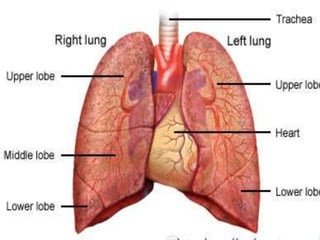
Pneumonia
- 2. INTRODUCTION Pneumonia is an infection of the lungs that is caused by bacteria, viruses, fungi, or parasites. It is characterized primarily by inflammation of the alveoli in the lungs or by alveoli that are filled with fluid (alveoli are microscopic sacs in the lungs that absorb oxygen). At times a very serious condition, pneumonia can make a person very sick or even cause death. Although the disease can occur in young and healthy people, it is most dangerous for older adults, babies, and people with other diseases or impaired immune systems.
- 3. Pneumonia is an inflammation or infection of the lungs most commonly caused by a bacteria or virus. Pneumonia can also be caused by inhaling vomit or other foreign substances. In all cases, the lungs' air sacs fill with pus , mucous, and other liquids and cannot function properly.This means oxygen cannot reach the blood and the cells of the body.
- 4. .
- 5. Classification by cause Bronchiolitis obliterans organizing pneumonia:(BOOP) is caused by inflammation inflammation of the small airways of the lungs.It is also known as cryptogenic organizing pneumonitis(COP). Eosinophilic pneumonia Eosinophilic pneumonia is invasion of the lung by eosinophils, a particular kind of white blood cell. Eosinophilic pneumonia often occurs in response to infection with a parasite or after exposure to certain types of environmental factors.
- 6. Chemical pneumonia Chemical pneumonia (usually called chemical pneumonitis) is caused by chemical toxicants such as pesticides, which may enter the body by inhalation or by skin contact. When the toxic substance is an oil, the pneumonia may be called lipoid pneumonia.
- 7. Aspiration pneumonia: This type of pneumonia occurs when people inhale foreign materials.The inhaled foreign materials cause inflammation of the bronchial tubes and lungs and May also result in formation of pus in the lungs. Often the inhaled foreign materials are stomach contents like secretions, vomits, food items and drinks. Dental problems, old age, having sedative drugs, being alcoholic, coma, and anesthesia are some of the contributing factors of aspiration pneumonia. The lung’s response depends primarily on the quantity and nature of the inhaled substance.The more will be the acidic nature of the material, the more will be the intensity of the lung injury.
- 8. Dust pneumonia: It is caused by excessive exposure to dust storms.With dust pneumonia, dust settles all the way into the alveoli of the lungs stopping the cilia from moving and preventing the lungs from ever clearing themselves. Necrotizing Pneumonia: Although overlapping with many other classification , necrotizing P pneumonia include Pneumonias that cause substantial necroses of lung cells and sometimes even lung abscess
- 9. Opportunistic pneumonia: includes those that frequently strike immunocompromised victims. Main pathogens are cytomegalovirus, Pneumocystis jiroveci, Mycobacterium avium- intracellulare, invasive aspergillosis, invasive candidiasis, as well as the "usual bacteria" that strike immunocompetent people as well. Double Pneumonia: This is historical term for acute lung injury or acute respiratory syndrome . However the term was and is still used by the people to denote Pneumonia affecting both lungs.
- 10. Lobar pneumonia Involvement of entire lobe Lobular pneumonia Involvement of parts of lobe only, segmental or of alveoli contiguous to bronchi
- 11. Usual Interstitial pneumonia (UIP) UIPInterstitial pneumonia is form of lung disease characterized by progressive scarring of both lungs.The scarring involves supporting framework (interstitial) of the lungs
- 13. Acute Pneumonia: Acute pneumonia lasts less than three weeks indurations . Acute Pneumonia further divided into :- Classic bacterial bronchopneumonia such as streptococcus pneumonia and atypical pneumonia such as interstitial pneumonitis of mycoplasama pneumonia and aspiration pneumonia syndromes. Chronic pneumonia syndrome:- This occurs or tend to be either non infectious or mycobacterial fungal or mixed bacterial infection caused by airway obstruction . It includes actinomyces and blastomyces dermatitidis as well as mycobacterium tuberculosis and atypical mycobacterium.
