Presentation1.pptx imaging of the peritoneum and mesentry.
- 1. Imaging of the peritoneum and mesenteric lesions. Dr/ ABD ALLAH NAZEER. MD.
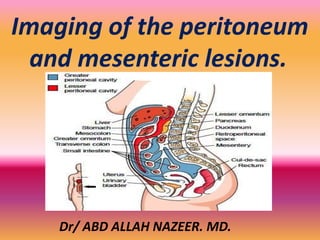
- 2. The peritoneum is a thin, translucent, serous membrane and is the largest and most complexly arranged serous membrane in the body. The peritoneum that lines the abdominal wall is called the parietal peritoneum, whereas the peritoneum that covers a viscus or an organ is called a visceral peritoneum. The peritoneal cavity is a potential space between the parietal peritoneum, which lines the abdominal wall, and the visceral peritoneum, which envelopes the abdominal organs. In men, the peritoneal cavity is closed, but in women, it communicates with the extraperitoneal pelvis exteriorly through the fallopian tubes, uterus, and vagina. Peritoneal ligaments, mesentery, and omentum divide the peritoneum into two compartments: the main region, called the greater sac, and a diverticulum, omental bursa, or lesser sac . Peritoneal ligaments are double layers or folds of peritoneum that support a structure within the peritoneal cavity; omentum and mesentery are specifically named peritoneal ligaments. Most abdominal ligaments arise from the ventral or dorsal mesentery. Anatomic definitions.
- 4. Mesenteries The visceral peritoneum lines all the organs that are intraperitoneal. The parietal peritoneum lines the anterior, lateral and posterior walls of the peritoneal cavity. The deepest portion of the peritoneal cavity is the pouch of Douglas in women and the retrovesical space in men, both in the upright and supine position. The mesentery is a double fold of the peritoneum. True mesenteries all connect to the posterior peritoneal wall. These are: The small bowel mesentery The transverse mesocolon The sigmoid mesentery (or mesosigmoid) Specialized mesenteries do not connect to the posterior peritoneal wall. These are: The greater omentum: connects the stomach to the colon The lesser omentum: connects the stomach to the liver The mesoappendix: connects the appendix to the ileum
- 6. Omentum: The omentum is divided into the greater and lesser omentum. The greater omentum is subdivided into: Gastrocolic ligament (yellow arrow): the largest component Gastrosplenic ligament: up to the hilus of the spleen Gastrophrenic ligament: not shown on this illustration The lesser omentum is subdivided into: Gastrohepatic ligament: connects the left lobe of the liver to the lesser curvature of the stomach. Hepatoduodenal ligament (blue arrow): free edge of the omentum, which contains the portal vein, hepatic artery and common bile duct .
- 11. Peritoneal circulation: These compartments enable the peritoneal cavity to have a normal circulation for peritoneal fluid. In the normal abdomen without intraperitoneal disease, there is a small amount of peritoneal fluid that continuously circulates. The movement of fluid in this circulatory pathway is produced by the movement of the diaphram and peristalsis of bowel. It predominantly flows up the right paracolic gutter which is deeper and wider than the left and is partially cleared by the subphrenic lymphatics. There are watershed regions in the peritoneal cavity that are areas of fluid stasis: Ileocolic region Root of the sigmoid mesentery Pouch of Douglas When you are staging a patient for gastrointestinal malignancy you have to look for disease in these areas of stasis. Clearly the surgeons do better in finding subtle disease in these areas.
- 13. Peritoneal anatomy after intra-abdominal contrast injection.
- 14. Imaging Modalities. US: may depict peritoneal collections or ascites and is used to guide drainage of ascites and large superficial fluid collections CT : is the most common imaging modality used to detect diseases of the peritoneum to fully delineate peritoneal anatomy and the extent of disease, we prefer to perform isotropic imaging with coronal and sagittal reformations.
- 15. Magnetic resonance (MRI). Disadvantages of MR imaging include: 1- motion artifacts caused by respiration and peristalsis 2- chemical shift artifacts at the bowel- mesentery interface. 3-the spatial resolution of MR imaging is lower than that of CT, a characteristic that may make it difficult to assess small peritoneal lesions. 4-Patients who are ill may not tolerate prolonged MR imaging examinations.
- 17. Pathology OF Peritoneum and Mesentery. Cystic Masses Mucinous Carcinomatosis Pseudomyxoma peritonei Mesenteric cyst - Lymphangioma Enteric Duplication Cyst Nonpancreatic Pseudocyst Enteric cyst and mesothelial cyst Peritoneal Inclusion Cyst Tuberculosis Echinococcal Cyst Cystic teratoma
- 18. Solid Masses Peritoneal metastases Lymphoma Carcinoid Gastrointestinal Stromal Tumor - GIST Inflammatory Pseudotumor Mesenteric fibromatosis - Desmoid Sclerosing Mesenteritis Malignant mesothelioma Primary Peritoneal Serous Carcinoma Desmoplastic Small Round Cell Tumor Retro-peritoneal liposarcoma.
