23204922
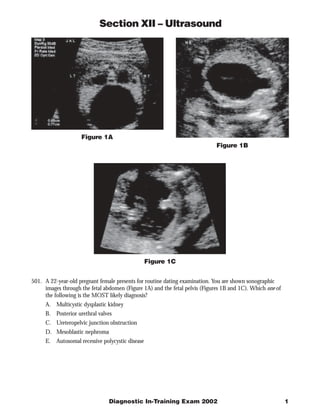
- 1. Section XII – Ultrasound Figure 1A Figure 1B Figure 1C 501. A 22-year-old pregnant female presents for routine dating examination. You are shown sonographic images through the fetal abdomen (Figure 1A) and the fetal pelvis (Figures 1B and 1C). Which one of the following is the MOST likely diagnosis? A. Multicystic dysplastic kidney B. Posterior urethral valves C. Ureteropelvic junction obstruction D. Mesoblastic nephroma E. Autosomal recessive polycystic disease Diagnostic In-Training Exam 2002 1
- 2. Section XII – Ultrasound Question #501 Findings: Bilateral hydronephrosis, megacystis, and a dilated posterior urethra (“keyhole”) in a male fetus. Rationales: A) Incorrect. The multicystic dysplastic kidney contains multiple cysts of various sizes that are not connected but replace essentially all renal parenchyma. The kidney is usually large but can be normal sized. Multicystic dysplastic kidney is usually a unilateral process with a good prognosis. Bilateral multicystic dysplastic kidney is uniformly fatal because of the nonfunctional status of the affected kidneys. In bilateral multicystic dysplastic kidney, there is often oligohydramnios and there should be no fluid in the bladder. These features differ from those in the test case. B) Correct. Posterior urethral valves obstruct the prostatic urethra in the male fetus, resulting in a dilated proximal urethra and bladder. Most affected fetuses have sonographically evident hydroureteronephrosis, secondary to reflux or obstruction. In some cases, the kidneys are small or echogenic or contain cysts, all of which are signs of cystic renal dysplasia. Moderate to severe oligohydramnios is common. The features of posterior urethral valves are present in the test case. C) Incorrect. Ureteropelvic junction (UPJ) obstruction is the most common congenital urinary tract anomaly. Sonographically, the diagnosis is suggested by the presence of a dilated renal pelvis and calyces in the setting of a non-dilated ureter and a normal bladder. The degree of pelvicaliectasis and parenchymal thinning is variable. The bilateral hydronephrosis, megacystis and dilated posterior urethra do not favor UPJ obstruction. D) Incorrect. Mesoblastic nephroma, (also termed fetal renal hamartoma) is a common renal mass in infants under 1 year of age. The common presenting sign is a painless abdominal mass. Microscopically, mesoblastic nephroma contains intersecting bundles of spindle cells, dysplastic tubules, and islands of cartilage. The sonographic features are usually those of a large, echogenic mass with a homogeneous echopattern or heterogeneous echotexture related to areas of necrosis or hemorrhage. Occasionally concentric hypo- and hyperechoic rings surround the mass. E) Incorrect. The typical sonographic features of prenatally detected autosomal recessive (infantile) disease are bilateral, markedly enlarged, and echogenic kidneys, associated with oligohydramnios and a small bladder. These features are substantially different from those in the test case. The abnormal renal enlargement and echogenicity arise from dilatation of renal tubules, creating a multiplicity of sonic interfaces. The cystic tubules are usually too small to resolve as discrete cysts. Citations: Callen. Ultrasonography in Obstetrics and Gynecology. 4th ed. WB Saunders Co., Philadelphia, PA. 2000. 2 American College of Radiology
- 3. Section XII – Ultrasound Figure 2A Figure 2B 502. A 27-year-old pregnant woman presents at 19 weeks gestation with size greater than dates. You are shown two sonograms through the fetal cranium (Figure 2A, coronal; Figure 2B, axial). Which one of the following is the MOST likely diagnosis? A. Hydrocephalus B. Hydranencaphaly C. Holoprosencephaly D. Porencephaly E. Anencephaly Diagnostic In-Training Exam 2002 3