- 14. Community Acquired pneumonia Community acquired pneumonia occurs outsides of hospital setting .Most people get CAP by breathing in germs (especially by sleeping)that live in mouth nose or throat Nosocomial and others Organisms that have been exposed to strong antibiotics and have developed resistance are called nosocomial organisms. If they enter the lungs, a person may develop nosocomial pneumonia. Resistant bacteria are often found in nursing homes and hospitals. An example is MRSA, or methicillin-resistant Staph aureus, which can cause skin infections as well as pneumonia.
- 15. Similarly, outbreaks of the H5N1 influenza (bird flu) virus and severe acute respiratory syndrome (SARS) have resulted in serious pneumonia infections. Anthrax, plague, and tularemia also may cause pneumonia, but their occurrences are rare.
- 16. Atypical pneumonia :It also known as walking pneumonia, is the type of pneumonia not caused by one of the more traditional pathogens. Its clinical presentation contrasts to that of "typical" pneumonia. A variety of microorganisms can cause it. When it develops independently from another disease it is called primary atypical pneumonia (PAP). atypical organisms include special bacteria, viruses, fungi, and protozoa. In addition, this form of pneumonia is atypical in presentation with only moderate amounts of sputum, no consolidation, only small increases in white cell counts, and no alveolar exudate. At the time that atypical pneumonia was first described, organisms like Mycoplasma, Chlamydophila, and Legionella still were not recognized as bacteria and instead considered viruses. Hence "atypical pneumonia" was also called "non- bacterial.It includes following.
- 17. Bacterial pneumonia : As the name suggests, this type of pneumonia is caused by different types of bacteria.The most pneumonia inducing bacterium is Streptococcus pneumonia.This pneumonia types generally affects people who have weakened immune system for reasons like old age, illness, malnutrition etc. Bacterial pneumonia is indicated with signs like rapid breathing, increased pulse rate, high fever with chills and shaking, acute chest pain, chattering teeth, palpitations, greenish and rust colored mucus, heavy perspiration etc. Viral pneumonia :This variant of pneumonia can be caused by different types of viruses.The most common forms of viruses causing viral pneumonia are flu virus, parainfluenza virus, herpes simplex virus, rhinovirus, adenovirus, Hantavirus, cytomegalovirus and respiratory syncytial virus. Symptoms of virus induced pneumonia are similar to that of the pneumonia episodes caused by bacteria. People with viral pneumonia are at risk of developing bacterial pneumonia.
- 18. The pneumonia episodes triggered by cytomegalovirus or CMV are more common among immune suppressed individuals. CMV belongs to the group of herpes viruses. Patients undergoing processes like bone marrow transplants and solid organ transplants often get infected with CMV.The CMV induced pneumonia is generally accompanied by no significant symptom. However, if CMV causes pneumonia in AIDS patients, people undergoing chemotherapy, bone marrow or organ transplant patients the consequences can be quite severe. Recently obtained statistics have revealed that 20 percent of the patients undergoing bone marrow transplants develop CMV pneumonia.The mortality rate is exceedingly high among patients who suffer from CMV pneumonia simultaneously with hypoxemia (a condition characterized by decreased levels of oxygen in blood).
- 19. Mycoplasma Pneumonia : The condition is named so as it is triggered by mycoplasmas (tiniest free- living agents causing diseases in human beings). The mycoplasmas are known to possess features of both bacteria and viruses. People of every age group can suffer from mycoplasma pneumonia.The symptoms of mycoplasma pneumonia differ significantly from symptoms of the other types of pneumonia. Patients may experience symptoms like rashes and anemia. Some patient may also develop neurological syndromes like encephalitis, myelitis and meningitis.
- 20. Fungal pneumonia : Fungal pneumonia is one of the rarest types of pneumonia.The fungus causing this type of pneumonia is Pneumocystis carinii.This pneumonia types is also more common among people with weak immune system. Often pneumocystis carina pneumonia is described as a complication experienced by AIDS patients. Cancer patients are also at risk of pneumocystis carinii pneumonia.
