Atrial fibrillation is the most common arrhythmia in mitral stenosis and can cause serious complications such as systemic embolisms. Anticoagulant medication (Warfarin “Coumadin” : is still used prophylactically, it helps to prevent thrombus formation at the level of the dilated left atrium. Right heart failure symptoms: due to Pulmonary venous HTN Hemoptysis (Coughing Blood): due to rupture of bronchial vessels due to elevated pulmonary pressure Mortality: Due to progressive pulmonary congestion, infection, and thromboembolism 248
- 12. Physical Exam Findings of MS Presence of bilateral peripheral edema, especially in the ankle, with warm skin, slightly cyanotic; The present of hepatojugular reflux ( blood outpouring in the veins of the neck, secondary to liver stasis); prominent "a" wave in jugular venous pulsations (JVP): Due to pulmonary hypertension and right ventricular hypertrophy Signs of right-sided heart failure: in advanced disease Lung auscultation may reveal the present of hyperemia rales, at the level of lung bases (pulmonary edema); Mitral facies:(Malar flush) When MS is severe and the cardiac output is diminished, there is vasoconstriction, resulting in pinkish-purple patches on the cheeks Clinical Manifestations exertional dyspnea and fatigue (most common) orthopnea, paroxysmal nocturnal dyspnea, cough, hemoptysis cyanosis Right-sided heart failure – distended neck veins, peripheral edema, hepatomegaly, abdominal discomfort Auscultation: o Mid diastolic murmur (apex) 249
- 13. Evaluation of MS ECG: may show atrial fibrillation and LA enlargement CXR: LA enlargement and pulmonary congestion. Occasionally calcified MV ECHO: The GOLD STANDARD for diagnosis. Asses mitral valve mobility, gradient and mitral valve area Management of MS MS like AS is a mechanical problem and medical therapy does not prevent progression Medical Therapy is aimed at preventing the complications of systemic embolization and bacterial endocarditis as well as atrial fibrillation. Patients who have asymptomatic mitral stenosis require only antibiotic prophylaxis. IE prophylaxis: also with Patients with prosthetic valves or a Hx of IE for dental procedures. Patients with mild pulmonary congestion can be managed with diuretics alone. β - Blockers can be used to reduce heart rate and improve diastolic filling time. 250
- 14. When patients have atrial fibrillation, digoxin, β-blockers, or calcium channel blockers can be used for ventricular response rate control. Patients with atrial fibrillation require anticoagulation to prevent thrombus formation in the atrium. Once the patient has symptoms despite adequate medical management, mechanical correction of mitral stenosis by: Balloon valvuloplasty :. It is minimally invasive procedure; done by cardiac Catheterization. Surgery: by Commissurotomy which is an open-heart surgery that repairs a mitral valve that is narrowed from mitral valve stenosis. Mitral valve replacement – when stenosis is severe MS Surgical Treatment 251
- 15. Aortic Regurgitation Definition: o is the leaking of the aortic valve that causes blood to flow in the reverse direction during ventricular diastole, from the aorta into the left ventricle. Compensatory Mechanisms: o LV dilation, LVH. Progressive dilation leads to heart failure Causes o Rheumatic Fever – most common cause o Bicuspid aortic valve disease o Severe hypertension o Congenital anomaly 252
- 16. Symptoms & Signs of AR Asymptomatic until 4th or 5th decade Rate of Progression: 4-6% per year Progressive Symptoms include: o Dyspnea: Shortness of breath o Orthopnea : is shortness of breath which occurs when lying flat, causing the person to have to sleep propped up in bed or sitting in a chair o Paroxsymal Nocturnal Dyspnea (PND): refers to attacks of severe shortness of breath and coughing that generally occur at night. o Nocturnal angina: due to slowing of heart rate and reduction of diastolic blood pressure o Palpitations: due to increased force of contraction Physical Findings of AR Wide pulse pressure : most sensitive Auscultation: Diastolic blowing murmur at the left sternal border Austin flint murmur (apex) -mid-diastolic or presystolic murmur: Due to diastolic displacement of the anterior leaflet of the mitral valve by the aortic regurgitation stream causing it to vibrate. Systolic ejection murmur: due to increased flow across the aortic valve Florid pulmonary edema Pulmonary edema is accumulation of fluid in the interstitial spaces of the lungs (Interstitial Edema) due to an imbalance in the oncotic and hydrostatic pressure in the lungs. Florid pulmonary edema: the excess fluid is filled in the space between the capillary and lung interstitial spaces. 253
