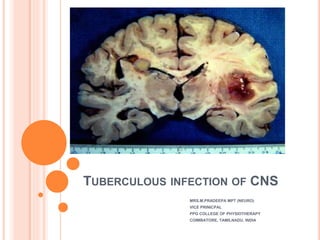
Tuberculous infection of CNS
- 1. TUBERCULOUS INFECTION OF CNS MRS.M.PRADEEPA MPT (NEURO) VICE PRINICPAL PPG COLLEGE OF PHYSIOTHERAPY COIMBATORE, TAMILNADU, INDIA
- 2. INTRODUCTION Tuberculosis of the central nervous system (CNS) is a highly devastating form of tuberculosis Tuberculosis is an infection caused by one of two Mycobacteria – Mycobacterium tuberculosis and Mycobacterium bovis. The disease involves the nervous system in 10% of patients. Can result from either haematogenous spread from distant systemic infection (e.g. pulmonary tuberculosis) or direct extension from local infection (e.g. tuberculous otomastoiditis).
- 3. EPIDEMIOLOGY Tuberculosis remains a leading cause of morbidity and mortality in the developing world. It may account for 1/6th of the 3 million of global mortality. CNS involvement is thought to occur in 2-5% of patients with tuberculosis and up to 15% of those with AIDS- related tuberculosis 6,7. Although CNS involvement by tuberculosis is seen in all age groups, there is a predilection for younger patients, with 60-70% of cases occurring in patients younger than 20 years of age. In endemic regions, tuberculomas account for as many as 50% of all intracranial masses Male predominance
- 4. RISK FACTORS Children HIV-infected patients Malnutrition Recent measles in children Alcoholism Malignancies Use of immunosuppressive agents in adults
- 5. CLASSIFICATION Extra-axial Tuberculous meningitis (leptomeningitis): most common Tuberculous pachymeningitis: rare Intra-axial Intracranial tuberculous granuloma (tuberculoma) Focal tuberculous cerebritis Intracranial tuberculous abscess Tuberculous rhombencephalitis Tuberculous encephalopathy
- 6. PATHOGENESIS OF TUBERCULOSIS The acquisition of M. tuberculosis infection occurs through the inhalation of droplet nuclei containing the bacilli, eventually leading to deposition in the lung alveoli. In the alveoli, the bacilli interact with alveolar macrophages through a multitude of different receptors. Numerous cytokines and chemokines are released, the activation of a type 1 T-helper cell-mediated immune response occurs, and, ultimately, a granuloma is formed. Prior to the actual containment of the infection, bacilli are filtered into draining lymph nodes, and there exists a low-level bacteremia in which M. tuberculosis disseminates to distant sites in the body (haematogenous seeding) In case of CNS involvement the characteristic lesions known as Rich’s foci tuberculous subpial or subependymal foci about 1 mm in diameter are formed
- 7. PATHOGENESIS CNS TB is a three step process 1. Hematogenous seeding of meninges during bacteremia of primary TB 2. Quiescent phase: may last from few weeks to many years. 3. Mycobacteria in Richs foci multiply and with immune or traumatic stimulus rupture or grow and clinical manifestations occur.
- 8. PATHOGENESIS For CNS tuberculosis, the disease begins with the development of small tuberculous foci (Rich foci) in the brain, spinal cord, or meninges. The location of these foci and the capacity to control them ultimately determine which form of CNS tuberculosis occurs. CNS tuberculosis manifests itself primarily as tuberculous meningitis (TBM) and less commonly as tubercular encephalitis, intracranial tuberculoma, or a tuberculous brain abscess
- 10. TUBERCULOUS MENINGITIS This is the commonest manifestation of tuberculous infection of the nervous system. In children, it usually results from bacteraemia following the initial phase of primary pulmonary tuberculosis. In adults, it may occur many years after the primary infection. Tuberculous meningitis may manifest in two forms: 1. Leptomeningitis: common 2. Pachymeningitis: rare
- 11. EPIDEMIOLOGY Tuberculous meningitis, although seen in all age groups, has a peak incidence in childhood (particularly 0-4 years of age) in high prevalence areas. In low prevalence areas, it is more frequently encountered in adolescents and adults.