- 21. Ventilator-associated and hospital-acquired pneumonia Ventilator-associated pneumonia (VAP) is pneumonia that develops 48 hours or longer after mechanical ventilation is given by means of an end tracheal tube or tracheotomy.Ventilator- associated pneumonia (VAP) results from the invasion of the lower respiratory tract and lung parenchyma by microorganisms. Intubation compromises the integrity of the or pharynx and trachea and allows oral and gastric secretions to enter the lower airways.
- 22. Congestion: In the first 24 hours:This stage is characterized histological by vascular engorgement, intra- alveolar fluid, small numbers of neutrophils, often numerous bacteria. Grossly, the lung is heavy and hyperemic. Red hepatization or consolidation:Vascular congestion persists, with extravasations of red cells into alveolar spaces, along with increased numbers of neutrophils and fibrin.The filling of airspaces by the exudates leads to a gross appearance of solidification, or consolidation, of the alveolar parenchyma.This appearance has been likened to that of the liver, hence the term "hepatization
- 23. Grey hepatization: Red cells disintegrate, with persistence of the neutrophils and fibrin.The alveoli still appear consolidated, but grossly the color is paler and the cut surface is drier. Resolution (complete recovery):The exudates is digested by enzymatic activity, and cleared by macrophages or by cough mechanism. Enzymes produced by neutrophils will liquefy exudates, and this will either be coughed up in sputum or be drained via lymph.
- 24. Bacteria and viruses are the primary causes of pneumonia.When a person breathes pneumonia-causing germs into his lungs and his body's immune system cannot otherwise prevent entry, the organisms settle in small air sacs called alveoli and continue multiplying. As the body sends white blood cells to attack the infection, the sacs become filed with fluid and pus - causing pneumonia.
- 25. Bacterial Streptococcus pneumoniae is the most common cause of bacterial pneumonia. People who suffer from chronic obstructive pulmonary disease (COPD) or alcoholism most often get pneumonia from Klebsiella pneumoniae and Hemophilus influenzae.Atypical pneumonia, a type of pneumonia that typically occurs during the summer and fall months, is caused by the bacteria Mycoplasma pneumoniae. People who have Legionnaire's disease caused by the bacterium Legionella pneumoniae (often found in contaminated water supplies and air conditioners) may also develop pneumonia as part of the overall infection.Another type of bacteria responsible for pneumonia is called Chlamydia pneumoniae. Pneumocystis carinii pneumonia is a form of pneumonia that usually affects both lungs and is found in patients with weakened or compromised immune systems from such conditions as cancer and HIV/AIDS and those treated withTNF (tumor necrosis factor) for rheumatoid arthritis
- 26. Viral Viral pneumonias are pneumonias that do not typically respond to antibiotic treatment (in contrast to bacterial pneumonias). Adenoviruses, rhinovirus, influenza virus (flu), respiratory syncytial virus (RSV), and parainfluenza virus are all potential causes of viral pneumonia. Fungal Fungal pneumonia is uncommon,but it may occur in individuals with weakened immune systems due to AIDS, immunosuppressive drugs, or other medical problems. Histoplasmosis, coccidiomycosis, blast mycosis, aspergillosis, and cryptococcosis are fungal infections that can lead to fungal pneumonia
- 27. Risk Factors 1. Cigarette smoking disrupts both mucocillary and macrophage activity. 2. Immuno-compromised patients and those with a low neutrophil count. 3.Prolonged immobility and shallow breathing. 4. Conditions which causes pneumonia like cancer, COPD. 5.Alcohol intoxication: Alcohol suppress the body reflexes, may be associated with aspiration and decrease white cell mobilization and tacheobronchial culinary motion.
- 28. Advanced age: In advanced age possible depressed cough and glottis reflexes and nutritional depletion. 7.Respiratory therapy with improperly cleaned equipment. 8.People living in environment or social settings in which the risk of disease is high. 9.General anesthetic, sedative or opioid preparations that promote respiratory depression , which causes a shallow breathing pattern and predispose to the pooling of bronchial secretions and potential development of pneumonia. 10.Nothing-by-mouth(NPO) status, placement of nasogastric or end tracheal tube.