- 4. Section XII – Ultrasound Question #502 Findings: A coronal sonogram of the fetal head shows a single monoventricle and fused midline thalami. There is no evidence of the formation of distinct lateral ventricles. No falx or other midline structure is identified. A thin rim of surrounding brain parenchyma is present. These findings are most consistent with diagnosis of alobar holoprosencephaly. Rationales: A) Incorrect. Hydrocephalus is a term used to describe dilatation of the ventricular system. The cerebral cortex is present but can be markedly thinned in fetuses with very severe hydrocephalus. The falx and other midline structures are normal. The frontal horns of the lateral ventricles are separated and the thalami are normal rather than fused, as seen in fetuses with holoprosencephaly. The absence of distinct lateral ventricles and the apparent fusion of the thalami make hydrocephalus an unlikely diagnosis. B) Incorrect. Hydranencephaly is characterized by complete or near complete absence of the cerebral hemispheres, which are replaced with cerebrospinal fluid (CSF) contained within intact meninges. Occasionally, a minute amount of cerebral cortex is preserved, but is usually not detectable by sonography. Thus, in hydranencephalic fetuses, sonography of the fetal head demonstrates no cortical mantle. There is variable development of the falx. The finding of an irregular cortical mantle in the fetus in the test case eliminates hydranencephaly as a diagnostic possibility. In addition, hydranencephaly is extremely rare, and the few reported cases have been primarily in the third trimester. C) Correct. Holoprosencephaly represents a continuum of anomalous development. The most severe form is alobar holoprosencephaly, in which no cleavage of the prosencephalon has occurred. The brain is small and lacks a normal ventricular system. A monoventricular cavity is present; the thalami are fused and the third ventricle is absent. The test case is an example of alobar holoprosencephaly. An intermediate form of holoprosencephaly is termed semilobar holoprosencephaly. A monoventricular cavity with rudimentary occipital horns is present, and the thalamus and basal ganglia are totally or partially fused. In the least severe type, lobar holoprosencephaly, the two hemispheres and lateral ventricles are separated. The frontal horns are hypoplastic, but the remainder of the ventricular system develops nearly normally. The basal ganglia and thalami are usually separated. A strong association with aneuploidy has been demonstrated. Prenatal ultrasound can identify the vast majority of affected fetuses before the time of viability. D) Incorrect. Porencephaly refers to a CSF-filled cyst or cavity within the brain, which many communicate with the ventricular system. The cystic space is thought to be the consequence of a vascular, traumatic, or infectious destructive process that focally damages the parenchyma. The prenatal sonographic findings of porencephaly include a cystic space in the brain parenchyma and a normally formed ventricular system, although hydrocephalus may be present. The falx and infratentorial structures are normal. Porencephaly is an unlikely diagnosis in the test case because of the abnormal ventricular system shown in the test images. E) Incorrect. Anencephaly results from a failure of the rostral neuropore to close and is distinguished by absence of the cerebral hemispheres and accompanying cranium. In this case, a normal calvarium is demonstrated which excludes the diagnosis. The diagnosis is usually made in utero. Imaging studies are rarely needed postnatally. Citations: Diagnostic ultrasound of fetal anomalies: Text and Atlas. Nyberg DA, Mahoney BS, Pretorius DH. Yearbook Medical Publishers, 1990. 4 American College of Radiology
- 5. Section XII – Ultrasound Figure 3A Figure 3B 503. A 29-year-old otherwise healthy male with acute renal failure following successful completion of a marathon on a hot day. You are shown two longitudinal images (Figure 3A and Figure 3B) through the right hepatorenal fossa. Which one of the following is the MOST likely diagnosis? A. Hemorrhagic renal cyst B. Angiomyolipoma C. Renal cell carcinoma D. Adrenal metastases E. Myelolipoma Diagnostic In-Training Exam 2002 5