- 21. Mucinous Carcinomatosis. Mucinous carcinomatosis is the most common cystic tumor to affect the peritoneal cavity. Usually these metastases arise from mucinous carcinomas of the ovary or of the gastrointestinal tract (stomach, colon, pancreas). The prognosis is poor. However, when low-grade mucinous adenocarcinoma of the appendix spreads to the peritoneal cavity, the consequence is typically pseudomyxoma peritonei, which is a distinct tumor with a better prognosis. In peritoneal carcinomatosis we see tumor nodules along the peritoneal lining (arrow), omental tumor deposits, and bowel obstruction.
- 22. Mucinous Carcinomatosis with a tumor nodule along the right paracolic gutter.
- 23. Peritoneal mucinous carcinomatosis that caused small bowel obstruction in a 40-year-old man who complained of progressive abdominal pain, nausea, and vomiting. Intravenous and oral contrast-enhanced CT scans show low-attenuation mucinous ascites that infiltrates between the folds of the small bowel mesentery. There are low-attenuation mucinous metastatic deposits in the greater omentum (arrows in a) and soft-tissue attenuation deposits along the peritoneal surfaces and in the paracolic gutters (arrows in b).
- 24. Pseudomyxoma peritonei. Pseudomyxoma peritonei is the result of a mucinous adenocarcinoma of the appendix, which presents as a mucocele and spreads to the peritoneal cavity. It is a clinical syndrome, characterized by recurrent and recalcitrant voluminous mucinous ascites due to surface growth on the peritoneum without significant invasion of underlying tissues. A typical feature of pseudomyxoma peritonei is scalloped indentation of the surface of the liver and spleen. Unlike peritoneal metastases, there are no tumor nodules. There may be some calcifications.
- 25. Pseudomyxoma peritonei in a 70-year-old woman who complained of increasing abdominal girth. Longitudinal (a) and transverse (b) sonograms of the abdomen show complex, hypoechoic ascites that contains nonmobile echoes and centrally displaced small bowel that has a starburst appearance.
- 27. Pseudomyxoma peritonei with pronounced scalloping of the liver and almost destruction of the spleen. Notice the calcifications.
- 28. Pseudomyxoma peritonei with thickened mesentery (arrow).
- 29. Mesenteric cyst – Lymphangioma. Mesenteric cyst is a descriptive term for any cystic lesion within the mesentery. Usually it is a lymphangioma. Other mesenteric cysts like enteric duplication cyst, enteric cyst, nonpancreatic pseudocyst and mesothelial cyst are very uncommon and have no specific features. Lymphangioma is a benign lesion of vascular origin. Most lymphangiomas are located in the neck, but 5% of lymphangiomas are abdominal. Lymphangioma has enhancing septa. Unlike in cystic peritoneal metastases, ascites is not a feature of lymphangioma. When you see a septated cystic lesion without ascites the most likely diagnosis is a lymphangioma.
- 30. (Lymphangioma).
- 32. (Lymphangioma).
- 33. Enteric Duplication Cyst. Enteric duplication cyst is a cyst with a wall that has all three layers of the bowel wall, i.e. mucosa, submucosa and muscularis propria. Although we commonly think of duplication cysts when we see a cystic mass adjacent to the bowel, we have to realize, that these are rare lesions. They may occur anywhere in the mesentery, so either adjacent to or away from the bowel. On the left an enteric duplication cyst. It is located in the transverse mesocolon. This patient was suspected of having a cystic pancreatic tumor. The specimen demonstrates all the bowel wall layers
- 36. Nonpancreatic Pseudocyst. Nonpancreatic pseudocyst is a residual of an old hematoma or infection. Most of these patients have a history of prior abdominal trauma. Often there is a thickened wall and there can be some debris within the lesion.
- 37. On the left a specimen and CT image of a nonpancreatic pseudocyst. Notice the thick wall. Probably this is an old hematoma or abscess.
- 38. Enteric cyst and mesothelial cyst.
- 41. Tuberculosis. T.B can produce very thick ascites, that can be loculated in distribution. Because of this, it can simulate a cystic lesion. Usually there is accompanying abnormality of the terminal ileum and lymphadenopathy. The lymph nodes most often are of low attenuation (caseated). So these are the things to look for.
- 42. TB the peritoneum is usually very thick (arrow).
- 47. Solid Masses. Peritoneal metastases Peritoneal metastases are the most common peritoneal solid masses. Gastrointestinal and ovarian cancers are the most common etiologies. Usually there are omental metastases, i.e. omental cake and ascites. On the left a CT demonstrating omental cake in a patient with ovarian cancer.
