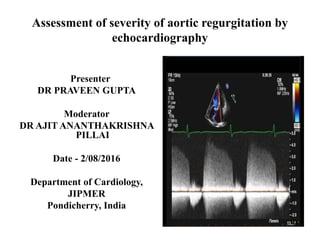
Echocardiography assessment of Aortic Regurgitation severity
- 1. Assessment of severity of aortic regurgitation by echocardiography Presenter DR PRAVEEN GUPTA Moderator DR AJIT ANANTHAKRISHNA PILLAI Date - 2/08/2016 Department of Cardiology, JIPMER Pondicherry, India
- 2. Introduction Aortic Regurgitation (AR) is diastolic reflux of blood from the aorta to the LV Caused by Malfunction of the aortic valve leaflets Dilation of the aortic root and annulus Combination of these factors Aortic root disease >50% of all Aortic valve replacement (AVRs)
- 3. Evaluating the Severity of Aortic Regurgitation Effective regurgitant orifice area Volume or fraction of regurgitant flow Size or extent of the regurgitant jet within the LV
- 4. Evaluating the Severity of Aortic Regurgitation By Colour flow imaging Record jet in multiple imaging planes to provide a three- dimensional assessment of its dimensions Area of the jet,estimated by planimetry. Parasternal long-axis view, the height of the jet just below the valve measured This dimension can also be expressed as a percentage of left ventricular outflow tract dimension to provide an estimate of severity Three examples of aortic regurgitation are provided, all taken from the parasternal long- axis view using color Doppler. Mild (A), moderate (B), and severe (C) aortic regurgitation are illustrated.
- 5. Evaluating the Severity of Aortic Regurgitation by colour flow imaging The greater the percentage is of the left ventricular outflow tract that is filled by the jet at its origin, the more severe the regurgitation. A jet that occupies > 60% of the LVOT (either height or area) indicates severe AR. A similar approach uses the short-axis view with the imaging plane positioned immediately proximal to the aortic valve . The outflow tract is directly visualized as a circular space, and the regurgitant jet is visualized as a two-dimensional shape within this circle
- 6. Using transesophageal echocardiography, the jet can be visualized from the short-axis view, just below the aortic valve. A: The regurgitant orifice is visualized with two-dimensional imaging. B: Color Doppler is used to demonstrate flow within the regurgitant orifice. C: The regurgitant orifice area is measured by planimetry (0.75 cm2).
- 7. Evaluating the Severity of Aortic Regurgitation By Colour flow imaging A:The schematic demonstrates how the dimensions of the color jet of aortic regurgitation can be used to estimate severity. B: The jet height just below the aortic valve (arrows) can be measured and compared with the dimension of the left ventricular outflow tract. This is a useful measure of severity
- 8. Evaluating the Severity of Aortic Regurgitation By colour flow imaging Both length of the jet and area of jet method conveys unreliable information about overall severity. The best dimensional predictors of angiographic severity are, jet area indexed to the LV short-axis area (parasternal short-axis view) and jet diameter indexed to LVOT diameter immediately proximal to the valve (paraternal long axis view)
- 9. Limitations to the use of color flow mapping Eccentric jets tends to alter the perception of severity Size of the jet is instrument dependent. Changes in gain, color scale, transducer frequency, and wall filters affect the jet appearance Jet is greater from an apical view compared with a parasternal view Regurgitant orifice area in chronic aortic regurgitation changes (and usually decreases) during diastole, and it lead to color Doppler to overestimate severity because the visualized jet area would reflect peak rather than mean orifice area
- 10. Vena Contracta • Narrowest portion of a jet that occurs at or just downstream from the orifice • Measure of the effective regurgitant orifice area (EROA) • Independent of flow rate and driving pressure • Small errors in measurement lead to a large percent error and misclassification of the severity of regurgitation
- 11. Vena Contracta Vena contracta width of ≥ 6 mm correlates well with severe AR (sensitivity 95%, specificity 90%) Vena contracta width of < 3 mm specific for mild AR. Enriquez-Sarano M, et al. NEJM 2004; 351: 1539-1546 .
- 12. Proximal Isovelocity Surface Area (PISA) by colour flow Acceleration of flow occurs proximal to the valve plane with a series of isovelocity “surfaces” leading to the high-velocity jet in the regurgitant orifice. Velocity for a PISA =aliasing velocity where a distinct red-blue interface seen (at this interface, velocity is equivalent to Nyquist limit). Surface area of the PISA region is 2πr2
- 13. Proximal Isovelocity Surface Area Peak regurgitant flow obtained by multiplying surface area by aliasing velocity Effective regurgitant orifice area (EROA) is peak regurgitant flow divided by peak velocity obtained by CW Doppler.
