A new age for frail older people?
•
1 gefällt mir•5,510 views
Deloitte report on the challenges and solutions in caring for the increasing numbers of frail older people. For further information, please visit http://www.deloitte.com/view/en_GB/uk/industries/life-sciences/better-care-for-frail-older-people/index.htm
Melden
Teilen
Melden
Teilen
Downloaden Sie, um offline zu lesen
Empfohlen
Frailty: building understanding, empathy and the skills to support self-care
Guest speaker:Dr Dawn Moody, Director - Fusion48
An opportunity to learn about some innovative approaches to making the health and care workforce 'Fit for Frailty'* (*British Geriatrics Society 2015).
Learning outcomes:
To explore the Frailty Fulcrum as a tool for holistic assessment and management of frailty
To hear how Virtual Reality is being used to build empathy for older people living with frailty
To learn about the impact of a county-wide, multi-agency, multi-professional training an toolkit for care professionals working with older people
Resources:www.fusion48.net
Presentation slides Frailty: building understanding, empathy and the skills t...

Presentation slides Frailty: building understanding, empathy and the skills t...NHS Improving Quality
Empfohlen
Frailty: building understanding, empathy and the skills to support self-care
Guest speaker:Dr Dawn Moody, Director - Fusion48
An opportunity to learn about some innovative approaches to making the health and care workforce 'Fit for Frailty'* (*British Geriatrics Society 2015).
Learning outcomes:
To explore the Frailty Fulcrum as a tool for holistic assessment and management of frailty
To hear how Virtual Reality is being used to build empathy for older people living with frailty
To learn about the impact of a county-wide, multi-agency, multi-professional training an toolkit for care professionals working with older people
Resources:www.fusion48.net
Presentation slides Frailty: building understanding, empathy and the skills t...

Presentation slides Frailty: building understanding, empathy and the skills t...NHS Improving Quality
Weitere ähnliche Inhalte
Mehr von Deloitte UK
Mehr von Deloitte UK (20)
The COVID-19 crisis: Economic impact and policy responses

The COVID-19 crisis: Economic impact and policy responses
Kürzlich hochgeladen
Models Call Girls In Hyderabad 9630942363 Hyderabad Call Girl & Hyderabad Escort ServiceModels Call Girls In Hyderabad 9630942363 Hyderabad Call Girl & Hyderabad Esc...

Models Call Girls In Hyderabad 9630942363 Hyderabad Call Girl & Hyderabad Esc...GENUINE ESCORT AGENCY
Kürzlich hochgeladen (20)
Russian Call Girls Service Jaipur {8445551418} ❤️PALLAVI VIP Jaipur Call Gir...

Russian Call Girls Service Jaipur {8445551418} ❤️PALLAVI VIP Jaipur Call Gir...
Independent Call Girls Service Mohali Sector 116 | 6367187148 | Call Girl Ser...

Independent Call Girls Service Mohali Sector 116 | 6367187148 | Call Girl Ser...
Top Rated Pune Call Girls (DIPAL) ⟟ 8250077686 ⟟ Call Me For Genuine Sex Serv...

Top Rated Pune Call Girls (DIPAL) ⟟ 8250077686 ⟟ Call Me For Genuine Sex Serv...
Call Girls Amritsar Just Call 8250077686 Top Class Call Girl Service Available

Call Girls Amritsar Just Call 8250077686 Top Class Call Girl Service Available
Models Call Girls In Hyderabad 9630942363 Hyderabad Call Girl & Hyderabad Esc...

Models Call Girls In Hyderabad 9630942363 Hyderabad Call Girl & Hyderabad Esc...
Independent Call Girls In Jaipur { 8445551418 } ✔ ANIKA MEHTA ✔ Get High Prof...

Independent Call Girls In Jaipur { 8445551418 } ✔ ANIKA MEHTA ✔ Get High Prof...
Call Girl In Pune 👉 Just CALL ME: 9352988975 💋 Call Out Call Both With High p...

Call Girl In Pune 👉 Just CALL ME: 9352988975 💋 Call Out Call Both With High p...
Coimbatore Call Girls in Thudiyalur : 7427069034 High Profile Model Escorts |...

Coimbatore Call Girls in Thudiyalur : 7427069034 High Profile Model Escorts |...
Call Girls Hyderabad Just Call 8250077686 Top Class Call Girl Service Available

Call Girls Hyderabad Just Call 8250077686 Top Class Call Girl Service Available
Call Girls Kolkata Kalikapur 💯Call Us 🔝 8005736733 🔝 💃 Top Class Call Girl Se...

Call Girls Kolkata Kalikapur 💯Call Us 🔝 8005736733 🔝 💃 Top Class Call Girl Se...
Andheri East ^ (Genuine) Escort Service Mumbai ₹7.5k Pick Up & Drop With Cash...

Andheri East ^ (Genuine) Escort Service Mumbai ₹7.5k Pick Up & Drop With Cash...
Top Quality Call Girl Service Kalyanpur 6378878445 Available Call Girls Any Time

Top Quality Call Girl Service Kalyanpur 6378878445 Available Call Girls Any Time
Call Girls Madurai Just Call 9630942363 Top Class Call Girl Service Available

Call Girls Madurai Just Call 9630942363 Top Class Call Girl Service Available
Low Rate Call Girls Bangalore {7304373326} ❤️VVIP NISHA Call Girls in Bangalo...

Low Rate Call Girls Bangalore {7304373326} ❤️VVIP NISHA Call Girls in Bangalo...
Russian Call Girls Lucknow Just Call 👉👉7877925207 Top Class Call Girl Service...