- 6. Section XII – Ultrasound Question #503 Findings: Images demonstrate a 4.5 cm homogeneously hyperechoic suprarenal solid mass. Rationales: A) Incorrect. This mass is solid and hyperechoic in appearance. In contrast, a hemorrhagic renal cyst would arise in the renal parenchyma. It may appear echogenic but it should have through transmission. B) Incorrect. Angiomyolipomas are benign renal tumors composed of varying proportions of adipose tissue, smooth muscle cells, and blood vessels. Although the sonographic findings in this patient are similar to those of an angiomyolipoma, the suprarenal location of the mass excludes the diagnosis of angiomyolipoma. C) Incorrect. Renal cell carcinomas are typically hypoechoic, although up to 30% of renal cell carcinomas under 3 cm in size may be hyperechoic. Again, however, the suprarenal appearance of this mass, and its homogeneous hyperechoic nature make renal cell carcinoma unlikely. D) Incorrect. Metastases to the adrenal are common, but this young patient has no other known malignancy. In addition, metastases are typically hypoechoic, not hyperechoic as in the test patient. E) Correct. Myelolipomas are rare, benign, non hyperfunctioning adrenal tumors composed of varying proportions of fat and bone marrow elements. If enough fat is present (as in this case), these tumors are typically seen as an echogenic mass in the adrenal bed. Citations: Rumack CM, Wilson SR, Charboneau JW. Diagnostic ultrasound, 2nd ed. Mosby . St. Louis, MO, 1998. 6 American College of Radiology
- 7. Section XII – Ultrasound Figure 4A Figure 4B 504. A 30-year-old female presents with pain in the iliac fossa five days after renal transplant. You are shown gray scale (Figure 4A) and pulsed Doppler (Figure 4B) sonograms of the transplant. Which one of the following is the MOST likely diagnosis? A. Renal vein thrombosis B. Cyclosporine toxicity C. Hyperacute rejection D. Renal artery spasm E. Post transplant lymphoproliferative disorder Diagnostic In-Training Exam 2002 7
- 8. Section XII – Ultrasound Question #504 Findings: Grayscale image demonstrates mild nephromegaly at 14.1 cm. The spectral display of Doppler shifts shows reversal of diastolic flow. This means that intrarenal resistance to arterial inflow has increased. When there is very high resistance to inflow, systolic Doppler curves are also reduced to narrow, short, vertical spikes. This was confirmed in all segments of the kidney and no detectable renal venous signal was obtainable. Rationales: A) Correct. Acute renal vein thrombosis (RVT) is a rare complication of renal transplantation (<1% of renal transplant patients) and results in high intrarenal impedance and reduced arterial inflow, especially diastolic. Doppler imaging reveals absent renal venous flow with reversed diastolic arterial flow. Grayscale imaging often demonstrates a swollen kidney. B) Incorrect. Cyclosporine is an integral part of immunosuppressive therapy for renal transplantation. It exhibits an inhibitory effect on antigen-reactive T lymphocytes. Therapy with cyclosporine can result in damage to the renal tubules. Clinical signs include oliguria, fever, and hypertension. Cyclosporine induced nephropathy does not usually cause an abnormal grayscale appearance. The arterioles are usually spared, and so diastolic flow is not reduced or reversed. Occasionally an elevated RI can be seen occasionally, presumably, because of intrarenal edema or spasm of arcuate arteries. Although the resistive indices are elevated they do not typically result in reversed diastolic arterial flow. The reversal of diastolic flow makes the diagnosis of cyclosporine toxicity unlikely in the test patient. C) Incorrect. Hyperacute rejection is mediated by preexisting humoral antibodies and occurs during or within hours of surgery. This form of rejection occurs in recipients who have been sensitized by previous blood transfusions, pregnancies, or a previous graft. Resistive