lecture 18 dr may
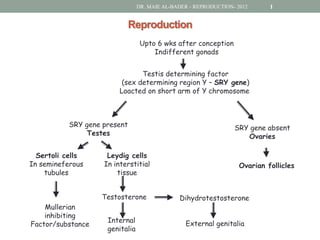
- 1. DR. MAIE AL-BADER - REPRODUCTION- 2012 1 Reproduction Upto 6 wks after conception Indifferent gonads Testis determining factor (sex determining region Y – SRY gene) Loacted on short arm of Y chromosome SRY gene present SRY gene absent Testes Ovaries Sertoli cells Leydig cells In semineferous In interstitial Ovarian follicles tubules tissue Testosterone Dihydrotestosterone Mullerian inhibiting Internal External genitalia Factor/substance genitalia
- 2. DR. MAIE AL-BADER - REPRODUCTION- 2012 2 Development of Internal Genitalia - males Before 6 wks gestation BOTH DUCTS exist in both sexes Between 6 – 8 weeks: in male, testes develop In males once the testes develop: • SERTOLI CELLS: secrete Mullerian Inhibition Factor/substance (MIF or MIS) which leads to regression of the mullerian duct • LEYDIG CELLS: secrete testosterone which lead to the growth & development of the Wolffian duct. This duct will give rise to the male internal genitalia (epididymis, vas deferens, seminal vesicle, ejaculatory duct)
- 3. DR. MAIE AL-BADER - REPRODUCTION- 2012 3 Development of Internal Genitalia - females In females: • The internal genitalia are: fallopian tubes, uterus and upper third of vagina. The absence of testosterone and MIS will lead to female internal genitalia
- 4. DR. MAIE AL-BADER - REPRODUCTION- 2012 4 Development of External Genitalia – males & females In males: • 5a-dihydrotestosterone (dependent on 5a-reductase) external genitalia (penis, prostate, scrotum and penile urethra) In females: • The external genitalia are: clitoris, labia majora and minora and lower two thirds of the vagina
- 5. DR. MAIE AL-BADER - REPRODUCTION- 2012 5 Male Reproductive System • Paired testes suspended in the scrotal sacs of the scrotum • Testes develop in abdominal cavity but descend into scrotal sac during development (sterility!) • Boys under 6 yrs of age: if testis didn’t descend, then surgical intervention
- 6. DR. MAIE AL-BADER - REPRODUCTION- 2012 6 Organ Function Testes Produce sperms and sex hormones Epididymis Sites of maturation (ability to swim) and some storage of sperm Vas deferens Conduct and store sperm Urethra Conducts sperm (and urine) Penis Organ of copulation (sexual intercourse)
- 7. DR. MAIE AL-BADER - REPRODUCTION- 2012 7 Testes consist of 2 Parts: 1. Seminiferous tubules: • Germinal cells: sperms • Sertoli cells: possess FSH receptors 2. Interstitial tissue: Interstitial/Leydig cells (possess LH receptors) testosterone
- 8. DR. MAIE AL-BADER - REPRODUCTION- 2012 8 Spermatogenesis • Spermatogenesis • occurs in the seminiferous tubules upon LH & FSH stimulation (starting at ~13 yrs of age) • Takes on average 70 days to complete • 120 million sperm are produced/day (~ 60 - 150 million/day) • Spermiogenesis: mediated by Sertoli cells that are responsible for eliminating most of the spermatid cytoplasm to give spermatozoa
- 9. DR. MAIE AL-BADER - REPRODUCTION- 2012 9 Mature sperm (spermatozoa) contain 3 parts: 1. Head: contains a nucleus covered by an acrosome (stores enzymes to penetrate egg) 2. Middle piece: contains mitochondria wrapped around microtubules of the flagellum (mitochondria provide energy for movement) 3. Tail: contains microtubules as components of flagellum; its movements propels sperm
- 10. DR. MAIE AL-BADER - REPRODUCTION- 2012 10 • Mature sperm gain motility in epididymis and become more resistant to changes in pH & temperature (most sperms stored in the vas deferens) • During ejaculation sperms and secretions from the seminal vesicle, prostate gland and bulbourethral gland make up the semen which is carried by the ejaculatory duct to the urethra
- 11. DR. MAIE AL-BADER - REPRODUCTION- 2012 11 Control of Male Sex Hormone Secretion
- 12. DR. MAIE AL-BADER - REPRODUCTION- 2012 12 Functions of Testosterone • It is the main sex hormone in males • Essential for development of male secondary sex characteristics – Tallness, longer legs, broad shoulders – Enlargement of larynx and vocal cords; deepening of voice – Greater muscles strength (athletes, side effects) – Sex drive and aggressiveness – Oil and sweat glands secretion leading to acne and body odor – Development of hair on face, chest and back – Triggers baldness if appropriate genes are present • Essential for the maturation of sperm