- 30. Cough Rusty or green mucus (sputum) coughed up from lungs Fever Fast breathing and shortness of breath Shaking chills Chest pain that usually worsens when taking a deep breath (pleuritic pain) Fast heartbeat Fatigue and feeling very weak
- 31. Nausea and vomiting Diarrhea Sweating Headache Muscle pain Confusion or delirium Dusky or purplish skin color (cyanosis) from poorly oxygenated blood
- 32. In a community setting (general practice), pneumonia is usually diagnosed based on symptoms and physical examination alone. But in the hospitals following tests should be conducted to make a diagnose History( particularly of a recent respiratory infection), physical examination. Chest x-rays can reveal areas of opacity (seen as white) which represent consolidation. Chest CT (computed tomography) can reveal pneumonia that is not seen on chest x-ray.
- 33. Sputum cultures generally take at least two to three days, so they are mainly used to confirm that the infection is sensitive to an antibiotic that has already been started. 5.Acomplete blood count may show a high white blood cell count, indicating the presence of an infection or inflammation. 6.Bronchoscopy is a procedure in which a thin, flexible, lighted viewing tube is inserted into the nose or mouth after a local anesthetic is administered.The breathing passages can then be directly examined by the doctor, and specimens from the infected part of the lung can be obtained.
- 34. Goal:The goal of treatment is to control symptoms such as fever cough and shortness of breath until the person recover another goal is to minimize development of serious complications such as severe shortness of breath and hypoxia., First step in treatment of Pneumonia is prevention. The risk of developing Pneumonia can be reduced by not smoking and avoiding air pollutants, and contact with people who are sick with Pneumonia, influenza and other respiratory infections. Good hand washing practice minimizes the spread of viruses, bacteria and microorganism that cause Pneumonia.
- 35. Mild cases of pneumonia that occur in generally healthy adults may be treated at homes.Treatment includes getting plenty of rest and fluids and using a humidifier.The physician will also recommend over- the - counter or prescription medications to relieve pain, fever and cough. Antibiotics are prescribed if the illness is a form of bacterial pneumonia.Antibiotics are ineffective in curing viral pneumonia.
- 36. Hospitalization:- Moderate to severe Pneumonia result in low level of oxygen in the blood and require hospitalization and intravenous antibiotic administration if the cause is a bacterial infection. . Oxygen therapy: - Supplemental oxygen helps to relieve the shortness of the breath and ensure that the vital organs such as the Heart and the Brain get the enough oxygen. Concentrations of the oxygen and the types of the devices used vary depending on the severity of an individual's condition.
- 37. In the most severe cases in which complications such as hypoxia, respiratory failure and shock occurs are likely to occur, a breathing tube may be inserted into the lungs through the mouth to keep the airway open ( intubation). Bronchodilators:- If there is a shortness of breath, a bronchodilator may be needed. Bronchodilators help to relax and open up the lower airways in the lungs and are inhaled into the lungs using a device called an inhaler. Albuterol, Formoterol, Arformoterol, Aminophylline,Theophylline are common examples of the bronchodilators used.
- 38. Bacterial pneumonias are usually treated with antibiotics. Initially antibiotic choice depends on the characteristics of the person affected, such as age, underlying health, and the location the infection was acquired. Amoxicillin is recommended first line for community- acquired pneumonia.The duration of treatment has traditionally been seven to ten days, but there is increasing evidence that short courses (three to five days) are similarly effective. Antibiotics recommended for hospital-acquired pneumonia include third- and fourth-generation cephalosporin’s, carbapenems, fluoroquinolones, amino glycosides, and vancomycin.These antibiotics are often given intravenously, and may be used in combination
- 39. Viral pneumonias are treated with rest and plenty of fluids. Neuraminidase inhibitors may be used to treat viral pneumonia caused by influenza viruses (influenza A and influenza B). Influenza A may be treated with rimantadine or amantadine, while influenza A or B may be treated with oseltamivir, zanamivir.These are of most benefit if they are started within 48 hours of the onset of symptoms. Fungal pneumonias are usually treated with antifungal medications.