- 17. Pathophysiology of AR The Evaluation of AR CXR: enlarged cardiac silhouette and aortic root enlargement ECHO: Evaluation of the AV and aortic root with measurements of LV dimensions and function (cornerstone for decision making and follow up evaluation) Aortography: Used to confirm the severity of disease Management of AR General: IE prophylaxis in dental procedures with a prosthetic AV or history of endocarditis. Medical: Vasodilators (ACEI’s), Nifedipine improve stroke volume and reduce regurgitation only if pt symptomatic or HTN. Serial Echocardiograms: to monitor progression. Surgical Treatment: Definitive Tx Simplified Indications for Surgical Treatment of AR o ANY Symptoms at rest or exercise o Asymptomatic treatment if: EF drops below 50% or LV becomes dilated 254
- 18. Mitral Regurgitation Definition: Backflow of blood from the LV to the LA during systole Mild (physiological) MR is seen in 80% of normal individuals. MR Causes Infective Endocarditis Acute MI: papillary muscle rupture or rupture of a chorda tendinea secondary to MI Malfunction or disruption of prosthetic valve Acute rheumatic fever with carditis is the predominant cause. The Natural History of MR Compensatory phase: 10-15 years Patients with asymptomatic severe MR have a 5%/year mortality rate Once the patient’s EF becomes <60% and/or becomes symptomatic, mortality rises sharply Mortality: From progressive dyspnea and heart failure Clinical Manifestations of MR Fatigue & weakness – due to CO – predominant complaint exertional dyspnea & cough – pulmonary congestion palpitations – due to atrial fibrillation (occur in 75% of pts.) Right-sided heart failure – distended neck veins, edema, ascites, hepatomegaly Auscultation: holosystolic murmur at the apex radiating to the axilla 255
- 19. Pathophysiology of MR Imaging studies in MR ECG: May show, LA enlargement, atrial fibrillation and LV hypertrophy with severe MR CXR: LA enlargement, central pulmonary artery enlargement. ECHO: Estimation of LA, LV size and function. Valve structure assessment TEE (TransEsophageal Echocardiogram) if transthoracic echo is inconclusive. Management of MR The treatment of acute aortic regurgitation is surgery to repair or replace the valve. Medical therapy may be used to stabilize the patient en route to surgery; however, surgery should not be delayed in favor of efforts at medical management. Do not attempt to alleviate tachycardia with beta-blockers. Mild-to-moderate tachycardia is beneficial in these patients because it allows less time for the heart to have backfill, which lowers regurgitant volume. Medications o Vasodilator such as hydralazine o Rate control for atrial fibrillation with β-blockers, CCB, digoxin o Anticoagulation in atrial fibrillation and flutter 256
- 20. o Diuretics for fluid overload Serial Echocardiography: o Mild: 2-3 years, Moderate: 1-2 years, Severe: 6-12 months IE prophylaxis: Patients with prosthetic valves or a Hx of IE for dental procedures. MV Replacement in Severe MR Mitral Valve Prolapse When 1 or both of the valve leaflets bulge into the left atrium during ventricular contraction more common in women Cause: due to an inherited connective tissue disorder enlargement of one or both valve leaflets Elongates/stretches the chordae tendinae & papillary muscles regurgitation may occur usually asymptomatic Extra heart sound (Mitral click) – an early sign that a valve leaflet is ballooning into the left atrium fatigue, shortness of breath arrhythmias may develop – dizziness, chest pain, dyspnea, palpitations, syncope high-pitched late systolic murmur 257