- 14. PISA Limitations Isovelocity contour flattens as it approaches the orifice, underestimating flow Proximal structures can distort the isovelocity contour Sensitive to errors in radius measurement 10% error in radius leads to 21% error in flow Multiple measurements Technically challenging
- 15. Evaluating the Severity of Aortic Regurgitation by Continuous Doppler The simplest approach compares the density or darkness of the envelope of the antegrade aortic flow and the regurgitant jet. Mild aortic regurgitation the velocity of the regurgitant jet remains relatively high and the envelope appears flat. With more severe aortic regurgitation, steeper slope of the Doppler envelope. The deceleration of jet velocity can be described as either the slope or the pressure half-time of the jet Factors, including aortic compliance, blood pressure, and left ventricular size and compliance affect these measures
- 16. Evaluating the Severity of Aortic Regurgitation by Continuous Wave Doppler This schematic illustrates how hemodynamic changes are reflected in the Doppler velocity tracing. Left: Mild aortic regurgitation (AR) is associated with a fairly flat contour of the regurgitant jet. Right: As severity increases, the slope of the jet becomes steeper. These changes are the result of the instantaneous pressure gradient between the aorta and left ventricle during diastole
- 17. Pressure Half-Time Rate at which aortic and LV pressures equalize Most relaible in the setting of acute regurgitation Rapid rate of decline in aortic pressure is reflected in steeper diastolic deceleration slope A pressure half-time less than 250 milliseconds or a slope greater than 400 cm/sec2 are indicators of severe aortic regurgitation
- 18. Evaluating the Severity of Aortic Regurgitation Pressure Half-Time Continuous wave Doppler imaging of the aortic regurgitation (AR) jet permits quantitation of both slope and pressure half-time (P½t). Top: An example of mild aortic regurgitation is demonstrated. The slope is relatively flat and the P½t is long. Bottom: An example of severe aortic regurgitation demonstrates a much steeper slope and shorter P½t.
- 19. Pressure Half-Time For a given severity of AR, P1/2 will be shortened by elevated LVEDP or vasodilator therapy that reduces AR With acute AR-triangular-shaped CW-Doppler with linear deceleration slope from maximum velocity to baseline
- 21. Limitations of pressure half-time assessment Pressure half-time sensitive to chronicity of AR Acute AR leads to much shorter values than chronic AR when LV is dilated with increased compliance Pressure half-time varies with SVR Vasodilators may shorten the pressure half-time even as the aortic regurgitant fraction improves
- 22. Evaluating the Severity of Aortic Regurgitation Regurgitant Volume or Fraction Pulsed Doppler imaging Stroke volume at any valve annulus is derived as the product of CSA and VTI of flow at the annulus In the absence of regurgitation, SV determinations at different sites (LVOT, mitral annulus, pulmonic annulus) should be equal Mild: < 30 cc (< 30%) Mild-moderate: 30-44 cc (30-39%) Moderately severe: 45-59 cc (40-49%) Severe: ≥60 cc (≥50%)
- 23. Evaluating the Severity of Aortic Regurgitation Regurgitant Volume or Fraction Stroke volume can be measured through any valve within the heart. This schematic demonstrates how stroke volume can be calculated at the level of the aortic valve and mitral valve . The difference in stroke volume represents the regurgitant volume. In addition, the regurgitant fraction can be calculated
- 24. Regurgitant Volume or Fraction Limitation Cannot be used in presence of shunts Sensitive to small measurement errors Requires multiple measurements, Assumes no regurgitation at reference valve Limited quantitative information Affected by sample volume location
- 25. Evaluating the Severity of Aortic Regurgitation Pulsed Doppler imaging Severe AR - diastolic flow reversal in the descending aorta Nonquantitative approach using pulsed Doppler imaging Presence of holodiastolic flow reversal in the descending aorta has been correlated with severe aortic regurgitation False positives may occur if a PDA is present This parameter is dependent on vessel compliance and the location of the sample volume
- 26. Evaluating the Severity of Aortic Regurgitation by M-mode echocardiography and two-dimensional imaging End-diastolic End-systolic LV dimensions Ejection fraction Fractional shortening End-systolic wall stress LV systolic dysfunction Increase in end-systolic dimension
- 27. Criteria for Severe AR Jet width >_65% of LVOT Vena contracta >0.6 cm Holodiastolic flow reversal in the proximal abdominal aorta Rvol>_60 ml/beat RF>50% ERO>_0.3 cm2 Angiography grade 3+ to 4+ Evidence of LV dilation
- 28. Take Home Message The best dimensional predictors of angiographic severity are jet area indexed to the LV short-axis area (parasternal short-axis view) and jet diameter indexed to LVOT diameter immediately proximal to the valve (paraternal long axis view) Jet length is not a reliable index of severity The pressure half-time is most relaible in the setting of acute regurgitation Holodiastolic flow reversal is a marker of at least moderate regurgitation
- 29. References • Recommendations for Evaluation of the Severity of Native Valvular Regurgitation with Two-dimensional and Doppler Echocardiography, A report from the American Society of Echocardiography’s Nomenclature and Standards Committee and The Task Force on Valvular Regurgitation • Feigenbaum's Echocardiography, 6th Edition, Feigenbaum, Harvey; Armstrong, William F.; Ryan, Thomas,Copyright ©2005 Lippincott Williams & Wilkins • Braunwald's Heart Disease: A Textbook of Cardiovascular Medicine, 10th Edition
Editor's Notes
- acuity of onset, aortic and LV compliance, hemodynamic conditions, and severity of the lesion.