Russian Call Girls Lucknow Just Call 👉👉7877925207 Top Class Call Girl Service...
9630942363 Genuine Call Girls In Ahmedabad Gujarat Call Girls Service

9630942363 Genuine Call Girls In Ahmedabad Gujarat Call Girls Service
Top Rated Hyderabad Call Girls Chintal ⟟ 9332606886 ⟟ Call Me For Genuine Se...

Top Rated Hyderabad Call Girls Chintal ⟟ 9332606886 ⟟ Call Me For Genuine Se...
Mumbai ] (Call Girls) in Mumbai 10k @ I'm VIP Independent Escorts Girls 98333...![Mumbai ] (Call Girls) in Mumbai 10k @ I'm VIP Independent Escorts Girls 98333...](data:image/gif;base64,R0lGODlhAQABAIAAAAAAAP///yH5BAEAAAAALAAAAAABAAEAAAIBRAA7)
![Mumbai ] (Call Girls) in Mumbai 10k @ I'm VIP Independent Escorts Girls 98333...](data:image/gif;base64,R0lGODlhAQABAIAAAAAAAP///yH5BAEAAAAALAAAAAABAAEAAAIBRAA7)
Mumbai ] (Call Girls) in Mumbai 10k @ I'm VIP Independent Escorts Girls 98333...
Call Girls Rishikesh Just Call 8250077686 Top Class Call Girl Service Available

Call Girls Rishikesh Just Call 8250077686 Top Class Call Girl Service Available
Call Girls Service Jaipur {8445551418} ❤️VVIP BHAWNA Call Girl in Jaipur Raja...

Call Girls Service Jaipur {8445551418} ❤️VVIP BHAWNA Call Girl in Jaipur Raja...
A new age for frail older people?
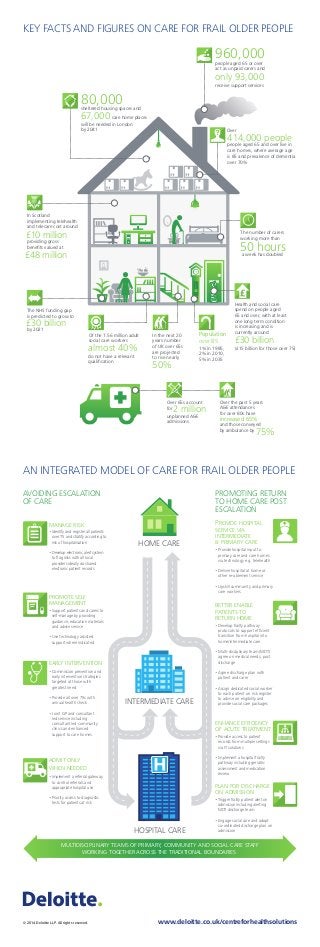
- 1. KEY FACTS AND FIGURES ON CARE FOR FRAIL OLDER PEOPLE © 2014 Deloitte LLP. All rights reserved. www.deloitte.co.uk/centreforhealthsolutions Health and social care spend on people aged 65 and over, with at least one long term condition is increasing and is currently around (£15 billion for those over 75) £30 billion people aged 65 and over live in care homes, where average age is 85 and prevalence of dementia over 70% 960,000people aged 65 or over act as unpaid carers and only 93,000 receive support services The number of carers working more than a week has doubled 50 hours Over 414,000 people In Scotland implementing telehealth and telecare cost around providing gross benefits valued at 80,000sheltered housing spaces and 67,000 will be needed in London by 2041 care home places £10 million £48 million The NHS funding gap is predicted to grow to by 2021 £30 billion do not have a relevant qualification Of the 1.56 million adult social care workers almost 40% In the next 20 years number of UK over 65s are projected to rise nearly 50% 1% in 1985, 2% in 2010, 5% in 2035 Population over 85 Over 65s account for unplanned A&E admissions 2 million Over the past 5 years A&E attendances for over 80s have and those conveyed by ambulance by increased 65% 75% AN INTEGRATED MODEL OF CARE FOR FRAIL OLDER PEOPLE AVOIDING ESCALATION OF CARE multidisciplinary teams of primary, community and social care staff working together across the traditional boundaries INTERMEDIATE CARE PROMOTING RETURN TO HOME CARE POST ESCALATION HOSPITAL CARE HOME CARE manage risk plan for discharge on admission •Trigger frailty patient alert on admission including alerting MDT discharge team •Engage social care and adopt co-ordinated discharge plan on admission promote self management •Support patients and carers to self-manage by providing guidance, education materials and advice service •Use technology assisted support where indicated early intervention •Commission prevention and early intervention strategies targeted at those with greatest need •Provide all over 75s with annual health check • Joint GP and consultant led service including consultant led community clinics and enhanced support to care homes admit only when needed •Implement a referral gateway to control referrals and appropriate hospital use •Priority access to diagnostic tests for patients at risk better enable patients to return home •Develop frailty pathway protocols to support efficient transition from hospital into home/intermediate care •Multi-disciplinary team (MDT) agree on medical needs, post discharge •Agree discharge plan with patient and carer •Assign dedicated social worker to each patient on risk register to advise on eligibility and provide social care packages enhance efficiency of acute treatment •Provide access to patient records from multiple settings via IT solutions •Implement a hospital frailty pathway including geriatric assessment and medication review •Identify and register all patients over 75 and stratify according to risk of hospitalisation •Develop electronic alert system to flag risks with all local providers ideally via shared electronic patient records Provide hospital service via intermediate & primary care •Provide hospital input to primary care and care homes via technology e.g. telehealth •Deliver hospital at home or other re-ablement service •Upskill community and primary care workers