- 12. LEPTOMENINGITIS Common and presents with thick tuberculous exudate within the subarachnoid space, particularly pronounced at the base of the brain especially in the interpeduncular fossa, anterior to the pons and around the cerebellum and may also extend into the Sylvian fissures. In contrast to bacterial meningitis, extension over the surfaces of the cerebral hemispheres is relatively uncommon. Eventually, mass-like regions of caseous necrosis can form within this exudate, representing extra-axial tuberculomas. CSF flow is disrupted, and obstructive hydrocephalus is common. An additional complication is arteritis that may result in ischemic infarcts, which are seen in approximately a third of cases, especially in children
- 13. PATCHYMENINGITIS Tuberculous pachymeningitis is a rare form of CNS tuberculosis characterized by a chronic tuberculous infection leading to a dura mater involvement. Common sites of involvement are cavernous sinuses, floor of middle cranial fossa and tentorium. Characterized by thick plaque-like regions of pachymeningeal enhancement. This term should be reserved for cases where it is an isolated abnormality, and not confused with the sometimes dramatic thickening of dura adjacent to a tuberculoma.
- 15. CLINICAL FEATURES OF TB MENINGITIS The clinical features of tuberculous meningitis (TBM) result from: Infection. Exudation – which may obstruct the basal cisterns and result in hydrocephalus. Vasculitis – secondary to inflammation around vessels, resulting in infarction of brain and spinal cord. The basal meninges are generally most severely affected.
- 16. The majority of patients are adults; childhood TBM is now rare. Non-specific prodromal symptoms develop over 2– 8 weeks. Staging is useful for predicting outcome. Stage I Early Stage II intermediate Stage III advanced Fever (in 80%) Confusion Coma Lethargy Cranial nerve paresis Meningism Vasculitis - hemi/quadriparesis, ataxia, dysarthria
- 17. Seizures may occur at the onset. Involuntary movements (chorea, myoclonus) occur in 10%. Atypically the illness may develop slowly over months presenting with dementia or rapidly like pyogenic (bacterial) meningitis. Occasionally cerebral features prevail rather than signs of meningitis. Untreated, the illness may progress from phase 1 to death over a 3-week period. Arachnoiditis inflammatory exudate may result in hydrocephalus/dementia/blindness
- 18. INVESTIGATION OF TB MENINGITIS General: Anaemia, leucocytosis. Hyponatraemia (if inappropriate ADH secretion occurs). Cerebrospinal fluid Cell count, differential count, cytology (50–4000/mm3 – predominantly lymphocytes) Glucose, with a simultaneous blood sugar (<50% blood glucose) Protein (>1g/l) Acid-fast stain, Gram stain, appropriate bacteriologic culture and sensitivity, India ink (all causes of lymphocytic meningitis) Cryptococcal antigen, herpes antigen (other causes of lymphocytic meningitis) Culture for M. tuberculosis (50–80% positive) Polymerase chain reaction (PCR) to detect Mycobacterium DNA – specificity and sensitivity 100% and 70%.
- 19. Tuberculin skin test: Positive in 50% of cases. (Negative if recent steroids or acquired primary infection.) Chest x-ray: Hilar lymphadenopathy, infiltrate, cavitations, effusion, scar. CT scan and MRI Hydrocephalus, basal meningeal thickening, infarcts, oedema, tuberculomas and obliteration of the subarachnoid space.
- 21. DIFFERENTIAL DIAGNOSIS Viral meningoencephalitis Subacute/chronic meningitis
- 22. MANAGEMENT Normal regime: 2 months 1. Isoniazid (300 mg daily) 2. Rifampicin (600 mg daily) 3. Pyrazinamide (15–30 mg/kg daily) Then for 6 months 1. Isoniazid and Rifampicin Drug resistance suspected due to previous antituberculous therapy - Add a fourth drug – streptomycin (1 g daily) or ethambutal (25 mg/kg daily).