- 21. Mitral Valve Prolapse Interventions: antibiotic prophylaxis to prevent endocarditis If w/ dysrhythmia – avoid caffeine, alcohol, stop smoking anti-arrhythmic drugs for chest pain – nitrates, calcium channel blockers, beta blockers surgery not indicated Tricuspid Stenosis usually occurs together w/ aortic or mitral stenosis may be due to rheumatic heart disease blood flow from right atrium to right ventricle right ventricular output left ventricular filling CO blood accumulates in systemic circulation systemic pressure S/Sx: symptoms of right-sided heart failure o hepatomegaly o peripheral edema o neck vein engorgement o CO – fatigue, hypotension Tricuspid Regurgitation Uncommon TR is most commonly secondary, caused by dilation of the right ventricle (RV) with malfunction of a normal valve, RV dysfunction–induced heart failure (HF), and pulmonary outflow tract obstruction. TR is less commonly primary, due to valvular abnormalities caused by infective endocarditis in users of illicit IV drugs, blunt chest trauma, rheumatic fever, congenital defects. An insufficient tricuspid valve allows blood to flow back into the right atrium venous congestion & right ventricular output blood flow towards the lungs 258
- 22. Clinical Manifestations of TR Symptoms of TR are often nonspecific, and severe TR may be well tolerated, producing few overt symptoms for a prolonged period. With isolated severe TR, Patients may complain of : o fatigue and decreased exercise tolerance as a result of low cardiac output. Elevated right atrial (RA) pressure also leads to peripheral edema and hepatic congestion with decreased appetite and abdominal fullness. o Long-standing severe TR results in right-heart failure: o Ascites (accumulation of fluid in the peritoneal cavity, causing abdominal swelling) o Anasarca (severe generalized, massive edema) o Decreased urine output o Active pulsing in the neck veins (Jugular venous distention) o The murmur of TR is frequently not heard. When evident, it is a holosystolic murmur 259
- 23. Pulmonary Stenosis rare, usually congenital in origin flow of blood to the pulmonary artery due to narrowing blood flows back to right ventricle and right atrium right ventricle hypertrophy to compensate for blood volume and force blood to the pulmonary artery Symptoms & Signs harsh systolic murmur fatigue, dyspnea on exertion, cyanosis poor weight gain or failure to thrive in infants hepatomegaly, ascites, edema Pulmonary Regurgitation a rare condition caused by infective endocarditis, tumors or RF blood flows back into Right ventricle Right ventricle and atrium hypertrphy symptoms of Right-sided heart failure Valve Repair Valvuloplasty Is repair of cardiac valve patient does not require continuous anti-coagulant medication usually require cardiopulmonary bypass machine 1. Commissurotomy – to separate the fused leaflets Balloon Valvuloplasty performed in the cardiac cath. lab. balloon inflated for 10-30 secs., w/ multiple inflations common used for mitral and aortic stenosis 260
- 24. Closed surgical valvuloplasty done in the OR under GA Midsternal incision, a small hole is cut into the heart, the surgeon’s finger or a dilator is used to open the commissure Open Commissurotomy done w/ direct visualization of the valve, thrombus and calcifications may be identified and removed 2. Annuloplasty Is repair of valve annulus (junction of the valve leaflets and the muscular heart wall) narrows the diameter of the valve’s orifice, useful for valvular regurgitation 3. Chordoplasty Is repair of chordae tendineae , done for mitral valve regurgitation caused by stretched, torn or shortened chordae tendineae Valve Replacement Mechanical valves Example: Caged ball valve, Tilting-disk valve more durable, used for younger pts. risk of thromboembolism – long-term use of anti-coagulants Tissue or biological valves: xenografts – porcine or bovine heterografts (7-10 yrs viability) homografts – from cadaver tissue donations (10-15 yrs) autografts – excising the pts.’s own pulmonic valve and portion of pulmonary artery for use as the aortic valve Long-term anticoagulant therapy Antibiotic prophylaxis --------------------------- 261