- 40. Over-the-counter medications are also commonly prescribed to better manage pneumonia symptoms.These include treatments for reducing fever, reducing aches and pains, and suppressing coughs. In addition, it is important to get plenty of rest and sleep and drink lots of fluids. Hospitalization for pneumonia may be required if symptoms are especially bad or a patient has a weakened immune system or other serious illness. At the hospital, patients generally are treated with intravenous antibiotics and possibly put on oxygen. Typically, oral antibiotics, rest, simple analgesics, and fluids are sufficient for complete resolution.
- 41. There are several ways to prevent pneumonia.There are two vaccines that are available to prevent pneumococcal disease (the bacterial infection that is the most common cause of pneumonia): pneumococcal conjugate vaccine (Prevnar) : Prevnar is generally administered as part of the normal infant immunization procedure and is recommended for children less than 2 years of age or between two and four years with certain medical conditions. pneumococcal polysaccharide vaccine (Pneumovax) : Pneumovax is provided for adults who are at increased risk of developing pneumococcal pneumonia, such as the elderly, diabetics, those with chronic heart, lung, or kidney disease, alcoholics, smokers, and those without a spleen.
- 42. The pneumonia vaccine may not completely prevent older adults from getting pneumonia, but it can reduce the severity of a future pneumonia.
- 43. In addition to vaccinations, physicians recommend that people wash hands refrain from smoking eat healthfully exercise stay away from sputum or cough particles from others with pneumonia. Avoid over crowding Never neglect a common cold Sleep in the well ventilated room
- 44. Educate mothers to burp babies after giving feeds When child has measles, whooping cough etc, try to prevent pneumonia by proper treatment & care If pneumonia develops start treatment as quickly as possible.
- 45. Assessment The nursing history should explore following area with the client in whom pneumonia is suspected or confirmed: Contact with other clients experiencing similar manifestation (suggests viral or mycoplasmal pneumonia) Factors suggesting the presence of noninfectious diseases that produce manifestations similar to pneumonia (e.g pulmonary embolism, allergic reaction to drugs or other substance, cancer) Lowered levels of consciousness, which increase the risk of aspiration.
- 46. Presence of tuberculosis or contact with others who have active tuberculosis. Presence & character of any chest pain. Presence & character of cough & sputum production.
- 47. Perform respiratory infection every 4 hour, including determination of the rate & character of respiration, auscultation of breath sounds, & assessment of skin & nail beds to determine the severity of hypoxia. In addition to physical examination, transcutaneous oxygen level analysis or ABG measurements may be used to evaluate the need for oxygen support.
- 48. Nursing Diagnosis Impaired gas exchange related to retained secretion & inflammatory pulmonary infection. Interventions: Administer oxygen to maintain oxygen saturation above 92% or as ordered. If oxygen administered, monitor oral mucus membranes. Assess the skin underneath the oxygen tubing for signs of pressure ulcer
- 49. Ineffective airway clearance related to excessive secretion & weak cough Interventions: Teach client to take increase fluid intake, effective coughing & deep breathing techniques. Encourage client to use their incentive spirometclient er every 2 hours while awake. Only thickened liquid should give to with dysphasia. If indicated more aggressive measures to maintain airway patency may be required (e.g. chest physiotherapy, suctioning, and artificial airway).
- 50. Activity intolerance related to decreased oxygen levels for metabolic demands. Interventions: Assess the client’s baseline activity level & response to activity. Schedule activities after treatments or medications. Provide psychological support & quite environment to reduce anxiety & promote rest. Regulate nursing care & visitors as warranted by clients condition. Gradually increase activities on the basis of tolerance.
- 51. Impaired oral mucus membrane related to breathing through mouth. Interventions: Assess the oral mucus membrane every shift. If the client can swab the mouth, leave swabs & water on the over-bed table. If the client can’t moisten the mouth, swab the mouth for the client.