- 13. DR. MAIE AL-BADER - REPRODUCTION- 2012 13 Female Reproductive System
- 14. DR. MAIE AL-BADER - REPRODUCTION- 2012 14 Organ Function Ovaries Produce egg each month; produce sex hormones Oviducts (fallopian tubes) Conduct egg; location of fertilization Uterus (womb) Houses developing embryo and fetus Vagina Receives penis during copulation and serves as birth canal
- 15. DR. MAIE AL-BADER - REPRODUCTION- 2012 15 Oogenesis • Mitosis of primordial oogonia occurs in female fetus until midgestation (peak of 7 million oocytes) and then ceases. Then there is progressive loss of oocytes & by puberty there are approximately 400,000 oocytes (only ~400 follicles ovulate in women) • Oocyte begins first meiotic division in utero: first division is arrested in prophase until the time of ovulation
- 16. DR. MAIE AL-BADER - REPRODUCTION- 2012 16 • At the time of ovulation, the primary oocyte completes the first meiotic division producing the first polar body and a secondary oocyte • Sperm cell penetration (fertilization) initiates the completion of the second meiotic division and the expulsion of a second polar body
- 17. DR. MAIE AL-BADER - REPRODUCTION- 2012 17 • The follicles (granulosa and thecal cells) produce female sex hormones • Changes in the ovary are the result of changing levels of FSH and LH from the anterior pituitary • At menopause: oogenesis ceases
- 18. DR. MAIE AL-BADER - REPRODUCTION- 2012 18 Control of Ovarian Steroidogenesis Which receptors do the following cells have? Thecal cell, Granulosa cell, Luteal cell
- 19. DR. MAIE AL-BADER - REPRODUCTION- 2012 19 Menstrual cycle • Ovarian cycle • Follicular phase • Ovulation • Luteal phase • Endometrial cycle • Proliferative phase • Secretory phase • Menstruation
- 20. DR. MAIE AL-BADER - REPRODUCTION- 2012 20
- 21. DR. MAIE AL-BADER - REPRODUCTION- 2012 21 Ovarian Cycle: Follicular Phase • Lasts from day 1 to about day 13 of the cycle (assuming that the cycle is 28 days) during which: • 7-12 primary follicles stimulated secondary follicle graafian follicle (only ONE will become mature graafian follicle) • Granulosa and thecal cells secrete estradiol (peaks at ~ day 12; 2 days before ovulation) • Granulosa cells are stimulated by FSH; thecal cells are stimulated by LH • Toward the end of the follicular phase: FSH and estradiol stimulate the production of LH receptors in graafian follicle preparing the follicle to the next half of the cycle • The rapid increase in estradiol secretion positive feedback effect rapid LH secretion LH SURGE
- 22. DR. MAIE AL-BADER - REPRODUCTION- 2012 22 Ovarian Cycle: Ovulation & Luteal Phase Ovulation • A woman usually ovulates only one ovum a month • FSH growth and maturation of graafian follicle & rapid estradiol secretion makes a thin walled blister on ovary surface estradiol secretion triggers LH surge rupture graafian follicle wall (day 14) OVULATION expulsion of secondary oocyte (with the 1st polar body) out of the ovaries into fallopian tube • If ova is fertilized by a sperm entering its cytoplasm ova completes the second meiotic division formation of 2nd polar body Luteal Phase • After ovulation LH stimulates empty follicle (corpus luteum) to secrete estradiol & progesterone (and inhibin which inhibits FSH only) negative feedback inhibition of FSH and LH prevents the development of a new follicle regression of corpus luteum decrease in estrogen and progesterone (starting at day 22 reaching very low levels by day 28) MENSTRUATION
- 23. DR. MAIE AL-BADER - REPRODUCTION- 2012 23 Endometrial Cycle: Proliferative, Secretory & Menstrual Phases Proliferative Phase • Occurs during ovarian follicular phase • An increase in estradiol stimulates the growth (proliferation) of stratum functionale of the endometrium Secretory Phase • Occurs during ovarian luteal phase • An increase in progesterone stimulates development of uterine glands • Effects of increased estradiol and progesterone levels: • endometrium becomes thick, vascular and spongy in appearance • the uterine glands become engorged with glycogen, lipids & proteins • endometrium ready to accept and nourish an embryo Menstruation • Resulting from: • A decrease in estradiol and progesterone levels during late luteal phase • Constriction of the spiral arteries leading to necrosis and sloughing of the stratum functionale