- 23. Intrathecal therapy: Streptomycin 50 mg may be given daily or more frequently in seriously ill patients. When obstructive hydrocephalus occurs, combined intraventricular (through the shunt reservoir or drainage catheter) and lumbar intrathecal treatment injections may be administered. Steroid therapy: Adjunctive steroids reduce neurological sequelae, hearing loss and mortality in patients with TBM without HIV.
- 24. TUBERCULOMA Intracranial tuberculous granulomas, also known as CNS tuberculomas, are common in endemic areas and may occur either in isolation or along with tuberculous meningitis Tuberculomata may occur in cerebral hemispheres, cerebellum or brain stem with or without tuberculous meningitis, and may produce a space- occupying effect. Lesions may be single or multiple.
- 25. PATHOGENESIS OF TUBERCULOMAS A tuberculoma is distinct from a tuberculous abscess in that it demonstrates evidence of granulomatous reaction and caseous necrosis histologically. Tuberculomas have a solid granulomatous core made up of epitheloid cells and macrophages containing mycobacteria and some may undergo liquefaction.
- 26. CLINICAL FEATURES The clinical presentation of CNS tuberculoma is usually more subtle than that of TB meningitis. Tuberculomas accompany TB meningitis in 10% of patients Lesions may occur in the brain, spinal cord, subarachnoid, subdural, or epidural space Include headache, seizures, focal neurologic deficits, and papilledema
- 27. INVESTIGATION OF TUBERCULOMAS TB organisms may not necessarily be identified in tuberculomas, whereas they are necessary to make the diagnosis of tuberculous abscess. CT Tuberculomas may appear as a round or lobulated nodule with moderate to marked edema. MRI Isointense to grey matter, usually appears as ring- enhancement
- 29. DIFFERENTIAL DIAGNOSIS Other infection Neurocysticercosis Cerebral toxoplasmosis CNS cryptococcosis Bacterial cerebral abscesses Neurosarcoidosis Cerebral metastases CNS lymphoma
- 30. TREATMENT AND PROGNOSIS Most resolve over a few weeks with antituberculous therapy.
- 31. POTT’S DISEASE This was first described by Percivall Pott. He noted this as a painful kyphotic deformity of the spine associated with paraplegia. Tuberculous spondylitis, also known as Pott disease, refers to vertebral body osteomyelitis and intervertebral diskitis from tuberculosis (TB). The spine is the most frequent location of musculoskeletal tuberculosis, and commonly related symptoms are back pain and lower limb weakness/paraplegia. This arises in the lower thoracic region, can extend over several segments and may spread through the intervertebral foramen into pleura, peritoneum or psoas muscle (psoas abscess). Chronic epidural infection follows tuberculous osteomyelitis of the vertebral bodies.
- 32. EPIDEMIOLOGY In developing countries, spinal TB is mostly a disease of childhood or adolescence. 1/5th of TB population is in India. 3% are suffering from skeletal TB, 50% of these suffer from spinal lesion and almost 50% are from pediatric group. An estimated 2 million or more patients have active spinal tuberculosis. The incidence is now increasing, probably due to the development of antibiotic resistance
- 34. PATHOLOGY The spine is involved due to hematogenous spread via the venous plexus of Batson. There is usually a slow collapse of one or usually more vertebral bodies, which spreads underneath the longitudinal ligaments. This results in an acute kyphotic or "gibbus" deformity. This angulation, coupled with epidural granulation tissue and bony fragments, can lead to cord compression. Unlike pyogenic infections, the discs can be preserved and it more commonly involves the thoracic spine. In late-stage spinal TB, large paraspinal abscesses without severe pain or frank pus are common, leading to the expression "cold abscess".
- 35. TYPES OF POTT’S DISEASE Paradiscal: This is the commonest type. In this, the contagious areas two adjacent vertebrae along with the intervening disc are affected. Central: Body of single vertebrae affected leading to early collapse of the weakened vertebrae. The nearby disc maybe normal. The collapse may be a ‘wedging’ or ‘concertina’ collapse. Anterior: Infection is localised to anterior part of vertebral body. Infection spreads up and down under the anterior longitudinal ligament. Posterior: Posterior complex vertebrae i.e., the pedicle, lamina, spinous process and transverse process is affected.