- 51. Lymphoma. NHL is the most common cause of lymphadenopathy. Usually there are other sites with lymphoma. The CT attenuation at diagnosis is very homogeneous in most cases with minimal to no enhancement. Heterogeneous attenuation is seen only in cases with aggressive histology. During treatment the attenuation becomes heterogeneous as a result of necrosis and fibrosis. Calcification may occur
- 52. NHL located in the small bowel mesentery.
- 54. Lymphomatosis. Intravenous and oral contrast-enhanced CT scan shows soft tissue diffusely infiltrating through the peritoneum, encasing the small bowel, and lining the folds of the small bowel mesentery. Ascites and diffuse peritoneal thickening are present.
- 55. Carcinoid. Carcinoid is a slow-growing neuroendocrine tumour most commonly found in the small bowel. Less than 10% of patients with carcinoid will develop the carcinoid syndrome, caused by the overproduction of serotonin, which can lead to symptoms of cutaneous flushing, diarrhea and bronchoconstriction. Carcinoid metastasizes to the mesentery, which at times is easier to appreciate than the primary tumor in the small bowel. There is associated bowel wall thickening due to a desmoplastic reaction.
- 56. Carcinoid with central calcification (blue arrow). Positive octreoscan in a patient with carcinoid and liver metastases (blue arrows)
- 58. Gastrointestinal Stromal Tumor - GIST Primary small bowel tumors can extend into the mesentery and the typical example of that is the GIST. You can have a large mesenteric component and such a small attachment to the bowel, that you may not appreciate it. On CT they are of mixed density due to necrosis and hemorrhage and they tend to be well vascularized, so they will enhance like the case on the left.
- 59. Gastrointestinal Stromal Tumor - GIST
- 61. Mesenteric fibromatosis – Desmoid. Mesenteric fibromatosis is also known as intra- abdominal fibromatosis, abdominal desmoid or desmoid tumor. On the left a 33-year-old man who complains of an increasing abdominal girth, abdominal fullness, and a palpable abdominal mass. First study the images on the left and continue with the MR. Look for some imaging features that are helpful in the differential diagnosis.
- 63. Mesenteric fibromatosis – Desmoid low density tumor located in the greater omentum (upper image) and the gastrosplenic ligament (lower image).
- 64. Sclerosing Mesenteritis (panniculitis). This disease has multiple synonyms reflecting the wide histological spectrum: mesenteric panniculitis, fibrosing mesenteritis and mesenteric lipodystrophy. Pathologically it is a chronic inflammation of unknown etiology. This entity is more common than previously thought. The signs and symptoms are variable. Patients present with pain, a palpable mass or bowel complications, but in many cases it is an incidental finding on CT made for other reasons.
- 76. Primary Peritoneal Serous Carcinoma. This tumor is also one of the primary peritoneal malignancies. It occurs exclusively in women. This tumor is histologically identical to malignant ovarian surface epithelial tumors. It was once thought to be very rare, but now almost one third of tumors previously diagnosed as ovarian cancer are diagnosed as primary peritoneal serous carcinoma. Consider this diagnosis when: Ovaries are normal or involvement of extraovarian sites is greater than that of the ovarian surface or if ovaries are involved, yet disease is confined to the surface epithelium As a radiologist you should consider this diagnosis if you think of metastatic ovarian cancer but the ovaries are normal.
- 77. Primary peritoneal serous carcinoma.
- 79. Desmoplastic Small Round Cell Tumor. This tumor is also one of the primary peritoneal malignancies. It is a rare malignancy of uncertain origin. It occurs primarily in young men with a mean age of 19 years. Consider this diagnosis if you see something that looks like peritoneal carcinomatosis in a young man that has no history of a primary malignancy. It is a very aggressive tumor with a poor prognosis.
- 80. Desmoplastic Small Round Cell Tumor.
- 82. Miscellaneous lesions of the peritoneum. Peritoneal fluid: Ascites.
- 83. Ascites at CT and MRI images.
- 84. Shock bowel with hemoperitoneum.
- 85. Pneumoperitoneum at X-Ray chest.
- 86. Pneumoperitoneum at CT Scan.
- 87. Pneumoperitoneum of the abdomen.
- 88. Peritonitis with fluid collection and abscess at the pelvis.
- 89. Abscess from perforated diverticulitis.
- 90. Hydatid disease of the peritoneum. Almostly secondary to hepatic disease. The hydatid may be single or multiple.
- 91. Hydatid cyst at the pelvic peritoneum.
- 92. Torsion of the greater omentum with omental infarction.
- 94. CT images of missed towel within the peritoneum.
