Vertebral Artery Pathology: A Guide for Osteopaths
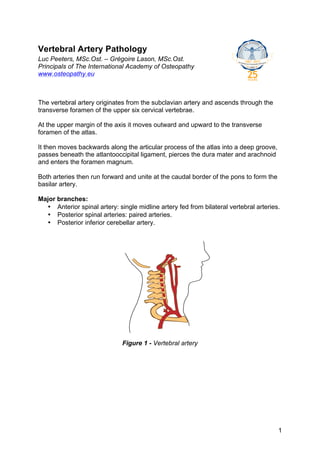
- 1. Vertebral Artery Pathology Luc Peeters, MSc.Ost. – Grégoire Lason, MSc.Ost. Principals of The International Academy of Osteopathy www.osteopathy.eu The vertebral artery originates from the subclavian artery and ascends through the transverse foramen of the upper six cervical vertebrae. At the upper margin of the axis it moves outward and upward to the transverse foramen of the atlas. It then moves backwards along the articular process of the atlas into a deep groove, passes beneath the atlantooccipital ligament, pierces the dura mater and arachnoid and enters the foramen magnum. Both arteries then run forward and unite at the caudal border of the pons to form the basilar artery. Major branches: • Anterior spinal artery: single midline artery fed from bilateral vertebral arteries. • Posterior spinal arteries: paired arteries. • Posterior inferior cerebellar artery. Figure 1 - Vertebral artery 1
- 2. Into foramen magnum Atlas Axis Figure 2 - Vertebral artery during head rotation Anomalies • Ten percent of patients have some form of anomaly in their vertebral arteries. • Compression of the vertebral arteries is seen in 5% of the population in a neutral position and the same in rotation. • One of the two or both vertebral arteries can be absent. • Variations in arterial diameter, average 4.3 mm on the right, 4.7mm on the left. • In the upper segment: tortuous vessel in 39% of specimens. • In 5-20% of specimens the posterior inferior cerebellar arteries have an extra dural origin approximately 1 cm. proximal to dural penetration. Possible pathologies • Arteriopathy may arise from heritable conditions such as Marfan’s disease or osteogenesis imperfect. • Arteriopathy may also arise from fibromuscular hyperplasia. • Arterial damage, particularly involving the tunica intima will yield the start of increased localised clotting and thereby thrombus formation. • Arterial flow changes can result from histological changes as well as from mechanical changes in the vessel. • Emboli present in three primary forms - liquid, solid or gaseous. The thrombus at the site of arterial damage is invariably the source of emboli yielding ischemic stroke from the vertebral artery. • Ischemia: the degree of ischemia as results from an embolism is the consequence of the size of the embolism, the location of the embolism and the presence/absence of collateral circulation to the affected area. • Aneurysm may occur: congenital aneurysms occur most commonly at the site where the two arteries join in the formation of the circle of Willis. At this point the tunica media is deficient and complicated by the development of atheroma, which weakens the arterial wall and local dilatation occurs. The aneurysms may compress the neighbouring structures or may suddenly rupture into the subarachnoid space. • Severe pain at back of head may be symptomatic of the disease of the vertebral artery just before entering skull. It is due to the close connection of the artery with the suboccipital nerve in the groove on the posterior arch of the atlas. 2
- 3. • Disease of the vertebral artery can affect speech. Pressure on the hypoglossal nerve then leads to paralysis of tongue muscles. • Vertebrobasilar artery occlusion: o Ipsilateral pain and temperature loss of face. o Contralateral pain and temperature loss of body. o Blindness. o Vertigo, nystagmus, nausea, vomiting. o Ipsilateral Horner’s syndrome. o Ipsilateral ataxia and other cerebellar signs. o Unilateral//bilateral hemiparesis. o Coma. Vertebral artery dissection A dissection occurs when a tear forms in the innermost part of the arterial wall, the tunica intima, allowing blood to collect behind the intima and the next layer of the artery, the tunica media. The literature indicates that vertebral artery dissection arises spontaneously, from trivial movement, minor or major trauma. Subintimal dissections tend to result in stenosis of the artery. Subadventitial dissections tend to result in aneurysm formation. An expanding hematoma in the wall of the artery is the root of the problem. The intramural hematoma can arise from haemorrhage of the vasa vasorum within/associated with the tunica media or from the development of an intimal flap in the lumen of the vessel. Concerning the typical vertebral artery tests: • There are no reliable or safe tests that will rule out a vertebral artery dissection in progress. There are no tests that will identify a patient at risk for vertebral artery dissection. • The case history is therefore of the outmost importance: o Dizziness. o Drop attacks. o Diplopia. o Dysarthria. o Dysphagia. o Ataxia. o Nausea. o Numbness. o Nystagmus. o Since many patients seek care for these symptoms, the presence of these symptoms, may or may not be an indication of a possible vertebral artery dissection in progress. It is rather the constellation of symptoms (for example: dizziness, nausea and diplopia in the same patient), the uniqueness of the symptom (for example: drop attacks) and the severity of the symptoms that should draw the osteopaths attention. o Neck pain that the patient never experienced before despite a history of cervical complaints, sudden headache without former history, referral pain from the vertebral artery are also alert signs. 3
- 4. Vertebral artery Internal carotid artery Figure 3 - Referred pain from the vertebral artery and internal carotid artery Figure 4 - Vertebral artery dissection It is clear that osteopaths can’t treat vertebral artery pathology. They must be aware of the phenomenon and recognise the symptoms for referral. In vertebral artery pathology of any kind, manipulating the cervical spine is contra- indicated. 4
- 5. Bibliography 1. Grant & Boileau J.C. (2004) Grant's Atlas of Anatomy 11th edition – April. Edited Lippincott, Williams & Wilkins. 2. Gray's Anatomy (1995) The Anatomical Basis of Medicine and Surgery. 38th British Edition - August Churchill Livingstone. 3. Haynes M.J., Vincent K., Fischhoff C., Bremner A.P., Lanlo O. & Hankey G.J. (2012) Assessing the risk of stroke from neck manipulation: a systematic review. International Journal of Clinical Practice 66 (10): 940–947. 4. Kim Y.K. & Schulman S. (2009). Cervical artery dissection: pathology, epidemiology and management. Thromb. Res. 123 (6): 810–21. 5. Rubinstein S.M., Peerdeman S.M.M, van Tulder M.W., Riphagen I. & Haldeman S. (2005) A systematic review of the risk factors for cervical artery dissection. Stroke 36 (7): 1575–1580. http://www.facebook.com/IAOdeutsch All rights reserved. © 2012. http://www.facebook.com/IAOenglish No part of this article may be http://www.facebook.com/IAOnederlands reproduced or made public by http://www.facebook.com/IAOfrancais printing, photocopying, microfilming, or by any means without the prior written permission of the publisher. iNeuro APP iCranialNerves APP Also available for Android. 5
