Roseola infantum Made Ridiculously Easy!!!
- 1. Viral Exanthem Part II: Roseola infantum:
- 2. Definition and nomenclature: Roseola infantum is an acute febrile illness with a maculopapular eruption. The classic presentation of roseola infantum is a 9- to 12-month-old infant who acutely develops a high fever and often a febrile seizure. After 3 days there is a rapid decline in fever, and a morbilliform rash appears. Also called: Exanthema subitum or Exanthem subitum Sixth Disease 3 day fever
- 3. Epidemiology: Incidence and prevalence: Roseola infantum is the most common exanthematic fever in children under the age of 2 years Incidence: 24% of acute febrile illness presenting at a paediatric emergency department. Age Peak incidence is between 6 and 9 months.
- 4. Pathophysiology: Causative organisms HHV‐6 (most commonly) HHV‐7 Roseola is spread as air borne or droplet infection. The child is probably infectious during the whole period of the disease and may be even before the high temperature begins.
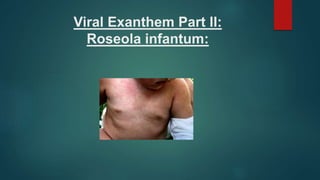
- 5. Clinical features: History The incubation period is from 10 to 15 days. Presentation: Early Symptoms: The first sign of illness is abrupt onset of fever, usually 39.5 - 40°C, which persists for 3–5 days ; Accompanied by few or no symptoms. Irritability, Inflamed tympanic membranes, Papules and ulcers at the posterior palate and uvula (Nagayama spots) Periorbital oedema and Haematuria Exanthem: As the temperature falls, an eruption of discrete rose‐pink maculopapules develops on the neck and trunk; May spread to the arms, face and legs. The lesions may have surrounding pallor and rarely become vesicular. Lasts for 2 days Patient’s cervical and occipital lymph nodes are usually enlarged.
- 6. Clinical variants: Primary infection in Adults: There may be a mononucleosis‐like illness, with variable fever or rash and with mainly cervical lymphadenopathy, which may persist for up to 3 months; or an acute but self‐limiting hepatitis
- 7. Differential diagnosis: Measles: Lack of upper respiratory tract symptoms. Rubella: Usually seen in older children Scarlet Fever Exanthematous drug reaction
- 8. Complications and co‐morbidities Febrile convulsions: occur in 13% of the cases. Fatal encephalitis: Thrombocytopenia Purpura fulminans Haemophagocytic syndrome Associations: Papular purpuric gloves and socks syndrome Gianotti–Crosti syndrome Stevens–Johnson syndrome Pityriasis rosea
- 9. Disease course and prognosis: Rash fades after 1-2 days leaving no scaling or pigmentation. Reactivation of the latent virus may occur, especially in immune suppression
- 10. Investigations: (1) Serology: Confirmation is by demonstrating a seroconversion or rise in antibody titre to HHV‐6, by indirect immunofluorescence using cells infected with HHV‐6 as antigen. IgM antibody appears 5–7 days after the rash, reaching maximum titre after 2 weeks and persisting for about 2 months. Does not distinguish between HHV- 6A and 6B strains (2) PCR: Molecular detection of viral RNA by RT‐PCR or DNA by PCR Distinguishes HHV‐6A from ‐6B HHV‐6 DNA has been demonstrated in the cerebrospinal fluid of children with both primary HHV‐6 infection and also at times of recurrent seizures following exanthem subitum, (3) Complete Blood Count: During the first 2 days there may be leukocytosis As the rash develops, leukopenia with a relative lymphopenia
- 11. Management: First line Only symptomatic measures are usually required. Second line Antiviral therapy with ganciclovir, valganciclovir, cidofovir or foscarnet would be appropriate in individuals with severe disease.
- 12. Roseola Infantum Timeline: Fever: Lasts 3-5 days Maculopapular Rash Appears as fever settles. Lasts 2 – 3 days IgM antibodies appear reaching peak titres in 2 weeks. Persisting for 2 months Incubation Period: 10-15 days 5-7 days later
- 13. Summary Of Viral Agents and their Clinical Manifestations:
- 14. Future Topics to be Discussed: 1)Rubella 2)Infectious Mononucleosis 3)Adenovirus 4)Enterovirus 5)Cytomegalovirus 6)West Nile Fever