- 37. CLINICAL FEATURES The classic systemic features of weight loss, night fever and cachexia are often absent. Pain occurs over the affected area and is made worse by weight bearing. Symptoms and signs of cord compression occur in approximately 20% of cases. The onset may be gradual as pus, caseous material or granulation tissue accumulate, or sudden as vertebral bodies collapse and a kyphosis develops.
- 38. STAGES ACCORDING TO CLINICAL PRESENTATION ACTIVE STAGE: BACK PAIN 1. Diffuse “radicular pain”, commonest presenting complaint. 2. Presents in the arm (cervical root), girdle (dorsal root), abdomen (dorso-lumbar root), groin (lumbar root), sciatic (lumbo-sacral root) STIFFNESS 1. Very early symptom. 2. Protective mechanism of the body. COLD ABSCESS 1. Patient may present with a swelling ‘cold abscess’ or problems secondary to its compression effects on nearby vicera. PARAPLEGIA (IF NEGLECTED IN EARLY STAGES) DEFORMITY CONSTITUIONAL SYMPTOMS Fever, Weight loss, Night sweats
- 39. HEALED STAGE: No systemic features but deformity persists. Radiological evidence of bone healing Patient may present with cold abscess or due to its compression effects 1. Retropharyngeal abscess — Dysphagia ,dyspnea, hoarseness of voice 2. Mediastinal abscess—Dysphagia 3. Psoas abscess— Flexion deformity of hip
- 40. NEUROLOGICAL COMPLICATIONS – POTT’S PARAPLEGIA
- 41. INVESTIGATION Straight x – ray 1. Reduced disc space, Blurred paradiscal margins, Destruction of bodies, Loss of trabecular pattern, Increased prevertebral soft tissue shadow, Subluxation /dislocation, Decreased lordosis or Kyphosis CT / MRI 1. T1: hypointense marrow in adjacent vertebrae 2. T2: hyperintense marrow, disc, soft tissue infection 3. T1 C+ (Gd): marrow, subligamentous, discal, dural enhancement 4. The paraspinal collections are typically well circumscribed, with fluid centers and well-defined enhancing margins.
- 43. DIFFERENTIAL DIAGNOSIS Brucellosis Fungal infection Sarcoidosis Pyogenic infection/spondylitis Metastasis
- 44. MANAGEMENT A needle biopsy is often sufficient Long-term anti-tuberculous therapy is commenced. If signs of cord compression develop, decompression is necessary. Anterior Transthoracic Decompression with strut graft fusion is sometimes performed. This permits clearance of pus and caseous debris without retracting the spinal cord. Posterolateral approach (costotransversectomy): One or more ribs are resected medially, along with the transverse processes.
- 45. TUBERCULOUS MENINGOMYELITIS Tuberculous meningomyelitis is a relatively rare but serious type of nervous system tuberculosis. This disorder is now more frequent in AIDS patients. This disease is caused by invasion of the spinal cord or the spinal meninges which may result from downward spread of intracranial infection or direct spread from epidural infection. Occasionally arises from rupture of local metastatic focus; resultant infection is confined to the spinal level. Tuberculosis Infection of the leptomeninges results in an exudate that encases the spinal cord and nerve roots.
- 46. CLINICAL FEATURES It can be Ascending myelitis, Root involvement, Descending myelitis Results in Back pain Root pain, paraesthesia Weakness mainly lower limb Pyramidal and segmental. Sensory loss. Sphincter disturbance
- 47. INVESTIGATION Imaging may be normal while CSF shows high protein, lymphocytes and rarely acid fast bacilli.
- 48. DIFFERENTIAL DIAGNOSIS Cytomegalovirus Cryptococcus Syphilis Lymphoma. .
- 49. MANAGEMENT Laminectomy and meningeal biopsy may be required to establish diagnosis. Antituberculous drugs - Rifampicin 0.45 g/d + ethambutol 0.75 g/d + pyrazi- namide 1.5 g/d + isoniazid 0.6 g/d. Surgically treated with abscess debridement and spinal stabilization
- 50. THANK YOU