Urinary system
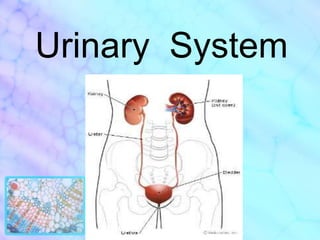
- 2. Urinary System The urinary system (excretory system) is the organ system that produces, stores, and eliminates urine. In humans it includes two kidneys, two ureters, the bladder, the urethra, and two sphincter muscles.
- 4. Regulation of electrolytes (e.g. sodium, potassium and calcium)
- 5. Regulation of blood pressure (via maintaining salt and water balance)
- 6. Serve the body as a natural filter of the blood
- 7. Responsible for the reabsorption of water, glucose, and amino acids
- 9. Ureters 2 muscular tubes that propel urine from the kidneys through renal pelvis to the urinary bladder
- 10. Urinary Bladder a distensible reservoir for urine located in the pelvis, posterior to pubis symphysis Size & shape change as it fills Contains three openings: two for ureters (Ureteric orifices) One for urethra (Internal urethral orifice) The triangular region defined by these three openings is called Trigone
- 13. In males, the urethra travels through the penis, and carries semen as well as urine
- 15. Kidney
- 16. Renal capsule Tough capsule made of collagenous fibers and connected on the kidney by areolar tissue As it proceeds medially towards the hilum, it connects with the connective tissue of the vessels which are entering kidney. Perirenal fascia (or renal fascia envelope), encloses the kidneys and the suprarenal glands and contain the perirenal fat as cushioning for these structures.
- 19. Cortex It is brownish-red in color, 1 cm wide and lies beneath fibrous renal capsule. Medullary rays penetrate the cortex,
- 22. Medulla It consists of several large pyramids. Their apices (papillae) point towards the renal pelvis. It can be distinguished in 2 zones: the reddish external zone (with internal and external striations); the pale internal zone.
- 25. The kidney is made up of 10-18 lobes.
- 26. The bases of the renal pyramids are enveloped by a cortex. Its apices are called renal papilla.
- 27. Renal papilla open to the renal pelvis via a branch of a renal pelvis called a calyx.
- 30. Nephrons
- 33. PARTS OF NEPHRON 4. Distal tubule a. Thick Ascending Limb (TAL) b. Macula densa c. Distal Convoluted Tubule (DCT) 5. Collecting Duct (CD)
- 34. Podocytes: * Podocytes are highly specialized cells * envelope the glomerular capillaries with foot projections. * The podocytes are thus the visceral layer of the Bowmann's capsule and part of the filtration barrier of the glomerular filtration.
- 45. Types of Nephrons Juxtamedullarynephrons Cortical nephrons
- 47. These have long loops of Henle that extend deep into the inner zone of the medulla.
- 49. Located in the renal cortex
- 51. Renal Interstitium Is the Connective Tissue of the kidney parenchyma that surrounds the nephrons, ducts, and blood and lymph vessels. Its volume, in the cortex, is relatively small, but increases in the medulla. It includes fibroblast-like cells, mononuclear cells, and small bundles of collagen fibers in a highly hydrated proteoglycan matrix.
- 54. Location: Cortex of the Kidney
- 55. Have long, tapering processes that are in contact with processes of like cells.
- 56. Cytoplasm contains occasional small lipid droplets and dilated cisternae of rough E.R. that may contain flocculent material of low electron density.
- 57. These interstitial cells are believed to produce the fibrous and amorphous components of the extracellular matrix.
- 59. Location: Cortex of the Kidney
- 60. More or less spherical in shape
- 61. Have a large heterochromatic nucleus surrounded by a relatively thin rim of cytoplasm.
- 62. It is likely that they are early stages of monocyte-macrophage lineage.***Both of these cells synthesize and secrete collagen and glycosaminoglycans of the extracellular matrix.
- 64. Fibroblast-like cells that differ from those of the cortex in their orientation and in their ultrastructure.
- 66. Presence of multiple lipid droplets
- 67. Have endocrine function in the regulation of systemic blood pressure.
- 69. Histophysiology of the Kidney Vasa recta containing descending arterioles and ascending venules act as countercurrent exchangers Interaction between collecting ducts, loops of Henle, and vasa rectae is required for concentrating urine by the countercurrent exchange mechanism
- 75. Urinary System Ureters, Urinary Bladder and Urethra
- 76. Ureters…
- 77. Ureters Lined by “Transitional Epithelium (UROTHELIUM)” in the luminal surface of it’s wall Smooth Muscle and CT in the remainder wall. Inner : longitudinal layer Middle : circular layer Outer : longitudinal layer – – only at distal end of ureter
- 79. Muscular coat
- 80. Fibrous coat or Adventitia
- 82. Mucosa Inner layer Consists of : EPITHELIUM transitional type, avascular and w/out lymphatics LAMINA PROPRIA w/ areolar CT and vascular
- 83. Mucosa The urinary sites have no muscularis mucosae, and therefore, the lamina propria and the submucosa tend to merge. Sometimes the connective tissue closest to the mucularis is called the submucosa. There is no distinct submucosa
- 84. Mucosa LP
- 85. Mucosa LP
- 86. Muscular Coat “Muscularis” Consists of Smooth Muscle Main function is peristalsis – –propel urine Inner : longitudinal layer Middle : circular layer Outer : longitudinal layer – – only at distal end of ureter
- 89. Muscular Coat In contrast to the muscularis of the intestinal tract, this muscular coat of UT is not arranged in clearly defined longitudinal and circular layer. Instead, it is made up of anastomosing bundles of muscle fibers of varying orientation. Although the inner bundles are predominantly of both layers, they grade with each other with no clearly defined boundary.