- 24. DR. MAIE AL-BADER - REPRODUCTION- 2012 24 Functions of Estrogens & Progesterone • Estrogen is responsible for development and maintenance of female secondary sexual characteristics. • Less body and facial hair, more fat beneath the skin to give a rounded appearance. • Enlargement of pelvic girdle and cavity to give wider hips. • Both estrogen and progesterone – are required for breast development – help maintain endometrium during pregnancy – help suppress gonadotropin secretion – inhibit prolactin secretion
- 25. DR. MAIE AL-BADER - REPRODUCTION- 2012 25 Fertilization, Pregnancy & Parturition Fertilization • During the act of sexual intercourse, the male ejaculates ~ 300 million sperms into the female vagina • ONLY ~100-200 sperms survive to enter fallopian tube & stay for ~3 days • Secondary oocyte in the fallopian tube lasts for ~ 24 hrs following ovulation • So when does fertilization occur ?
- 26. DR. MAIE AL-BADER - REPRODUCTION- 2012 26 Cleavage & Blastocyst Formation • Cleavage occurs as the zygote goes down the fallopian tube giving a morula • Blastocyst (early embryonic structure) consists of: • An inner cell mass develops into fetus • Surrounding chorion (trophoblast cells) will become part of placenta • Day 5th - 6th: blastocyst is attached to the uterine wall (trophoblast cells initiate implantation) • Day 7th - 10th: blastocyst is completely buried in the endometrium and the hormone human chorionic gonadotrophin (hCG) is now secreted
- 27. DR. MAIE AL-BADER - REPRODUCTION- 2012 27 Implantation & Formation of Placenta • If fertilization does not take place corpus luteum begins to regress (10 days after ovulation) decreased secretion of steroids menstruation • If fertilization takes place, above changes are prevented by secretion of hCG: • This hormone is identical to LH: maintain corpus luteum secretion of estradiol and progesterone maintain the endometrium prevents menstruation • it is required for the first 5-8 weeks of pregnancy until the placenta becomes active
- 28. DR. MAIE AL-BADER - REPRODUCTION- 2012 28 The Structure & Function of the Placenta • The placenta is a unique organ where exchange between fetal blood and mother's blood takes place. • By the 10th week it is fully formed and has begun to produce estrogen and progesterone • Chorionic villi are treelike extensions of the chorion: they project into the surrounding maternal tissues; maternal and fetal blood do not mix
- 29. DR. MAIE AL-BADER - REPRODUCTION- 2012 29 Functions of Placenta 1. Exchange of molecules across placenta: • The umbilical arteries deliver fetal blood chorionic villi blood circulates within the villi umbilical vein back to the fetus • Maternal blood is delivered to and drained from the cavities within decidua basalis (maternal part; located between the chorionic villi) maternal and fetal blood are brought close together • Serves as a site for the exchange of gases (O2 and CO2), nutrient molecules and waste products
- 30. DR. MAIE AL-BADER - REPRODUCTION- 2012 30 2. Endocrine function of placenta: • Human chorionic gonadotropin (hCG) • Fetal-placental unit • After 5 ½ weeks of conception: • Placenta starts secreting estrogens and progesterone • Placenta is an incomplete gland because: • It lacks precursors, cholesterol • It lacks enzymes needed to convert progesterone into androgens (therefore in fetus progesterone is converted into androgens converted into estrogens in placenta) • Fetal-placental unit: interaction between placenta and embryo to produce steroid hormones
- 31. DR. MAIE AL-BADER - REPRODUCTION- 2012 31 Labour & Parturition • Powerful contractions of the uterus in LABOUR: • are needed for childbirth (PARTURITION) • are stimulated by oxytocin and prostaglandins
- 32. DR. MAIE AL-BADER - REPRODUCTION- 2012 32 Lactation