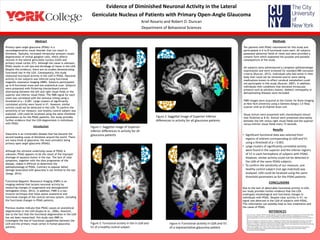
Evidence of Diminished Neuronal Activity in the Lateral Geniculate Nucleus of Patients with Primary Open-Angle Glaucoma
- 1. Primary open-angle glaucoma (POAG) is a neurodegenerative visual disorder that can result in blindness. Typically, increased intraocular pressure causes degeneration of retinal ganglion cells, which affects neurons in the lateral geniculate nucleus (LGN) and primary visual cortex (V1). Although the cause is unknown, POAG results in cell loss and shrinkage of tissue in the LGN. Despite this evidence, there are no studies demonstrating functional loss in the LGN. Consequently, this study measured functional activity in the LGN in POAG. Neuronal activity in ten subjects was inferred using functional magnetic resonance imaging (fMRI). Subjects participated up to 8 functional scans and one anatomical scan. Subjects were presented with flickering checkerboard stimuli alternating between the left and right visual fields or the superior and inferior visual fields. The fMRI signal for each voxel was correlated with the stimulus timing using a threshold of p = 0.001. Large clusters of significantly correlated activity were found in V1. However, similar activity could not be detected in the LGN. To confirm the sensitivity of our measure, one healthy control subject was analyzed. LGN could be localized using the same threshold parameters as for the POAG patients. Our study provides further evidence that the LGN degenerates in individuals with POAG. Abstract Results Methods Ten patients with POAG volunteered for this study and participated in 6 to 8 functional scans each. All subjects possessed abnormal fields of vision and were provided a consent form which explained the purpose and possible consequences of the study. All subjects were administered a complete ophthalmologic examination and were screened for standard MRI exclusion criteria (Duncan, 2012). Individuals who had metal in their body that could not be removed and/or were taking medications known to effect cerebral metabolism could not participate in this study (Duncan, 2007). In addition, individuals with conditions that elevated intraocular pressure such as pituitary lesions, diabetic retinopathy or demyelinating diseases were excluded. FMRI images were acquired at the Center for Brain Imaging at New York University using a Siemens Allegra 3.0 Tesla scanner with an 8-channel brain coil. Visual stimuli were presented with checkerboard stimuli that flickered at 8 Hz. Stimuli were presented alternately between the left versus right visual fields and the superior versus inferior visual fields every 15 seconds. CONCLUSIONS Introduction Glaucoma is an irreversible disease that has become the second leading cause of blindness around the world. There are many kinds of glaucoma, the most prevalent being primary open angle glaucoma (POAG). Although the ultimate underlying cause of POAG is unknown, POAG appears to be the result of the improper drainage of aqueous humor in the eye. The lack of clear symptoms, together with the slow progression of the disease, makes it difficult to determine the pathophysiology of POAG. Contrary to popular belief, damage associated with glaucoma is not limited to the eye (Songs, 2014). Functional Magnetic Resonance Imaging (FMRI) is an imaging method that locates neuronal activity by measuring changes of oxygenated and deoxygenated hemoglobin (Chen, 2012). In addition, FMRI is a non- invasive technique that helps assess anatomical and functional changes of the central nervous system, including the functional changes in POAG patients. Previous studies indicate that POAG causes an anatomical degeneration in the LGN (Gupta et al., 2006). However, due to the fact that the functional degeneration in the LGN has not been researched, this study uses fMRI to investigate the loss of functional capabilities between the LGN and the primary visual cortex in human glaucoma patients. Evidence of Diminished Neuronal Activity in the Lateral Geniculate Nucleus of Patients with Primary Open-Angle Glaucoma Ariel Rosario and Robert O. Duncan Department of Behavioral Sciences REFERENCES • Chen, Z.Q., Gao, J., Zhang H. (2012) Functional magnetic resonance imaging in glaucoma. Zhonghua Yan Ke Za Zhi, 48: 1045-1048. • Duncan, R.O., Sample, P.A., Bowd, C., Weinreb, R.N. & Zangwill, L.M. (2012). Arterial spin labeling fMRI measurements of decreased blood flow in primary visual cortex correlates with decreased visual function in human glaucoma. Vision Res, 1(60), 51- 60. • Duncan, R.O., Sample, P.A., Weinreb, R.N., Bowd, C., & Zangwill, L.M. (2007). Retinotopic organization of primary visual cortex in glaucoma: a method for comparing cortical function with damage to the optic disk. Invest Ophthalmol Vis Sci,48(2), 733-744. • Gupta, N., Ly, T., Zhang, P., Kaufman, Q., Weinreb, R.N., & Yücel, N. (2006). Chronic ocular hypertension induces dendrite pathology in the lateral geniculate nucleus of the brain. Exp Eye Res, 84(1), 176-184. • Song, Y., Mu, K., Wang J., Lin, F., Chen, Z., Yan, X., Hao, Y., Zhu, W., & Zhang, H. (2014). Altered spontaneous brain activity in primary open angle glaucoma: a resting-state functional magnetic resonance imaging study. PLoS One 9(2): e89493. doi:10.1371/journal.pone.0089493 Figure 3: Functional activity in the in LGN and V1 of a healthy control subject Figure 2: Saggittal image of Superior-Inferior differences in activity for all glaucoma patients Figure 1: Saggittal image of Superior- Inferior differences in activity for all glaucoma patients • Significant functional data was selected from regions of interest corresponding to LGN and V1 using a threshold of p = 0.001. • Large clusters of significantly correlated activity were found in the superior and the inferior regions of V1 in each hemisphere of subjects with POAG. However, similar activity could not be detected in the LGN of the same POAG subjects. • To confirm the sensitivity of our measure, one healthy control subject (not age-matched) was analyzed. LGN could be localized using the same threshold parameters as for the POAG patients. Figure 4: Functional activity in LGN and V1 of a representative glaucoma patient Due to the lack of detectable functional activity in LGN, our study provides further evidence that the LGN undergoes morphological and functional changes in individuals with POAG. Despite clear activity in V1, no signal was detected in the LGN of subjects with POAG. This information can possibly lead to new treatments and the cause of POAG.