- 91. Fibrous Coat “Adventitia” or “serosa” Supporting layer of Fibrous CT With Adipose tissue, vessels an nerves
- 93. Urinary Bladder
- 95. Mucosa
- 96. Muscularis
- 98. Urinary Bladder wall: Mucosa * innermost portion of the urinary bladder is the mucosa.
- 99. Urinary Bladder wall: Mucosa Layers you will found in Mucosa Transitional Epithelium Lamina Propria 2.1. subepithelial region 2.2. Deeper zone
- 100. Urinary Bladder wall: Mucosa Layers in mucosa:
- 101. Urinary Bladder wall: Mucosa Layers in mucosa: 2. Lamina Propria - wider in urinary bladder than in ureter - have two zones: - subepithelial region - deep zone
- 102. Urinary Bladder wall: Mucosa Lamina Propria: Subepithelial Region - denser with fine fibers - numerous fibroblasts Lamina Propria: Deeper Zone - Typical loose or moderately dense irregular connective tissue, which extends between the muscle fibers as interstitial connective tissue
- 103. Urinary Bladder wall: muscularis similar to those in the ureter except for its thickness A smooth muscle smooth muscle of the bladder is called the detrusor muscle Contraction of this muscle expels urine from the bladder.
- 105. Urinary Bladder wall: muscularis Muscularis is subdivided into three layers of anastomoting smooth muscle(that’s why they can’t be clearly separated from each other), namely: a.) inner longitudinal layer b.) middle circular layer - thickest c.) outer longitudinal layer – most prominent and compact on the dorsal and ventral surfaces of bladder The interstitial connective tissue(loose connective tissue) merges with the connective tissue of serosa
- 107. Urinary Bladder wall: Serosa Located at the superior surface of the bladder composed of a simple squamous epithelium overlying a small bit of connective tissue Have two layers: Superficial connective tissue Peritonel mesothelium (outermost layer) Beyond the serosa, covering the bladder is perivesical fat. This is a layer of fat surrounding bladder
- 108. Internal urethral sphincter toward the opening of urethra, the muscle fibers form the involuntary internal urethral sphincter A ring-like arrangement of muscle around the opening of urethra, in the region of trigone at the base of bladder
- 109. Urethra…
- 111. start of the urethra
- 112. composed of smooth muscle
- 115. Prostatic Urethra First portion 3 to 4 cm from the neck of the bladder to the prostate gland Lined with transitional epithelium (urothelium)
- 117. Transitional epithelium is the lining proximal to the ejaculatory duct and distal to this, it becomes psuedostratified or stratified columnar epithelium with occasional mucus-secreting goblet cells. Most of the cells in the lumen are polygonal in outline with abundant microvilli. These microvilli tend to confine at the periphery, leaving the central area smooth.
- 118. Membranous Urethra Second part (shortest) 1 cm from the apex of the prostate gland to the bulb of the penis It passes through external urethral sphincter, which is composed of skeletal muscles(voluntary) Lined with pseudostratified columnar epithelium
- 119. Spongy(penile) Urethra Third part (longest) About 15 cm through the length of the penis and opens on the body surface of the glands penis Surrounded by spongy tissue called “corpus spongiosum” Lined with pseudostratified columnar epithelium except at the distal part where it is lined with stratified squamous epithelium
- 120. Spongy(penile) Urethra Ducts of the “bulbourethral glands (cowper’s glands)” and the mucus-secreting “urethral glands (glands of Littré)” empty into this area. *Bulbourethral glands (cowper’s glands) - small exocrine glands present in the reproductive system of human males *Urethral glands (glands of Littré) - glands secrete mucus, which is incorporated into the semen, and are most numerous in the section of the urethra that runs through the penis
- 122. Female Urethra Short 3 to 5 cm in length from the bladder to the vestibule of the vagina Lined by stratified squamous epithelium before it terminates Psuedostratifiedcolumnar epithelium at the midportion
- 123. Female Urethra In the lumen, there are openings of numerous small urethral glands Other glands, paraurethral glands secreting alkaline secretion opens in each side of external urethral orifice. Lamina propria is highly vascularized layer of loose CT with abundant elastic fibers Urethral sphincter (voluntary) is composed of striated muscles.
- 124. Female Urethra Short 3 to 5 cm in length from the bladder to the vestibule of the vagina Lined by stratified squamous epithelium before it terminates Psuedostratifiedcolumnar epithelium at the midportion
Hinweis der Redaktion
- Inner : longitudinal layerMiddle : circular layerOuter : longituinal layer
- Inner : longitudinal layerMiddle : circular layerOuter : longituinal layer
- LP
- LP