indices can be elevated and diastolic flow reversal can occur in hyperacute rejection. However, hyperacute rejection is an unlikely diagnosis in the test case because of the onset of symptoms 5 days after transplantation.. D) Incorrect. Pulsed Doppler examination shows arterial Doppler shifts arising from within the allograft. This means that the renal arteries are patent. Spasm of the renal arteries would dampen or completely obliterate Doppler signals arising from intrarenal arteries. E) Incorrect. Renal transplant recipients, particularly those treated with cyclosporine, are at increased risk for the development of post-transplant lymphoproliferative disorder (PTLD) and lymphoma. Allograft involvement by PTLD or lymphoma causes either an iso- or hypoechoic mass or diffuse cortical thickening, which are not seen in the tests case. Moreover, one would not expect PTLD to develop within five days. Citations: Rumack CM, Wilson SR, Charboneau JW. Diagnostic ultrasound, 2nd ed. Mosby . St. Louis, MO, 1998. 8 American College of Radiology
- 9. Section XII – Ultrasound Figure 5A Figure 5B 505. A 25-year-old female with a palpable right adnexal mass on routine physical examination. You are shown longitudinal (Figure 5A) and transverse (Figure 5B) endovaginal images of the right ovary. Which one of the following is the MOST likely diagnosis? A. Endometrioma B. Cystadenocarcinoma C. Tubo-ovarian abscess D. Dermoid E. Hydatid of Morgagni Diagnostic In-Training Exam 2002 9
- 10. Section XII – Ultrasound Question #505 Findings: A 4 cm predominantly cystic mass with a heterogeneous echotexture (reticulated mesh-like appearance) arises from and is partially marginated by the right ovary. Rationales: A) Incorrect. Endometriomas most often appear as cystic masses containing homogeneous hypoechoic low level echoes or debris and having irregular walls. If there is a large amount of bleeding of the endometrial tissue during the menstrual cycle, endometriomas can appear very echogenic. A solid endometrioma is usually homogeneous with medium-level echoes. Patients are asymptomatic or have dysmenorrhagia, dyspareunia, or infertility. In the test case, the finding of a heterogeneous mass and the presenting symptoms would be very unusual for an endometrioma. B) Incorrect. Cystadenocarcinoma is typically found in patients over the age of 40. The lack of septations and papillary projections also makes this diagnosis less than likely. C) Incorrect. Tubo-ovarian abscess tends to be an irregular, cystic lesion associated with inflammatory changes elsewhere in the pelvis. It is typically homogeneous and usually contains debris. A dilated fallopian tube is also common. Since pelvic inflammatory disease is a bilateral process, the contralateral adnexum is also abnormal Finally, patients are asymptomatic and have pelvic pain and vaginal discharge. None of these findings is present in the test images, and therefore, the diagnosis of tubo-ovarian abscess would be very unlikely. D) Correct. Dermoids (mature cystic teratomas) may have a very variable appearance ranging from completely anechoic to completely hyperechoic. However, a cystic mass with an echogenic mural module (dermoid plug), a highly echogenic mass with ill-defined acoustic shadowing (“tip of the iceberg”), bony and odontoid elements, a fat-fluid or hair-fluid level, or finally, as in this case, a “dermoid mesh” are considered to be relatively specific. Complications of dermoids include torsion, rupture resulting in chemical peritonitis (rupture occurs in approximately 1% of cases), and malignant transformation (approximately 2% of cases in older women). E) Incorrect. Part of the cranial end of the paramesonephric duct may persist as a vesicular appendage to the uterine tube, the hydatid of Morgagni. Sonographically these are small, unilocular, thin-walled cysts, an appearance that does not fit this case. Citations: Callen. Ultrasound in Obstetrics & Gynecology, 4th ed. WB Saunders, Philadelphia, PA. 10 American College of Radiology
